Lidocaine - Lidocaine Hydrochloride injection, Solution prescribing information
INDICATIONS AND USAGE
Lidocaine Hydrochloride Injection, USP is indicated for the production of local anesthesia, by infiltration techniques, such as percutaneous injection, and by peripheral nerve block techniques, such as brachial plexus and inter-costal, when the accepted procedures for these techniques as described in standard textbooks are observed.
DOSAGE AND ADMINISTRATION
Table 1 (Recommended Dosages) summarizes the recommended volumes and concentrations of lidocaine hydrochloride injection for various types of anesthetic procedures. The dosages suggested in this table are for normal healthy adults and refer to the use of epinephrine-free solutions. When larger volumes are required, only solutions containing epinephrine should be used, except in those cases where vasopressor drugs may be contraindicated.
There have been adverse event reports of chondrolysis in patients receiving intra-articular infusions of local anesthetics following arthroscopic and other surgical procedures. Lidocaine is not approved for this use (see WARNINGS and DOSAGE AND ADMINISTRATION ).
These recommended doses serve only as a guide to the amount of anesthetic required for most routine procedures. The actual volumes and concentrations to be used depend on a number of factors such as type and extent of surgical procedure, depth of anesthesia and degree of muscular relaxation required, duration of anesthesia required and the physical condition of the patient. In all cases the lowest concentration and smallest dose that will produce the desired result should be given. Dosages should be reduced for children and for elderly and debilitated patients and patients with cardiac and/or liver disease.
The onset of anesthesia, the duration of anesthesia and the degree of muscular relaxation are proportional to the volume and concentration (i.e. total dose) of local anesthetic used. Thus, an increase in volume and concentration of lidocaine hydrochloride injection will decrease the onset of anesthesia, prolong the duration of anesthesia, provide a greater degree of muscular relaxation and increase the segmental spread of anesthesia. However, increasing the volume and concentration of lidocaine hydrochloride injection may result in a more profound fall in blood pressure when used in epidural anesthesia. Although the incidence of side effects with lidocaine is quite low, caution should be exercised when employing large volumes and concentrations, since the incidence of side effects is directly proportional to the total dose of local anesthetic agent injected.
CONTRAINDICATIONS
Lidocaine HCl is contraindicated in patients with a known history of hypersensitivity to local anesthetics of the amide type.
ADVERSE REACTIONS
To report SUSPECTED ADVERSE REACTIONS, contact Fresenius Kabi USA, LLC at 1-800-551-7176 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Systemic
Adverse experiences following the administration of lidocaine HCl are similar in nature to those observed with other amide local anesthetic agents. These adverse experiences are, in general, dose-related and may result from high plasma levels caused by excessive dosage, rapid absorption or inadvertent intravascular injection, or may result from a hypersensitivity, idiosyncrasy or diminished tolerance on the part of the patient. Serious adverse experiences are generally systemic in nature.
The following types are those most commonly reported:
Central Nervous System
CNS manifestations are excitatory and/or depressant and may be characterized by lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred or double vision, vomiting, sensations of heat, cold or numbness, twitching, tremors, convulsions, unconsciousness, respiratory depression and arrest. The excitatory manifestations may be very brief or may not occur at all, in which case the first manifestation of toxicity may be drowsiness merging into unconsciousness and respiratory arrest.
Drowsiness following the administration of lidocaine HCl is usually an early sign of a high blood level of the drug and may occur as a consequence of rapid absorption.
Cardiovascular System
Cardiovascular manifestations are usually depressant and are characterized by bradycardia, hypotension, and cardiovascular collapse, which may lead to cardiac arrest.
Allergic
Allergic reactions are characterized by cutaneous lesions, urticaria, edema or anaphylactoid reactions. Allergic reactions may occur as a result of sensitivity either to local anesthetic agents or to the methylparaben used as a preservative in the multiple dose vials. Allergic reactions as a result of sensitivity to lidocaine HCl are extremely rare and, if they occur, should be managed by conventional means. The detection of sensitivity by skin testing is of doubtful value.
Neurologic
The incidences of adverse reactions associated with the use of local anesthetics may be related to the total dose of local anesthetic administered and are also dependent upon the particular drug used, the route of administration and the physical status of the patient. In a prospective review of 10,440 patients who received lidocaine HCl for spinal anesthesia, the incidences of adverse reactions were reported to be about 3% each for positional headaches, hypotension and backache; 2% for shivering; and less than 1% each for peripheral nerve symptoms, nausea, respiratory inadequacy and double vision. Many of these observations may be related to local anesthetic techniques, with or without a contribution from the local anesthetic.
There have been reported cases of permanent injury to extraocular muscles requiring surgical repair following retrobulbar administration.
DESCRIPTION
Lidocaine Hydrochloride Injection, USP is a local anesthetic which is a sterile, nonpyrogenic solution intended for parenteral injection. See INDICATIONS AND USAGE for specific uses.
Lidocaine hydrochloride is chemically designated as 2-(Diethylamino) 2’,6’ acetoxylidide monohydrochloride and has the following structural formula:
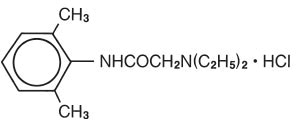
C 14 H 22 N 2 O • HCl M.W. 288.82
Each mL contains: Lidocaine hydrochloride 10 or 20 mg; methylparaben 0.1%; sodium chloride (7 mg and 6 mg of sodium chloride for 1% and 2% respectively) to render it isotonic; Water for Injection q.s. Hydrochloric acid and/or sodium hydroxide may have been added for pH adjustment (5.0 to 7.0).
CLINICAL PHARMACOLOGY
Mechanism of Action
Lidocaine HCl stabilizes the neuronal membrane by inhibiting the ionic fluxes required for the initiation and conduction of impulses, thereby effecting local anesthetic action.
Hemodynamics
Excessive blood levels may cause changes in cardiac output, total peripheral resistance, and mean arterial pressure. With central neural blockade these changes may be attributable to block of autonomic fibers, a direct depressant effect of the local anesthetic agent on various components of the cardiovascular system. The net effect is normally a modest hypotension when the recommended dosages are not exceeded.
Pharmacokinetics and Metabolism
Information derived from diverse formulations, concentrations and usages reveals that lidocaine HCl is completely absorbed following parenteral administration, its rate of absorption depending, for example, upon various factors such as the site of administration and the presence or absence of a vasoconstrictor agent. Except for intravascular administration, the highest blood levels are obtained following intercostal nerve block and the lowest after subcutaneous administration.
The plasma binding of lidocaine HCl is dependent on drug concentration, and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 mcg of free base/mL, 60 to 80% of lidocaine HCl is protein bound. Binding is also dependent on the plasma concentration of the alpha-1-acid glycoprotein.
Lidocaine HCl crosses the blood-brain and placental barriers, presumably by passive diffusion.
Lidocaine HCl is metabolized rapidly by the liver, and metabolites and unchanged drug are excreted by the kidneys. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage, and conjugation. N-dealkylation, a major pathway of biotransformation, yields the metabolites monoethylglycinexylidide and glycinexylidide. The pharmacological/toxicological actions of these metabolites are similar to, but less potent than, those of lidocaine HCl. Approximately 90% of lidocaine HCl administered is excreted in the form of various metabolites, and less than 10% is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2,6-dimethylaniline.
The elimination half-life of lidocaine HCl following an intravenous bolus injection is typically 1.5 to 2 hours. Because of the rapid rate at which lidocaine HCl is metabolized, any condition that affects liver function may alter lidocaine kinetics. The half-life may be prolonged two-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine HCl kinetics but may increase the accumulation of metabolites.
Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine HCl required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6 mcg free base/mL. In the rhesus monkey arterial blood levels of 18 to 21 mcg/mL have been shown to be threshold for convulsive activity.
HOW SUPPLIED
Lidocaine Hydrochloride Injection is preserved with 0.1% methylparaben and is available in the following concentrations:
Product Code | Unit of Sale | Strength | Each |
920102 | NDC 63323-201-02 Unit of 25 | 1% 20 mg per 2 mL (10 mg per mL) | NDC 63323-201-01 2 mL Vial |
20110 | NDC 63323-201-10 Unit of 25 | 1% 100 mg per 10 mL (10 mg per mL) | NDC 63323-201-03 10 mL Multiple Dose Vial |
20202 | NDC 63323-202-02 Unit of 25 | 2% 40 mg per 2 mL (20 mg per mL) | NDC 63323-202-01 2 mL Vial |
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature].
Protect from light.