Primaquine Phosphate - Primaquine Phosphate tablet, Film Coated prescribing information
INDICATIONS AND USAGE
Primaquine phosphate is indicated for the radical cure (prevention of relapse) of vivax malaria.
DOSAGE AND ADMINISTRATION
Primaquine phosphate tablets are recommended only for the radical cure of vivax malaria, the prevention of relapse in vivax malaria, or following the termination of chloroquine phosphate suppressive therapy in an area where vivax malaria is endemic. Patients suffering from an attack of vivax malaria or having parasitized red blood cells should receive a course of chloroquine phosphate, which quickly destroys the erythrocytic parasites and terminates the paroxysm. Primaquine phosphate tablets should be administered concurrently to eradicate the exoerythrocytic parasites in adults at a dosage of 1 tablet (equivalent to 15 mg base) daily for 14 days.
Primaquine phosphate tablets can be taken with or without food. Administration of primaquine phosphate tablets with food may reduce the incidence of gastrointestinal symptoms.
CONTRAINDICATIONS
Known hypersensitivity reactions to primaquine phosphate, other 8-aminoquinolones, or to any component in primaquine.
Severe glucose-6-phosphate dehydrogenase (G6PD) deficiency (see WARNINGS, Hemolytic Anemia ).
Pregnant women (see WARNINGS, Pregnancy ).
Breastfeeding by a lactating woman when the infant is found to be G6PD deficient or if G6PD status is unknown (see WARNINGS, Nursing Mothers ).
Because quinacrine hydrochloride appears to potentiate the toxicity of antimalarial compounds which are structurally related to primaquine, the use of quinacrine in patients receiving primaquine is contraindicated. Similarly, primaquine should not be administered to patients who have received quinacrine recently, as toxicity is increased.
ADVERSE REACTIONS
To report SUSPECTED ADVERSE REACTIONS, please call Ingenus Pharmaceuticals, LLC at 1-877-748-1970 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch
Gastrointestinal: Nausea, vomiting, epigastric distress, abdominal cramps.
Hematologic: Leukopenia, hemolytic anemia, decreased hemoglobin, methemoglobinemia.
Hemolytic anemia occurs commonly in patients with G6PD deficiency and may be severe or fatal in patients with severe G6PD deficiency (see WARNINGS ).
Methemoglobin levels are usually <10%, but methemoglobinemia may be severe in nicotinamide adenine dinucleotide (NADH) methemoglobin reductase deficient individuals or in patients with other risk factors (see PRECAUTIONS ).
Leukopenia was observed in patients with rheumatoid arthritis or lupus erythematosus (see PRECAUTIONS ).
Cardiac: Cardiac arrhythmia and QT interval prolongation (see PRECAUTIONS , OVERDOSAGE ).
Nervous System: Dizziness.
Skin and Soft Tissue: Rash, pruritus.
Drug Interactions
Pharmacodynamics Interactions
Quinacrine
Concurrent use of quinacrine (mepacrine) and primaquine are contraindicated. Increased toxicity was seen when quinacrine was used with pamaquine, another 8-aminoquinoline (see CONTRAINDICATIONS ).
Hemolytic Agents and Methemoglobinemia-Inducing Drugs
The concurrent administration of hemolytic agents or methemoglobinemia-inducing drugs and primaquine should be avoided (see PRECAUTIONS ). If the concurrent administration cannot be avoided, close blood monitoring is required.
QT Interval Prolonging Drugs
The pharmacodynamic interaction potential to prolong the QT interval of the electrocardiogram between primaquine and other drugs that effect cardiac conduction is unknown. If primaquine is used concomitantly with other drugs that prolong the QT interval, close and frequent electrocardiogram monitoring is advised (see PRECAUTIONS , ADVERSE REACTIONS , and OVERDOSAGE ).
Effects of Other Drugs on the Pharmacokinetics of Primaquine
Potent CYP2D6 Inhibitors
Published clinical and non-clinical reports indicate reduced CYP2D6 activity may decrease the formation of active metabolites of primaquine, which may reduce antimalarial efficacy of primaquine. Where possible, consider alternative medications that are not potent CYP2D6 inhibitors. If concurrent use with primaquine is necessary, increase monitoring for possible relapse.
Effects of Primaquine on the Pharmacokinetics of Other Drugs
CYP1A2 Substrates
Published clinical and non-clinical reports indicate primaquine inhibits CYP1A2 enzyme activity and thus may lead to increased exposure of CYP1A2 substrate drugs (e.g., duloxetine, alosetron, theophylline and tizanidine) when co-administered with primaquine. Since data are limited, no predictions can be made regarding the extent of the impact on CYP1A2 substrate drug exposures. Increase monitoring for adverse reactions associated with the CYP1A2 substrate drug when concurrently administered with primaquine.
P-gp Substrates with Narrow Therapeutic Index
In vitro observations suggest that primaquine inhibits the P-gp membrane transporter. Therefore, there is a potential for increased concentrations of drugs that are P-gp substrates when co-administered with primaquine. Increase monitoring for adverse reactions associated with narrow therapeutic index drugs that are P-gp substrates (e.g., digoxin and dabigatran) when concomitantly administered with primaquine.
DESCRIPTION
Primaquine phosphate is 8-[(4-amino-1-methylbutyl) amino]-6-methoxyquinoline phosphate, a synthetic compound with potent antimalarial activity. The molecular formula of primaquine phosphate is C 15 H 21 N 3 O·2H 3 PO 4 and its molecular weight is 455.34. The structural formula of primaquine phosphate is:
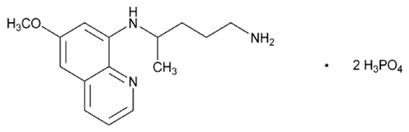
Figure 1: Primaquine phosphate structure.
Each Primaquine phosphate tablet, USP contains 26.3 mg of primaquine phosphate (equivalent to 15 mg of primaquine base). The dosage is customarily expressed in terms of the base.
Inactive Ingredients: Hypromellose, Lactose Monohydrate, Magnesium Stearate, Microcrystalline Cellulose, Triacetin, Pregelatinized Starch, FD&C Yellow#6/Sunset Yellow FCF Aluminum Lake, Talc, Titanium Dioxide.
CLINICAL PHARMACOLOGY
Microbiology
Mechanism of Action
Primaquine phosphate is an 8-aminoquinoline antimalarial drug. The mechanism of action has not been fully established. The major assumptions are an inhibition of the mitochondrial system of dormant parasites, and an oxidative stress generated through reactive metabolites in infected cells. In humans, primaquine phosphate activity is probably related to hydroxylated metabolites generated intrahepatically by CYP2D6.
Antimicrobial Activity
Primaquine phosphate is active against the dormant liver forms of P.vivax , namely hypnozoites, as well as exoerythrocytic stages of the parasite. Thereby, it prevents the development of the blood (erythrocytic) forms of the parasite which are responsible for relapses in vivax malaria. Primaquine phosphate is also active against gametocytes of Plasmodium falciparum .
Resistance
Development of resistance to primaquine phosphate in Plasmodium species has not been well studied.
Pharmacokinetics
Following single oral dosing, the C max and AUC of primaquine increase approximately dose-proportionally over a primaquine base dose range of 15 mg to 45 mg (3 times the approved dose).
The pharmacokinetic parameters and properties of primaquine and carboxyprimaquine (main circulating metabolite not expected to be active) in patients with P. vivax malaria following Oral Administration of primaquine are provided in TABLE 1.
| PK Parameter 15 mg once daily in adult patients (18 years of age and older) with P. vivax malaria, unless otherwise specified | Day | Primaquine | Carboxyprimaquine |
| C max (ng/mL) | 1 | 50.7 ± 21.2 | 291 ± 52 |
| C max (ng/mL) | 14 | 49.7 ± 14.4 | 432 ±112 |
| AUC or AUC 0-24 (μg/mL•h) AUC for primaquine, AUC 0-24 for carboxyprimaquine | 1 | 0.48 ± 0.26 | 5.15 ± 1.01 |
| AUC or AUC 0-24 (μg/mL•h) † | 14 | 0.49 ± 0.19 | 7.24 ± 1.82 |
| Primaquine | |||
| Absorption | |||
| Bioavailability Healthy participants | >70 % | ||
| T max | 2.3 ± 1.1 hours | ||
| Effect of food on primaquine (relative to fasting) Values refer to increase in mean systemic exposure with bread and butter: 82% fat, ~28g fat after single dose of 30 mg primaquine in healthy participants Geometric mean [95% confidence interval] | ↑ 14% [3, 27] (AUC); ↑ 26% [12, 40] (C max ) | ||
| Distribution | |||
| % Bound to human plasma proteins | 74% (mainly to alpha 1 acid glycoprotein) | ||
| Volume of distribution (V) IV dose administration of [ 14 C]-primaquine in healthy participants | 243 ± 69 L | ||
| Metabolism | |||
| Metabolic pathways | -Oxidative deamination, MAO-A -Hydroxylation of the quinoline ring, CYP2D6 -Direct conjugations | ||
| Elimination | |||
| Major route of elimination | Metabolism | ||
| Apparent Clearance (CL/F) | 37.6 ± 14.7 L/hr | ||
| Mean terminal half-life (t 1/2 ) The mean terminal half-life of carboxyprimaquine is approximately 22 hours | 5.6 ± 1.0 hours | ||
| % of dose excreted in urine The main circulating metabolite, carboxyprimaquine is subjected to further metabolism and not eliminated through urine , Oral administration of [ 14 C]-primaquine in healthy participants; no data in feces | 64%, (including 3.6% of primaquine, the remnant being metabolites other than carboxyprimaquine) | ||
| C max =maximum plasma concentration; AUC=area under the plasma concentration-time curve from time zero up to infinity; MAO-A = monoamine oxidase A | |||
Specific Populations
Gender and ethnicity
No gender nor ethnicity effect has been evidenced in studies conducted to date.
Elderly patients
There are no pharmacokinetics studies in patients older than 52 years of age.
Hepatic impairment
Single dose pharmacokinetics study performed in patients with mild or moderate hepatic impairment indicate that only moderate hepatic dysfunction impacted significantly the PK of primaquine with a 3-fold lower primaquine C max in patients with moderate hepatic dysfunction as compared to healthy subjects. The primaquine AUC was not significantly modified.
No data are available after repeated dosing in patients with hepatic impairment. It is not known whether in patients with hepatic impairment, accumulation of primaquine and its metabolites could occur or if there could be an impact on generation of metabolites contributing to pharmacological activity.
Renal impairment
Single dose pharmacokinetics studies performed in patients with chronic severe (eGFR 15 to 29 mL/min) or end-stage (< 15 mL/min) renal impairment indicate higher primaquine C max (up to 1.7-fold higher as compared to healthy subjects) but no evidence of major difference in AUC or t 1/2 . It is not known whether after repeated dosing there could be an accumulation of metabolites that are mainly excreted by renal route.
Drug Interaction Studies
Effect of other Drugs on the Pharmacokinetics of primaquine
In vitro data suggest primaquine is not a substrate of either P-gp or BCRP membrane transporters.
Effect of primaquine on the Pharmacokinetics of other drugs
In vitro data suggest primaquine has the potential to inhibit CYP1A2 enzyme activity, but no or low potential to inhibit MAO-A, MAO-B, or CYP450 isoforms 2A6, 2C8, 2C9, 2C19, 2D6, 3A4 enzymes involved in drug biotransformation.
In vitro data suggest primaquine has the potential to inhibit the P-gp membrane transporter.
Pharmacogenomics
Based on experiments in mice, primaquine activity probably depends on the formation of CYP2D6 metabolite(s). CYP2D6 polymorphism may be associated with variability in clinical response to primaquine.
CLINICAL STUDIES
Persons with acute attacks of vivax malaria, provoked by the release of erythrocytic forms of the parasite, respond readily to therapy, particularly to chloroquine phosphate. Primaquine eliminates tissue (exoerythrocytic) infection and prevents relapses in experimentally induced vivax malaria in human volunteers and in persons with naturally occurring infections and is a valuable adjunct to conventional therapy in vivax malaria.
HOW SUPPLIED
Primaquine phosphate tablets, USP are supplied as orange colored, round, biconvex, film-coated tablets of 26.3 mg (= 15 mg base), debossed with a "059" on one side and plain on the other side.
Available in bottles of 100 tablets (NDC 50742-191-01) and bottles of 500 tablets (NDC 50742-191-05)
Store at 25°C (77°F); excursions permitted to 15°C – 30°C (59°F – 86°F) [see USP Controlled Room Temperature]
Dispense in tight, light-resistant container as defined in the USP/NF.