Mexiletine Hydrochloride - Mexiletine Hydrochloride capsule prescribing information
BOXED WARNING WARNINGS
Mortality
In the National Heart, Lung and Blood Institute's Cardiac Arrhythmia Suppression Trial (CAST), a long-term, multicentered, randomized, double-blind study in patients with asymptomatic non-life-threatening ventricular arrhythmias who had a myocardial infarction more than six days but less than two years previously, an excessive mortality or non-fatal cardiac arrest rate (7.7%) was seen in patients treated with encainide or flecainide compared with that seen in patients assigned to carefully matched placebo-treated groups (3.0%). The average duration of treatment with encainide or flecainide in this study was ten months.
The applicability of the CAST results to other populations (e.g., those without recent myocardial infarction) is uncertain. Considering the known proarrhythmic properties of mexiletine and the lack of evidence of improved survival for any antiarrhythmic drug in patients without life-threatening arrhythmias, the use of mexiletine as well as other antiarrhythmic agents should be reserved for patients with life-threatening ventricular arrhythmia.
Acute Liver Injury
In postmarketing experience abnormal liver function tests have been reported, some in the first few weeks of therapy with mexiletine hydrochloride. Most of these have been observed in the setting of congestive heart failure or ischemia and their relationship to mexiletine hydrochloride has not been established.
INDICATIONS AND USAGE
Mexiletine hydrochloride capsules are indicated for the treatment of documented ventricular arrhythmias, such as sustained ventricular tachycardia, that, in the judgement of the physician, are life-threatening. Because of the proarrhythmic effects of mexiletine, its use with lesser arrhythmias is generally not recommended. Treatment of patients with asymptomatic ventricular premature contractions should be avoided.
Initiation of mexiletine treatment, as with other antiarrhythmic agents used to treat life-threatening arrhythmias, should be carried out in the hospital.
Antiarrhythmic drugs have not been shown to enhance survival in patients with ventricular arrhythmias.
DOSAGE AND ADMINISTRATION
The dosage of mexiletine hydrochloride must be individualized on the basis of response and tolerance, both of which are dose-related. Administration with food or antacid is recommended. Initiate mexiletine therapy with 200 mg every eight hours when rapid control of arrhythmia is not essential. A minimum of two to three days between dose adjustments is recommended. Dose may be adjusted in 50 or 100 mg increments up or down.
As with any antiarrhythmic drug, clinical and electrocardiographic evaluation (including Holter monitoring if necessary for evaluation) are needed to determine whether the desired antiarrhythmic effect has been obtained and to guide titration and dose adjustment.
Satisfactory control can be achieved in most patients by 200 to 300 mg given every eight hours with food or antacid. If satisfactory response has not been achieved at 300 mg q8h, and the patient tolerates mexiletine well, a dose of 400 mg q8h may be tried. As the severity of CNS side effects increases with total daily dose, the dose should not exceed 1,200 mg/day.
In general, patients with renal failure will require the usual doses of mexiletine hydrochloride. Patients with severe liver disease, however, may require lower doses and must be monitored closely. Similarly, marked right-sided congestive heart failure can reduce hepatic metabolism and reduce the needed dose. Plasma level may also be affected by certain concomitant drugs (see PRECAUTIONS: Drug Interactions).
Loading Dose
When rapid control of ventricular arrhythmia is essential, an initial loading dose of 400 mg of mexiletine hydrochloride may be administered, followed by a 200 mg dose in eight hours. Onset of therapeutic effect is usually observed within 30 minutes to two hours.
Some patients responding to mexiletine may be transferred to a 12-hour dosage schedule to improve convenience and compliance. If adequate suppression is achieved on a mexiletine hydrochloride dose of 300 mg or less every eight hours, the same total daily dose may be given in divided doses every 12 hours while carefully monitoring the degree of suppression of ventricular ectopy. This dose may be adjusted up to a maximum of 450 mg every 12 hours to achieve the desired response.
Transferring to Mexiletine Hydrochloride
The following dosage schedule, based on theoretical considerations rather than experimental data, is suggested for transferring patients from other Class I oral antiarrhythmic agents to mexiletine. Mexiletine hydrochloride treatment may be initiated with a 200 mg dose, and titrated to response as described above, 6-12 hours after the last dose of quinidine sulfate, 3-6 hours after the last dose of procainamide, 6-12 hours after the last dose of disopyramide or 8-12 hours after the last dose of tocainide.
In patients in whom withdrawal of the previous antiarrhythmic agent is likely to produce life-threatening arrhythmias, hospitalization of the patient is recommended.
When transferring from lidocaine to mexiletine, the lidocaine infusion should be stopped when the first oral dose of mexiletine hydrochloride is administered. The infusion line should be left open until suppression of the arrhythmia appears to be satisfactorily maintained. Consideration should be given to the similarity of the adverse effects of lidocaine and mexiletine and the possibility that they may be additive.
CONTRAINDICATIONS
Mexiletine hydrochloride capsules are contraindicated in the presence of cardiogenic shock or pre-existing second- or third-degree AV block (if no pacemaker is present).
WARNINGS
ADVERSE REACTIONS
Mexiletine hydrochloride commonly produces reversible gastrointestinal and nervous system adverse reactions but is otherwise well tolerated. Mexiletine has been evaluated in 483 patients in one-month and three-month controlled studies and in over 10,000 patients in a large compassionate use program. Dosages in the controlled studies ranged from 600-1,200 mg/day; some patients (8%) in the compassionate use program were treated with higher daily doses (1,600-3,200 mg/day). In the three-month controlled trials comparing mexiletine to quinidine, procainamide and disopyramide, the most frequent adverse reactions were upper gastrointestinal distress (41%), lightheadedness (10.5%), tremor (12.6%) and coordination difficulties (10.2%). Similar frequency and incidence were observed in the one-month placebo-controlled trial. Although these reactions were generally not serious, and were dose-related and reversible with a reduction in dosage, by taking the drug with food or antacid or by therapy discontinuation, they led to therapy discontinuation in 40% of patients in the controlled trials. Table 1 presents the adverse events reported in the one-month placebo-controlled trial.
Table 1 : Comparative Incidence (%) of Adverse Events Among Patients Treated with Mexiletine and Placebo in the 4-Week, Double-blind Crossover Trial
Mexiletine N=53 | Placebo N=49 | |
Cardiovascular | ||
Palpitations | 7.5 | 10.2 |
Chest Pain | 7.5 | 4.1 |
Increased Ventricular Arrhythmia /PVC's | 1.9 | |
Digestive | ||
Nausea/Vomiting/Heartburn | 39.6 | 6.1 |
Central Nervous System | ||
Dizziness/Lightheadedness | 26.4 | 14.3 |
Tremor | 13.2 | |
Nervousness | 11.3 | 6.1 |
Coordination Difficulties | 9.4 | |
Changes in Sleep Habits | 7.5 | 16.3 |
Paresthesias/Numbness | 3.8 | 2.0 |
Weakness | 1.9 | 4.1 |
Fatigue | 1.9 | 2.0 |
Tinnitus | 1.9 | 4.1 |
Confusion/Clouded Sensorium | 1.9 | 2.0 |
Other | ||
Headache | 7.5 | 6.1 |
Blurred Vision/Visual Disturbances | 7.5 | 2.0 |
Dyspnea/Respiratory | 5.7 | 10.2 |
Rash | 3.8 | 2.0 |
Non-specific Edema | 3.8 |
Table 2 presents the adverse reactions occurring in one percent or more of patients in the three-month controlled studies.
Table 2: Comparative Incidence (%) of Adverse Events Among Patients Treated with Mexiletine or Control Drugs in the 12-Week Double-blind Trials
Mexiletine N = 430 | Quinidine N = 262 | Procainamide N = 78 | Disopyramide N = 69 | |
Cardiovascular | ||||
Palpitations | 4.3 | 4.6 | 1.3 | 5.8 |
Chest Pain | 2.6 | 3.4 | 1.3 | 2.9 |
Angina/Angina-like Pain | 1.7 | 1.9 | 2.6 | 2.9 |
Increased Ventricular Arrhythmias/PVC's | 1.0 | 2.7 | 2.6 | |
Digestive | ||||
Nausea/Vomiting/Heartburn | 39.3 | 21.4 | 33.3 | 14.5 |
Diarrhea | 5.2 | 33.2 | 2.6 | 8.7 |
Constipation | 4.0 | 6.4 | 11.6 | |
Changes in Appetite | 2.6 | 1.9 | ||
Abdominal Pain/Cramps/Discomfort | 1.2 | 1.5 | 1.4 | |
Central Nervous System | ||||
Dizziness/Lightheadedness | 18.9 | 14.1 | 14.1 | 2.9 |
Tremor | 13.2 | 2.3 | 3.8 | 1.4 |
Coordination Difficulties | 9.7 | 1.1 | 1.3 | |
Changes in Sleep Habits | 7.1 | 2.7 | 11.5 | 8.7 |
Weakness | 5.0 | 5.3 | 7.7 | 2.9 |
Nervousness | 5.0 | 1.9 | 6.4 | 5.8 |
Fatigue | 3.8 | 5.7 | 5.1 | 1.4 |
Speech Difficulties | 2.6 | 0.4 | ||
Confusion/Clouded Sensorium | 2.6 | 3.8 | ||
Paresthesias/Numbness | 2.4 | 2.3 | 2.6 | |
Tinnitus | 2.4 | 1.5 | ||
Depression | 2.4 | 1.1 | 1.3 | 1.4 |
Other | ||||
Blurred Vision/Visual Disturbances | 5.7 | 3.1 | 5.1 | 7.2 |
Headache | 5.7 | 6.9 | 7.7 | 4.3 |
Rash | 4.2 | 3.8 | 10.3 | 1.4 |
Dyspnea/ Respiratory | 3.3 | 3.1 | 5.1 | 2.9 |
Dry Mouth | 2.8 | 1.9 | 5.1 | 14.5 |
Arthralgia | 1.7 | 2.3 | 5.1 | 1.4 |
Fever | 1.2 | 3.1 | 2.6 |
Less than 1%: Syncope, edema, hot flashes, hypertension, short-term memory loss, loss of consciousness, other psychological changes, diaphoresis, urinary hesitancy/retention, malaise, impotence/decreased libido, pharyngitis, congestive heart failure.
An additional group of over 10,000 patients has been treated in a program allowing administration of mexiletine hydrochloride under compassionate use circumstances. These patients were seriously ill with the large majority on multiple drug therapy. Twenty-four percent of the patients continued in the program for one year or longer. Adverse reactions leading to therapy discontinuation occurred in 15 percent of patients (usually upper gastrointestinal system or nervous system effects). In general, the more common adverse reactions were similar to those in the controlled trials. Less common adverse events possibly related to mexiletine use include:
Syncope and hypotension, each about 6 in 1,000; bradycardia, about 4 in 1,000; angina/angina-like pain, about 3 in 1,000; edema, atrioventricular block/conduction disturbances and hot flashes, each about 2 in 1,000; atrial arrhythmias, hypertension and cardiogenic shock, each about 1 in 1,000.
Short-term memory loss, about 9 in 1,000 patients; hallucinations and other psychological changes, each about 3 in 1,000; psychosis and convulsions/seizures, each about 2 in 1,000; loss of consciousness, about 6 in 10,000.
Dysphagia, about 2 in 1,000; peptic ulcer, about 8 in 10,000; upper gastrointestinal bleeding, about 7 in 10,000; esophageal ulceration, about 1 in 10,000. Rare cases of severe hepatitis/acute hepatic necrosis.
Rare cases of exfoliative dermatitis and Stevens-Johnson Syndrome with mexiletine treatment have been reported.
Abnormal liver function tests, about 5 in 1,000 patients; positive ANA and thrombocytopenia, each about 2 in 1,000; leukopenia (including neutropenia and agranulocytosis), about 1 in 1,000; myelofibrosis, about 2 in 10,000 patients.
Diaphoresis, about 6 in 1,000; altered taste, about 5 in 1,000; salivary changes, hair loss and impotence/decreased libido, each about 4 in 1,000; malaise, about 3 in 1,000; urinary hesitancy/retention, each about 2 in 1,000; hiccups, dry skin, laryngeal and pharyngeal changes and changes in oral mucous membranes, each about 1 in 1,000; SLE syndrome, about 4 in 10,000.
Blood dyscrasias were not seen in the controlled trials but did occur among 10,867 patients treated with mexiletine in the compassionate use program (see PRECAUTIONS ).
Myelofibrosis was reported in two patients in the compassionate use program: one was receiving long-term thiotepa therapy and the other had pretreatment myeloid abnormalities.
In postmarketing experience, there have been isolated, spontaneous reports of pulmonary changes including pulmonary infiltration and pulmonary fibrosis during mexiletine therapy with or without other drugs or diseases that are known to produce pulmonary toxicity. A causal relationship to mexiletine therapy has not been established. In addition, there have been isolated reports of drowsiness, nystagmus, ataxia, dyspepsia, hypersensitivity reaction, and exacerbation of congestive heart failure in patients with pre-existing compromised ventricular function. There have been rare reports of pancreatitis associated with mexiletine treatment.
DESCRIPTION
Mexiletine hydrochloride, USP is an orally active antiarrhythmic agent. It is a white to off-white crystalline powder with slightly bitter taste, freely soluble in water and in alcohol. Mexiletine hydrochloride, USP has a pKa of 9.2. The chemical name of mexiletine hydrochloride, USP is 1-methyl-2-(2,6-xylyloxy)ethylamine hydrochloride and its structural formula is:
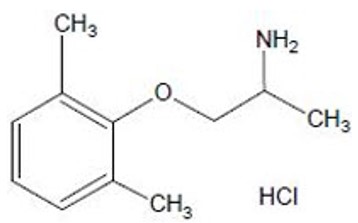
C 11 H 17 NO·HCl Mol. Wt. 215.72
Each capsule for oral administration, contains 250 mg of mexiletine hydrochloride, USP. 100 mg of mexiletine hydrochloride, USP is equivalent to 83.31 mg of mexiletine base. In addition, each capsule contains the following excipients: colloidal silicon dioxide, magnesium stearate and pregelatinized corn starch. The capsule shell contains: FD&C Yellow #6, gelatin, titanium dioxide, FD&C Blue #1 and D&C Yellow #10. The imprinting ink contains: ammonium hydroxide, black iron oxide, propylene glycol and shellac.
CLINICAL PHARMACOLOGY
Mechanism of Action
Mexiletine hydrochloride is a local anesthetic, antiarrhythmic agent, structurally similar to lidocaine, but orally active. In animal studies, mexiletine has been shown to be effective in the suppression of induced ventricular arrhythmias, including those induced by glycoside toxicity and coronary artery ligation. Mexiletine, like lidocaine, inhibits the inward sodium current, thus reducing the rate of rise of the action potential, Phase 0. Mexiletine decreased the effective refractory period (ERP) in Purkinje fibers. The decrease in ERP was of lesser magnitude than the decrease in action potential duration (APD), with a resulting increase in the ERP/APD ratio.
Electrophysiology in Man
Mexiletine is a Class 1B antiarrhythmic compound with electrophysiologic properties in man similar to those of lidocaine, but dissimilar from quinidine, procainamide, and disopyramide.
In patients with normal conduction systems, mexiletine has a minimal effect on cardiac impulse generation and propagation. In clinical trials, no development of second-degree or third-degree AV block was observed. Mexiletine did not prolong ventricular depolarization (QRS duration) or repolarization (QT intervals) as measured by electrocardiography. Theoretically, therefore, mexiletine may be useful in the treatment of ventricular arrhythmias associated with a prolonged QT interval.
In patients with pre-existing conduction defects, depression of the sinus rate, prolongation of sinus node recovery time, decreased conduction velocity and increased effective refractory period of the intraventricular conduction system have occasionally been observed.
The antiarrhythmic effect of mexiletine has been established in controlled comparative trials against placebo, quinidine, procainamide and disopyramide. Mexiletine hydrochloride, at doses of 200-400 mg q8h, produced a significant reduction of ventricular premature beats, paired beats, and episodes of non-sustained ventricular tachycardia compared to placebo and was similar in effectiveness to the active agents. Among all patients entered into the studies, about 30% in each treatment group had a 70% or greater reduction in PVC count and about 40% failed to complete the 3-month studies because of adverse effects. Follow-up of patients from the controlled trials has demonstrated continued effectiveness of mexiletine in long-term use.
Hemodynamics
Hemodynamic studies in a limited number of patients, with normal or abnormal myocardial function, following oral administration of mexiletine hydrochloride, have shown small, usually not statistically significant, decreases in cardiac output and increases in systemic vascular resistance, but no significant negative inotropic effect. Blood pressure and pulse rate remain essentially unchanged. Mild depression of myocardial function, similar to that produced by lidocaine, has occasionally been observed following intravenous mexiletine therapy in patients with cardiac disease.
Pharmacokinetics
Mexiletine is well absorbed (~90%) from the gastrointestinal tract. Unlike lidocaine, its first-pass metabolism is low. Peak blood levels are reached in two to three hours. In normal subjects, the plasma elimination half-life of mexiletine is approximately 10-12 hours. It is 50-60% bound to plasma protein, with a volume of distribution of 5-7 liters/kg. Mexiletine is mainly metabolized in the liver, the primary pathway being CYP2D6 metabolism, although it is also a substrate for CYP1A2. With involvement of CYP2D6, there can be either poor or extensive metabolizer phenotypes. Since approximately 90% of mexiletine hydrochloride is metabolized in the liver into inactive metabolites, pathological changes in the liver can restrict hepatic clearance of mexiletine hydrochloride and its metabolites. The metabolic degradation proceeds via various pathways including aromatic and aliphatic hydroxylation, dealkylation, deamination and N-oxidation. Several of the resulting metabolites are submitted to further conjugation with glucuronic acid (phase II metabolism); among these are the major metabolites p-hydroxymexiletine, hydroxy-methylmexiletine and N-hydroxy-mexiletine. Approximately 10% is excreted unchanged by the kidney. While urinary pH does not normally have much influence on elimination, marked changes in urinary pH influence the rate of excretion: acidification accelerates excretion, while alkalinization retards it.
Several metabolites of mexiletine have shown minimal antiarrhythmic activity in animal models. The most active is the minor metabolite N-methylmexiletine, which is less than 20% as potent as mexiletine. The urinary excretion of N-methylmexiletine in man is less than 0.5%. Thus, the therapeutic activity of mexiletine is due to the parent compound.
Hepatic impairment prolongs the elimination half-life of mexiletine. In eight patients with moderate to severe liver disease, the mean half-life was approximately 25 hours.
Consistent with the limited renal elimination of mexiletine, little change in the half-life has been detected in patients with reduced renal function. In eight patients with creatinine clearance less than 10 mL/min, the mean plasma elimination half-life was 15.7 hours; in seven patients with creatinine clearance between 11-40 mL/min, the mean half-life was 13.4 hours.
The absorption rate of mexiletine is reduced in clinical situations such as acute myocardial infarction in which gastric emptying time is increased. Narcotics, atropine and magnesium-aluminum hydroxide have also been reported to slow the absorption of mexiletine. Metoclopramide has been reported to accelerate absorption.
Mexiletine plasma levels of at least 0.5 mcg/mL are generally required for therapeutic response. An increase in the frequency of central nervous system adverse effects has been observed when plasma levels exceed 2 mcg/mL. Thus, the therapeutic range is approximately 0.5 to 2 mcg/mL. Plasma levels within the therapeutic range can be attained with either three times daily or twice daily dosing but peak to trough differences are greater with the latter regimen, creating the possibility of adverse effects at peak and arrhythmic escape at trough. Nevertheless, some patients may be transferred successfully to the twice daily regimen. (See DOSAGE AND ADMINISTRATION .)
HOW SUPPLIED
Mexiletine Hydrochloride Capsules, USP are supplied in bottles of 90 hard gelatin capsules containing 250 mg of mexiletine hydrochloride, USP:
Mexiletine Hydrochloride Capsules, USP, 250 mg have an orange body and green cap with the marking "250" in black ink on the cap. Capsules contain white or almost white powder. (NDC 62135-785-90).
Store at 25°C (77°F); excursions permitted to 15–30°C (59–86°F) [see USP Controlled Room Temperature].
Dispense with a child-resistant closure (as required).
Rx Only
Manufactured by: Rivopharm S.A. 6928, Manno, Switzerland
Manufactured for: Chartwell RX, LLC. Congers, NY 10920
L71750
Rev. 10/2023