Get your patient on Vasotec - Enalapril Maleate tablet (Enalapril Maleate)
Vasotec - Enalapril Maleate tablet prescribing information
WARNING: FETAL TOXICITY
See full prescribing information for complete boxed warning.
- When pregnancy is detected, discontinue VASOTEC ® as soon as possible.
- Drugs that act directly on the renin-angiotensin system can cause injury and death to the developing fetus (see WARNINGS, Fetal Toxicity ).
INDICATIONS AND USAGE
Hypertension
VASOTEC is indicated for the treatment of hypertension.
VASOTEC is effective alone or in combination with other antihypertensive agents, especially thiazide-type diuretics. The blood pressure lowering effects of VASOTEC and thiazides are approximately additive.
Heart Failure
VASOTEC is indicated for the treatment of symptomatic congestive heart failure, usually in combination with diuretics and digitalis. In these patients VASOTEC improves symptoms, increases survival, and decreases the frequency of hospitalization (see CLINICAL PHARMACOLOGY , Heart Failure , Mortality Trials for details and limitations of survival trials).
Asymptomatic Left Ventricular Dysfunction
In clinically stable asymptomatic patients with left ventricular dysfunction (ejection fraction ≤35 percent), VASOTEC decreases the rate of development of overt heart failure and decreases the incidence of hospitalization for heart failure (see CLINICAL PHARMACOLOGY , Heart Failure , Mortality Trials for details and limitations of survival trials).
In using VASOTEC consideration should be given to the fact that another angiotensin-converting enzyme inhibitor, captopril, has caused agranulocytosis, particularly in patients with renal impairment or collagen vascular disease, and that available data are insufficient to show that VASOTEC does not have a similar risk (see WARNINGS , Neutropenia/Agranulocytosis ).
In considering use of VASOTEC, it should be noted that in controlled clinical trials ACE inhibitors have an effect on blood pressure that is less in black patients than in non-blacks. In addition, it should be noted that black patients receiving ACE inhibitors have been reported to have a higher incidence of angioedema compared to non-blacks (see WARNINGS , Head and Neck Angioedema ).
DOSAGE AND ADMINISTRATION
Hypertension
In patients who are currently being treated with a diuretic, symptomatic hypotension occasionally may occur following the initial dose of VASOTEC. The diuretic should, if possible, be discontinued for two to three days before beginning therapy with VASOTEC to reduce the likelihood of hypotension (see WARNINGS , Hypotension ). If the patient’s blood pressure is not controlled with VASOTEC alone, diuretic therapy may be resumed.
If the diuretic cannot be discontinued an initial dose of 2.5 mg should be used under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS , Hypotension and PRECAUTIONS , Drug Interactions ).
The recommended initial dose in patients not on diuretics is 5 mg once a day. Dosage should be adjusted according to blood pressure response. The usual dosage range is 10 to 40 mg per day administered in a single dose or two divided doses. In some patients treated once daily, the antihypertensive effect may diminish toward the end of the dosing interval. In such patients, an increase in dosage or twice daily administration should be considered. If blood pressure is not controlled with VASOTEC alone, a diuretic may be added. Concomitant administration of VASOTEC with potassium supplements, potassium salt substitutes, or potassium-sparing diuretics may lead to increases of serum potassium (see PRECAUTIONS ).
Dosage Adjustment in Hypertensive Patients with Renal Impairment
The usual dose of enalapril is recommended for patients with a creatinine clearance more than 30 mL/min (serum creatinine of up to approximately 3 mg/dL). For patients with creatinine clearance less than or equal to 30 mL/min (serum creatinine more than or equal to 3 mg/dL), the first dose is 2.5 mg once daily. The dosage may be titrated upward until blood pressure is controlled or to a maximum of 40 mg daily.
| Renal Status | Creatinine Clearance (mL/min) | Initial Dose (mg/day) |
|---|---|---|
Normal Renal Function | >80 mL/min | 5 mg |
Mild Impairment | ≤80 >30 mL/min | 5 mg |
Moderate to Severe Impairment | ≤30 mL/min | 2.5 mg |
Dialysis Patients See WARNINGS, Anaphylactoid Reactions During Membrane Exposure . | 2.5 mg on dialysis days Dosage on nondialysis days should be adjusted depending on the blood pressure response. |
Heart Failure
VASOTEC is indicated for the treatment of symptomatic heart failure, usually in combination with diuretics and digitalis. In the placebo-controlled studies that demonstrated improved survival, patients were titrated as tolerated up to 40 mg, administered in two divided doses.
The recommended initial dose is 2.5 mg. The recommended dosing range is 2.5 to 20 mg given twice a day. Doses should be titrated upward, as tolerated, over a period of a few days or weeks. The maximum daily dose administered in clinical trials was 40 mg in divided doses.
After the initial dose of VASOTEC, the patient should be observed under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS and PRECAUTIONS , Drug Interactions ). If possible, the dose of any concomitant diuretic should be reduced which may diminish the likelihood of hypotension. The appearance of hypotension after the initial dose of VASOTEC does not preclude subsequent careful dose titration with the drug, following effective management of the hypotension.
Asymptomatic Left Ventricular Dysfunction
In the trial that demonstrated efficacy, patients were started on 2.5 mg twice daily and were titrated as tolerated to the targeted daily dose of 20 mg (in divided doses).
After the initial dose of VASOTEC, the patient should be observed under medical supervision for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS and PRECAUTIONS , Drug Interactions ). If possible, the dose of any concomitant diuretic should be reduced which may diminish the likelihood of hypotension. The appearance of hypotension after the initial dose of VASOTEC does not preclude subsequent careful dose titration with the drug, following effective management of the hypotension.
Dosage Adjustment in Patients with Heart Failure and Renal Impairment or Hyponatremia
In patients with heart failure who have hyponatremia (serum sodium less than 130 mEq/L) or with serum creatinine greater than 1.6 mg/dL, therapy should be initiated at 2.5 mg daily under close medical supervision (see DOSAGE AND ADMINISTRATION , Heart Failure , WARNINGS and PRECAUTIONS , Drug Interactions ). The dose may be increased to 2.5 mg b.i.d. (twice a day), then 5 mg b.i.d (twice a day) and higher as needed, usually at intervals of four days or more if at the time of dosage adjustment there is not excessive hypotension or significant deterioration of renal function. The maximum daily dose is 40 mg.
Pediatric Hypertensive Patients
The usual recommended starting dose is 0.08 mg/kg (up to 5 mg) once daily. Dosage should be adjusted according to blood pressure response. Doses above 0.58 mg/kg (or in excess of 40 mg) have not been studied in pediatric patients (see CLINICAL PHARMACOLOGY , Clinical Pharmacology in Pediatric Patients ).
VASOTEC is not recommended in neonates and in pediatric patients with glomerular filtration rate less than 30 mL/min/1.73 m 2 , as no data are available.
Preparation of Suspension (for 200 mL of a 1.0 mg/mL suspension)
Add 50 mL of sodium citrate and citric acid oral solution, USP to a polyethylene terephthalate (PET) bottle containing ten 20 mg tablets of VASOTEC and shake for at least 2 minutes. Let concentrate stand for 60 minutes. Following the 60-minute hold time, shake the concentrate for an additional minute. Add 150 mL of Ora-Sweet SF to the concentrate in the PET bottle and shake the suspension to disperse the ingredients. The suspension should be refrigerated at 2° to 8°C (36° to 46°F) and can be stored for up to 30 days. Shake the suspension before each use.
CONTRAINDICATIONS
VASOTEC is contraindicated in patients who are hypersensitive to this product and in patients with a history of angioedema related to previous treatment with an angiotensin-converting enzyme inhibitor and in patients with hereditary or idiopathic angioedema.
Do not coadminister aliskiren with VASOTEC in patients with diabetes (see PRECAUTIONS , Drug Interactions ).
VASOTEC is contraindicated in combination with a neprilysin inhibitor (e.g., sacubitril). Do not administer VASOTEC within 36 hours of switching to or from sacubitril/valsartan, a neprilysin inhibitor (see WARNINGS , Head and Neck Angioedema ).
ADVERSE REACTIONS
VASOTEC has been evaluated for safety in more than 10,000 patients, including over 1000 patients treated for one year or more. VASOTEC has been found to be generally well tolerated in controlled clinical trials involving 2987 patients. For the most part, adverse experiences were mild and transient in nature. In clinical trials, discontinuation of therapy due to clinical adverse experiences was required in 3.3 percent of patients with hypertension and in 5.7 percent of patients with heart failure. The frequency of adverse experiences was not related to total daily dosage within the usual dosage ranges. In patients with hypertension the overall percentage of patients treated with VASOTEC reporting adverse experiences was comparable to placebo.
Hypertension
Adverse experiences occurring in greater than one percent of patients with hypertension treated with VASOTEC in controlled clinical trials are shown below. In patients treated with VASOTEC, the maximum duration of therapy was three years; in placebo-treated patients the maximum duration of therapy was 12 weeks.
| VASOTEC (n=2314) Incidence (discontinuation) | Placebo (n=230) Incidence | |
|---|---|---|
Body As A Whole | ||
Fatigue | 3.0 (<0.1) | 2.6 |
Orthostatic Effects | 1.2 (<0.1) | 0.0 |
Asthenia | 1.1 (0.1) | 0.9 |
Digestive | ||
Diarrhea | 1.4 (<0.1) | 1.7 |
Nausea | 1.4 (0.2) | 1.7 |
Nervous/Psychiatric | ||
Headache | 5.2 (0.3) | 9.1 |
Dizziness | 4.3 (0.4) | 4.3 |
Respiratory | ||
Cough | 1.3 (0.1) | 0.9 |
Skin | ||
Rash | 1.4 (0.4) | 0.4 |
Heart Failure
Adverse experiences occurring in greater than one percent of patients with heart failure treated with VASOTEC are shown below. The incidences represent the experiences from both controlled and uncontrolled clinical trials (maximum duration of therapy was approximately one year). In the placebo-treated patients, the incidences reported are from the controlled trials (maximum duration of therapy is 12 weeks). The percentage of patients with severe heart failure (NYHA Class IV) was 29 percent and 43 percent for patients treated with VASOTEC and placebo, respectively.
| VASOTEC (n=673) Incidence (discontinuation) | Placebo (n=339) Incidence | |
|---|---|---|
Body As A Whole | ||
Orthostatic Effects | 2.2 (0.1) | 0.3 |
Syncope | 2.2 (0.1) | 0.9 |
Chest Pain | 2.1 (0.0) | 2.1 |
Fatigue | 1.8 (0.0) | 1.8 |
Abdominal Pain | 1.6 (0.4) | 2.1 |
Asthenia | 1.6 (0.1) | 0.3 |
Cardiovascular | ||
Hypotension | 6.7 (1.9) | 0.6 |
Orthostatic Hypotension | 1.6 (0.1) | 0.3 |
Angina Pectoris | 1.5 (0.1) | 1.8 |
Myocardial Infarction | 1.2 (0.3) | 1.8 |
Digestive | ||
Diarrhea | 2.1 (0.1) | 1.2 |
Nausea | 1.3 (0.1) | 0.6 |
Vomiting | 1.3 (0.0) | 0.9 |
Nervous/Psychiatric | ||
Dizziness | 7.9 (0.6) | 0.6 |
Headache | 1.8 (0.1) | 0.9 |
Vertigo | 1.6 (0.1) | 1.2 |
Respiratory | ||
Cough | 2.2 (0.0) | 0.6 |
Bronchitis | 1.3 (0.0) | 0.9 |
Dyspnea | 1.3 (0.1) | 0.4 |
Pneumonia | 1.0 (0.0) | 2.4 |
Skin | ||
Rash | 1.3 (0.0) | 2.4 |
Urogenital | ||
Urinary Tract Infection | 1.3 (0.0) | 2.4 |
Other serious clinical adverse experiences occurring since the drug was marketed or adverse experiences occurring in 0.5 to 1.0 percent of patients with hypertension or heart failure in clinical trials are listed below and, within each category, are in order of decreasing severity.
Body As A Whole: Anaphylactoid reactions (see WARNINGS , Anaphylactoid and Possibly Related Reactions ).
Cardiovascular: Cardiac arrest; myocardial infarction or cerebrovascular accident, possibly secondary to excessive hypotension in high risk patients (see WARNINGS , Hypotension ); pulmonary embolism and infarction; pulmonary edema; rhythm disturbances including atrial tachycardia and bradycardia; atrial fibrillation; palpitation, Raynaud’s phenomenon.
Digestive: Ileus, pancreatitis, hepatic failure, hepatitis (hepatocellular [proven on rechallenge] or cholestatic jaundice) (see WARNINGS , Hepatic Failure ), melena, anorexia, dyspepsia, constipation, glossitis, stomatitis, dry mouth.
Hematologic: Rare cases of neutropenia, thrombocytopenia and bone marrow depression.
Musculoskeletal: Muscle cramps.
Nervous/Psychiatric: Depression, confusion, ataxia, somnolence, insomnia, nervousness, peripheral neuropathy (e.g., paresthesia, dysesthesia), dream abnormality.
Respiratory: Bronchospasm, rhinorrhea, sore throat and hoarseness, asthma, upper respiratory infection, pulmonary infiltrates, eosinophilic pneumonitis.
Skin: Exfoliative dermatitis, toxic epidermal necrolysis, Stevens-Johnson syndrome, pemphigus, herpes zoster, erythema multiforme, urticaria, pruritus, alopecia, flushing, diaphoresis, photosensitivity.
Special Senses: Blurred vision, taste alteration, anosmia, tinnitus, conjunctivitis, dry eyes, tearing.
Urogenital: Renal failure, oliguria, renal dysfunction (see PRECAUTIONS and DOSAGE AND ADMINISTRATION ), flank pain, gynecomastia, impotence.
Miscellaneous: A symptom complex has been reported which may include some or all of the following: a positive ANA, an elevated erythrocyte sedimentation rate, arthralgia/arthritis, myalgia/myositis, fever, serositis, vasculitis, leukocytosis, eosinophilia, photosensitivity, rash and other dermatologic manifestations.
Angioedema: Angioedema has been reported in patients receiving VASOTEC, with an incidence higher in black than in non-black patients. Angioedema associated with laryngeal edema may be fatal. If angioedema of the face, extremities, lips, tongue, glottis and/or larynx occurs, treatment with VASOTEC should be discontinued and appropriate therapy instituted immediately (see WARNINGS , Head and Neck Angioedema ).
Hypotension: In the hypertensive patients, hypotension occurred in 0.9 percent and syncope occurred in 0.5 percent of patients following the initial dose or during extended therapy. Hypotension or syncope was a cause for discontinuation of therapy in 0.1 percent of hypertensive patients. In heart failure patients, hypotension occurred in 6.7 percent and syncope occurred in 2.2 percent of patients. Hypotension or syncope was a cause for discontinuation of therapy in 1.9 percent of patients with heart failure (see WARNINGS , Hypotension ).
Cough: See PRECAUTIONS , Cough .
Pediatric Patients
The adverse experience profile for pediatric patients appears to be similar to that seen in adult patients.
Clinical Laboratory Test Findings
Serum Electrolytes
Hyperkalemia (see PRECAUTIONS , Hyperkalemia ), hyponatremia.
Creatinine, Blood Urea Nitrogen
In controlled clinical trials minor increases in blood urea nitrogen and serum creatinine, reversible upon discontinuation of therapy, were observed in about 0.2 percent of patients with essential hypertension treated with VASOTEC alone. Increases are more likely to occur in patients receiving concomitant diuretics or in patients with renal artery stenosis (see PRECAUTIONS , Impaired Renal Function ). In patients with heart failure who were also receiving diuretics with or without digitalis, increases in blood urea nitrogen or serum creatinine, usually reversible upon discontinuation of VASOTEC and/or other concomitant diuretic therapy, were observed in about 11 percent of patients. Increases in blood urea nitrogen or creatinine were a cause for discontinuation in 1.2 percent of patients.
Hematology
Small decreases in hemoglobin and hematocrit (mean decreases of approximately 0.3 g percent and 1.0 vol percent, respectively) occur frequently in either hypertension or congestive heart failure patients treated with VASOTEC but are rarely of clinical importance unless another cause of anemia coexists. In clinical trials, less than 0.1 percent of patients discontinued therapy due to anemia. Hemolytic anemia, including cases of hemolysis in patients with G6PD deficiency, has been reported; a causal relationship to enalapril cannot be excluded.
Liver Function Tests
Elevations of liver enzymes and/or serum bilirubin have occurred (see WARNINGS , Hepatic Failure ).
To report SUSPECTED ADVERSE REACTIONS, contact Bausch Health US, LLC at 1-800-321-4576 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Drug Interactions
Neprilysin Inhibitors
Patients taking concomitant neprilysin inhibitors may be at increased risk for angioedema (see WARNINGS ).
Dual Blockade of the Renin-Angiotensin System (RAS)
Dual blockade of the RAS with angiotensin receptor blockers, ACE inhibitors, or aliskiren is associated with increased risks of hypotension, hyperkalemia, and changes in renal function (including acute renal failure) compared to monotherapy. Most patients receiving the combination of two RAS inhibitors do not obtain any additional benefit compared to monotherapy. In general, avoid combined use of RAS inhibitors. Closely monitor blood pressure, renal function, and electrolytes in patients on VASOTEC and other agents that affect the RAS.
Do not coadminister aliskiren with VASOTEC in patients with diabetes. Avoid use of aliskiren with VASOTEC in patients with renal impairment (GFR <60 mL/min).
Hypotension — Patients on Diuretic Therapy
Patients on diuretics and especially those in whom diuretic therapy was recently instituted, may occasionally experience an excessive reduction of blood pressure after initiation of therapy with enalapril. The possibility of hypotensive effects with enalapril can be minimized by either discontinuing the diuretic or increasing the salt intake prior to initiation of treatment with enalapril. If it is necessary to continue the diuretic, provide close medical supervision after the initial dose for at least two hours and until blood pressure has stabilized for at least an additional hour (see WARNINGS , Hypotension and DOSAGE AND ADMINISTRATION ).
Agents Causing Renin Release
The antihypertensive effect of VASOTEC is augmented by antihypertensive agents that cause renin release (e.g., diuretics).
Nonsteroidal Anti-Inflammatory Agents Including Selective Cyclooxygenase-2 Inhibitors (COX-2 Inhibitors )
In patients who are elderly, volume-depleted (including those on diuretic therapy), or with compromised renal function, coadministration of NSAIDs, including selective COX-2 inhibitors, with ACE inhibitors, including enalapril, may result in deterioration of renal function, including possible acute renal failure. These effects are usually reversible. Monitor renal function periodically in patients receiving enalapril and NSAID therapy.
In a clinical pharmacology study, indomethacin or sulindac was administered to hypertensive patients receiving VASOTEC. In this study there was no evidence of a blunting of the antihypertensive action of VASOTEC. However, reports suggest that NSAIDs may diminish the antihypertensive effect of ACE inhibitors.
Other Cardiovascular Agents
VASOTEC has been used concomitantly with beta adrenergic-blocking agents, methyldopa, nitrates, calcium-blocking agents, hydralazine, prazosin and digoxin without evidence of clinically significant adverse interactions.
Agents Increasing Serum Potassium
VASOTEC attenuates potassium loss caused by thiazide-type diuretics. Potassium-sparing diuretics (e.g., spironolactone, triamterene, or amiloride), potassium supplements, or potassium-containing salt substitutes may lead to significant increases in serum potassium. Therefore, if concomitant use of these agents is indicated because of demonstrated hypokalemia, they should be used with caution and with frequent monitoring of serum potassium. Potassium-sparing agents should generally not be used in patients with heart failure receiving VASOTEC.
Lithium
Lithium toxicity has been reported in patients receiving lithium concomitantly with drugs which cause elimination of sodium, including ACE inhibitors. A few cases of lithium toxicity have been reported in patients receiving concomitant VASOTEC and lithium and were reversible upon discontinuation of both drugs. It is recommended that serum lithium levels be monitored frequently if enalapril is administered concomitantly with lithium.
Gold
Nitritoid reactions (symptoms include facial flushing, nausea, vomiting and hypotension) have been reported rarely in patients on therapy with injectable gold (sodium aurothiomalate) and concomitant ACE inhibitor therapy including VASOTEC.
mTOR (Mammalian Target of Rapamycin) Inhibitors
Patients receiving coadministration of ACE inhibitor and mTOR inhibitor (e.g., temsirolimus, sirolimus, everolimus) therapy may be at increased risk for angioedema (see WARNINGS , Head and Neck Angioedema ).
DESCRIPTION
VASOTEC ® (enalapril maleate) is the maleate salt of enalapril, the ethyl ester of a long-acting angiotensin-converting enzyme inhibitor, enalaprilat. Enalapril maleate is chemically described as (S)-1-[ N -[1-(ethoxycarbonyl)-3-phenylpropyl]-L-alanyl]-L-proline, (Z) -2-butenedioate salt (1:1). Its empirical formula is C 20 H 28 N 2 O 5 •C 4 H 4 O 4 , and its structural formula is:
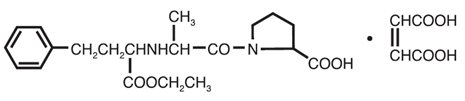
Enalapril maleate is a white to off-white, crystalline powder with a molecular weight of 492.53. It is sparingly soluble in water, soluble in ethanol, and freely soluble in methanol.
Enalapril is a pro-drug; following oral administration, it is bioactivated by hydrolysis of the ethyl ester to enalaprilat, which is the active angiotensin-converting enzyme inhibitor.
Enalapril maleate is supplied as 2.5 mg, 5 mg, 10 mg, and 20 mg tablets for oral administration. In addition to the active ingredient enalapril maleate, each tablet contains the following inactive ingredients: lactose, magnesium stearate, sodium bicarbonate, and starch. The 10 mg and 20 mg tablets also contain iron oxides.
CLINICAL PHARMACOLOGY
Mechanism of Action
Enalapril, after hydrolysis to enalaprilat, inhibits angiotensin-converting enzyme (ACE) in human subjects and animals. ACE is a peptidyl dipeptidase that catalyzes the conversion of angiotensin I to the vasoconstrictor substance, angiotensin II. Angiotensin II also stimulates aldosterone secretion by the adrenal cortex. The beneficial effects of enalapril in hypertension and heart failure appear to result primarily from suppression of the renin-angiotensin-aldosterone system. Inhibition of ACE results in decreased plasma angiotensin II, which leads to decreased vasopressor activity and to decreased aldosterone secretion. Although the latter decrease is small, it results in small increases of serum potassium. In hypertensive patients treated with VASOTEC alone for up to 48 weeks, mean increases in serum potassium of approximately 0.2 mEq/L were observed. In patients treated with VASOTEC plus a thiazide diuretic, there was essentially no change in serum potassium (see PRECAUTIONS ). Removal of angiotensin II negative feedback on renin secretion leads to increased plasma renin activity.
ACE is identical to kininase, an enzyme that degrades bradykinin. Whether increased levels of bradykinin, a potent vasodepressor peptide, play a role in the therapeutic effects of VASOTEC remains to be elucidated.
While the mechanism through which VASOTEC lowers blood pressure is believed to be primarily suppression of the renin-angiotensin-aldosterone system, VASOTEC is antihypertensive even in patients with low-renin hypertension. Although VASOTEC was antihypertensive in all races studied, black hypertensive patients (usually a low-renin hypertensive population) had a smaller average response to enalapril monotherapy than non-black patients.
Pharmacokinetics and Metabolism
Following oral administration of VASOTEC, peak serum concentrations of enalapril occur within about one hour. Based on urinary recovery, the extent of absorption of enalapril is approximately 60 percent. Enalapril absorption is not influenced by the presence of food in the gastrointestinal tract. Following absorption, enalapril is hydrolyzed to enalaprilat, which is a more potent angiotensin-converting enzyme inhibitor than enalapril; enalaprilat is poorly absorbed when administered orally. Peak serum concentrations of enalaprilat occur three to four hours after an oral dose of enalapril maleate. Excretion of VASOTEC is primarily renal. Approximately 94 percent of the dose is recovered in the urine and feces as enalaprilat or enalapril. The principal components in urine are enalaprilat, accounting for about 40 percent of the dose, and intact enalapril. There is no evidence of metabolites of enalapril, other than enalaprilat.
The serum concentration profile of enalaprilat exhibits a prolonged terminal phase, apparently representing a small fraction of the administered dose that has been bound to ACE. The amount bound does not increase with dose, indicating a saturable site of binding. The effective half-life for accumulation of enalaprilat following multiple doses of enalapril maleate is 11 hours. The disposition of enalapril and enalaprilat in patients with renal insufficiency is similar to that in patients with normal renal function until the glomerular filtration rate is 30 mL/min or less. With glomerular filtration rate ≤30 mL/min, peak and trough enalaprilat levels increase, time to peak concentration increases and time to steady state may be delayed. The effective half-life of enalaprilat following multiple doses of enalapril maleate is prolonged at this level of renal insufficiency (see DOSAGE AND ADMINISTRATION ). Enalaprilat is dialyzable at the rate of 62 mL/min.
Studies in dogs indicate that enalapril crosses the blood-brain barrier poorly, if at all; enalaprilat does not enter the brain. Multiple doses of enalapril maleate in rats do not result in accumulation in any tissues. Milk of lactating rats contains radioactivity following administration of 14 C-enalapril maleate. Radioactivity was found to cross the placenta following administration of labeled drug to pregnant hamsters.
Pharmacodynamics and Clinical Effects
Hypertension
Administration of VASOTEC to patients with hypertension of severity ranging from mild to severe results in a reduction of both supine and standing blood pressure usually with no orthostatic component. Symptomatic postural hypotension is therefore infrequent, although it might be anticipated in volume-depleted patients (see WARNINGS, Hypotension ).
In most patients studied, after oral administration of a single dose of enalapril, onset of antihypertensive activity was seen at one hour with peak reduction of blood pressure achieved by four to six hours.
At recommended doses, antihypertensive effects have been maintained for at least 24 hours. In some patients the effects may diminish toward the end of the dosing interval (see DOSAGE AND ADMINISTRATION , Hypertension ).
In some patients achievement of optimal blood pressure reduction may require several weeks of therapy.
The antihypertensive effects of VASOTEC have continued during long-term therapy. Abrupt withdrawal of VASOTEC has not been associated with a rapid increase in blood pressure.
In hemodynamic studies in patients with essential hypertension, blood pressure reduction was accompanied by a reduction in peripheral arterial resistance with an increase in cardiac output and little or no change in heart rate. Following administration of VASOTEC, there is an increase in renal blood flow; glomerular filtration rate is usually unchanged. The effects appear to be similar in patients with renovascular hypertension.
When given together with thiazide-type diuretics, the blood pressure lowering effects of VASOTEC are approximately additive.
In a clinical pharmacology study, indomethacin or sulindac was administered to hypertensive patients receiving VASOTEC. In this study there was no evidence of a blunting of the antihypertensive action of VASOTEC (see PRECAUTIONS , Drug Interactions ).
Heart Failure
In trials in patients treated with digitalis and diuretics, treatment with enalapril resulted in decreased systemic vascular resistance, blood pressure, pulmonary capillary wedge pressure and heart size, and increased cardiac output and exercise tolerance. Heart rate was unchanged or slightly reduced, and mean ejection fraction was unchanged or increased. There was a beneficial effect on severity of heart failure as measured by the New York Heart Association (NYHA) classification and on symptoms of dyspnea and fatigue. Hemodynamic effects were observed after the first dose and appeared to be maintained in uncontrolled studies lasting as long as four months. Effects on exercise tolerance, heart size, and severity and symptoms of heart failure were observed in placebo-controlled studies lasting from eight weeks to over one year.
Heart Failure, Mortality Trials
In a multicenter, placebo-controlled clinical trial, 2,569 patients with all degrees of symptomatic heart failure and ejection fraction ≤35 percent were randomized to placebo or enalapril and followed for up to 55 months (SOLVD-Treatment). Use of enalapril was associated with an 11 percent reduction in all-cause mortality and a 30 percent reduction in hospitalization for heart failure. Diseases that excluded patients from enrollment in the study included severe stable angina (>2 attacks/day), hemodynamically significant valvular or outflow tract obstruction, renal failure (creatinine >2.5 mg/dL), cerebrovascular disease (e.g., significant carotid artery disease), advanced pulmonary disease, malignancies, active myocarditis and constrictive pericarditis. The mortality benefit associated with enalapril does not appear to depend upon digitalis being present.
A second multicenter trial used the SOLVD protocol for study of asymptomatic or minimally symptomatic patients. SOLVD-Prevention patients, who had left ventricular ejection fraction ≤35% and no history of symptomatic heart failure, were randomized to placebo (n=2117) or enalapril (n=2111) and followed for up to 5 years. The majority of patients in the SOLVD-Prevention trial had a history of ischemic heart disease. A history of myocardial infarction was present in 80 percent of patients, current angina pectoris in 34 percent, and a history of hypertension in 37 percent. No statistically significant mortality effect was demonstrated in this population. Enalapril-treated subjects had 32% fewer first hospitalizations for heart failure, and 32% fewer total heart failure hospitalizations. Compared to placebo, 32 percent fewer patients receiving enalapril developed symptoms of overt heart failure. Hospitalizations for cardiovascular reasons were also reduced. There was an insignificant reduction in hospitalizations for any cause in the enalapril treatment group (for enalapril vs. placebo, respectively, 1166 vs. 1201 first hospitalizations, 2649 vs. 2840 total hospitalizations), although the study was not powered to look for such an effect.
The SOLVD-Prevention trial was not designed to determine whether treatment of asymptomatic patients with low ejection fraction would be superior, with respect to preventing hospitalization, to closer follow-up and use of enalapril at the earliest sign of heart failure. However, under the conditions of follow-up in the SOLVD-Prevention trial (every 4 months at the study clinic; personal physician as needed), 68% of patients on placebo who were hospitalized for heart failure had no prior symptoms recorded which would have signaled initiation of treatment.
The SOLVD-Prevention trial was also not designed to show whether enalapril modified the progression of underlying heart disease.
In another multicenter, placebo-controlled trial (CONSENSUS) limited to patients with NYHA Class IV congestive heart failure and radiographic evidence of cardiomegaly, use of enalapril was associated with improved survival. The results are shown in the following table.
| Survival (%) | ||
|---|---|---|
| Six Months | One Year | |
VASOTEC (n=127) | 74 | 64 |
Placebo (n=126) | 56 | 48 |
In both CONSENSUS and SOLVD-Treatment trials, patients were also usually receiving digitalis, diuretics or both.
Clinical Pharmacology in Pediatric Patients
A multiple dose pharmacokinetic study was conducted in 40 hypertensive male and female pediatric patients aged 2 months to ≤16 years following daily oral administration of 0.07 to 0.14 mg/kg enalapril maleate. At steady state, the mean effective half-life for accumulation of enalaprilat was 14 hours, and the mean urinary recovery of total enalapril and enalaprilat in 24 hours was 68% of the administered dose. Conversion of enalapril to enalaprilat was in the range of 63-76%. The overall results of this study indicate that the pharmacokinetics of enalapril in hypertensive children aged 2 months to ≤16 years are consistent across the studied age groups and consistent with pharmacokinetic historic data in healthy adults.
In a clinical study involving 110 hypertensive pediatric patients 6 to 16 years of age, patients who weighed <50 kg received either 0.625, 2.5 or 20 mg of enalapril daily and patients who weighed ≥50 kg received either 1.25, 5, or 40 mg of enalapril daily. Enalapril administered once daily lowered trough blood pressure in a dose-dependent manner. The dose-dependent antihypertensive efficacy of enalapril was consistent across all subgroups (age, Tanner stage, gender, race). However, the lowest doses studied, 0.625 mg and 1.25 mg, corresponding to an average of 0.02 mg/kg once daily, did not appear to offer consistent antihypertensive efficacy. In this study, VASOTEC was generally well tolerated.
In the above pediatric studies, enalapril maleate was given as tablets of VASOTEC and for those children and infants who were unable to swallow tablets or who required a lower dose than is available in tablet form, enalapril was administered in a suspension formulation (see DOSAGE AND ADMINISTRATION , Preparation of Suspension ).
HOW SUPPLIED
VASOTEC (enalapril maleate) Tablets | |||
NDC | Strength | Quantity | Description |
0187-0140-30 0187-0140-90 | 2.5 mg | Bottles of 30 (with desiccant) Bottles of 90 (with desiccant) | White, oval shaped tablet imprinted with “VASO 2.5” and scored on one side and scored on the other. |
0187-0141-30 0187-0141-90 | 5 mg | Bottles of 30 (with desiccant) Bottles of 90 (with desiccant) | White, rounded triangle shaped tablet imprinted with “VASO 5” on one side and scored on the other. |
0187-0142-30 0187-0142-90 0187-0142-10 | 10 mg | Bottles of 30 (with desiccant) Bottles of 90 (with desiccant) Bottles of 1,000 (with desiccant) | Rust red, rounded triangle shaped tablet imprinted with “VASO 10” on one side and scored on the other. |
0187-0143-30 0187-0143-90 0187-0143-10 | 20 mg | Bottles of 30 (with desiccant) Bottles of 90 (with desiccant) Bottles of 1,000 (with desiccant) | Peach, rounded triangle shaped tablet imprinted with “VASO 20” on one side and scored on the other. |
Storage
Store at 25°C (77°F); excursions permitted to 15° to 30°C (59° to 86°F) [see USP Controlled Room Temperature].
Keep container tightly closed.
Protect from moisture.
Dispense in a tight container as per USP, if product package is subdivided.
Mechanism of Action
Enalapril, after hydrolysis to enalaprilat, inhibits angiotensin-converting enzyme (ACE) in human subjects and animals. ACE is a peptidyl dipeptidase that catalyzes the conversion of angiotensin I to the vasoconstrictor substance, angiotensin II. Angiotensin II also stimulates aldosterone secretion by the adrenal cortex. The beneficial effects of enalapril in hypertension and heart failure appear to result primarily from suppression of the renin-angiotensin-aldosterone system. Inhibition of ACE results in decreased plasma angiotensin II, which leads to decreased vasopressor activity and to decreased aldosterone secretion. Although the latter decrease is small, it results in small increases of serum potassium. In hypertensive patients treated with VASOTEC alone for up to 48 weeks, mean increases in serum potassium of approximately 0.2 mEq/L were observed. In patients treated with VASOTEC plus a thiazide diuretic, there was essentially no change in serum potassium (see PRECAUTIONS ). Removal of angiotensin II negative feedback on renin secretion leads to increased plasma renin activity.
ACE is identical to kininase, an enzyme that degrades bradykinin. Whether increased levels of bradykinin, a potent vasodepressor peptide, play a role in the therapeutic effects of VASOTEC remains to be elucidated.
While the mechanism through which VASOTEC lowers blood pressure is believed to be primarily suppression of the renin-angiotensin-aldosterone system, VASOTEC is antihypertensive even in patients with low-renin hypertension. Although VASOTEC was antihypertensive in all races studied, black hypertensive patients (usually a low-renin hypertensive population) had a smaller average response to enalapril monotherapy than non-black patients.
Vasotec - Enalapril Maleate tablet PubMed™ news
- Journal Article • 2026 MayHypertensive retinopathy as a masquerade neuroretinitis in a child: a case report.
- Journal Article • 2026 MayThe endocrine product of renal (preglomerular) contractile pericytes depends on prolyl-4-hydroxylases 2 and 3.
- Journal Article • 2026 MayCardioprotective Effects of Prophylactic Angiotensin-Converting Enzyme Inhibitors in Anthracycline-Induced Cardiotoxicity: A Systematic Review and Meta-analysis of Randomized Trials.
- Journal Article • 2026 AprAdverse event of ACE inhibitors: A descriptive analysis of FAERS data.
- Journal Article • 2026 AprBiophysical and Raman Spectroscopy assessment of drug-induced photosensitivity: Insights from a randomised controlled pilot study.