Get your patient on Lidocaine Hydrochloride - Lidocaine Hydrochloride jelly (Lidocaine Hydrochloride)
Lidocaine Hydrochloride - Lidocaine Hydrochloride jelly prescribing information
INDICATIONS AND USAGE:
Lidocaine Hydrochloride Jelly USP, 2% is indicated for prevention and control of pain in procedures involving the male and female urethra for topical treatment of painful urethritis, and as an anesthetic lubricant for endotracheal intubation (oral and nasal).
DOSAGE AND ADMINISTRATION:
When Lidocaine Hydrochloride Jelly USP, 2% is used concomitantly with other products containing lidocaine, the total dose contributed by all formulations must be kept in mind.
The dosage varies and depends upon the area to be anesthetized, vascularity of the tissues, individual tolerance, and the technique of anesthesia. The lowest dosage needed to provide effective anesthesia should be administered. Dosages should be reduced for children and for elderly and debilitated patients. Although the incidence of adverse effects with Lidocaine Hydrochloride Jelly USP, 2% is quite low, caution should be exercised, particularly when employing large amounts, since the incidence of adverse effects is directly proportional to the total dose of local anesthetic agent administered.
For Surface Anesthesia of the Male Adult Urethra
Slowly instill approximately 15 mL (300 mg of lidocaine HCl) into the urethra or until the patient has a feeling of tension. A penile clamp is then applied for several minutes at the corona. An additional dose of not more than 15 mL (300 mg) can be instilled for adequate anesthesia.
Prior to sounding or cystoscopy, a penile clamp should be applied for 5 to 10 minutes to obtain adequate anesthesia. A total dose of 30 mL (600 mg) is usually required to fill and dilate the male urethra. Prior to catheterization, smaller volumes of 5 to 10 mL (100 to 200 mg) are usually adequate for lubrication.
For Surface Anesthesia of the Female Adult Urethra
Slowly instill 3 to 5 mL (60 to 100 mg of lidocaine HCl) of the jelly into the urethra. If desired, some jelly may be deposited on a cotton swab and introduced into the urethra. In order to obtain adequate anesthesia, several minutes should be allowed prior to performing urological procedures.
Lubrication for Endotracheal Intubation
Apply a moderate amount of jelly to the external surface of the endotracheal tube shortly before use. Care should be taken to avoid introducing the product into the lumen of the tube. Do not use the jelly to lubricate endotracheal stylettes. See WARNINGS and ADVERSE REACTIONS concerning rare reports of inner lumen occlusion. It is also recommended that use of endotracheal tubes with dried jelly on the external surface be avoided for lack of lubricating effect.
MAXIMUM DOSAGE:
No more than 600 mg of lidocaine hydrochloride should be given in any 12 hour period.
Children
It is difficult to recommend a maximum dose of any drug for children since this varies as a function of age and weight. For children less than ten years who have a normal lean body mass and a normal lean body development, the maximum dose may be determined by the application of one of the standard pediatric drug formulas (e.g., Clark's rule). For example, in a child of five years weighing 50 lbs., the dose of lidocaine hydrochloride should not exceed 75–100 mg when calculated according to Clark's rule. In any case, the maximum amount of lidocaine administered should not exceed 4.5 mg / kg (2 mg / lb) of body weight.
CONTRAINDICATIONS:
Lidocaine is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type or to other components of Lidocaine Hydrochloride Jelly USP, 2%.
ADVERSE REACTIONS:
Adverse experiences following the administration of lidocaine are similar in nature to those observed with other amide local anesthetic agents. These adverse experiences are, in general, dose-related and may result from high plasma levels caused by excessive dosage or rapid absorption, or may result from a hypersensitivity, idiosyncrasy, or diminished tolerance on the part of the patient. Serious adverse experiences are generally systemic in nature. The following types are those most commonly reported:
There have been rare reports of endotracheal tube occlusion associated with the presence of dried jelly residue in the inner lumen of the tube (see WARNINGS and DOSAGE AND ADMINISTRATION ).
Central Nervous System
CNS manifestations are excitatory and/or depressant and may be characterized by lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred or double vision, vomiting, sensations of heat, cold or numbness, twitching, tremors, convulsions, unconsciousness, respiratory depression and arrest. The excitatory manifestations may be very brief or may not occur at all, in which case the first manifestation of toxicity may be drowsiness merging into unconsciousness and respiratory arrest.
Drowsiness following the administration of lidocaine is usually an early sign of a high blood level of the drug and may occur as a consequence of rapid absorption.
Cardiovascular system
Cardiovascular manifestations are usually depressant and are characterized by bradycardia, hypotension, and cardiovascular collapse, which may lead to cardiac arrest.
Allergic
Allergic reactions are characterized by cutaneous lesions, urticaria, edema or anaphylactoid reactions. Allergic reactions may occur as a result of sensitivity either to the local anesthetic agent or to other components in the formulation. Allergic reactions as a result of sensitivity to lidocaine are extremely rare and, if they occur, should be managed by conventional means. The detection of sensitivity by skin testing is of doubtful value.
Drug Interactions
Patients who are administered local anesthetics are at increased risk of developing methemoglobinemia when concurrently exposed to the following drugs, which could include other local anesthetics:
Examples of Drugs Associated with Methemoglobinemia:
| Class | Examples |
| Nitrates/Nitrites | nitric oxide, nitroglycerin, nitroprusside, nitrous oxide |
| Local anesthetics | articaine, benzocaine, bupivacaine, lidocaine, mepivacaine, prilocaine, procaine, ropivacaine, tetracaine |
| Antineoplastic Agents | cyclophosphamide, flutamide, hydroxyurea, ifosfamide, rasburicase |
| Antibiotics | dapsone, nitrofurantoin, para-aminosalicylic acid, sulfonamides |
| Antimalarials | chloroquine, primaquine |
| Anticonvulsants | Phenobarbital, phenytoin, sodium valproate, |
| Other drugs | acetaminophen, metoclopramide, quinine, sulfasalazine |
DESCRIPTION
Lidocaine Hydrochloride Jelly USP, 2% is a sterile aqueous product that contains a local anesthetic agent and is administered topically (see INDICATIONS AND USAGE for specific uses).
Lidocaine Hydrochloride Jelly USP, 2% contains lidocaine hydrochloride which is chemically designated as acetamide, 2-(diethylamino)-N-(2,6-dimethylphenyl)-, monohydrochloride and has the following structural formula:
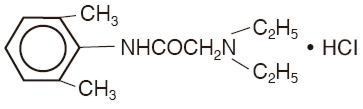
Lidocaine Hydrochloride Jelly USP, 2% also contains sodium carboxymethylcellulose, and the resulting mixture maximizes contact with mucosa and provides lubrication for instrumentation. The unused portion should be discarded after initial use.
Composition of Lidocaine Hydrochloride Jelly USP, 2%: Each mL contains 20 mg of lidocaine HCI. The formulation also contains sodium carboxymethylcellulose and sodium hydroxide and/or hydrochloric acid to adjust pH between 6.0 to 7.0.
CLINICAL PHARMACOLOGY:
Mechanism of action
Lidocaine stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
Onset of action
The onset of action is 3 to 5 minutes. It is ineffective when applied to intact skin.
Hemodynamics
Excessive blood levels may cause changes in cardiac output, total peripheral resistance, and mean arterial pressure. These changes may be attributable to a direct depressant effect of the local anesthetic agent on various components of the cardiovascular system.
Pharmacokinetics and Metabolism
Lidocaine may be absorbed following topical administration to mucous membranes, its rate and extent of absorption varies depending upon concentration and total dose administered, the specific site of application, and duration of exposure. In general, the rate of absorption of local anesthetic agents following topical application occurs most rapidly after intratracheal administration. Lidocaine is also well-absorbed from the gastrointestinal tract, but little intact drug may appear in the circulation because of biotransformation in the liver.
Lidocaine is metabolized rapidly by the liver, and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage, and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological / toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine. Approximately 90% of lidocaine administered is excreted in the form of various metabolites, and less than 10% is excreted unchanged.
The primary metabolite in urine is a conjugate of 4-hydroxy-2, 6-dimethylaniline.
The plasma binding of lidocaine is dependent on drug concentration, and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 mcg of free base per mL, 60 to 80 percent of lidocaine is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein.
Lidocaine crosses the blood-brain and placental barriers, presumably by passive diffusion.
Studies of lidocaine metabolism following intravenous bolus injections have shown that the elimination half-life of this agent is typically 1.5 to 2 hours. Because of the rapid rate at which lidocaine is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged twofold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics but may increase the accumulation of metabolites.
Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6 mcg free base per mL. In the rhesus monkey arterial blood levels of 18 to 21 mcg/mL have been shown to be the threshold for convulsive activity.
HOW SUPPLIED:
Lidocaine Hydrochloride Jelly USP, 2%
Box of 25
In unit use packages containing one single use vial and a URO-JET ® vial injector.
| Stock No. | ||
|---|---|---|
| 5 mL size | NDC 76329-3012-5 | 3012-SP |
| 10 mL size | NDC 76329-3013-5 | 3013-SP |
| 20 mL size | NDC 76329-3015-5 | 3015-SP |
In unit use packages containing one single use vial and a URO-JET ® AC (Anatomically Constricted) vial injector.
Box of 25
| Stock No. | ||
|---|---|---|
| 5 mL size | NDC 76329-3011-5 | 3011-SP |
Syringe Assembly Directions
Syringe Assembly Directions: USE ASEPTIC TECHNlQUE Do not assemble until ready to use.
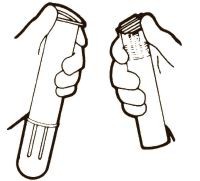 | 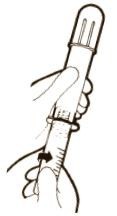 | 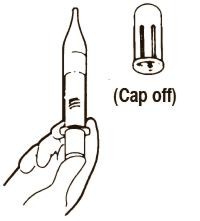 |
| 1)Open sterile pouch and drop contents directly onto sterile field. Remove protective caps. | 2)Thread vial into injector 3 half turns, or until needle penetrates stopper.• DO NOT PUSH VIAL INTO INJECTOR; THIS MAY CAUSE MISALIGNMENT. | 3)Remove cap and expel air. |
Store at controlled room temperature 15° to 30°C (59° to 86°F).
Mechanism of action
Lidocaine stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.