Get your patient on Sotyktu (Deucravacitinib)
Sotyktu prior authorization resources
Most recent state uniform prior authorization forms
Brand Resources
Sotyktu patient education
Patient toolkit
Dosage & administration
DOSAGE AND ADMINISTRATION
Recommended Evaluations and Immunizations Prior to Treatment Initiation
Evaluate patients for active and latent tuberculosis (TB) infection prior to initiating treatment with SOTYKTU. Do not administer SOTYKTU to patients with active TB. Start treatment for latent TB prior to initiation of SOTYKTU use [see Warnings and Precautions (5.3) ].
Complete all immunizations according to current immunization guidelines [see Warnings and Precautions (5.7) ] .
Recommended Dosage
The recommended dosage of SOTYKTU is 6 mg taken orally once daily, with or without food.
Do not crush, cut, or chew the tablets.
Recommended Dosage in Patients with Hepatic Impairment
SOTYKTU is not recommended in patients with severe hepatic impairment (Child-Pugh C) [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3) ].
No dosage adjustment is recommended for patients with mild (Child-Pugh A) or moderate (Child-Pugh B) hepatic impairment.

Sotyktu prescribing information
Indications and Usage, Psoriatic Arthritis (1.2 ) | 03/2026 |
INDICATIONS AND USAGE
SOTYKTU is a tyrosine kinase 2 (TYK2) inhibitor indicated for:
- the treatment of moderate-to-severe plaque psoriasis in adults who are candidates for systemic therapy or phototherapy. (1.1 )
Limitations of Use : Not recommended for use in combination with other potent immunosuppressants.
- the treatment of active psoriatic arthritis in adults. (1.2 )
Plaque Psoriasis
SOTYKTU is indicated for the treatment of moderate-to-severe plaque psoriasis in adults who are candidates for systemic therapy or phototherapy.
Limitations of Use :
SOTYKTU is not recommended for use in combination with other potent immunosuppressants.
Psoriatic Arthritis
SOTYKTU is indicated for the treatment of active psoriatic arthritis in adults.
DOSAGE AND ADMINISTRATION
Recommended Evaluations and Immunizations Prior to Treatment Initiation
Evaluate patients for active and latent tuberculosis (TB) infection prior to initiating treatment with SOTYKTU. Do not administer SOTYKTU to patients with active TB. Start treatment for latent TB prior to initiation of SOTYKTU use [see Warnings and Precautions (5.3) ].
Complete all immunizations according to current immunization guidelines [see Warnings and Precautions (5.7) ] .
Recommended Dosage
The recommended dosage of SOTYKTU is 6 mg taken orally once daily, with or without food.
Do not crush, cut, or chew the tablets.
Recommended Dosage in Patients with Hepatic Impairment
SOTYKTU is not recommended in patients with severe hepatic impairment (Child-Pugh C) [see Use in Specific Populations (8.7) and Clinical Pharmacology (12.3) ].
No dosage adjustment is recommended for patients with mild (Child-Pugh A) or moderate (Child-Pugh B) hepatic impairment.
DOSAGE FORMS AND STRENGTHS
Tablets: 6 mg of deucravacitinib, pink, round, biconvex, marked with “BMS 895” and “6 mg” on one side with no content on the other side.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary
Available data from case reports on SOTYKTU use during pregnancy are insufficient to evaluate a drug-associated risk of major birth defects, miscarriage, or adverse maternal or fetal outcomes.
In animal reproduction studies, no effects on embryo-fetal development were observed with oral administration of deucravacitinib to rats and rabbits during organogenesis at doses that were at least 72 times the maximum recommended human dose (MRHD) of 6 mg once daily (see Data ) .
All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. The background risk of major birth defects and miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Report pregnancies to the Bristol-Myers Squibb Company’s Adverse Event reporting line at 1-800-721-5072.
Data
Animal data
Deucravacitinib was administered orally during the period of organogenesis at doses of 5, 15, or 75 mg/kg/day in rats and 1, 3, or 10 mg/kg/day in rabbits. Deucravacitinib was not associated with embryo-fetal lethality or fetal malformations in either species. These doses resulted in maternal exposures (AUC) that were 211 times (rat) or 72 times (rabbit) the exposure at the MRHD.
In a pre- and post-natal development study in rats, deucravacitinib was administered orally from gestation day 6 through lactation day 20, at doses of 5, 15, or 50 mg/kg/day. At 50 mg/kg/day, F1 offspring had reduced body weight gains during the pre-weaning period. After weaning, body weights of affected F1 offspring gradually normalized to control levels. No maternal effects were observed at 50 mg/kg/day (87 times the MRHD based on AUC comparison). No deucravacitinib-related effects on postnatal developmental, neurobehavioral, or reproductive performance of offspring were noted at doses up to 15 mg/kg/day (15 times the MRHD based on AUC comparison).
Lactation
Risk Summary
There are no data on the presence of deucravacitinib in human milk, the effects on the breastfed infant, or the effects on milk production. Deucravacitinib is present in rat milk. When a drug is present in animal milk, it is likely that the drug will be present in human milk (see Data ). The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for SOTYKTU and any potential adverse effects on the breastfed infant from SOTYKTU or from the underlying maternal condition.
Data
Animal Data
A single oral dose of 5 mg/kg radiolabeled deucravacitinib was administered to lactating (post-partum days 8 to 12) rats. Deucravacitinib and/or its metabolites were present in the milk of lactating rats.
Pediatric Use
The safety and effectiveness of SOTYKTU in pediatric patients have not been established.
Geriatric Use
Plaque Psoriasis
In clinical trials of SOTYKTU in adults with moderate to severe plaque psoriasis, of the 1,519 subjects, 152 (10%) subjects were 65 years or older and 21 (1.4%) subjects were 75 years or older.
During the Week 0-16 period of the clinical trials 80 subjects ≥ 65 years old, including 12 subjects ≥ 75 years old, who received SOTYKTU without switching treatment arms, had a higher incidence of overall serious adverse reactions, including serious infections, and discontinuations due to adverse reactions compared with younger adult subjects.
No overall differences in effectiveness of SOTYKTU have been observed between patients 65 years of age and older and younger adult patients.
Psoriatic Arthritis
In clinical trials of SOTYKTU in adults with active psoriatric arthritis, of the 1312 subjects treated with SOTYKTU, 171 (13%) patients were 65 years or older and 22 (1.7%) subjects were 75 years or older. No overall differences safety or effectiveness of SOTYKTU or exposure of deucravacitinib were observed between subjects 65 years of age and older and younger adult subjects.
Renal Impairment
No dose adjustment of SOTYKTU is recommended in patients with mild, moderate, or severe renal impairment or in patients with end stage renal disease (ESRD) on dialysis [see Clinical Pharmacology (12.3) ] .
Hepatic Impairment
No dose adjustment of SOTYKTU is recommended in patients with mild (Child-Pugh A) or moderate (Child-Pugh B) hepatic impairment. SOTYKTU is not recommended for use in patients with severe hepatic impairment (Child-Pugh C) [see Adverse Reactions (6.1) and Clinical Pharmacology (12.3) ] .
CONTRAINDICATIONS
SOTYKTU is contraindicated in patients with a history of hypersensitivity reaction to deucravacitinib or to any of the excipients in SOTYKTU [see Warnings and Precautions (5.1) ] .
WARNINGS AND PRECAUTIONS
- Hypersensitivity Reactions: Hypersensitivity reactions, such as angioedema, have been reported. Discontinue if a clinically significant hypersensitivity reaction occurs. (5.1)
- Infections: SOTYKTU may increase the risk of infection. Avoid use in patients with active or serious infection. If a serious infection develops, discontinue SOTYKTU until the infection resolves. (5.2)
- Tuberculosis: Evaluate for latent or active TB prior to initiating treatment with SOTYKTU. (5.3)
- Malignancy: Malignancies including lymphomas were observed in clinical trials with SOTYKTU. Consider the benefits and risks prior to initiating or continuing SOTYKTU in patients with a malignancy. (5.4)
- Rhabdomyolysis and Elevated CPK: Discontinue SOTYKTU if markedly elevated CPK levels occur or myopathy is diagnosed or suspected . (5.5)
- Laboratory Abnormalities: Periodically evaluate serum triglycerides. Evaluate liver enzymes at baseline and during SOTYKTU treatment in patients with known or suspected liver disease. (5.6)
- Immunizations: Avoid use of SOTYKTU with live vaccines. (5.7)
- Potential Risks Related to JAK Inhibition: It is not known whether TYK2 inhibition may be associated with the observed or potential adverse reactions of JAK inhibition. Higher rates of all-cause mortality, including sudden cardiovascular death, major adverse cardiovascular events, overall thrombosis, deep venous thrombosis, pulmonary embolism, and malignancies (excluding non-melanoma skin cancer) were observed in patients treated with a JAK inhibitor compared to those treated with TNF blockers in patients with rheumatoid arthritis (RA). SOTYKTU is not approved for use in RA. (5.8)
Hypersensitivity Reactions
Hypersensitivity reactions, such as angioedema, have been reported in subjects receiving SOTYKTU. If a clinically significant hypersensitivity reaction occurs, institute appropriate therapy and discontinue SOTYKTU [see Contraindications (4) ].
Infections
SOTYKTU may increase the risk of infections.
Serious infections have been reported in subjects who received SOTYKTU. The most common serious infections reported with SOTYKTU included pneumonia and COVID-19 [see Adverse Reactions (6.1) ] .
Avoid use of SOTYKTU in patients with an active or serious infection.
Consider the risks and benefits of SOTYKTU prior to initiating treatment in patients:
- with chronic or recurrent infection
- who have been exposed to tuberculosis
- with a history of a serious or an opportunistic infection
- with underlying conditions that may predispose them to infection.
Closely monitor patients for the development of signs and symptoms of infection during and after treatment with SOTYKTU. Patients who develops a new infection during treatment with SOTYKTU should undergo prompt and complete diagnostic testing, have appropriate antimicrobial therapy be initiated, and be closely monitored. Interrupt SOTYKTU if a serious infection occurs. Do not resume SOTYKTU until the infection resolves or is adequately treated.
Viral Reactivation
Herpes virus reactivation (e.g., herpes zoster, herpes simplex) was reported in clinical trials with SOTYKTU [see Adverse Reactions (6.1) ] . In the 16‑week placebo-controlled period of Trials PSO-1 and PSO-2, herpes simplex infections were reported in 17 subjects (6.8 per 100 patient‑years) treated with SOTYKTU, and 1 subject (0.8 per 100 patient-years) treated with placebo. Multidermatomal herpes zoster was reported in an immunocompetent subject who received SOTYKTU.
The clinical implications of SOTYKTU on viral hepatitis reactivation are unknown. Subjects with positive screening tests for hepatitis B or C, or chronic hepatitis B, or untreated hepatitis C were excluded from clinical trials or closely monitored for evidence of reactivation. Consider viral hepatitis screening and monitoring for reactivation in accordance with clinical guidelines before starting therapy and during therapy with SOTYKTU. If signs of reactivation occur, consult a hepatitis specialist. SOTYKTU is not recommended for use in patients with active hepatitis B or hepatitis C.
Tuberculosis
In Trials PSO-1 and PSO-2, of 4 subjects with latent tuberculosis (TB) who were treated with SOTYKTU and received appropriate TB prophylaxis, no subjects developed active TB (during the mean follow-up of 34 weeks). One subject, who did not have latent TB, developed active TB after receiving 54 weeks of SOTYKTU.
Evaluate patients for latent and active TB infection prior to initiating treatment with SOTYKTU. Do not administer SOTYKTU to patients with active TB. Initiate treatment of latent TB prior to administering SOTYKTU.
Consider anti-TB therapy prior to initiation of SOTYKTU in patients with a past history of latent or active TB in whom an adequate course of treatment cannot be confirmed. Monitor patients receiving SOTYKTU for signs and symptoms of active TB during treatment.
Malignancy including Lymphomas
Malignancies, including lymphomas, were observed in clinical trials with SOTYKTU [see Adverse Reactions (6.1) ] .
Consider the benefits and risks for the individual patient prior to initiating or continuing therapy with SOTYKTU, particularly in patients with a known malignancy (other than a successfully treated non-melanoma skin cancer) and patients who develop a malignancy during treatment with SOTYKTU.
Rhabdomyolysis and Elevated CPK
Cases of rhabdomyolysis were reported in subjects treated with SOTYKTU resulting in interruption or discontinuation of SOTYKTU dosing.
Treatment with SOTYKTU was associated with an increased incidence of asymptomatic creatine phosphokinase (CPK) elevation and rhabdomyolysis compared to treatment with placebo. Discontinue SOTYKTU if markedly elevated CPK levels occur or myopathy is diagnosed or suspected. Instruct patients to promptly report any unexplained muscle pain, tenderness or weakness, particularly if accompanied by malaise or fever [see Adverse Reactions (6.1) ].
Laboratory Abnormalities
Triglyceride Elevations - Treatment with SOTYKTU was associated with increases in triglyceride levels [see Adverse Reactions (6.1) ] . The effect of this elevated parameter on cardiovascular morbidity and mortality has not been determined. Periodically evaluate serum triglycerides according to the clinical guidelines for hyperlipidemia while patients are receiving treatment with SOTYKTU. Manage patients according to clinical guidelines for the management of hyperlipidemia.
Liver Enzyme Elevations - Treatment with SOTYKTU has been associated with liver enzyme elevation. Liver serum transaminase elevations ≥3 times the ULN have been reported in subjects treated with SOTYKTU [see Adverse Reactions (6.1) ]. Evaluate liver enzymes at baseline and during treatment SOTYKTU in patients with known or suspected liver disease according to routine patient management. If increases in liver enzymes occur and drug-induced liver injury is suspected, interrupt SOTYKTU until a diagnosis of liver injury is excluded.
Immunizations
Prior to initiating therapy with SOTYKTU, complete all age-appropriate immunizations according to current immunization guidelines including prophylactic herpes zoster vaccination. Avoid use of live vaccines in patients treated with SOTYKTU. The response to live or non-live vaccines has not been evaluated.
Potential Risks Related to JAK Inhibition
It is not known whether TYK2 inhibition may be associated with the observed or potential adverse reactions of Janus Kinase (JAK) inhibition. In a large, randomized, postmarketing safety trial of a JAK inhibitor in rheumatoid arthritis (RA), patients 50 years of age and older with at least one cardiovascular risk factor, higher rates of all-cause mortality, including sudden cardiovascular death, major adverse cardiovascular events, overall thrombosis, deep venous thrombosis, pulmonary embolism, and malignancies (excluding non-melanoma skin cancer) were observed in patients treated with the JAK inhibitor compared to those treated with TNF blockers. SOTYKTU is not approved for use in RA.
ADVERSE REACTIONS
The following adverse reactions are discussed in greater detail in other sections of labeling:
- Infections [see Warnings and Precautions (5.2) ]
- Malignancy including Lymphomas [see Warnings and Precautions (5.4) ]
- Elevated CPK [see Warnings and Precautions (5.5) ]
- Laboratory Abnormalities [see Warnings and Precautions (5.6) ]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Plaque Psoriasis Clinical Trials
The safety of SOTYKTU was evaluated in two placebo- and active-controlled trials (Trial PSO-1 and Trial PSO-2) and an open-label extension trial in which subjects who completed Trial PSO-1 or Trial PSO-2 could enroll [see Clinical Studies (14.1) ]. In these clinical trials, a total of 1,519 subjects with moderate-to-severe plaque psoriasis who were candidates for systemic therapy or phototherapy received SOTYKTU 6 mg orally once daily. Of these, 1,141 subjects were exposed to SOTYKTU for at least one year.
In Trials PSO-1 and PSO-2, 1,681 subjects were randomized to receive SOTYKTU 6 mg once daily (840 subjects), placebo (419 subjects), or apremilast 30 mg twice daily (422 subjects). All subjects randomized to placebo switched to SOTYKTU at Week 16. All other subjects remained in their original treatment group until Week 24, at which point subjects could have continued on the same treatment or be switched to SOTYKTU or placebo. The mean age of subjects was 47 years. The majority of subjects were White (87%) and male (67%).
In the 16-week placebo-controlled period of the pooled clinical trials (Trials PSO-1 and PSO-2), discontinuation of therapy due to adverse reactions in subjects who received SOTYKTU was 2.4%, compared to 3.8% for placebo.
Table 1 summarizes the adverse reactions that occurred in at least 1% of subjects in the SOTYKTU group and at a higher rate than the placebo group during the 16-week controlled period.
| a Includes upper respiratory tract infection (viral, bacterial, and unspecified), nasopharyngitis, pharyngitis (including viral, streptococcal, and unspecified), sinusitis (includes acute, viral, bacterial), rhinitis, rhinotracheitis, tracheitis, laryngitis, and tonsillitis (including bacterial, streptococcal) b Includes oral herpes, genital herpes, herpes simplex, and herpes virus infection c Includes mouth ulceration, aphthous ulcer, tongue ulceration, and stomatitis d Includes acne, acne cystic, and dermatitis acneiform | ||
Adverse Reaction | SOTYKTU 6 mg once daily | Placebo |
N=840 n (%) | N=419 n (%) | |
Upper respiratory infections a | 161 (19.2) | 62 (14.8) |
Blood creatine phosphokinase increased | 23 (2.7) | 5 (1.2) |
Herpes simplex b | 17 (2) | 1 (0.2) |
Mouth ulcers c | 16 (1.9) | 0 (0.0) |
Folliculitis | 14 (1.7) | 0 (0.0) |
Acne d | 12 (1.4) | 1 (0.2) |
Adverse reactions that occurred in < 1% of subjects in the SOTYKTU group were herpes zoster.
Specific Adverse Reactions
Exposure adjusted incidence rates are reported for all the adverse reactions presented below.
Infections
In the 16-week placebo-controlled period, infections occurred in 29% of subjects in the SOTYKTU group (116 events per 100 patient-years) compared to 22% of subjects in the placebo group (83.7 events per 100 patient-years). The majority of infections were non-serious and mild to moderate in severity and did not lead to discontinuation of SOTYKTU.
In the 16-week placebo-controlled period, serious infections were reported in 5 subjects (2.0 per 100 patient-years) treated with SOTYKTU and 2 subjects (1.6 per 100 patient-years) treated with placebo.
The most common serious infections reported during the 52-week treatment period were pneumonia and COVID-19.
Malignancies
During the 0-to-52-week treatment period of the two clinical trials, Trial PSO-1 and PSO-2 (total exposure of 986 patient-years with SOTYKTU), malignancies (excluding non-melanoma skin cancer) were reported in 3 subjects treated with SOTYKTU (0.3 per 100 patient-years), including single cases each of breast cancer, hepatocellular carcinoma, and lymphoma after 24, 32, and 25 weeks of treatment, respectively.
During Trials PSO-1, PSO-2 and the open-label extension trial in which subjects who completed the controlled trials could enroll, a total of 3 subjects (0.1 per 100 patient-years) developed lymphoma while receiving SOTYKTU after 25, 77, and 98 weeks of treatment, respectively.
Laboratory Abnormalities
- Creatine Phosphokinase: In the 16-week placebo-controlled period, increased creatine phosphokinase (CPK) (including Grade 4) was reported in 23 subjects (9.3 per 100 patient-years) treated with SOTYKTU, and 5 subjects (4.1 per 100 patient-years) treated with placebo.
- Liver Enzyme Elevations: Events of increases in liver enzymes ≥3 times the ULN were observed in subjects treated with SOTYKTU [see Warnings and Precautions (5.5) ] . In the 16-week placebo-controlled period:
- ALT elevations ≥3 times the ULN was reported in 9 subjects (3.6 per 100 patient- years) treated with SOTYKTU, and 2 subjects (1.6 per 100 patient-years) treated with placebo.
- AST elevations ≥3 times the ULN was reported in 13 subjects (5.2 per 100 patient- years) treated with SOTYKTU, and 2 subjects (1.6 per 100 patient-years) treated with placebo.
- Decreased Glomerular Filtration Rate (GFR): In the 16-week placebo-controlled period in subjects who had moderate renal impairment (eGFR 30-59 mL/min) at baseline, decreased GFR was reported in 4 subjects (1.6 per 100 patient-years) treated with SOTYKTU, and 1 subject (0.8 per 100 patient-years) treated with placebo. Two of the SOTYKTU-treated subjects had worsening of baseline proteinuria.
- Lipid Elevations: Mean triglycerides increased by 10.3 mg/dL during the 16-week treatment period in subjects treated with SOTYKTU and by 9.1 mg/dL during the 52-week treatment period.
Safety Through Week 52
In Trials PSO-1 and PSO-2, the exposure adjusted incidence rate of adverse reactions in subjects treated with SOTYKTU from Week 0 through Week 52 without switching treatment did not increase compared to the rate observed during the first 16 weeks of treatment.
Psoriatic Arthritis Clinical Trials
The safety of SOTYKTU was evaluated in two placebo-controlled clinical trials in adults with active psoriatic arthritis, Trials PsA-1 and PsA-2 [see Clinical Studies (14.2) ] .
The overall safety profile of SOTYKTU observed in subjects with active psoriatic arthritis was generally consistent with the safety profile observed in subjects with plaque psoriasis.
DESCRIPTION
Deucravacitinib is a tyrosine kinase 2 (TYK2) inhibitor and is described chemically as:
6-(cyclopropanecarbonylamido)-4-[2-methoxy-3-(1-methyl-1,2,4-triazol-3-yl)anilino]-N-(trideuteriomethyl)pyridazine-3-carboxamide.
The molecular formula is C 20 H 19 D 3 N 8 O 3 and the molecular weight of the free base is 425.47. Deucravacitinib has the structural formula:

Deucravacitinib is a white to yellow powder. The solubility of deucravacitinib is pH dependent. Solubility decreases with increasing pH.
SOTYKTU (deucravacitinib) tablets are supplied in 6 mg strength for oral administration. Each tablet contains deucravacitinib as the active ingredient and the following inactive ingredients: anhydrous lactose, croscarmellose sodium, hypromellose acetate succinate, magnesium stearate, microcrystalline cellulose, and silicon dioxide. In addition, the film coating Opadry ® II Pink contains the following inactive ingredients: iron oxide red, iron oxide yellow, polyethylene glycol, polyvinyl alcohol, talc, and titanium dioxide.
CLINICAL PHARMACOLOGY
Mechanism of Action
Deucravacitinib is an inhibitor of tyrosine kinase 2 (TYK2). TYK2 is a member of the Janus kinase (JAK) family. Deucravacitinib binds to the regulatory domain of TYK2, stabilizing an inhibitory interaction between the regulatory and the catalytic domains of the enzyme. This results in allosteric inhibition of receptor-mediated activation of TYK2 and its downstream activation of Signal Transducers and Activators of Transcription (STATs) as shown in cell-based assays. JAK kinases, including TYK2, function as pairs of homo- or heterodimers in the JAK-STAT pathways. TYK2 pairs with JAK1 to mediate multiple cytokine pathways and also pairs with JAK2 to transmit signals as shown in cell-based assays. The precise mechanism linking inhibition of TYK2 enzyme to treatment of moderate-to-severe plaque psoriasis or active psoriatric arthritis is not currently known.
Pharmacodynamics
In patients with moderate to severe plaque psoriasis, deucravacitinib reduced psoriasis-associated gene expression in psoriatic skin in a dose dependent manner, including reductions in IL-23-pathway and type I IFN pathway regulated genes. In patients with moderate to severe plaque psoriasis and active psoriatic arthritis, deucravacitinib reduced circulating IL-17A, IL-19 and beta-defensin following 16 weeks of once daily treatment. In patients with active psoriatic arthritis, reduction in biomarkers including C-reactive protein (CRP), matrix metalloproteinase-3 (MMP3), matrix metalloproteinase-1 (MMP1), type I collagen degradation product (C1M) and TNF-alpha was also observed. The relationship between these pharmacodynamic markers and the mechanism(s) by which deucravacitinib exerts its clinical effects is unknown.
Cardiac Electrophysiology
At a dose 6 times the maximum recommended dose (6mg once daily), clinically significant QTc interval prolongation was not observed.
Pharmacokinetics
Following oral administration, deucravacitinib plasma C max and AUC increased proportionally over a dose range from 3 mg to 36 mg (0.5 to 6 times the approved recommended dosage) in healthy subjects. The accumulation of deucravacitinib was <1.4-fold following once daily dosing in healthy subjects. The pharmacokinetics of deucravacitinib and its active metabolite, BMT‑153261, were comparable between healthy subjects and subjects with plaque psoriasis.
The steady state C max and AUC 24 of deucravacitinib following administration of 6 mg once daily were 45 ng/mL and 473 ng·hr/mL respectively, in subjects with plaque psoriasis, and 53 ng/mL and 598 ng·hr/mL respectively, in subjects with psoriasis arthritis.
The steady state C max and AUC 24 of the active deucravacitinib metabolite, BMT-153261, following administration of 6 mg once daily were 5 ng/mL and 95 ng·hr/mL respectively, in subjects with plaque psoriasis subjects and 19 ng/mL and 209 ng·hr/mL respectively, in subjects with psoriasis arthritis subjects.
Absorption
The absolute oral bioavailability of deucravacitinib was 99% and the median T max ranged from 2 to 3 hours in healthy subjects.
Food Effect
No clinically significant differences in the pharmacokinetics of deucravacitinib were observed following administration of a high-fat, high-calorie meal (951 kcal in total, with approximate distribution of 52% fat, 33% carbohydrate and 15% protein). C max and AUC of deucravacitinib when administered with food were decreased by approximately 24% and 11%, respectively, and T max was prolonged by 1 hour. C max and AUC of BMT-153261 when administered with food were decreased by approximately 23% and 10%, respectively, and T max was prolonged by 2 hours.
Distribution
The volume of distribution of deucravacitinib at steady state is 140 L. Protein binding of deucravacitinib was 82 to 90% and the blood-to-plasma concentration ratio was 1.26.
Elimination
The terminal half-life of deucravacitinib was 10 hours. The renal clearance of deucravacitinib ranged from 27 to 54 mL/minute.
Metabolism
Deucravacitinib is metabolized by cytochrome P-450 (CYP) 1A2 to form major metabolite BMT-153261. Deucravacitinib is also metabolized by CYP2B6, CYP2D6, carboxylesterase (CES) 2, and uridine glucuronyl transferase (UGT) 1A9.
The active deucravacitinib metabolite, BMT-153261, has comparable potency to the parent drug, but the circulating exposure of BMT-153261 accounts for approximately 20% of the systemic exposure of the total drug-related components.
Excretion
After a single dose of radiolabeled deucravacitinib, approximately 13% and 26% of the dose was recovered as unchanged in urine and feces, respectively. Approximately 6% and 12% of the dose was detected as BMT-153261 in urine and feces, respectively.
Specific Populations
Patients with Renal Impairment
Deucravacitinib C max was 14% lower and 6% higher in patients with mild (eGFR ≥60 to <90 mL/min/1.73m 2 ) and moderate (eGFR ≥30 to <60 mL/min/1.73m 2 ) renal impairment, compared to subjects with normal renal function (eGFR ≥ 90 mL/min/1.73m 2 ); no change in C max was observed in patients with severe (eGFR <30 mL/min/1.73m 2 ) renal impairment, and end-stage renal disease (ESRD) (eGFR <15 mL/min/1.73m 2 ) on dialysis. Deucravacitinib AUC inf was unchanged in patients with mild renal impairment but higher by 39%, 28% and 34% in patients with moderate, severe and ESRD on dialysis, respectively, compared to subjects with normal renal function.
BMT-153261 C max was 11% lower, 8% lower, 28% higher and 9% higher in patients with mild, moderate, severe renal impairment and ESRD on dialysis, respectively, compared to subjects with normal renal function. BMT-153261 AUC inf was 2% lower, 24% higher, 81% higher and 27% higher in patients with mild, moderate, severe renal impairment and ESRD on dialysis, respectively, compared to subjects with normal renal function.
Dialysis did not substantially clear deucravacitinib from systemic circulation (5.4% of dose cleared per dialysis).
Patients with Hepatic Impairment
Deucravacitinib C max was higher by 4%, 10% and 1% in patients with mild (Child-Pugh Class A), moderate (Child-Pugh Class B), and severe (Child-Pugh Class C) hepatic impairment, respectively, compared to subjects with normal hepatic function. Deucravacitinib AUC inf was higher by 10%, 40% and 43% in patients with mild, moderate, and severe hepatic impairment, respectively, compared to subjects with normal hepatic function.
BMT-153261 C max was lower by 25%, 59% and 79% in patients with mild, moderate, and severe hepatic impairment, respectively, compared to subjects with normal hepatic function. BMT-153261 AUC inf was lower by 3%, 20% and 50% in patients with mild, moderate, and severe hepatic impairment, respectively, compared to subjects with normal hepatic function [see Use in Specific Populations (8.7) ] .
Body Weight, Gender, Race, and Age
Body weight, gender, race, and age did not have a clinically significant effect on deucravacitinib exposure.
Drug Interaction Studies
Clinical Trials
No clinically significant differences in the pharmacokinetics of deucravacitinib were observed when concomitantly administered with the following drugs: Cyclosporine (dual Pgp/BCRP inhibitor), fluvoxamine (CYP1A2 inhibitor), ritonavir (CYP1A2 inducer), diflunisal (UGT 1A9 inhibitor), pyrimethamine (OCT1 inhibitor), famotidine (H2 receptor antagonist), or rabeprazole (proton pump inhibitor).
No clinically significant differences in the pharmacokinetics of the following drugs were observed when concomitantly administered with deucravacitinib: Rosuvastatin, methotrexate, mycophenolate mofetil (MMF), metformin and oral contraceptives (norethindrone acetate and ethinyl estradiol).
In Vitro Studies
Cytochrome P450 (CYP) Enzymes: Deucravacitinib is not an inhibitor of CYP1A2, CYP2B6, CYP2C8, CYP2C9, CYP2C19, CYP2D6, or CYP3A4. Deucravacitinib is not an inducer of CYP1A2, CYP2B6, or CYP3A4.
Carboxylesterase (CES) Enzymes: Deucravacitinib is not an inhibitor of CES2.
Uridine diphosphate (UDP)-glucuronosyl transferase (UGT) Enzymes: Deucravacitinib is not an inhibitor of UGT1A1, UGT1A4, UGT1A6, UGT1A9, or UGT2B7.
Transporter Systems: Deucravacitinib is a substrate of Pgp, BCRP, and OCT1, but not OATP, NTCP, OAT1, OAT3, OCT2, MATE1, or MATE2K. Deucravacitinib is an inhibitor of BCRP and OATP1B3, but not an inhibitor of Pgp, OATP1B1, NTCP, BSEP, MRP2, OAT1, OAT3, OCT1, OCT2, MATE1, or MATE2-K.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
The carcinogenic potential of deucravacitinib was assessed in 2-year rat and 6-month rasH2 transgenic mouse studies. No evidence of tumorigenicity was observed in male or female rats that received deucravacitinib at oral doses up to 15 mg/kg/day (41 times the MRHD based on AUC comparison). No evidence of tumorigenicity was observed in male or female Tg.rasH2 mice that received deucravacitinib at oral doses up to 60 mg/kg/day.
Deucravacitinib was not mutagenic in a bacterial mutagenicity assay (Ames test) or clastogenic in an in vitro chromosomal aberration assay (cultured Chinese hamster ovary cells) or in an in vivo rat peripheral blood micronucleus assay.
In male rats, deucravacitinib had no effects on reproductive parameters (mating, fertility, and sperm morphology) or early embryonic development of their offspring at oral doses up to 50 mg/kg/day (178 times the MRHD based on AUC comparison).
In female rats, deucravacitinib had no effects on mating, fertility, or early embryonic parameters at oral doses up to 50 mg/kg/day (136 times the MRHD based on AUC comparison).
CLINICAL STUDIES
Plaque Psoriasis
The efficacy and safety of SOTYKTU were assessed in two multicenter, randomized, double-blind, placebo- and active-controlled clinical trials, Trial PSO-1 (NCT03624127) and Trial PSO-2 (NCT03611751) which enrolled subjects 18 years of age and older with moderate-to-severe plaque psoriasis who were eligible for systemic therapy or phototherapy. Subjects had a body surface area (BSA) involvement of ≥ 10%, a Psoriasis Area and Severity Index (PASI) score ≥ 12, and a static Physician’s Global Assessment (sPGA) ≥ 3 (moderate or severe).
In Trials PSO-1 and PSO-2, efficacy was assessed in 1,684 subjects randomized to either SOTYKTU (6 mg orally once daily), placebo, or apremilast (30 mg orally twice daily).
Endpoints
Both trials assessed responses at Week 16 compared to placebo for two co-primary endpoints:
- proportion of subjects who achieved a sPGA score of 0 (clear) or 1 (almost clear) with at least a 2-grade improvement from baseline;
- the proportion of subjects who achieved at least a 75% improvement in PASI scores from baseline (PASI 75).
Other comparisons between SOTYKTU and placebo that were secondary endpoints at Week 16:
- the proportion of subjects who achieved PASI 90, PASI 100, sPGA 0, scalp severity PGA (ss-PGA) score of 0 (clear) or 1 (almost clear) with at least 2-grade improvement, and Psoriasis Symptoms and Signs Diary (PSSD) Symptom Score of 0 (symptom-free).
Comparisons between SOTYKTU and apremilast were made for the following secondary endpoints and time points:
- at Week 16 and Week 24 (Trials PSO-1 and PSO-2), the proportion of subjects who achieved PASI 75, PASI 90, and sPGA 0/1 with at least a 2-grade improvement from baseline
- at Week 16 (Trials PSO-1 and PSO-2), the proportion of subjects who achieved sPGA 0 and ss-PGA 0/1 with at least a 2-grade improvement from baseline (scalp).
Baseline Characteristics
In both trials, the mean age was 47 years, the mean weight was 91 kg, 67% of subjects were male, 13% were Hispanic or Latino, 87% were White, 2% were Black, and 10% were Asian. At baseline, subjects had a median affected BSA of 20% and a median PASI score of 19. The proportion of subjects with sPGA score of 3 (moderate) and 4 (severe) at baseline were 80% and 20%, respectively. Approximately 18% of subjects had a history of psoriatic arthritis.
Across both trials, 40% of subjects had received prior phototherapy, 42% were naive to any systemic therapy (including biologic and/or non-biologic treatment), 41% received prior non-biologic systemic treatment, and 35% had received prior biologic therapy.
Results
Table 2 presents the efficacy results of SOTYKTU compared to apremilast and placebo in Trial PSO-1. Table 3 presents the efficacy results in Trial PSO-2.
| CI = Confidence interval; PASI = Psoriasis Area and Severity Index; sPGA = Static Physician Global Assessment; ss-PGA = Scalp Specific Physician’s Global Assessment a NRI = Non-Responder Imputation b Adjusted difference in proportions is the weighted average of the treatment differences across region, body weight and prior biologic use with the Cochran-Mantel-Haenszel weights. c Co-primary endpoints comparing SOTYKTU to placebo d Includes only subjects with baseline ss-PGA score of ≥ 3 | |||||
Endpoint | SOTYKTU (N=330) n (%) | Placebo (N=166) n (%) | Apremilast (N=168) n (%) | Difference, % (95% CI) b | |
Difference from Placebo | Difference from Apremilast | ||||
sPGA response of 0/1 (clear or almost clear) | |||||
Week 16 c | 178 (54) | 12 (7) | 54 (32) | 47 (40, 53) | 22 (13, 30) |
Week 24 | 194 (59) | 52 (31) | 27 (19, 36) | ||
sPGA response of 0 | |||||
Week 16 | 58 (18) | 1 (1) | 8 (5) | 17 (13, 21) | 13 (8, 18) |
PASI 75 response | |||||
Week 16 c | 193 (58) | 21 (13) | 59 (35) | 46 (39, 53) | 23 (14, 32) |
Week 24 | 228 (69) | 64 (38) | 31 (22, 40) | ||
PASI 90 response | |||||
Week 16 | 118 (36) | 7 (4) | 33 (20) | 32 (26, 38) | 16 (8, 24) |
Week 24 | 140 (42) | 37 (22) | 20 (12, 28) | ||
PASI 100 response | |||||
Week 16 | 47 (14) | 1 (1) | 14 (10, 18) | ||
ss-PGA response of 0/1 (scalp) d | (N=209) | (N=121) | (N=110) | ||
Week 16 | 147 (70) | 21 (17) | 43 (39) | 53 (44, 62) | 30 (19, 41) |
| CI = Confidence interval; PASI = Psoriasis Area and Severity Index; sPGA = Static Physician Global Assessment; ss-PGA = Scalp Specific Physician’s Global Assessment a NRI = Non-Responder Imputation b Adjusted difference in proportions is the weighted average of the treatment differences across region, body weight and prior biologic use with the Cochran-Mantel-Haenszel weights. c Co-primary endpoints comparing SOTYKTU to placebo d Includes only subjects with baseline ss-PGA score of ≥ 3 | |||||
Endpoint | SOTYKTU (N=511) n (%) | Placebo (N=255) n (%) | Apremilast (N=254) n (%) | Difference, % (95% CI) b | |
Difference from Placebo | Difference from Apremilast | ||||
sPGA response of 0/1 (clear or almost clear) | |||||
Week 16 c | 253 (50) | 22 (9) | 86 (34) | 41 (35, 46) | 16 (9, 23) |
Week 24 | 251 (49) | 75 (30) | 20 (13, 27) | ||
sPGA response of 0 | |||||
Week 16 | 80 (16) | 3 (1) | 16 (6) | 14 (11, 18) | 9 (5, 14) |
PASI 75 response | |||||
Week 16 c | 271 (53) | 24 (9) | 101 (40) | 44 (38, 49) | 13 (6, 21) |
Week 24 | 296 (58) | 96 (38) | 20 (13, 27) | ||
PASI 90 response | |||||
Week 16 | 138 (27) | 7 (3) | 46 (18) | 24 (20, 29) | 9 (3, 15) |
Week 24 | 164 (32) | 50 (20) | 13 (6, 19) | ||
PASI 100 response | |||||
Week 16 | 52 (10%) | 3 (1) | 9 (6, 12) | ||
ss-PGA response of 0/1 (scalp) d | (N=305) | (N=173) | (N=166) | ||
Week 16 | 182 (60) | 30 (17) | 61 (37) | 42 (34, 50) | 23 (14, 33) |
Examination of age, gender, race, body weight, baseline disease severity, and prior systemic therapy did not identify differences in response to SOTYKTU at Week 16 among these subgroups.
Maintenance and Durability of Response
In Trial PSO-1, among subjects who received SOTYKTU and had sPGA 0/1 response at Week 24, the sPGA 0/1 response at Week 52 was 78% (151/194). Among subjects who received SOTYKTU and had PASI 75 response at Week 24, the PASI 75 response at Week 52 was 82% (187/228). Among subjects who received SOTYKTU and had PASI 90 response at Week 24, the PASI 90 response at Week 52 was 74% (103/140).
In Trial PSO-2, to evaluate maintenance and durability of response, subjects who were originally randomized to SOTYKTU and were PASI 75 responders at Week 24, were re-randomized to either continue treatment on SOTYKTU or be withdrawn from therapy (i.e., receive placebo).
For subjects who were re-randomized and also had a sPGA score of 0 or 1 at Week 24, 70% (83/118) of subjects who continued on SOTYKTU maintained this response (sPGA 0 or 1) at Week 52 compared to 24% (28/119) of subjects who were re-randomized to placebo. In addition, at Week 52, 80% (119/148) of subjects who continued on SOTYKTU maintained PASI 75 compared to 31% (47/150) of subjects who were withdrawn from SOTYKTU.
For sPGA 0 or 1 responders at Week 24 who were re-randomized to treatment withdrawal (i.e., placebo), the median time to loss of sPGA score of 0 or 1 was approximately 8 weeks. For PASI 75 responders at Week 24 who were re-randomized to treatment withdrawal (i.e., placebo), the median time to loss of PASI 75 was approximately 12 weeks.
Patient Reported Outcomes
A greater proportion of subjects treated with SOTYKTU compared to placebo achieved Psoriasis Symptoms and Signs Diary (PSSD) symptom score of 0 (absence of itch, pain, burning, stinging, and skin tightness) at Week 16 (8% in SOTYKTU vs. 1% in placebo) in both trials.
Psoriatic Arthritis
The efficacy and safety of SOTYKTU were assessed in two multicenter randomized, double-blind, placebo-controlled trials (Trial PsA-1, [NCT04908202] and Trial PsA-2, [NCT04908189]) in subjects 18 years and older with active psoriatic arthritis (PsA) (≥3 swollen joints, ≥3 tender joints, a C-reactive protein (CRP) level of ≥3 mg/L) and with active or a history of plaque psoriasis. Subjects in both trials at baseline had a diagnosis of psoriatic arthritis for at least 3 months and met the Classification criteria for Psoriatic Arthritis (CASPAR) at screening. In Trial PsA-1, subjects also had presence of at least one bone erosion on X-ray of hands and/or feet. Trial PsA-2 included an active safety reference treatment arm (apremilast).
The efficacy of SOTYKTU was assessed in 1,294 subjects up to Week 16. Trial PsA-1 evaluated 670 subjects who were randomized to placebo or SOTYKTU 6 mg once daily. Trial PsA-2 evaluated 624 subjects who were randomized to placebo or SOTYKTU 6 mg once daily. In addition, 105 subjects were randomized to apremilast 30 mg twice daily in Trial PsA-2. In both trials, subjects randomized to placebo were switched to SOTYKTU at Week 16.
Baseline Characteristics
Across the two trials, the mean age was 51 years, the mean weight was 84 kg, 49% of subjects were male, 23% were Hispanic or Latino, 78% were White, and 0.4% were Black and 11% were Asian. In the two trials, subjects had a median duration of disease of 4.0 years and the majority of subjects had polyarthritis (76%) followed by oligoarthritis (14%). 8% of subjects had predominant distal interphalangeal joint involvement, while 16% had peripheral plus psoriatic spondylarthritis. Dactylitis and enthesitis were present in 31% and 49% of subjects respectively. 49% had psoriasis skin involvement that was ≥3% body surface area (BSA) and a Static Physician’s Global Assessment (sPGA) of at least 2.
In the two trials, the majority of subjects were naïve to biologic treatment and had experienced an inadequate response, intolerance or loss of response to nonsteroidal anti-inflammatory drugs (NSAIDs), conventional synthetic DMARDs (csDMARDs), or apremilast. In addition, Trial PsA-2 included anti-TNF alpha-experienced subjects. In the two trials, 56% of subjects were taking concomitant methotrexate (MTX). 10% were taking other concomitant csDMARDs, and 34% were not taking csDMARDs.
Endpoints and Results
The primary endpoint in both trials were the percentage of subjects who achieved an American College of Rheumatology (ACR) 20 response at Week 16.
ACR Response
In both trials, treatment with SOTYKTU resulted in statistically significant improvement in disease activity, as measured by ACR 20, compared to placebo at Week 16 (see Table 4). Improvement in disease activity was also demonstrated as measured by ACR 50/70 compared with placebo at Week 16. In both trials, ACR20 responses at Week 16 were consistent regardless of concomitant DMARD use, age, gender, race, or baseline disease characteristics in patients receiving SOTYKTU. In Trial PsA-2, similar ACR response rates were seen regardless of prior anti-TNF alpha therapy.
Trial PsA-1 | Trial PsA-2 | |||||
Endpoint | SOTYKTU (N = 336) | Placebo (N = 334) | Difference from Placebo (95% CI) | SOTYKTU (N = 312) | Placebo (N = 312) | Difference from Placebo (95% CI) |
ACR20 Response | ||||||
Week 16 (%) | 54 b | 34 | 20 (13, 27) | 54 b | 39 | 15 (7, 23) |
ACR50 Response | ||||||
Week 16 (%) | 25 | 14 | 11(5, 17) | 29 | 16 | 13 (6, 19) |
ACR70 Response | ||||||
Week 16 (%) | 12 | 5 | 6 (2, 10) | 11 | 5 | 5 (1, 9) |
ACR 20 [or 50 or 70]: American College of Rheumatology ≥20% (or ≥50% or ≥70%) improvement N is number of randomized subjects a NRI = Non-Responder Imputation b Multiplicity-controlled p≤0.0002, SOTYKTU vs. placebo comparison | ||||||
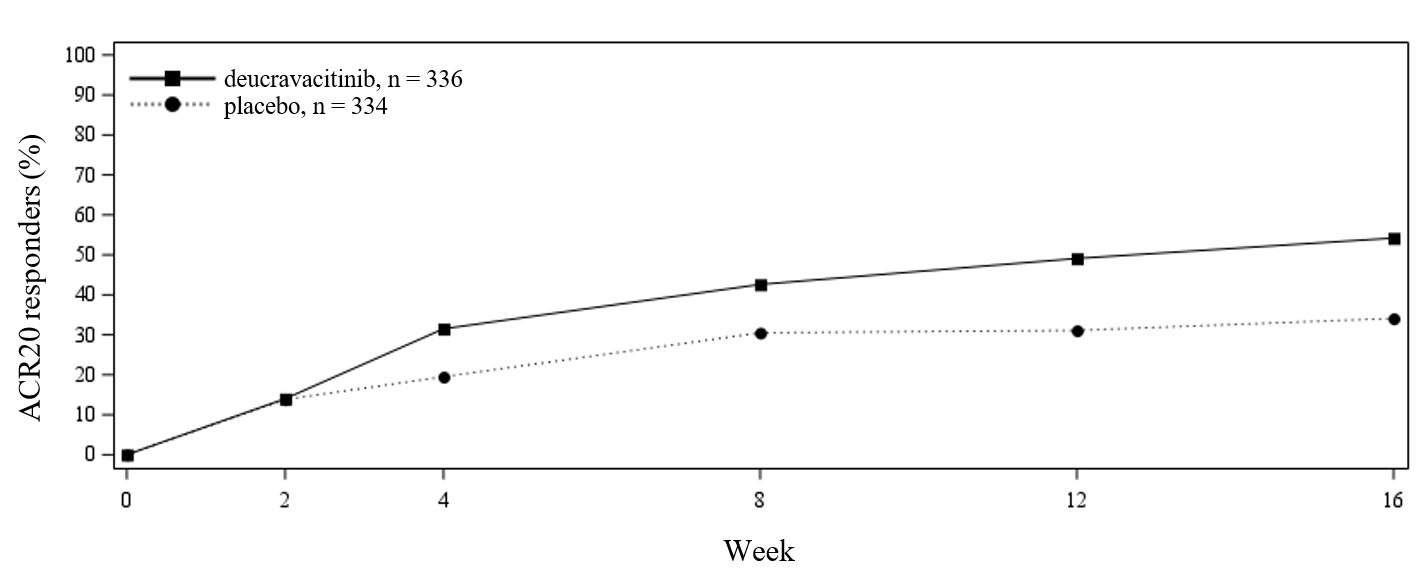
Improvements in ACR 20 and individual ACR components from baseline were observed in subjects treated with SOTYKTU at Week 16. The percentage of subjects achieving ACR20 responses in Trial PsA-1 by visit through Week 16 is shown in Figure 1. Similar responses were seen in Trial PsA-2 up to Week 16. Results of the components of the ACR response criteria for both trials are shown in Table 5.
Figure 1: Percent of Subjects Achieving ACR20 Responses in Trial PsA-1 through Week 16
Trial PsA–1 | Trial PsA–2 | |||
Placebo (N = 334) | SOTYKTU (N = 336) | Placebo (N = 312) | SOTYKTU (N = 312) | |
Number of Swollen Joints (0-66) | ||||
Baseline | 10.3 | 10.7 | 9.6 | 9.2 |
Mean change at Week 16 | -3.9 | -6.4 | -4 | -5.3 |
Number of Tender Joints (0-68) | ||||
Baseline | 19 | 19 | 16.6 | 15.2 |
Mean change at Week 16 | -6.5 | -9.2 | -5.8 | -8.1 |
Patient’s Assessment of Pain a (Pain VAS) | ||||
Baseline | 62.6 | 64.5 | 60.2 | 58.9 |
Mean change at Week 16 | -12.6 | -23.5 | -13.8 | -20.5 |
Physician’s Global Assessment (PGA) | ||||
Baseline | 62.5 | 62.3 | 60.1 | 59.7 |
Mean change at Week 16 | -18 | -30.4 | -21.5 | -29.8 |
Patient’s Global Assessment (PtGA) | ||||
Baseline | 63.4 | 63.6 | 61.2 | 58.7 |
Mean change at Week 16 | -13.4 | -22.1 | -13.5 | -20 |
Health Assessment Questionnaire – Disability index (HAQ-DI) b | ||||
Baseline | 1.3 | 1.4 | 1.2 | 1.1 |
Mean change at Week 16 | -0.2 | -0.4 | -0.2 | -0.3 |
High sensitivity C-Reactive Protein (hsCRP) (mg/L) | ||||
Baseline | 14.2 | 12.9 | 12.2 | 11.7 |
Mean change at Week 16 | -1.9 | -2.7 | -0.6 | -3.3 |
N is number of randomized subjects a Visual analog scale; 0=best, 100=worst (PGA/PtGA/pain) b Disability Index of the Health Assessment Questionnaire; 0 = no difficulty to 3 = inability to perform, measures the patient’s ability to perform the following: dressing, arising, eating, walking, hygiene, reaching, gripping, and activities of daily living. | ||||
In subjects with coexistent plaque psoriasis receiving SOTYKTU, statistically significant improvement was observed, relative to placebo, as measured by the Psoriasis Area Severity Index (PASI 75) at Week 16.
Physical Function Response
In both trials, subjects treated with SOTYKTU showed a statistically significant improvement from baseline in physical function as measured by the Health Assessment Questionnaire Disability Index (HAQ-DI) compared with placebo. The adjusted mean difference (95% CI) from placebo in HAQ-DI change from baseline at Week 16 was -0.17 (-0.24, -0.09) in Trial PsA-1 and -0.11 (-0.18, -0.04) in Trial PsA-2. The proportion of HAQ-DI responders (≥ 0.35 improvement from baseline) at Week 16 in Trial PsA-1 was 51% in the SOTYKTU group and 39% in the placebo group and in Trial PsA-2 was 49% in the SOTYKTU group and 43% in the placebo group.
Other Health-Related Outcomes
Health-related quality of life was assessed by the SF-36. Subjects treated with SOTYKTU showed improvements in SF-36 Physical Component Summary (PCS) score at Week 16 compared to placebo. There were also improvements in all four SF-36 (PCS) domain scale scores: physical functioning, role-physical, bodily-pain, and general health.
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
SOTYKTU™ (deucravacitinib) tablets are available as listed in the table below:
Tablet Strength | Tablet Color/Shape | Tablet Markings | Package Size | NDC Code |
6 mg | Pink, round, biconvex, film-coated tablet | Marked with “BMS 895” and “6 mg” on one side | Bottles of 30 with child-resistant closure | 0003-0895-11 |
Storage and Handling
Store SOTYKTU tablets at 20°C to 25°C (68°F to 77°F); excursions permitted between 15°C and 30°C (59°F and 86°F) [see USP Controlled Room Temperature].
Mechanism of Action
Deucravacitinib is an inhibitor of tyrosine kinase 2 (TYK2). TYK2 is a member of the Janus kinase (JAK) family. Deucravacitinib binds to the regulatory domain of TYK2, stabilizing an inhibitory interaction between the regulatory and the catalytic domains of the enzyme. This results in allosteric inhibition of receptor-mediated activation of TYK2 and its downstream activation of Signal Transducers and Activators of Transcription (STATs) as shown in cell-based assays. JAK kinases, including TYK2, function as pairs of homo- or heterodimers in the JAK-STAT pathways. TYK2 pairs with JAK1 to mediate multiple cytokine pathways and also pairs with JAK2 to transmit signals as shown in cell-based assays. The precise mechanism linking inhibition of TYK2 enzyme to treatment of moderate-to-severe plaque psoriasis or active psoriatric arthritis is not currently known.