Get your patient on Kygevvi (Doxecitine And Doxribtimine)
Kygevvi prescribing information
INDICATIONS AND USAGE
KYGEVVI is indicated for the treatment of thymidine kinase 2 deficiency (TK2d) in adults and pediatric patients with an age of symptom onset on or before 12 years.
DOSAGE AND ADMINISTRATION
- Obtain baseline transaminase (alanine aminotransferase [ALT] and aspartate aminotransferase [AST]) levels in all patients prior to treatment initiation. (2.1 )
- Recommended dosage (2.2 ):
KYGEVVI Dosage Level KYGEVVI Dosage (mg/kg/day) Starting 260 mg/kg/day (consisting of 130 mg doxecitine and 130 mg doxribtimine) Intermediate 520 mg/kg/day (consisting of 260 mg doxecitine and 260 mg doxribtimine) Maintenance 800 mg/kg/day (consisting of 400 mg doxecitine and 400 mg doxribtimine) - Titrate to the next dosage level based on tolerability after a minimum of 2 weeks at the current dosage level. (2.2 )
- Administer KYGEVVI orally in 3 equally divided doses with food. (2.2 )
- See full prescribing information for dosage and administration modifications, monitoring, and preparation and administration instructions. (2.4 )
- Use KYGEVVI only with ZX2000 administration kit. (2.4 )
Important Recommendation Prior to KYGEVVI Treatment Initiation
Obtain baseline liver transaminase (alanine aminotransferase [ALT] and aspartate aminotransferase [AST]) and total bilirubin levels in patients prior to treatment initiation with KYGEVVI [see Dosage and Administration (2.3) and Warnings and Precautions (5.1) ] .
Recommended Dosage
The recommended dosage of KYGEVVI is based on the patient's weight (Table 1). Titrate to the next dosage level based on tolerability after a minimum of 2 weeks at the current dosage level.
| KYGEVVI Dosage Level | KYGEVVI Dosage (mg/kg/day) |
|---|---|
| Starting | 260 mg/kg/day (consisting of 130 mg doxecitine and 130 mg doxribtimine) |
| Intermediate | 520 mg/kg/day (consisting of 260 mg doxecitine and 260 mg doxribtimine) |
| Maintenance | 800 mg/kg/day (consisting of 400 mg doxecitine and 400 mg doxribtimine) |
Administer KYGEVVI orally in 3 equally divided doses approximately 6 hours apart (plus or minus 2 hours) with food [see Clinical Pharmacology (12.3) ] .
After calculating the daily dose, use Table 2 to determine the required number of KYGEVVI packets, volume of water needed to reconstitute the powder from the packet(s), and individual volume that is administered 3 times a day [see Dosage and Administration (2.4) ].
Dosage and Administration Modifications and Monitoring
Liver Test Abnormalities
If signs or symptoms consistent with liver injury are observed, interrupt treatment with KYGEVVI until liver transaminase (ALT, AST) and total bilirubin levels have either returned to baseline or stabilized at a new baseline value. Consider re-starting KYGEVVI at the last tolerated dose and increase the dose based on tolerability [see Dosage and Administration (2.2) ] . Consider permanently discontinuing KYGEVVI if signs or symptoms consistent with liver injury persist or worsen. Monitor liver transaminases and total bilirubin levels yearly and as clinically indicated [see Warnings and Precautions (5.1) ] .
Gastrointestinal
Based on the severity of the diarrhea and/or vomiting, reduce the dose of KYGEVVI or interrupt treatment until diarrhea and/or vomiting improves or returns to baseline. Consider re-starting KYGEVVI at the last tolerated dose and increase the dose based on tolerability [see Dosage and Administration (2.2) ] . For persistent or recurring diarrhea and/or vomiting, consider discontinuing KYGEVVI permanently. Monitor for dehydration and treat promptly with electrolyte replacement [see Warnings and Precautions (5.2) ] .
Preparation and Administration Instructions
Use Table 2 for preparation and administration information.
| Total Daily Dose (mg/day) | Volume of Solution (mL) (administered 3 times per day) | Total mL of Water for Reconstitution | Total Number of KYGEVVI Packets for Reconstitution |
|---|---|---|---|
| 750 – 824 | 2.5 | 40 | 1 |
| 825 – 974 | 3 | ||
| 975 – 1,124 | 3.5 | ||
| 1,125 – 1,299 | 4 | ||
| 1,300 – 1,449 | 4.5 | ||
| 1,450 – 1,649 | 5 | ||
| 1,650 – 1,949 | 6 | ||
| 1,950 – 2,249 | 7 | ||
| 2,250 – 2,549 | 8 | ||
| 2,550 – 2,849 | 9 | ||
| 2,850 – 3,149 | 10 | ||
| 3,150 – 3,449 | 11 | ||
| 3,450 – 3,749 | 12 | ||
| 3,750 – 4,049 | 13 | ||
| 4,050 – 4,349 | 14 | 80 | 2 |
| 4,350 – 4,649 | 15 | ||
| 4,650 – 4,949 | 16 | ||
| 4,950 – 5,249 | 17 | ||
| 5,250 – 5,549 | 18 | ||
| 5,550 – 5,849 | 19 | ||
| 5,850 – 6,149 | 20 | ||
| 6,150 – 6,449 | 21 | ||
| 6,450 – 6,749 | 22 | ||
| 6,750 – 7,049 | 23 | ||
| 7,050 – 7,349 | 24 | ||
| 7,350 – 7,649 | 25 | ||
| 7,650 – 7,949 | 26 | ||
| 7,950 – 8,249 | 27 The volume of each individual dose, when multiplied by 3, may not match the corresponding water volume used in the preparation of the oral solution as the final volume of the reconstituted oral solution will increase after the powder from the packets is added to the water volume. | ||
| 8,250 – 8,549 | 28 | 120 | 3 |
| 8,550 – 8,849 | 29 | ||
| 8,850 – 9,749 | 30 | ||
| 9,750 – 11,249 | 35 | ||
| 11,250 – 12,749 | 40 | ||
| 12,750 – 14,249 | 45 | 160 | 4 |
| 14,250 – 15,749 | 50 | ||
| 15,750 – 17,249 | 55 | ||
| 17,250 – 18,749 | 60 | 200 | 5 |
| 18,750 – 20,249 | 65 | ||
| 20,250 – 21,749 | 70 | ||
| 21,750 – 23,249 | 75 | 240 | 6 |
| 23,250 – 24,749 | 80 | ||
| 24,750 – 26,249 | 85 | 280 | 7 |
| 26,250 – 27,749 | 90 | ||
| 27,750 – 29,249 | 95 | ||
| 29,250 – 30,749 | 100 | 320 | 8 |
| 30,750 – 32,249 | 105 | ||
| 32,250 – 33,749 | 110 | ||
| 33,750 – 35,249 | 115 | 360 | 9 |
| 35,250 – 36,749 | 120 | ||
| 36,750 – 38,249 | 125 | ||
| 38,250 – 39,749 | 130 | 400 | 10 |
| 39,750 – 41,249 | 135 | ||
| 41,250 – 42,749 | 140 | ||
| 42,750 – 44,249 | 145 | 440 | 11 |
| 44,250 – 45,749 | 150 | ||
| 45,750 – 47,249 | 155 | ||
| 47,250 – 48,749 | 160 | 480 | 12 |
| 48,750 – 50,249 | 165 | ||
| 50,250 – 51,749 | 170 | ||
| 51,750 – 53,249 | 175 | 520 | 13 |
| 53,250 – 54,749 | 180 | ||
| 54,750 – 56,249 | 185 | 560 | 14 |
| 56,250 – 57,749 | 190 | ||
| 57,750 – 59,249 | 195 | ||
| 59,250 – 60,749 | 200 | 600 | 15 |
| 60,750 – 62,249 | 205 | ||
| 62,250 – 63,749 | 210 | ||
| 63,750 – 65,249 | 215 | 640 | 16 |
| 65,250 – 66,749 | 220 | ||
| 66,750 – 68,249 | 225 |
Use the ZX2000 administration kit provided separately to prepare and administer the prescribed dose [see How Supplied/Storage and Handling (16) ] . Refer to the Instructions for Use for full preparation and administration information on use of KYGEVVI with the ZX2000 administration kit. Household devices such as measuring cups or spoons are not adequate measuring devices. KYGEVVI should be prepared and administered by adults only.
Preparation Instructions
Preparation of KYGEVVI with a liquid other than water has not been studied clinically and is not recommended.
- Obtain the required number of KYGEVVI packets to prepare a one-day supply of solution each morning.
- Use 40 mL of water per packet. Pour the prescribed volume of room temperature water (between 20°C - 25°C or 68°F - 77°F) into the mixing bottle.
- Add the powder from the required number of KYGEVVI packets into the mixing bottle.
- Screw the dosing cup tightly onto the mixing bottle and gently invert the mixing bottle back and forth at least 20 times. If powder remains, repeat until the powder dissolves.
- The mixed solution may appear cloudy and have some residual powder (inactive ingredients) remaining at the bottom or top.
Administration Instructions
Oral Administration
- Before each administration, gently invert the tightly closed mixing bottle slowly back and forth at least 3 times.
- Use 1 of 2 methods (dosing cup or oral syringe) to administer KYGEVVI solution. Choose the method based on the volume of solution to be administered per dose.
- Take KYGEVVI solution in 3 equally divided doses approximately 6 hours apart (plus or minus 2 hours) with food.
- Do not administer another dose if the dose is spit out or if a complete dose is not taken. Take the next dose at the next scheduled time.
- Discard any remaining KYGEVVI solution 16 hours after reconstitution or after taking or giving the 3 doses, whichever comes first.
Feeding Tube Administration
KYGEVVI is compatible with most commonly available feeding tubes. KYGEVVI is compatible with feeding tubes made with polyvinylchloride (PVC) free from DEHP (Phthalates), polyurethane (PUR), and silicone (SIL) material.
- Follow the instructions of the feeding tube manufacturer to administer KYGEVVI.
- Draw up the KYGEVVI solution using a syringe compatible with the feeding tube.
- Administer the solution immediately through the feeding tube.
- Flush any residual solution in the syringe or feeding tube until no solution is left. To flush the tube, a single flushing step with a volume of water equivalent to the tube's priming volume is sufficient.
- Discard any remaining KYGEVVI solution 16 hours after reconstitution or after taking or giving the 3 doses, whichever comes first.
Storage Instructions for Prepared KYGEVVI Solution
- Store reconstituted KYGEVVI solution at controlled room temperature between 20°C to 25°C (68°F to 77°F) or in the refrigerator between 2°C to 8°C (36°F to 46°F).
- Discard KYGEVVI solution 16 hours after reconstitution or after taking or giving the 3 doses, whichever comes first.
Missed Dose
If a dose is missed, take the missed dose as soon as possible but do not take within 2 hours of the next scheduled dose. In that case, skip the missed dose and resume the regular schedule. A double dose should not be taken to make up for the missed dose.
DOSAGE FORMS AND STRENGTHS
Powder for oral solution: 2 g doxecitine and 2 g doxribtimine as white to off-white powder in a single use packet.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary
There are no available data on KYGEVVI use during pregnancy to evaluate for a drug-associated risk of major birth defects, miscarriage, or other adverse maternal or fetal outcomes. Endogenous pyrimidine nucleosides are transported across the placenta. There are risks for adverse maternal and fetal outcomes during pregnancy with mitochondrial myopathies, including TK2 deficiency ( see Clinical Considerations ). In animal reproduction studies, oral administration of doxecitine and doxribtimine to pregnant rats and rabbits during organogenesis resulted in maternal and fetal toxicities in the rabbit at dose exposures 1233 and 811 times the maximum recommended human dose (MRHD) of 400 mg/kg/day doxecitine and 400 mg/kg/day doxribtimine, respectively, based on plasma exposure, but were not observed in the rat ( see Data ).
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20% respectively.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
Mitochondrial myopathies are associated with increased adverse perinatal outcomes, including preterm birth, pre-eclampsia and gestational diabetes.
Data
Animal Data
In an embryofetal development study in pregnant rats, once daily oral doses of 200, 600, and 2000 mg/kg/day doxecitine and doxribtimine were administered throughout organogenesis between gestation day (GD) 7 to 17. No maternal or embryofetal toxicity was observed up to 2000 mg/kg/day (1223 times and 425 times the MRHD of doxecitine and doxribtimine, respectively, based on plasma exposure).
In an embryofetal development study in pregnant rabbits, once daily oral doses of 200, 600, and 2000 mg/kg/day doxecitine and doxribtimine were administered throughout organogenesis between GD 7 and GD 19. Marked maternal toxicity and fetal malformations (dilated aorta with an associated narrow pulmonary trunk) were observed at the highest dose (1233 times and 811 times the MRHD of doxecitine and doxribtimine, respectively, based on plasma exposure). The maternal and fetal no observed adverse effect level (NOAEL) in rabbits (600 mg/kg/day) was associated with maternal plasma exposures 729 times and 126 times the MRHD of 400 mg/kg/day doxecitine and 400 mg/kg/day doxribtimine, respectively.
Lactation
Risk Summary
There are no data on the presence of doxecitine and doxribtimine or its metabolites in either human or animal milk, the effects on the breastfed infant, or the effects on milk production. Data from published literature reports the presence of nucleosides and nucleotides in human milk.
The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for KYGEVVI and any potential adverse effects on the breastfed infant from KYGEVVI or from the underlying maternal condition.
Pediatric Use
The safety and effectiveness of KYGEVVI for the treatment of thymidine kinase 2 deficiency (TK2d) have been established in pediatric patients with an age of symptom onset on or before 12 years. Use of KYGEVVI for this indication in this population is supported by evidence from two retrospective studies (Study 1, Study 2), one open-label study (Trial 1), and an expanded access program in which a total of 68 patients 0.7 years of age to less than 17 years of age were treated [see Clinical Studies (14) ] .
In Trial 1, compared to adults, a higher percentage of pediatric patients experienced adverse reactions of vomiting and elevated liver transaminases [see Adverse Reactions (6.1) ] . Serious adverse reactions in the pediatric population included hospitalization due to diarrhea in two patients [see Warnings and Precautions (5.2) ] .
Geriatric Use
Clinical studies of KYGEVVI did not include sufficient number of patients 65 years of age and older to determine whether they respond differently from younger adult patients.
Renal Impairment
Plasma concentrations of doxecitine and doxribtimine increased in patients with moderate or severe renal impairment. The pharmacokinetics (PK) of doxecitine and doxribtimine have not been evaluated in patients with mild renal impairment. An appropriate dosage adjustment of KYGEVVI in patients with renal impairment could not be determined because renal impairment had distinct effects on the PK of doxecitine and PK of doxribtimine, and it is not feasible to separately adjust the dosage for doxecitine or doxribtimine contained in KYGEVVI [see Clinical Pharmacology (12.3) ] .
CONTRAINDICATIONS
None.
WARNINGS AND PRECAUTIONS
- Elevated Liver Transaminase Levels : Obtain baseline liver transaminase (ALT, AST) and total bilirubin levels prior to treatment initiation with KYGEVVI. If signs or symptoms consistent with liver injury are observed, interrupt treatment. Consider permanently discontinuing KYGEVVI if signs/symptoms consistent with liver injury persist or worsen. Monitor patients yearly and as clinically indicated. (5.1 )
- Gastrointestinal Adverse Reactions : Reduce KYGEVVI dosage or interrupt treatment based on severity of diarrhea and/or vomiting. If persistent severe diarrhea and/or vomiting occurs, consider discontinuing KYGEVVI permanently. (5.2 )
Elevated Liver Transaminase Levels
Elevated liver transaminase [alanine aminotransferase (ALT) and/or aspartate aminotransferase (AST)] levels were reported in patients treated with KYGEVVI [see Adverse Reactions (6.1) ] . In Study 1, two patients permanently discontinued treatment with KYGEVVI upon recurrence of elevated liver enzymes after a rechallenge at a reduced dose.
Obtain baseline liver transaminase (ALT, AST) and total bilirubin levels in patients prior to treatment initiation with KYGEVVI. If signs or symptoms consistent with liver injury are observed, interrupt treatment with KYGEVVI until liver transaminase (ALT, AST) and total bilirubin levels have either returned to baseline or stabilized at a new baseline value. Consider permanently discontinuing KYGEVVI if signs or symptoms consistent with liver injury persist or worsen. Monitor liver transaminases and total bilirubin levels yearly and as clinically indicated [see Dosage and Administration (2.3) ] .
Gastrointestinal Adverse Reactions
Diarrhea and vomiting leading to hospitalization, dose reduction, and permanent discontinuation were reported in patients treated with KYGEVVI [see Adverse Reactions (6.1) ] .
Based on the severity of the diarrhea and/or vomiting, reduce the dosage of KYGEVVI or interrupt treatment until diarrhea and/or vomiting improves or returns to baseline. Consider restarting KYGEVVI at the last tolerated dose, and increase the dose as tolerated. For persistent or recurring diarrhea and/or vomiting, consider discontinuing KYGEVVI permanently and provide supportive care with electrolyte repletion as clinically indicated.
ADVERSE REACTIONS
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Elevated Liver Transaminase Levels [see Warnings and Precautions (5.1) ]
- Gastrointestinal Adverse Reactions [see Warnings and Precautions (5.2) ]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The safety of KYGEVVI was evaluated in a prospective, open-label, single-arm study in pediatric and adult patients with genetically confirmed TK2d previously treated with pyrimidine nucleosides (Trial 1). Additional safety information was derived from retrospective chart review studies (Study 1, Study 2) and from an expanded access program [see Clinical Studies (14) ] .
Permanent discontinuation of KYGEVVI due to an adverse reaction occurred in 9% of patients (Trial 1, Study 1, and Study 2). The adverse reactions which resulted in permanent discontinuation of KYGEVVI in >2% of patients were diarrhea (3%) and elevated liver enzymes (3%). In the expanded access program, diarrhea resulted in permanent discontinuation in 2 patients.
Dose reductions of KYGEVVI due to an adverse reaction occurred in 22% of patients (Trial 1, Study 1, and Study 2). Adverse reactions which required dose reduction in >2% of patients included diarrhea (21%) and abdominal pain (3%).
Diarrhea resulted in hospitalization in 2 pediatric patients (Study 1 and expanded access program).
Adverse Reactions from Trial 1
A total of 47 patients, between the ages of 0.7 and 74 years of age at enrollment, received KYGEVVI or pyrimidine nucleosides dosages up to 800 mg/kg/day [see Clinical Studies (14) ] . KYGEVVI is not approved for use in patients with an age of TK2d symptom onset > 12 years. The mean (SD) KYGEVVI or pyrimidine nucleosides exposure during Trial 1 was 6.6 (2) years.
Table 3 summarizes the adverse reactions reported in ≥ 5% patients treated with KYGEVVI or pyrimidine nucleosides.
| Adverse reactions | Treated Patients (N=47) n (%) |
|---|---|
| Diarrhea | 34 (72) |
| Abdominal pain (including abdominal pain upper) | 11 (23) |
| Vomiting | 10 (21) |
| Alanine aminotransferase increased (ALT) | 10 (21) |
| Aspartate aminotransferase increased (AST) | 8 (17) |
Adverse reactions, vomiting and elevated liver transaminases, were observed in a higher percentage of pediatric patients than in adult patients. In Trial 1, vomiting occurred in 28% (9/32) of pediatric patients compared to 7% (1/15) of adult patients. Elevated liver transaminases occurred in 25% (8/32) for ALT and 22% (7/32) for AST of pediatric patients compared to 13% (2/15) for ALT and 7% (1/15) for AST of adult patients.
Laboratory Adverse Reaction
Elevated liver enzymes have been observed as a clinical manifestation of TK2d. In Trial 1 and Study 1, elevations in alanine aminotransferase (ALT) and/or aspartate aminotransferase (AST) occurred in 28% (14/50) and 22% (11/50) of patients respectively. In Trial 1, of all the patients who started treatment with elevated AST/ALT at baseline, 5% had last post-baseline ALT values that were higher severity than the baseline severity while continuing treatment [see Warnings and Precautions (5.1) ] .
DESCRIPTION
KYGEVVI is a combination of doxecitine and doxribtimine, both of which are pyrimidine nucleosides. KYGEVVI is a powder for oral solution. Both doxecitine and doxribtimine are white to off-white powders and soluble in water.
Doxecitine
The chemical name of doxecitine is 4-Amino-1-((2R,4S,5R)-4-hydroxy-5-(hydroxymethyl)tetrahydrofuran-2-yl)pyrimidin-2(1H)-one. The molecular formula is C 9 H 13 N 3 O 4 and the molecular weight is 227.22 g/mol. The chemical structure is:
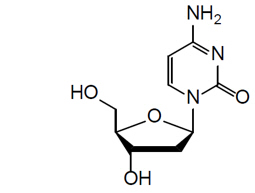
Doxribtimine
The chemical name of doxribtimine is 1-((2R,4S,5R)-4-Hydroxy-5-(hydroxymethyl)tetrahydrofuran-2-yl)-5-methylpyrimidine-2,4(1H,3H)-dione. The molecular formula is C 10 H 14 N 2 O 5 and the molecular weight is 242.23 g/mol. The chemical structure is:
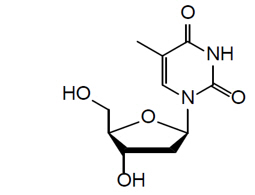
Each packet of KYGEVVI powder contains 2 grams doxecitine and 2 grams doxribtimine. The inactive ingredients are colloidal silicon dioxide and magnesium stearate.
CLINICAL PHARMACOLOGY
Mechanism of Action
Administration of KYGEVVI is intended to incorporate the pyrimidine nucleosides, deoxycytidine and deoxythymidine, into skeletal muscle mitochondrial deoxyribonucleic acid (DNA). This action restores mitochondrial DNA copy number in TK2d mutant mice.
Pharmacodynamics
The exposure-response relationship and time course of pharmacodynamic response for the safety and effectiveness of KYGEVVI have not been fully characterized.
Pharmacokinetics
Following oral administration of doxecitine and doxribtimine in healthy adult subjects, the baseline-adjusted maximum plasma concentration (C max ) and area under the plasma concentration-time curve (AUC) increased in a less than dose proportional manner for doxecitine at doses ranging from 43 mg/kg to 133 mg/kg and more than dose proportional manner for doxribtimine at doses ranging from 43 mg/kg to 133 mg/kg. There is minimal or no accumulation of doxecitine and doxribtimine following multiple dose administrations. Following oral administration of doxecitine and doxribtimine at the recommended maintenance dosage of 800 mg/kg/day under fed conditions in 18 TK2d pediatric and adult subjects, the estimated baseline-unadjusted geometric mean C max at steady state was 12 ng/mL and 19 ng/mL for doxecitine and doxribtimine, respectively, and the geometric mean AUC from time 0 to 24 hours (AUC 0-24hr ) was 108 ng∙h/mL and 191 ng∙h/mL for doxecitine and doxribtimine, respectively. Inter-subject variability (geometric CV%) in C max and AUC 0-24h values of doxecitine and doxribtimine were greater than 70%.
Absorption
The absolute bioavailability of doxecitine and doxribtimine following oral administration has not been determined. The median time to peak plasma concentration (T max ) was approximately 2 hours for doxecitine and 4 hours for doxribtimine.
Effect of Food
Following an oral administration of 133 mg/kg doxecitine and 133 mg/kg doxribtimine with a high-fat, high-calorie meal in healthy adult subjects, baseline-adjusted plasma C max and AUC 0-t increased by 79% and 137%, respectively, for doxecitine; and increased by 27% and 74%, respectively, for doxribtimine, compared to fasted conditions [see Dosage and Administration (2.2) ] .
Distribution
In vitro plasma protein binding of doxecitine and doxribtimine was less than 10% over the concentration range between 0.23 mcg/mL and 23 mcg/mL.
Elimination
The mean half-life was approximately 1 hour for doxecitine and 5 hours for doxribtimine following a single oral administration of 133 mg/kg doxecitine and 133 mg/kg doxribtimine under fed conditions in healthy adult subjects.
Metabolism
Doxecitine and doxribtimine are primarily degraded (catabolized) by cytidine deaminase and thymidine phosphorylase, respectively, to their nucleobases and the 2-deoxy-α-D-ribose 1-phosphate moiety. Intermediate products of doxecitine catabolism are deoxyuridine, uracil, and dihydrouracil with the end products β-alanine, ammonia, and carbon dioxide (CO 2 ). Thymine, the pyrimidine nucleobase of doxribtimine, is subsequently catabolized to dihydrothymine and ultimately to γ-amino-isobutyric acid and CO 2 .
Doxecitine and doxribtimine are not known to be metabolized by cytochrome P450 (CYP) isoforms.
Excretion
Urinary excretion of intact doxecitine and doxribtimine was <1% of the dose in healthy subjects following an oral administration of doxecitine and doxribtimine.
Specific Populations
Male and Female Patients
The pharmacokinetics of doxecitine and doxribtimine were not significantly different between male and female subjects.
Patients with Renal Impairment
The pharmacokinetics of doxecitine and doxribtimine in subjects with moderate (estimated glomerular filtration rate [eGFR] ≥ 30 and ≤ 59 mL/min/1.73 m 2 ) or severe (eGFR ≥ 15 and ≤ 29 mL/min/1.73 m 2 ) renal impairment were compared with healthy subjects with normal renal function following a single oral administration of 133 mg/kg doxecitine and 133 mg/kg doxribtimine. Baseline-adjusted plasma doxecitine AUC was 122% and 66% higher in subjects with moderate and severe renal impairment, respectively, compared with matched control subjects with normal renal function. Baseline adjusted plasma doxribtimine AUC was 447% and 148% higher in subjects with moderate and severe renal impairment, respectively, compared with matched control subjects with normal renal function [see Use in Specific Populations (8.6) ] .
Patients with Hepatic Impairment
No studies have been conducted to evaluate the effect of hepatic impairment on the pharmacokinetics of doxecitine and doxribtimine.
Drug Interaction Studies
In Vitro Studies
CYP enzymes : Doxecitine and doxribtimine are not inducers, inhibitors, or substrates of CYP isozymes at clinically relevant concentrations.
Transporter systems : Doxecitine and doxribtimine do not inhibit P-glycoprotein (P-gp), BCRP, BSEP, OATP1B1, OATP1B3, OAT1, OAT3, OCT1, OCT2, MATE1, or MATE2-K at clinically relevant concentrations. Doxribtimine may be a substrate of BCRP, but its clinical significance is unknown.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Animal studies to evaluate the carcinogenic potential of doxecitine and doxribtimine have not been conducted.
Mutagenesis
Doxecitine and doxribtimine were not mutagenic or clastogenic in an in vitro bacterial reverse mutation (Ames) and an in vivo rat micronucleus assay. Doxecitine and doxribtimine induced chromosomal aberrations in the absence of metabolic activation in an in vitro cytogenetic study in human lymphocytes. One compound (alpha-hydroxythymidine) originating from a doxribtimine starting material and present in the final drug product was positive for mutagenesis in the Ames assay and positive for clastogenesis in human peripheral lymphocytes when tested alone.
Impairment of Fertility
Doxecitine and doxribtimine had no effect on male or female fertility or early embryonic development at doses up to 2000 mg/kg/day in rats (1131 times and 1223 times the MRHD in males and females respectively for 400 mg/kg/day doxecitine and 1056 times and 425 times the MRHD in males and females respectively for 400 mg/kg/day doxribtimine, based on plasma exposure).
CLINICAL STUDIES
The efficacy of KYGEVVI for the treatment of patients with TK2d, with an age of symptom onset on or before 12 years of age, was established based on data from one Phase 2 clinical study (Trial 1), two retrospective chart review studies (Study 1, Study 2), and an expanded access program. The survival in treated patients was compared with survival in an untreated external control group comprised of untreated patients from published literature and Study 2.
Trial 1 (NCT03845712) is a prospective, open-label, single-arm study in 47 patients with genetically confirmed TK2d previously treated with pyrimidine nucleosides. Thirty-eight of these 47 patients have an age of TK2d symptom onset ≤12 years; none of the 38 patients discontinued treatment. The initial oral dose of KYGEVVI was matched to the patient's pyrimidine nucleoside dose of 260-800 mg/kg/day upon entering the study in patients with an age of TK2d symptom onset ≤ 12 years, and dosage was titrated, as needed, over a maximum of 4 weeks to the maintenance dose of 800 mg/kg/day.
Study 1 (NCT03701568) was a retrospective chart review study in 38 patients with genetically confirmed TK2d treated with pyrimidine nucleosides. Twenty-nine of these patients had an age of TK2d symptom onset ≤12 years; none of the 29 patients discontinued treatment. Thirty-five of these 38 patients were later enrolled in Trial 1 to receive treatment with KYGEVVI and one was later enrolled in Study 2. KYGEVVI was not administered in Study 1. Patients enrolled in Study 1 were receiving pyrimidine nucleoside treatment at doses 160-800 mg/kg/day.
Study 2 (NCT05017818) was a retrospective chart review study in 61 patients with genetically confirmed TK2d (43 untreated patients and 18 patients treated with pyrimidine nucleoside therapy). Nine of these 61 patients were also included in the expanded access program and 1 patient was included in Study 1. Twenty-seven of the 43 untreated patients had an age of TK2d symptom onset ≤12 years, and 13 of the 18 treated patients had an age of TK2d symptom onset ≤12 years. Twenty-two untreated patients were included in the untreated external control group used to evaluate survival. Of the 18 treated patients, 6 (33%) discontinued treatment due to an adverse reaction. KYGEVVI was not administered in Study 2. Patients enrolled in Study 2 were receiving pyrimidine nucleoside treatment at doses 200-1200 mg/kg/day.
Expanded Access Program
The expanded access program data included 43 patients receiving KYGEVVI; 9 patients were included in Study 2.
Efficacy Results
A total of 82 patients with genetically confirmed TK2d and the age of symptom onset ≤12 years were treated with KYGEVVI or pyrimidine nucleosides. Efficacy was assessed by comparing overall survival in the treated patients to an external control group of untreated patients matched to treated patients using age of TK2d symptom onset (≤ 2 years or >2 to ≤ 12 years). A total of 78 matched pairs were identified.
Of the 78 treated patients included in the survival analysis, 54% were male and 36% were of Hispanic or Latino ethnicity. Eighty-two percent of patients were White, 4% Black or African American, 5% Asian, 3% Other, and 1% American Indian or Alaska Native. The median age of TK2d symptom onset was 1.5 years (range: 0.01 to 12 years). The median duration of treatment was 4 years (range: 1 day to 12 years) and the median dose received was 762 mg/kg/day (range: 260 to 800 mg/kg/day).
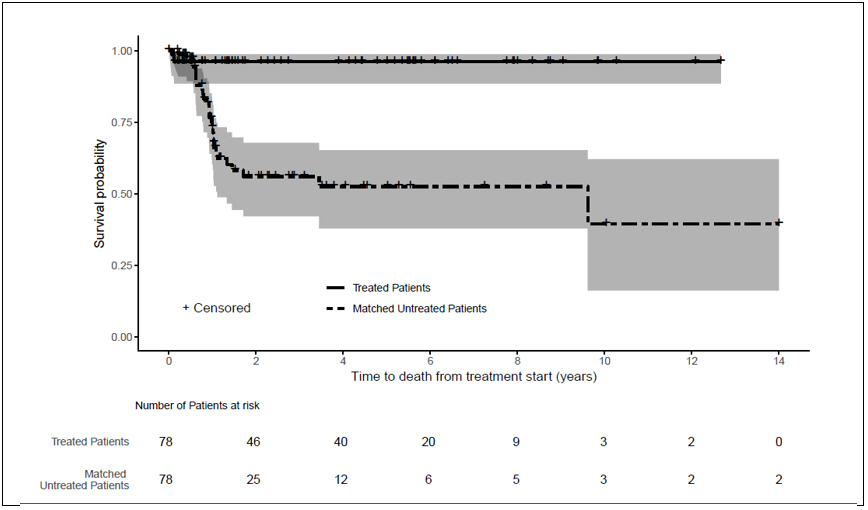
Treatment reduced the overall risk of death from treatment start by approximately 86% (95% CI: 61%, 96%) (Table 4, Figure 1).
| Treated Patients (n= 78) | Matched Untreated Patients (n=78) | |
|---|---|---|
| CI: Confidence Interval | ||
| Number of Deaths (%) An additional censoring step for untreated subjects was performed for each matched pair where the untreated subject died and had a longer follow-up time than the matched treated subject who was censored. The follow-up time of the untreated subject was then censored at the follow-up time of the treated subject. | 3 (3.8%) | 28 (35.9%) |
| Restricted Mean Survival Time in Years (95% CI) , Based on the area under the survival curves up to 4-, 6-, 10-years post treatment start. | ||
|
|
|
| Hazard Ratio Estimates based on Cox Proportional Hazard Model with Firth correction that includes matched pair as a strata, age of symptom onset as a continuous covariate, and treatment (treated or untreated) as a time independent variable. | ||
| For Risk of death from treatment start | 0.14 (0.04, 0.39) | |
| (95%CI) | ||
Note: Treated patients were matched 1:1 to untreated patients by category of age of TK2d symptom onset (≤2 years or >2 to ≤12 years). Within each category of age of symptom onset, the matching was performed as follows: treated patients were sorted in descending order, according to their age of treatment initiation; the first treated patient in the sorted list was matched with the sorted untreated patient having the highest last known age; this matched untreated patient was then no longer available for matching with any remaining treated patients; the procedure continues in order through the sorted list of treated patients. Time of treatment start in the untreated patient was set to that of the matched treated patient.
| Figure 1: Kaplan-Meier Survival Curves for Time to Death from Treatment Start in Patients with TK2d Treated with KYGEVVI and Matched Untreated Patients (External control) Treated patients were from Trial 1, Study 1, Study 2, and the expanded access program. Untreated patients were from published literature and Study 2. , Kaplan-Meier Curves with 95% confidence intervals using log-log transformation and with treatment group as strata variable; Age of TK2d Symptom Onset ≤ 12 years. An additional censoring step for untreated subjects in the footnote (b) of Table 4 was performed. |
|
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
KYGEVVI is supplied as follows:
Package 1 of 2
NDC 50474-350-01: Each single use packet contains 4 g of KYGEVVI as a white to off-white powder (2 g doxecitine and 2 g doxribtimine)
NDC 50474-350-30: Carton contains 30 packets
Package 2 of 2
The ZX2000 administration kit for use with KYGEVVI is supplied separately and contains the following:
- One dosing system (includes mixing bottle and dosing cup)
- Two 10 mL oral syringes
- Two spare seals
Storage and Handling
Store KYGEVVI packets at 20°C to 25°C (68°F to 77°F); excursion permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Store reconstituted KYGEVVI solution at controlled room temperature or in the refrigerator. Discard KYGEVVI solution 16 hours after reconstitution or after taking or giving the 3 doses, whichever comes first [see Dosage and Administration (2.5) ].
INSTRUCTIONS FOR USE
KYGEVVI (KY-JEH-vee) (doxecitine and doxribtimine) powder, for oral solution
Table of contents
- Instructions for use
- Important information
- Before you start
- Supplies for preparing and taking or giving KYGEVVI
- Important information
- What you need to know before preparing and taking or giving KYGEVVI
- Storing KYGEVVI packets and oral solution
- Preparing your one-day supply of KYGEVVI
- Get supplies ready
- Measure water and add powder from packets
- Mix and inspect medicine
- Dosing methods
- How to measure your individual dose
- Individual doses 50 mL or more
- Measure and take or give your individual dose
- Individual doses less than 50 mL
- Measure and take or give your individual dose
- Between individual doses
- Clean up after first and second individual dose
- End-of-day clean up
- Pour out and clean up after third individual dose
- Dosing cup maintenance
- Replacing the seal if misplaced or damaged
- Contact information
Instructions For Use
Important information This Instructions for Use contains information on how to prepare a one-day supply of KYGEVVI, and take or give an individual dose of KYGEVVI.
Read this Instructions for Use before taking or giving KYGEVVI and each time you get a refill. There may be new information. This information does not take the place of talking to your healthcare provider about your or your child's medical condition or treatment.
When you are prescribed KYGEVVI for the first time, you will be provided with the carton(s) of 30 KYGEVVI packets and the ZX2000 administration kit (see Figure A ). Only use the dosing cup, mixing bottle, and oral syringes provided with your ZX2000 administration kit. Do not use a household measuring cup or measuring spoon.
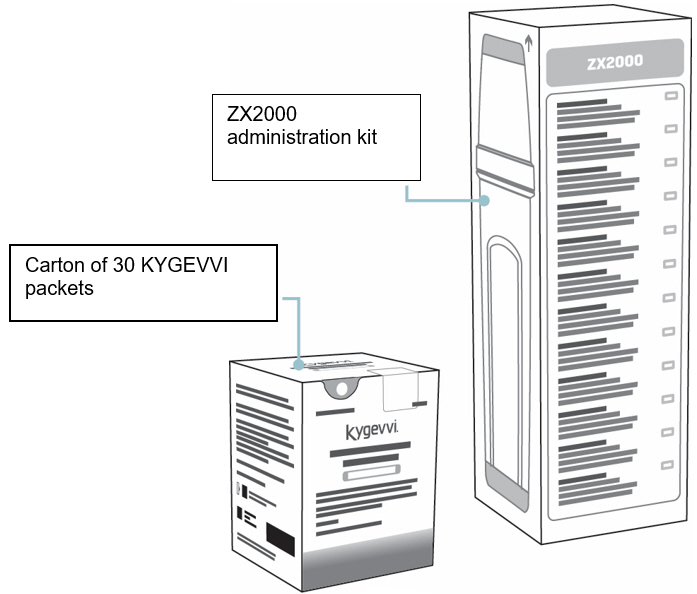 |
| Figure A |
Before you start
Supplies for preparing and taking or giving KYGEVVI Carton of 30 KYGEVVI packets
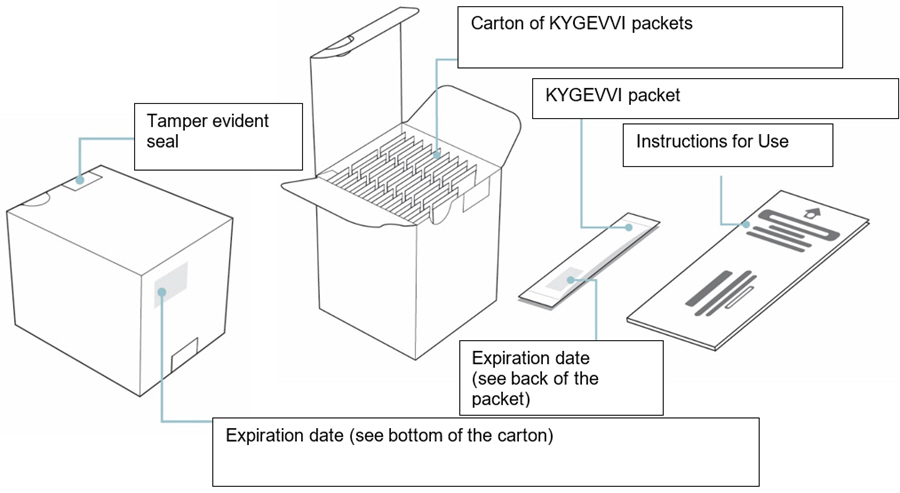
Before you start
Supplies for preparing and taking or giving KYGEVVI
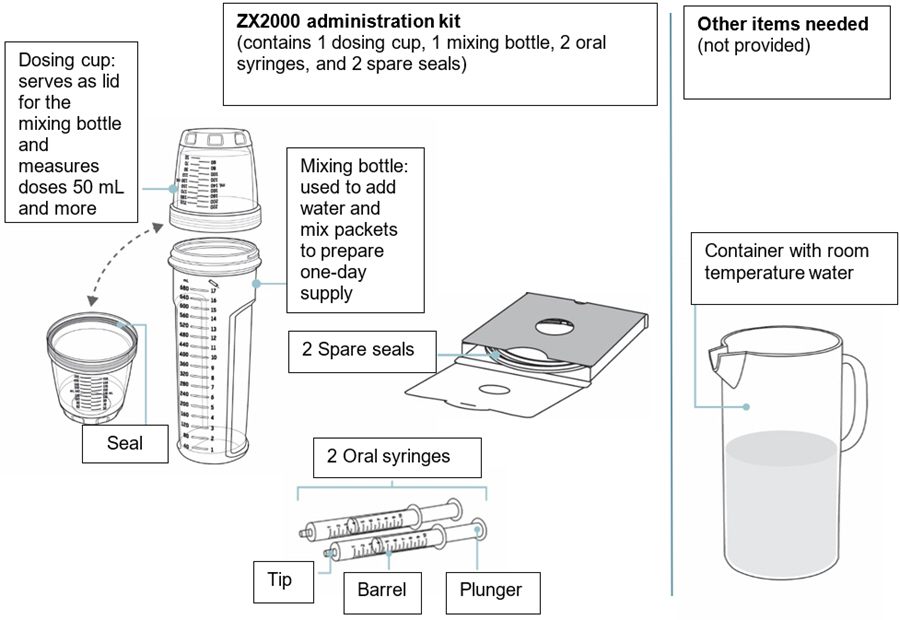
Important information
What you need to know before preparing and taking or giving KYGEVVI
- You will prepare a one-day supply of KYGEVVI solution to be taken in 3 equal doses throughout the day (about 6 hours apart).
- KYGEVVI solution should be prepared on the same day as taking or giving your dose.
- KYGEVVI should be prepared and given by adults only.
- Take or give KYGEVVI exactly as prescribed by your healthcare provider.
- Do not change your dose without talking with your healthcare provider.
- Do not take or give more than the prescribed amount of KYGEVVI solution.
- Take KYGEVVI solution with food.
- Do not use KYGEVVI packets after the expiration date on the packet or carton.
- Only use the dosing cup, mixing bottle, and oral syringes provided with your ZX2000 administration kit. Do not use a household measuring cup or measuring spoon.
- Each ZX2000 administration kit comes with two oral syringes. Keep the second oral syringe as a spare.
- Rinse and dry the mixing bottle and dosing cup before first use. Do not use the dosing cup, mixing bottle, or oral syringe if it appears dirty or damaged.
- Each ZX2000 administration kit can be used for 6 months. Contact your healthcare provider when you need a replacement.
- Contact your healthcare provider or pharmacist for a replacement if your mixing bottle, dosing cup, or oral syringe is damaged or if the markings are missing or no longer readable.
- Do not use the packets if the tamper evident seal on the carton is broken.
- Mix KYGEVVI powder only with room temperature water. Do not mix KYGEVVI powder with any other liquids or foods.
- You may have KYGEVVI solution left over after taking or giving the 3 individual doses. Throw away (discard) any remaining KYGEVVI solution 16 hours after preparing or after taking or giving the 3 doses, whichever comes first.
- If powder spills out of a packet before use, do not use the packet. Throw it away and use a new KYGEVVI packet.
- If KYGEVVI solution comes in contact with your eyes or skin, rinse under cold water and contact your healthcare provider.
|  |
Important information
Storing KYGEVVI packets and oral solution:
- Store KYGEVVI packets at room temperature between 68°F to 77°F (20°C to 25°C).
- Store the prepared KYGEVVI solution at room temperature between 68°F to 77°F (20°C to 25°C) or in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Make sure the dosing cup is screwed on tightly to the mixing bottle when storing your KYGEVVI solution to avoid spills or leaks.
- When storing or carrying the KYGEVVI solution, keep the mixing bottle upright.
- Use the KYGEVVI solution within 16 hours of preparing. Throw away (discard) any remaining solution 16 hours after preparing or after taking or giving the 3 doses, whichever comes first.
- Keep KYGEVVI and all medicines out of the reach of children.
Preparing your one-day supply of KYGEVVI
Get supplies ready
Step 1
- Wash your hands well with soap and water.
- Place the mixing bottle, dosing cup, and oral syringe (if you need one to measure your individual dose) on a clean, well-lit flat work surface. If the dosing cup is attached to the mixing bottle, unscrew it from the mixing bottle and set it down (see Figure B ).
- Make sure "KYGEVVI" appears on the carton.
- Check the expiration date printed on the bottom of the KYGEVVI carton. When opening the KYGEVVI carton for the first time, break the tamper evident seal.
- Remove the prescribed number of KYGEVVI packets needed for your one-day supply of KYGEVVI out of the carton. Your one-day supply of KYGEVVI will be divided into 3 individual doses.
- Do not open the KYGEVVI packets until Step 2.
 |
| Figure B |
Preparing your one-day supply of KYGEVVI
Measure water and add powder from packets
Step 2
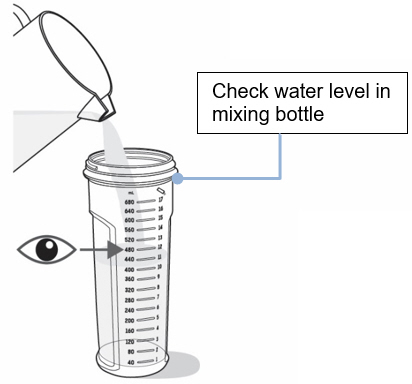
- On a flat surface, pour the prescribed amount of room temperature water into the mixing bottle (see Figure C ).
- Do not pour the water into the dosing cup.
- Important: Do not add the powder from the packets to the mixing bottle before this step.
- Check to make sure the mixing bottle is filled with water up to the marking that matches the amount prescribed by your healthcare provider. The marking should also match the number of packets needed for your one-day supply (see Figure C ).
- Check you have counted out the correct number of KYGEVVI packets for your one-day supply, as shown on your prescription.
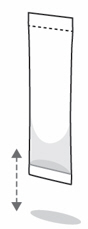
- Tap the packet on a hard surface to settle the powder to the bottom of the packet away from the dotted line (see Figure D ).
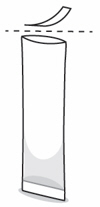
- Carefully fold and tear or cut along the dotted line (see Figure E ). If you spill any powder, do not use it. Throw the packet away and use a new packet.
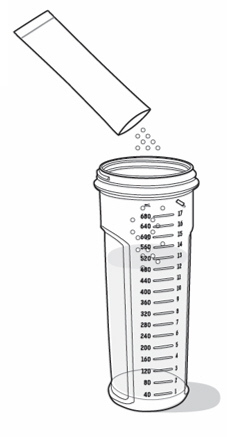
- Empty the entire packet contents into the mixing bottle containing water. Be careful not to drop the packet into the mixing bottle (see Figure F ).
- Pour only 1 packet into the mixing bottle at a time. Repeat Steps 2d to 2f , for each packet until you have poured the prescribed number of packets for your one-day supply.
 |  |  |  |
| Figure C | Figure D | Figure E | Figure F |
Preparing your one-day supply of KYGEVVI
Mix and inspect medicine
Step 3
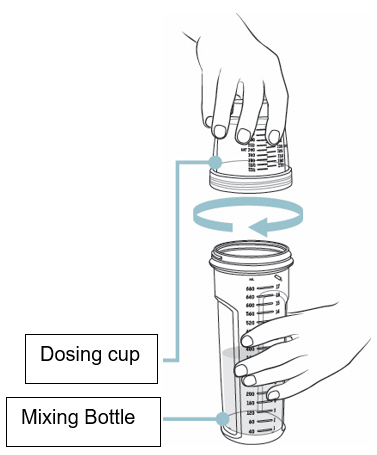
- Screw the dosing cup tightly onto the mixing bottle (see Figure G ).
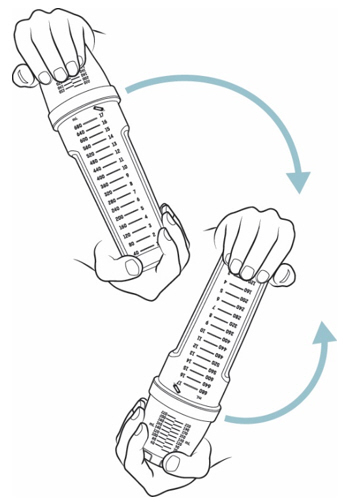
- Place one hand at the end of the mixing bottle and the other hand at the end of the dosing cup. Gently turn the mixing bottle upside down and back at least 20 times (see Figure H ).
- Check the solution. If you see any powder, keep turning the mixing bottle upside down and back until the powder dissolves (see Figure I ).
- The mixed solution may be cloudy and have some remaining powder at the bottom or top. This is normal.
You have now prepared your one-day supply of KYGEVVI solution for 3 individual doses . Take KYGEVVI solution with food .
| Figure G | Figure H | Figure I |
 |  |  |
Dosing methods
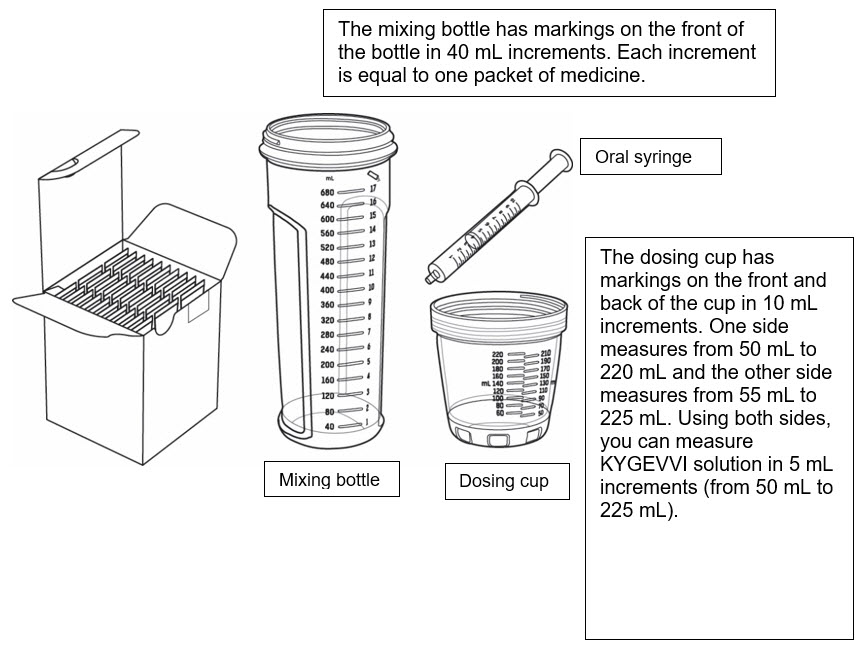
How to measure your individual dose
There are 2 different methods to take or give KYGEVVI solution depending on your individual dose. Use the table below to identify which steps you should follow:
| Individual doses 50 mL or more | Individual doses less than 50 mL (dosing cup used for dose preparation only) |
| Example 100 mL | Example 14 mL |
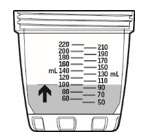 | 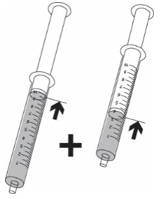 |
| Use dosing cup Follow Step 4 | Use oral syringe Follow Step 5 |
Individual doses 50 mL or more
Measure and take or give your individual dose
Step 4: Dosing cup
- Check to make sure the dosing cup is screwed on tightly to the mixing bottle.
- Mix the already prepared solution by slowly turning the mixing bottle upside down and back at least 3 times.
- Unscrew the dosing cup from the mixing bottle and place it on a flat surface.
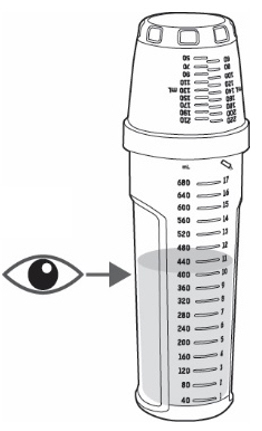
- Pour KYGEVVI solution from the mixing bottle into the dosing cup until it reaches the marking on the dosing cup for your prescribed individual dose (see Figure J ). Note: Your dose may be different than the dose shown in Figure J .
- Drink or give the entire solution from the dosing cup (see Figure K ).
- When it is time for the second or third individual dose , repeat Steps 4a to 4e for each individual dose.
- After the first or second individual dose , go to Step 6 for instructions on how to clean your supplies and store KYGEVVI solution. After the third individual dose , go to Step 7 for instructions on how to clean your supplies and dispose of unused KYGEVVI solution.
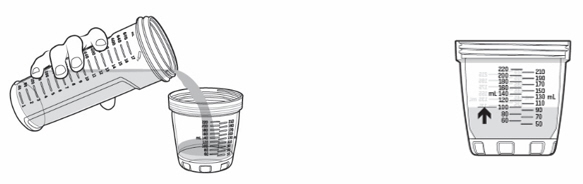 Figure J Figure J |
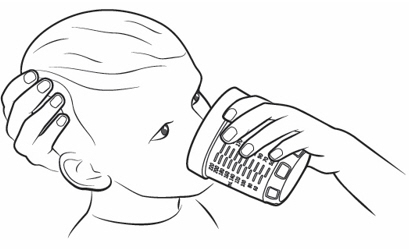 Figure K Figure K |
Individual doses less than 50 mL
Measure and take or give your individual dose
Step 5: Oral syringe
| If your individual dose is more than 10 mL, you will need to use the same oral syringe more than 1 time. |
- Check to make sure the dosing cup is screwed on tightly to the mixing bottle.
- Mix the already prepared solution by slowly turning the mixing bottle upside down and back at least 3 times.
- Unscrew the dosing cup from the mixing bottle and place on a flat surface.
- Pour slightly more than the amount of KYGEVVI solution needed for your prescribed individual dose into the dosing cup (see Figure L ).
- Push the plunger of the oral syringe all the way down to make sure there is no air in the oral syringe when measuring the dose (see Figure M ).
- Place the tip of the oral syringe into the dosing cup with the oral solution. Fill the oral syringe by pulling the plunger back until it reaches the marking on the oral syringe that matches your prescribed individual dose (see Figure N ). Note: If your individual dose is more than 10 mL, you will need to use the same oral syringe more than 1 time. Follow your healthcare provider's instructions on how to measure your dose.
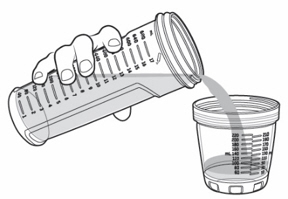 Figure L
Figure L 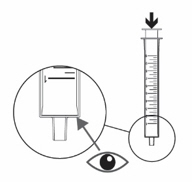 Figure M
Figure M 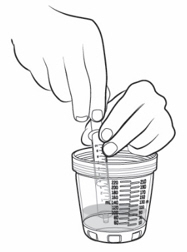 Figure N
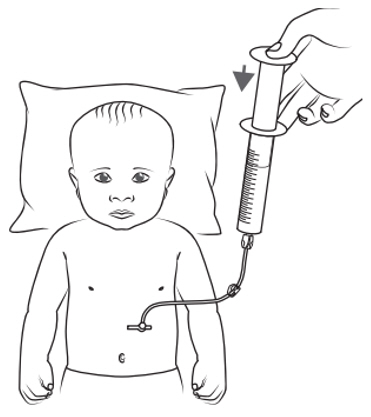
Figure N - Place the tip of the oral syringe into the mouth and point the tip towards the inside of either cheek (see Figure O ).
- If you are giving KYGEVVI to a young child, the child must be seated and held in place to prevent the oral solution from going down the wrong way or choking.
- Slowly push the plunger all the way down until the oral syringe is empty (see Figure O ).
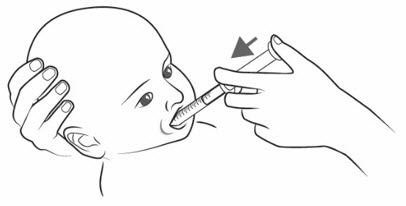 Figure O
Figure O - If your prescribed individual dose is more than 10 mL, repeat Steps 5d to 5h until you take or give the full individual dose.
- Pour back any remaining solution from the dosing cup into the mixing bottle.
- When it is time for the second or third individual dose , repeat Steps 5a to 5j for each individual dose.
- After the first or second individual dose , go to Step 6 for instructions on how to clean your supplies and store KYGEVVI solution. After the third individual dose , go to Step 7 for instructions on how to clean your supplies and dispose of unused KYGEVVI solution.
Between individual doses Clean up after first and second individual dose
Step 6 After you complete the first or second individual dose:
- Rinse the dosing cup with cold water after each use (see Figure P ).
- Dry the dosing cup with a clean, dry towel.
- After the dosing cup is dry, screw the dosing cup tightly onto the mixing bottle (see Figure Q ) and store it at room temperature or in the refrigerator until it is time for the next individual dose.
- If you used the oral syringe, clean it with cold water:
- Rinse the oral syringe with cold water by filling the oral syringe with water and pushing it back out (see Figure R ). Then remove the plunger from the barrel and rinse the plunger and barrel under running tap water until it is clean (see Figure R ).
- Let the oral syringe barrel and plunger dry in the open air. After the oral syringe barrel and plunger are dry, put the plunger back into the barrel.
- Do not wash the dosing cup or oral syringe in the dishwasher.
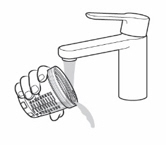 Figure P Figure P | 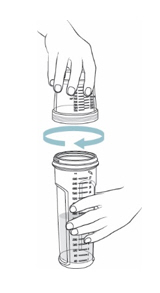 Figure Q Figure Q |
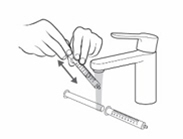 Figure R Figure R |
End-of-day clean up
Pour out and clean up after third individual dose
Step 7 After you take or give the third individual dose, throw away any remaining KYGEVVI solution in the sink. Do not save KYGEVVI solution for another day.
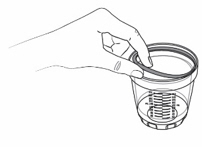
- Remove the seal from the dosing cup to thoroughly clean it (see Figure S ).
- Clean the mixing bottle, dosing cup and seal by hand with soap and warm water. Use a brush to remove any residue left in the mixing bottle or dosing cup (see Figure T ).
- Dry the mixing bottle, dosing cup and seal with a clean towel. Put the dry seal back into the dosing cup, with the thin side of the seal facing the groove.
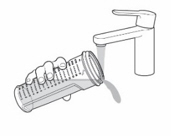
- If you used the oral syringe, clean it with cold water:
- Rinse the oral syringe with cold water by filling the oral syringe with water and pushing it back out (see Figure U ). Then remove the plunger from the barrel and rinse the plunger and barrel under running tap water until it is clean (see Figure U ).
- Let the oral syringe barrel and plunger dry in the open air. After the oral syringe barrel and plunger are dry, put the plunger back into the barrel.
- Do not wash the mixing bottle, dosing cup, seal, or oral syringe in the dishwasher.
- Store all supplies in a clean, dry area out of the reach of children for the next day's use.
 |  | |
| Figure S | Figure T | 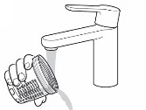 |
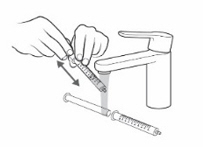 Figure U Figure U | ||
Dosing cup maintenance
Replacing the seal if misplaced or damaged
Changing the dosing cup seal
If you misplace the dosing cup seal or you notice leakage when the dosing cup is screwed on tightly to the mixing bottle, change the seal using one of the two spare seals provided in the ZX2000 administration kit. Follow these steps to replace the seal:
- Remove the seal in the dosing cup (see Figure V ). Skip this step if you misplaced the seal.
- Wash the dosing cup groove with warm water (see Figure W ).
- Get a new seal from the spare seal box (see Figure X ).
- Insert the seal into the groove of the dosing cup with the thin side of the seal facing the groove (see Figure Y ).
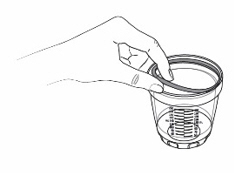 Figure V Figure V | 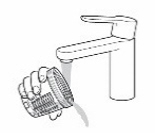 Figure W Figure W |
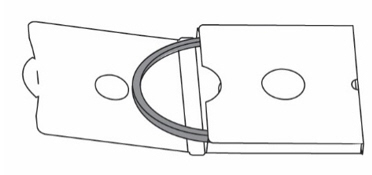 Figure X Figure X | 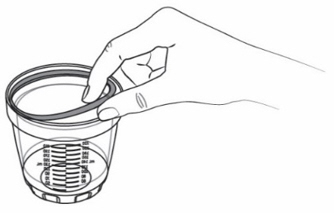 Figure Y Figure Y |
Contact Information
Contact your healthcare provider or pharmacist if you have any questions about this Instructions for Use. You may also contact UCBCares at 1-844-599-CARE (2273) for assistance.
KYGEVVI manufactured for: UCB, Inc., Smyrna, GA 30080 This Instructions for Use has been approved by the U.S. Food and Drug Administration. Approved: 11/2025
Mechanism of Action
Administration of KYGEVVI is intended to incorporate the pyrimidine nucleosides, deoxycytidine and deoxythymidine, into skeletal muscle mitochondrial deoxyribonucleic acid (DNA). This action restores mitochondrial DNA copy number in TK2d mutant mice.