Get your patient on Furosemide - Furosemide injection, Solution (Furosemide)
Furosemide - Furosemide injection, Solution prescribing information
WARNING
Furosemide is a potent diuretic which, if given in excessive amounts, can lead to a profound diuresis with water and electrolyte depletion. Therefore, careful medical supervision is required and dose and dose schedule must be adjusted to the individual patient's needs. (See DOSAGE AND ADMINISTRATION .)
INDICATIONS AND USAGE
Parenteral therapy should be reserved for patients unable to take oral medication or for patients in emergency clinical situations.
Edema: Furosemide is indicated in adults and pediatric patients for the treatment of edema associated with congestive heart failure, cirrhosis of the liver, and renal disease, including the nephrotic syndrome. Furosemide is particularly useful when an agent with greater diuretic potential is desired.
Furosemide is indicated as adjunctive therapy in acute pulmonary edema. The intravenous administration of furosemide is indicated when a rapid onset of diuresis is desired, e.g., in acute pulmonary edema.
If gastrointestinal absorption is impaired or oral medication is not practical for any reason, furosemide is indicated by the intravenous or intramuscular route. Parenteral use should be replaced with oral furosemide as soon as practical.
DOSAGE AND ADMINISTRATION
Adults: Parenteral therapy with Furosemide Injection should be used only in patients unable to take oral medication or in emergency situations and should be replaced with oral therapy as soon as practical.
Edema
The usual initial dose of furosemide is 20 to 40 mg given as a single dose, injected intramuscularly or intravenously. The intravenous dose should be given slowly (1 to 2 minutes). Ordinarily a prompt diuresis ensues. If needed, another dose may be administered in the same manner 2 hours later or the dose may be increased. The dose may be raised by 20 mg and given not sooner than 2 hours after the previous dose until the desired diuretic effect has been obtained. This individually determined single dose should then be given once or twice daily. Therapy should be individualized according to patient response to gain maximal therapeutic response and to determine the minimal dose needed to maintain that response. Close medical supervision is necessary.
When furosemide is given for prolonged periods, careful clinical observation and laboratory monitoring are particularly advisable. (See PRECAUTIONS: Laboratory Tests .)
If the physician elects to use high dose parenteral therapy, add the furosemide to either Sodium Chloride Injection USP, Lactated Ringer's Injection USP, or Dextrose (5%) Injection USP after pH has been adjusted to above 5.5, and administer as a controlled intravenous infusion at a rate not greater than 4 mg/min. Furosemide Injection is a buffered alkaline solution with a pH of about 9 and drug may precipitate at pH values below 7. Care must be taken to ensure that the pH of the prepared infusion solution is in the weakly alkaline to neutral range. Acid solutions, including other parenteral medications (e.g., labetalol, ciprofloxacin, amrinone, milrinone) must not be administered concurrently in the same infusion because they may cause precipitation of the furosemide. In addition, furosemide injection should not be added to a running intravenous line containing any of these acidic products.
Acute Pulmonary Edema
The usual initial dose of furosemide is 40 mg injected slowly intravenously (over 1 to 2 minutes). If a satisfactory response does not occur within 1 hour, the dose may be increased to 80 mg injected slowly intravenously (over 1 to 2 minutes).
If necessary, additional therapy (e.g., digitalis, oxygen) may be administered concomitantly.
Geriatric Patients
In general, dose selection for the elderly patient should be cautious, usually starting at the low end of the dosing range. (See PRECAUTIONS: Geriatric Use .)
CONTRAINDICATIONS
Furosemide is contraindicated in patients with anuria and in patients with a history of hypersensitivity to furosemide.
ADVERSE REACTIONS
Adverse reactions are categorized below by organ system and listed by decreasing severity.
Gastrointestinal System Reactions
1.Hepatic encephalopathy in patients with hepatocellular insufficiency 2.Pancreatitis 3.Jaundice (intrahepatic cholestatic jaundice) 4.Increased liver enzymes 5.Anorexia 6.Oral and gastric irritation 7.Cramping 8.Diarrhea 9.Constipation 10.Nausea 11.Vomiting
Systemic Hypersensitivity Reactions
1.Severe anaphylactic or anaphylactoid reactions (e.g. with shock) 2.Systemic vasculitis 3.Interstitial nephritis 4.Necrotizing angiitis
Central Nervous System Reactions
1.Tinnitus and hearing loss 2.Paresthesias 3.Vertigo 4.Dizziness 5.Headache 6.Blurred vision 7.Xanthopsia
Hematologic Reactions
1.Aplastic anemia 2.Thrombocytopenia 3.Agranulocytosis 4.Hemolytic anemia 5.Leukopenia 6.Anemia 7.Eosinophilia
Dermatologic-Hypersensitivity Reactions
1.Exfoliative dermatitis 2.Bullous pemphigoid 3.Erythema multiforme 4.Purpura 5.Photosensitivity 6.Urticaria 7.Rash 8.Pruritus 9.Stevens-Johnson Syndrome 10.Toxic epidermal necrolysis
Cardiovascular Reaction
1.Orthostatic hypotension may occur and be aggravated by alcohol, barbiturates or narcotics. 2.Increase in cholesterol and triglyceride serum levels.
Other Reactions
1.Hyperglycemia 2.Glycosuria 3.Hyperuricemia 4.Muscle spasm 5.Weakness 6.Restlessness 7.Urinary bladder spasm 8.Thrombophlebitis 9.Transient injection site pain following intramuscular injection 10.Fever
Whenever adverse reactions are moderate or severe, furosemide dosage should be reduced or therapy withdrawn.
To report SUSPECTED ADVERSE REACTIONS, contact Devatis Inc. at 1-833-534-4406 or druginfo@devatis.com or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch or www.devatis.com.
Drug Interactions: Furosemide may increase the ototoxic potential of aminoglycoside antibiotics, especially in the presence of impaired renal function. Except in life-threatening situations, avoid the combination.
Furosemide should not be used concomitantly with ethacrynic acid because of the possibility of ototoxicity.
Patients receiving high doses of salicylates concomitantly with furosemide, as in rheumatic diseases, may experience salicylate toxicity at lower doses because of competitive renal excretory sites.
There is a risk of ototoxic effects if cisplatin and furosemide are given concomitantly. In addition, nephrotoxicity of nephrotoxic drugs such as cisplatin may be enhanced if furosemide is not given in lower doses and with positive fluid balance when used to achieve forced diuresis during cisplatin treatment.
Furosemide has a tendency to antagonize the skeletal muscle relaxing effect of tubocurarine and may potentiate the action of succinylcholine.
Lithium generally should not be given with diuretics because they reduce lithium's renal clearance and add a high risk of lithium toxicity.
Furosemide combined with angiotensin converting enzyme inhibitors or angiotensin II receptor blockers may lead to severe hypotension and deterioration in renal function, including renal failure. An interruption or reduction in the dosage of furosemide, angiotensin converting enzyme inhibitors, or angiotensin receptor blockers may be necessary.
Furosemide may add to or potentiate the therapeutic effect of other antihypertensive drugs. Potentiation occurs with ganglionic or peripheral adrenergic blocking drugs.
Furosemide may decrease arterial responsiveness to norepinephrine. However, norepinephrine may still be used effectively.
In isolated cases, intravenous administration of furosemide within 24 hours of taking chloral hydrate may lead to flushing, sweating attacks, restlessness, nausea, increase in blood pressure, and tachycardia. Use of furosemide concomitantly with chloral hydrate is therefore not recommended.
Phenytoin interferes directly with renal action of furosemide.
Methotrexate and other drugs that, like furosemide, undergo significant renal tubular secretion may reduce the effect of furosemide. Conversely, furosemide may decrease renal elimination of other drugs that undergo tubular secretion. High-dose treatment of both furosemide and these other drugs may result in elevated serum levels of these drugs and may potentiate their toxicity as well as the toxicity of furosemide.
Furosemide can increase the risk of cephalosporin-induced nephrotoxicity even in the setting of minor or transient renal impairment.
Concomitant use of cyclosporine and furosemide is associated with increased risk of gouty arthritis secondary to furosemide-induced hyperuricemia and cyclosporine impairment of renal urate excretion.
One study in six subjects demonstrated that the combination of furosemide and acetylsalicylic acid temporarily reduced creatinine clearance in patients with chronic renal insufficiency. There are case reports of patients who developed increased BUN, serum creatinine and serum potassium levels, and weight gain when furosemide was used in conjunction with NSAIDs.
Literature reports indicate that coadministration of indomethacin may reduce the natriuretic and antihypertensive effects of furosemide in some patients by inhibiting prostaglandin synthesis. Indomethacin may also affect plasma renin levels, aldosterone excretion, and renin profile evaluation. Patients receiving both indomethacin and furosemide should be observed closely to determine if the desired diuretic and/or antihypertensive effect of furosemide is achieved.
DESCRIPTION
Furosemide is a diuretic which is an anthranilic acid derivative.
Chemically, it is 4-chloro -N -furfuryl-5-sulfamoylanthranilic acid.
Furosemide Injection 10 mg/mL is a sterile, non-pyrogenic solution in vials for intravenous and intramuscular injection.
Furosemide is a white to off-white odorless crystalline powder. It is practically insoluble in water, sparingly soluble in alcohol, freely soluble in dilute alkali solutions and insoluble in dilute acids.
The structural formula is as follows:
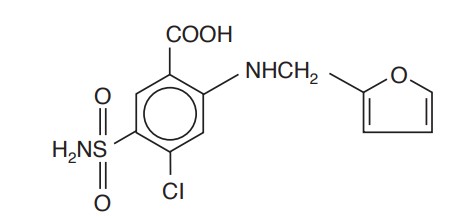
E ach mL contains: Furosemide 10 mg, Water for Injection q.s., Sodium Chloride for isotonicity, Sodium Hydroxide and, if necessary, Hydrochloric Acid to adjust pH between 8.0 and 9.3.
CLINICAL PHARMACOLOGY
Investigations into the mode of action of furosemide have utilized micropuncture studies is rats, stop flow experiments in dogs and various clearance studies in both humans and experimental animals. It has been demonstrated that furosemide inhibits primarily the reabsorption of sodium and chloride not only in the proximal and distal tubules but also in the loop of Henle. The high degree of efficacy is largely due to this unique site of action. The action on the distal tubule is independent of any inhibitory effect on carbonic anhydrase and aldosterone.
Recent evidence suggests that furosemide glucuronide is the only or at least the major biotransformation product of furosemide in man. Furosemide is extensively bound to plasma proteins, mainly to albumin. Plasma concentrations ranging from 1 to 400 μg/mL are 91 to 99% bound in healthy individuals. The unbound fraction averages 2.3 to 4.1% at therapeutic concentrations.
The onset of diuresis following intravenous administration is within 5 minutes and somewhat later after intramuscular administration. The peak effect occurs within the first half hour. The duration of diuretic effect is approximately 2 hours.
In fasted normal men, the mean bioavailability of furosemide from furosemide tablets and furosemide oral solution is 64 % and 60%, respectively, of that from an intravenous injection of the drug. Although furosemide is more rapidly absorbed from the oral solution (50 minutes) than from the tablet (87 minutes), peak plasma levels and area under the plasma concentration-time curves do not differ significantly. Peak plasma concentrations increase with increasing dose but times-to-peak do not differ among doses. The terminal half-life of furosemide is approximately 2 hours.
Significantly more furosemide is excreted in urine following the intravenous injection than after the tablet or oral solution. There are no significant differences between the two oral formulations in the amount of unchanged drug excreted in urine.
HOW SUPPLIED
Furosemide Injection, USP (10 mg/mL)
NDC-73043-022-01 | 2 mL single dose amber colored vials | Boxes of 25 |
NDC-73043-023-01 | 4 mL single dose amber colored vials | Boxes of 25 |
NDC-73043-024-01 | 10 mL single dose amber colored vials | Boxes of 25 |
NDC-73043-025-01 | 2 mL single dose amber colored ampoules | Boxes of 25 |
NDC-73043-026-01 | 4 mL single dose amber colored ampoules | Boxes of 25 |
Do not use if solution is discolored. Store at 20° to 25°C (68° to 77°F) ; excursions permitted to 15˚ to 30˚C (59˚ to 86˚F) [see USP Controlled Room Temperature]
Protect from light.
Made in Turkey
Distributed by: Devatis, Inc. San Clemente, CA 92672
Revised: 10/2024
KTP6643KT-01
Furosemide - Furosemide injection, Solution PubMed™ news
- Journal Article • 2026 MayComparison of loop diuretics for chronic heart failure: a systematic review and meta-analysis.
- Journal Article • 2026 MaySafety and Feasibility of the eLymTM System for Interstitial Decongestion in Acute Decompensated Heart Failure: Primary results of the DELTA-HF trial.
- Journal Article • 2026 MayFurosemide stress test predicts discontinuation of continuous renal replacement treatments in critically ill patients with acute kidney injury: a prospective multicenter trial.
- Journal Article • 2026 MayA Novel, Interpretable Machine Learning Model Predicts Furosemide Dosing After Congenital Cardiac Surgery.
- Journal Article • 2026 MayDilated Cardiomyopathy Phenotype With Global (Four-Chamber) Involvement in a Cat: Echocardiographic, Pathological, Histopathological, and Immunohistochemical Findings.