Get your patient on Spironolactone And Hydrochlorothiazide - Spironolactone And Hydrochlorothiazide tablet (Spironolactone And Hydrochlorothiazide)
Spironolactone And Hydrochlorothiazide - Spironolactone And Hydrochlorothiazide tablet prescribing information
INDICATIONS AND USAGE
Spironolactone, an ingredient of spironolactone and hydrochlorothiazide tablets, has been shown to be a tumorigen in chronic toxicity studies in rats (see Precautions section). Spironolactone and hydrochlorothiazide tablets should be used only in those conditions described below. Unnecessary use of this drug should be avoided.
Spironolactone and hydrochlorothiazide tablets are indicated for:
Edematous conditions for patients with:
Congestive heart failure:
•For the management of edema and sodium retention when the patient is only partially responsive to, or is intolerant of, other therapeutic measures;
•The treatment of diuretic-induced hypokalemia in patients with congestive heart failure when other measures are considered inappropriate;
•The treatment of patients with congestive heart failure taking digitalis when other therapies are considered inadequate or inappropriate.
Cirrhosis of the liver accompanied by edema and/or ascites:
- Aldosterone levels may be exceptionally high in this condition. Spironolactone and hydrochlorothiazide tablets are indicated for maintenance therapy together with bed rest and the restriction of fluid and sodium.
The nephrotic syndrome:
- For nephrotic patients when treatment of the underlying disease, restriction of fluid and sodium intake, and the use of other diuretics do not provide an adequate response.
Essential hypertension:
•For patients with essential hypertension in whom other measures are considered inadequate or inappropriate;
•In hypertensive patients for the treatment of a diuretic-induced hypokalemia when other measures are considered inappropriate;
•Spironolactone and hydrochlorothiazide tablets are indicated for the treatment of hypertension, to lower blood pressure. Lowering blood pressure reduces the risk of fatal and nonfatal cardiovascular events, primarily strokes and myocardial infarctions. These benefits have been seen in controlled trials of antihypertensive drugs from a wide variety of pharmacologic classes, including the classes to which this drug principally belongs. There are no controlled trials demonstrating risk reduction with spironolactone and hydrochlorothiazide tablets.
Control of high blood pressure should be part of comprehensive cardiovascular risk management, including, as appropriate, lipid control, diabetes management, antithrombotic therapy, smoking cessation, exercise, and limited sodium intake. Many patients will require more than one drug to achieve blood pressure goals. For specific advice on goals and management, see published guidelines, such as those of the National High Blood Pressure Education Program's Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC).
Numerous antihypertensive drugs, from a variety of pharmacologic classes and with different mechanisms of action, have been shown in randomized controlled trials to reduce cardiovascular morbidity and mortality, and it can be concluded that it is blood pressure reduction, and not some other pharmacologic property of the drugs, that is largely responsible for those benefits. The largest and most consistent cardiovascular outcome benefit has been a reduction in the risk of stroke, but reductions in myocardial infarction and cardiovascular mortality also have been seen regularly.
Elevated systolic or diastolic pressure causes increased cardiovascular risk, and the absolute risk increase per mmHg is greater at higher blood pressures, so that even modest reductions of severe hypertension can provide substantial benefit. Relative risk reduction from blood pressure reduction is similar across populations with varying absolute risk, so the absolute benefit is greater in patients who are at higher risk independent of their hypertension (for example, patients with diabetes or hyperlipidemia), and such patients would be expected to benefit from more aggressive treatment to a lower blood pressure goal.
Some antihypertensive drugs have smaller blood pressure effects (as monotherapy) in black patients, and many antihypertensive drugs have additional approved indications and effects (e.g., on angina, heart failure, or diabetic kidney disease). These considerations may guide selection of therapy.
Usage in Pregnancy. The routine use of diuretics in an otherwise healthy woman is inappropriate and exposes mother and fetus to unnecessary hazard. Diuretics do not prevent development of toxemia of pregnancy, and there is no satisfactory evidence that they are useful in the treatment of developing toxemia.
Edema during pregnancy may arise from pathologic causes or from the physiologic and mechanical consequences of pregnancy. Spironolactone and hydrochlorothiazide tablets are indicated in pregnancy when edema is due to pathologic causes just as it is in the absence of pregnancy (however, see Precautions: Pregnancy ). Dependent edema in pregnancy, resulting from restriction of venous return by the expanded uterus, is properly treated through elevation of the lower extremities and use of support hose; use of diuretics to lower intravascular volume in this case is unsupported and unnecessary. There is hypervolemia during normal pregnancy which is not harmful to either the fetus or the mother (in the absence of cardiovascular disease), but which is associated with edema, including generalized edema, in the majority of pregnant women. If this edema produces discomfort, increased recumbency will often provide relief. In rare instances, this edema may cause extreme discomfort that is not relieved by rest. In these cases, a short course of diuretics may provide relief and may be appropriate.
DOSAGE AND ADMINISTRATION
Optimal dosage should be established by individual titration of the components.
Edema in adults (congestive heart failure, hepatic cirrhosis, or nephrotic syndrome). The usual maintenance dose of spironolactone and hydrochlorothiazide tablets is 100 mg each of spironolactone and hydrochlorothiazide daily, administered in a single dose or in divided doses, but may range from 25 mg to 200 mg of each component daily depending on the response to the initial titration. In some instances it may be desirable to administer separate tablets of either spironolactone or hydrochlorothiazide in addition to spironolactone and hydrochlorothiazide tablets in order to provide optimal individual therapy.
The onset of diuresis with spironolactone and hydrochlorothiazide tablets occurs promptly and, due to prolonged effect of the spironolactone component, persists for two to three days after spironolactone and hydrochlorothiazide tablets are discontinued.
Essential hypertension. Although the dosage will vary depending on the results of titration of the individual ingredients, many patients will be found to have an optimal response to 50 mg to 100 mg each of spironolactone and hydrochlorothiazide daily, given in a single dose or in divided doses.
Concurrent potassium supplementation is not recommended when spironolactone and hydrochlorothiazide tablets are used in the long-term management of hypertension or in the treatment of most edematous conditions, since the spironolactone content of spironolactone and hydrochlorothiazide tablets is usually sufficient to minimize loss induced by the hydrochlorothiazide component.
CONTRAINDICATIONS
Spironolactone and hydrochlorothiazide tablets are contraindicated in patients with anuria, acute renal insufficiency, significant impairment of renal excretory function, hypercalcemia, hyperkalemia, Addison's disease, and in patients who are allergic to thiazide diuretics or to other sulfonamide-derived drugs. Spironolactone and hydrochlorothiazide tablets may also be contraindicated in acute or severe hepatic failure.
ADVERSE REACTIONS
The following adverse reactions have been reported and, within each category (body system), are listed in order of decreasing severity.
Hydrochlorothiazide:
Body as a whole: Weakness.
Cardiovascular: Hypotension including orthostatic hypotension (may be aggravated by alcohol, barbiturates, narcotics, or antihypertensive drugs).
Digestive: Pancreatitis, jaundice (intrahepatic cholestatic jaundice), diarrhea, vomiting, sialoadenitis, cramping, constipation, gastric irritation, nausea, anorexia.
Eye Disorders: Acute myopia and acute angle-closure glaucoma (see Warnings ).
Hematologic: Aplastic anemia, agranulocytosis, leukopenia, hemolytic anemia, thrombocytopenia.
Hypersensitivity: Anaphylactic reactions, necrotizing angitis (vasculitis and cutaneous vasculitis), respiratory distress including pneumonitis and pulmonary edema, photosensitivity, fever, urticaria, rash, purpura.
Metabolic: Electrolyte imbalance (see Precautions ), hyperglycemia, glycosuria, hyperuricemia.
Musculoskeletal: Muscle spasm.
Nervous system/psychiatric: Vertigo, paresthesias, dizziness, headache, restlessness.
Renal: Renal failure, renal dysfunction, interstitial nephritis (see Warnings ).
Skin: Erythema multiforme, pruritus.
Special senses: Transient blurred vision, xanthopsia.
Spironolactone:
Digestive: Gastric bleeding, ulceration, gastritis, diarrhea and cramping, nausea, vomiting.
Reproductive: Gynecomastia (see Precautions ), inability to achieve or maintain erection, irregular menses or amenorrhea, postmenopausal bleeding, breast pain. Carcinoma of the breast has been reported in patients taking spironolactone but a cause and effect relationship has not been established.
Hematologic: Leukopenia (including agranulocytosis), thrombocytopenia.
Hypersensitivity: Fever, urticaria, maculopapular or erythematous cutaneous eruptions, anaphylactic reactions, vasculitis.
Metabolism: Hyperkalemia, electrolyte disturbances (see Warnings and Precautions ).
Musculoskeletal: Leg cramps.
Nervous system/psychiatric: Lethargy, mental confusion, ataxia, dizziness, headache, drowsiness.
Liver/biliary: A very few cases of mixed cholestatic/hepatocellular toxicity, with one reported fatality, have been reported with spironolactone administration.
Renal: Renal dysfunction (including renal failure).
Skin: Stevens-Johnson Syndrome (SJS), toxic epidermal necrolysis (TEN), drug rash with eosinophilia and systemic symptoms (DRESS), alopecia, pruritus.
Post Marketing Experience
Non-melanoma Skin Cancer: Hydrochlorothiazide is associated with an increased risk of non-melanoma skin cancer. In a study conducted in the Sentinel System, increased risk was predominantly for squamous cell carcinoma (SCC) and in white patients taking large cumulative doses. The increased risk for SCC in the overall population was approximately 1 additional case per 16,000 patients per year, and for white patients taking a cumulative dose of ≥50,000 mg the risk increase was approximately 1 additional SCC case for every 6,700 patients per year.
Drug interactions:
ACE inhibitors, Angiotensin II receptor antagonists, aldosterone blockers, potassium supplements, heparin, low molecular weight heparin, and other drugs known to cause hyperkalemia: Concomitant administration may lead to severe hyperkalemia.
Alcohol, barbiturates, or narcotics: Potentiation of orthostatic hypotension may occur.
Antidiabetic drugs (e.g., oral agents, insulin): Dosage adjustment of the antidiabetic drug may be required (see Precautions ).
Corticosteroids, ACTH: Intensified electrolyte depletion, particularly hypokalemia, may occur.
Pressor amines (e.g., norepinephrine): Both spironolactone and hydrochlorothiazide reduce the vascular responsiveness to norepinephrine. Therefore, caution should be exercised in the management of patients subjected to regional or general anesthesia while they are being treated with spironolactone and hydrochlorothiazide tablets.
Skeletal muscle relaxants, nondepolarizing (e.g., tubocurarine): Possible increased responsiveness to the muscle relaxant may result.
Lithium: Lithium generally should not be given with diuretics. Diuretic agents reduce the renal clearance of lithium and add a high risk of lithium toxicity.
Nonsteroidal anti-inflammatory drugs (NSAIDs): In some patients, the administration of an NSAID can reduce the diuretic, natriuretic, and antihypertensive effects of loop, potassium-sparing, and thiazide diuretics. Combination of NSAIDs, e.g., indomethacin, with potassium-sparing diuretics has been associated with severe hyperkalemia. Therefore, when spironolactone and hydrochlorothiazide tablets and NSAIDs are used concomitantly, the patient should be observed closely to determine if the desired effect of the diuretic is obtained.
Acetylsalicylic acid : Acetylsalicylic acid may reduce the efficacy of spironolactone. Therefore, when spironolactone and hydrochlorothiazide tablets and acetylsalicylic acid are used concomitantly, spironolactone and hydrochlorothiazide tablets may need to be titrated to higher maintenance dose and the patient should be observed closely to determine if the desired effect is obtained.
Digoxin: Spironolactone has been shown to increase the half-life of digoxin. This may result in increased serum digoxin levels and subsequent digitalis toxicity. Monitor serum digoxin levels and adjust dose accordingly. Thiazide-induced electrolyte disturbances, i.e. hypokalemia, hypomagnesemia, increase the risk of digoxin toxicity, which may lead to fatal arrhythmic events (see Precautions ).
Cholestyramine: Hyperkalemic metabolic acidosis has been reported in patients given spironolactone concurrently with cholestyramine
Abiraterone: Spironolactone binds to the androgen receptor and may increase prostate-specific antigen (PSA) levels in abiraterone-treated prostate cancer patients. Concomitant use of spironolactone is not recommended.
Mitotane : Avoid concomitant use of spironolactone and hydrochlorothiazide tablets and mitotane. Spironolactone reduces mitotane plasma levels. The effect of concomitant spironolactone on the pharmacokinetics of mitotane has not been studied; however, patients exhibited significantly lower mitotane levels compared to those who did not receive concomitant spironolactone despite receiving higher mitotane doses.
DESCRIPTION
Spironolactone and hydrochlorothiazide oral tablets contain:
Spironolactone, USP. . . . . . . . . . . . . . . . 25 mg
Hydrochlorothiazide, USP . . . . . . . . . . . . 25 mg
Spironolactone, an aldosterone antagonist, is 17-hydroxy-7α-mercapto-3-oxo-17α-pregn-4-ene-21-carboxylic acid γ-lactone acetate and has the following structural formula:
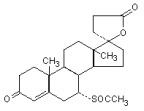
Spironolactone is practically insoluble in water, soluble in alcohol, and freely soluble in benzene and in chloroform.
Hydrochlorothiazide, a diuretic and antihypertensive, is 6-chloro-3,4-dihydro-2H-1,2,4-benzothiadiazine-7-sulfonamide 1,1-dioxide and has the following structural formula:
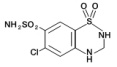
Hydrochlorothiazide is slightly soluble in water and freely soluble in sodium hydroxide solution.
Inactive ingredients include anhydrous lactose, colloidal silicon dioxide, D&C yellow #10 lake, docusate sodium, FD&C yellow #6 lake, magnesium stearate, microcrystalline cellulose, peppermint flavor, povidone, sodium benzoate, and sodium starch glycolate.
ACTIONS / CLINICAL PHARMACOLOGY
Mechanism of action: Spironolactone and hydrochlorothiazide tablets are a combination of two diuretic agents with different but complementary mechanisms and sites of action, thereby providing additive diuretic and antihypertensive effects. Additionally, the spironolactone component helps to minimize the potassium loss characteristically induced by the thiazide component.
The diuretic effect of spironolactone is mediated through its action as a specific pharmacologic antagonist of aldosterone, primarily by competitive binding of receptors at the aldosterone-dependent sodium-potassium exchange site in the distal convoluted renal tubule. Hydrochlorothiazide promotes the excretion of sodium and water primarily by inhibiting their reabsorption in the cortical diluting segment of the distal renal tubule.
Spironolactone and hydrochlorothiazide tablets are effective in significantly lowering the systolic and diastolic blood pressure in many patients with essential hypertension, even when aldosterone secretion is within normal limits.
Both spironolactone and hydrochlorothiazide reduce exchangeable sodium, plasma volume, body weight, and blood pressure. The diuretic and antihypertensive effects of the individual components are potentiated when spironolactone and hydrochlorothiazide are given concurrently.
Pharmacokinetics: Spironolactone is rapidly and extensively metabolized. Sulfur-containing products are the predominant metabolites and are thought to be primarily responsible, together with spironolactone, for the therapeutic effects of the drug. The following pharmacokinetic data were obtained from 12 healthy volunteers following the administration of 100 mg of spironolactone (as tablets) daily for 15 days. On the 15th day, spironolactone was given immediately after a low fat breakfast and blood was drawn thereafter.
Accumulation Factor: AUC (0–24 hr, day 15)/ AUC (0–24 hr, day 1) | Mean Peak Serum Concentration | Mean (SD) Post Steady-State Half-Life | |
7-α-(thiomethyl) spirolactone (TMS) | 1.25 | 391 ng/mL at 3.2 hr | 13.8 hr (6.4) (terminal) |
6-β-hydroxy-7-α-(thiomethyl) spirolactone (HTMS) | 1.50 | 125 ng/mL at 5.1 hr | 15 hr (4) (terminal) |
Canrenone (C) | 1.41 | 181 ng/mL at 4.3 hr | 16.5 hr (6.3) (terminal) |
Spironolactone | 1.30 | 80 ng/mL at 2.6 hr | Approximately 1.4 hr (0.5) (β half-life) |
The pharmacological activity of spironolactone metabolites in man is not known. However, in the adrenalectomized rat the antimineralocorticoid activities of the metabolites C, TMS, and HTMS, relative to spironolactone, were 1.10, 1.28, and 0.32, respectively. Relative to spironolactone, their binding affinities to the aldosterone receptors in rat kidney slices were 0.19, 0.86, and 0.06, respectively.
In humans, the potencies of TMS and 7-α-thiospirolactone in reversing the effects of the synthetic mineralocorticoid, fludrocortisone, on urinary electrolyte composition were 0.33 and 0.26, respectively, relative to spironolactone. However, since the serum concentrations of these steroids were not determined, their incomplete absorption and/or first-pass metabolism could not be ruled out as a reason for their reduced in vivo activities.
Spironolactone and its metabolites are more than 90% bound to plasma proteins. The metabolites are excreted primarily in the urine and secondarily in bile.
The effect of food on spironolactone absorption (two 100 mg spironolactone tablets) was assessed in a single dose study of 9 healthy, drug-free volunteers. Food increased the bioavailability of unmetabolized spironolactone by almost 100%. The clinical importance of this finding is not known.
Hydrochlorothiazide is rapidly absorbed following oral administration. Onset of action of hydrochlorothiazide is observed within one hour and persists for 6 to 12 hours. Hydrochlorothiazide plasma concentrations attain peak levels at one to two hours and decline with a half-life of four to five hours. Hydrochlorothiazide undergoes only slight metabolic alteration and is excreted in urine. It is distributed throughout the extracellular space, with essentially no tissue accumulation except in the kidney.
HOW SUPPLIED
Spironolactone and hydrochlorothiazide tablets, USP are supplied as follows:
Spironolactone and hydrochlorothiazide tablets, 25 mg/25 mg are buff, round, unscored, debossed MP 40.
Bottles of 100 | NDC 53489-144-01 |
Bottles of 500 | NDC 53489-144-05 |
Bottles of 1000 | NDC 53489-144-10 |
Store at 20° to 25°C (68° to 77°F).
[See USP Controlled Room Temperature]
DISPENSE IN TIGHT, LIGHT-RESISTANT CONTAINER.
Distributed by: Sun Pharmaceutical Industries, Inc. Cranbury, NJ 08512
Rev. 13, December 2025
Mechanism of action: Spironolactone and hydrochlorothiazide tablets are a combination of two diuretic agents with different but complementary mechanisms and sites of action, thereby providing additive diuretic and antihypertensive effects. Additionally, the spironolactone component helps to minimize the potassium loss characteristically induced by the thiazide component.
The diuretic effect of spironolactone is mediated through its action as a specific pharmacologic antagonist of aldosterone, primarily by competitive binding of receptors at the aldosterone-dependent sodium-potassium exchange site in the distal convoluted renal tubule. Hydrochlorothiazide promotes the excretion of sodium and water primarily by inhibiting their reabsorption in the cortical diluting segment of the distal renal tubule.
Spironolactone and hydrochlorothiazide tablets are effective in significantly lowering the systolic and diastolic blood pressure in many patients with essential hypertension, even when aldosterone secretion is within normal limits.
Both spironolactone and hydrochlorothiazide reduce exchangeable sodium, plasma volume, body weight, and blood pressure. The diuretic and antihypertensive effects of the individual components are potentiated when spironolactone and hydrochlorothiazide are given concurrently.