Get your patient on Ferriprox - Deferiprone tablet (Deferiprone)
Ferriprox - Deferiprone tablet prescribing information
WARNING: AGRANULOCYTOSIS AND NEUTROPENIA
• FERRIPROX can cause agranulocytosis that can lead to serious infections and death. Neutropenia may precede the development of agranulocytosis. [see Warnings and Precautions (5.1 )]
• Measure the absolute neutrophil count (ANC) before starting FERRIPROX therapy and monitor regularly while on therapy.
• Interrupt FERRIPROX therapy if neutropenia develops. [see Warnings and Precautions (5.1 )]
• Interrupt FERRIPROX if infection develops, and monitor the ANC more frequently. [see Warnings and Precautions (5.1 )]
• Advise patients taking FERRIPROX to report immediately any symptoms indicative of infection. [see Warnings and Precautions (5.1 )]
1 INDICATIONS AND USAGE
FERRIPROX Tablets are indicated for the treatment of transfusional iron overload in adult and pediatric patients 8 years of age and older with thalassemia syndromes, sickle cell disease or other anemias.
Limitation s of Use
• Safety and effectiveness have not been established for the treatment of transfusional iron overload in patients with myelodysplastic syndrome or in patients with Diamond Blackfan anemia.
2 DOSAGE AND ADMINISTRATION
2.1 Important Dosage and Administration Information
FERRIPRO X T ablets are available in two different 1,000 mg formulations , which have different oral dosing regimens to achieve the same total daily dosage.
- FERRIPROX Tablets (twice a day) - 1,000 mg - given two times a day [see Dosage and Administration (2.2 )]
- FERRIPROX Tablets (three times a day) - 1,000 mg - given three times a day [see Dosage and Administration (2.3 )]
To prevent medication errors, before prescribing and dispensing, ensure that the tablet formulation is appropriate for the dosing regimen. Each tablet has distinct identifying characteristics [see Dosage Forms and Strengths (3 )].
For patients who have trouble swallowing tablets, consider the use of FERRIPROX Oral Solution (see the prescribing information for FERRIPROX Oral Solution).
Monitoring for Safety
Due to the risk of agranulocytosis, monitor ANC before and during FERRIPROX therapy.
Test ANC prior to start of FERRIPROX therapy and monitor on the following schedule during treatment:
• First six months of therapy: Monitor ANC weekly;
• Next six months of therapy: Monitor ANC once every two weeks;
• After one year of therapy: Monitor ANC every two to four weeks (or at the patient’s blood transfusion interval in patients that have not experienced an interruption due to any decrease in ANC [see Warnings and Precautions (5.1 )] .
Due to the risk of hepatic transaminase elevations, monitor ALT before and monthly during FERRIPROX therapy [see Warnings and Precautions (5.2 )] .
Due to the risk of zinc deficiency, monitor zinc levels before and regularly during FERRIPROX therapy [see Warnings and Precautions (5.3 )] .
2.2 Recommended Dosage for 1,000 mg FERRIPROX T ablets ( twice a day) for Adult and Pediatric Patients with Transfusional Iron Overload due to Thalassemia Syndromes, Sickle Cell Disease or Other Anemias
Starting Dos ag e for T wice a Day Tablets
The recommended starting oral dosage of FERRIPROX Tablets (twice a day) is 75 mg/kg/day (actual body weight) in two divided doses per day (taken approximately 12 hours apart), with food. Round the total daily dose to the nearest 500 mg (half-tablet). Table 1 describes the number of FERRIPROX Tablets (twice a day) needed to achieve the 75 mg/kg/day total starting daily dosage.
| Table 1 : Number of FERRIPROX 1,000 mg T ablets (twice a day) Needed to Achieve the Total Starting Daily Dosage of 75 mg/k g (rounded to the nearest half-tablet) | ||
| Body Weight (kg) | Morning | Evening |
| 20 | 0.5 | 1 |
| 30 | 1 | 1.5 |
| 40 | 1.5 | 1.5 |
| 50 | 2 | 2 |
| 60 | 2 | 2.5 |
| 70 | 2.5 | 3 |
| 80 | 3 | 3 |
| 90 | 3.5 | 3.5 |
To minimize gastrointestinal upset when first starting therapy, dosing can start at 45 mg/kg/day and increase weekly by 15 mg/kg/day increments until the full prescribed dose is achieved.
Dos ag e Adjustment s for T wice a Day Tablets
Tailor dosage adjustments of FERRIPROX Tablets (twice a day) to the individual patient’s response and therapeutic goals (maintenance or reduction of body iron burden). The maximum total daily oral dosage is 99 mg/kg (actual body weight) divided into two doses taken approximately 12 hours apart with food. Table 2 describes the number of FERRIPROX Tablets (twice a day) needed to achieve the 99 mg/day total maximum daily dosage.
| Table 2 : Number of FERRIPROX 1,000 mg Tablets (twice a day) Needed to A chieve a Total Maximum Recommended Daily Dosage of 99 mg/kg (rounded to the nearest half-tablet) | ||
| Body Weight (kg) | Morning | Evening |
| 20 | 1 | 1 |
| 30 | 1.5 | 1.5 |
| 40 | 2 | 2 |
| 50 | 2.5 | 2.5 |
| 60 | 3 | 3 |
| 70 | 3.5 | 3.5 |
| 80 | 4 | 4 |
| 90 | 4.5 | 4.5 |
2 .3 Recommended Dos age for 1,000 mg FERRIPROX T ablets (three times a day) for Adult and Pediatric Patients with Transfusional Iron Overload due to Thalassemia Syndromes, Sickle Cell Disease or Other Anemias
Starting Dos ag e for Three Times a Day Tablets
The recommended starting oral dosage of FERRIPROX Tablets (three times a day) is 75 mg/kg/day (actual body weight), in three divided doses per day. Table 3 describes the number of FERRIPROX Tablets (three times a day) needed to achieve the 75 mg/kg/day total starting dosage). Round dose to the nearest 500 mg (half-tablet).
| Table 3 : Number of F ERRIPROX 1,000 mg T ablets (three times a day) Needed to Achieve the Total Starting Daily Dosage of 75 mg/kg (rounded to the nearest half-tablet) | |||
| Body Weight (kg) | Morning | Midday | Evening |
| 20 | 0.5 | 0.5 | 0.5 |
| 30 | 1 | 0.5 | 1 |
| 40 | 1 | 1 | 1 |
| 50 | 1.5 | 1 | 1.5 |
| 60 | 1.5 | 1.5 | 1.5 |
| 70 | 2 | 1.5 | 2 |
| 80 | 2 | 2 | 2 |
| 90 | 2.5 | 2 | 2.5 |
To minimize gastrointestinal upset when first starting therapy, dosing can start at 45 mg/kg/day and increase weekly by 15 mg/kg/day increments until the full prescribed dose is achieved.
Dosage Adjustments for Three Times Daily Tablets
Tailor dosage adjustments for FERRIPROX Tablets (three times a day) to the individual patient’s response and therapeutic goals (maintenance or reduction of body iron burden). The maximum oral dosage is 99 mg/kg/day (actual body weight), in three divided doses per day. Table 4 describes the number of FERRIPROX Tablets (three times a day) needed to achieve the 99 mg/day total maximum daily dosage.
| Table 4: Number of FERRIPROX 1,000 mg Tablets (three times a day) Needed to Achieve the Maximum Total Daily Dosage of 99 mg/kg (rounded to the nearest half-tablet) | |||
| Body Weight (kg) | Morning | Midday | Evening |
| 20 | 0.5 | 0.5 | 1 |
| 30 | 1 | 1 | 1 |
| 40 | 1.5 | 1 | 1.5 |
| 50 | 1.5 | 1.5 | 2 |
| 60 | 2 | 2 | 2 |
| 70 | 2.5 | 2 | 2.5 |
| 80 | 2.5 | 2.5 | 3 |
| 90 | 3 | 3 | 3 |
2.4 Monitoring Ferritin Levels to Assess Efficacy
Monitor serum ferritin concentration every two to three months to assess the effect of FERRIPROX on body iron stores. If the serum ferritin is consistently below 500 mcg/L, consider temporarily interrupting FERRIPROX therapy until serum ferritin rises above 500 mcg/L.
2.000000000000000e+00 5 Dosage Modification for Drug Interactions
3 DOSAGE FORMS AND STRENGTHS
- Tablets (twice a day): 1,000 mg, capsule-shaped, white to off-white tablets with functional scoring, engraved “FPX” bisect “DR” on one side, “APO” bisect “1000” on the other”.
- Tablets (three times a day): 1,000 mg film-coated, capsule-shaped, white to off-white tablets with functional scoring, and imprinted with “APO” score “1000” on one side and plain on the other.
8 USE IN SPECIFIC POPULATION S
8.1 Pregnancy
Risk Summary
In animal reproduction studies, oral administration of deferiprone to pregnant rats and rabbits during organogenesis at doses 33% and 49%, respectively, of the maximum recommended human dose (MRHD) resulted in structural abnormalities, embryo-fetal mortality and alterations to growth (see Data) . The limited available data from deferiprone use in pregnant women are insufficient to inform a drug-associated risk of major birth defects and miscarriage. Based on evidence and developmental toxicity in animal studies, FERRIPROX can cause fetal harm when administered to a pregnant woman. Advise pregnant women and females of reproductive potential of the potential risk to a fetus.
The estimated background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss, or other adverse outcomes . In the U.S. general population, the estimated background risk of major birth defects and of miscarriage is 2-4% and 15-20%, respectively.
Data
Human Data
Post-marketing data available from 39 pregnancies of deferiprone-treated patients and 10 pregnancies of partners of deferiprone-treated patients are as follows:
Of the 39 pregnancies in deferiprone-treated patients, 23 resulted in healthy newborns, 6 ended in spontaneous abortion, 9 had unknown outcomes, and 1 infant was born with anal atresia, nephroptosis, ventricular septal defect, hemivertebra and urethral fistula.
Of the 10 pregnancies in partners of deferiprone-treated patients, 5 resulted in healthy newborns, 1 resulted in a healthy newborn with slight hypospadias, 1 was electively terminated, 1 resulted in the intrauterine death of twins, and 2 had unknown outcomes.
Animal Data
During organogenesis, pregnant rats and rabbits received deferiprone at oral doses of 0, 30, 80 or 200 mg/kg/day, and 0, 10, 50, or 150 mg/kg/day, respectively. The daily dose was administered as two equal divided doses approximately 7 hours apart. Doses of 200 mg/kg/day in rats and 150 mg/kg/day in rabbits, approximately 33% and 49% of the MRHD, respectively, resulted in increased post-implantation loss and reduced fetal weights in the presence of maternal toxicity (reduced maternal body weight and body weight gain in both rats and rabbits; abnormal large placenta at low incidence in rats). The 200 mg/kg/day dose in rats resulted in external, visceral and skeletal fetal malformations such as cranial malformations, cleft palate, limb malrotation, anal atresia, internal hydrocephaly, anophthalmia and fused bones. The dose of 150 mg/kg/day in rabbits resulted in external fetal malformations (partially opened eyes) and minor blood vessel and skeletal variations.
In rats, malformations including micrognathia and persistent ductus arteriosus could be observed in the absence of maternal toxicity at doses equal to or greater than 30 and 80 mg/kg/day, approximately 5% and 13% of the MHRD, respectively.
8.2 Lactation
Risk Summary
There is no information regarding the presence of deferiprone in human milk, the effects on the breastfed child, or the effects on milk production.
Because of the potential for serious adverse reactions in the breastfed child, including the potential for tumorigenicity shown for deferiprone in animal studies, advise patients that breastfeeding is not recommended during treatment with FERRIPROX, and for at least 2 weeks after the last dose.
8.3 Females and Males of Reproductive Potential
Pregnancy Testing
Pregnancy testing is recommended for females of reproductive potential prior to initiating FERRIPROX.
Contraception
Females
FERRIPROX can cause embryo-fetal harm when administered to a pregnant woman [see Use in Specific Populations (8.1 )] . Advise female patients of reproductive potential to use effective contraception during treatment with FERRIPROX and for at least 6 months after the last dose.
Males
Based on genotoxicity findings, advise males with female partners of reproductive potential to use effective contraception during treatment with FERRIPROX and for at least 3 months after the last dose [ see Nonclinical Toxicology (13.1 ) ] .
8.4 Pediatric Use
The safety and effectiveness of FERRIPROX for the treatment of transfusional iron overload due to thalassemia syndromes have been established in pediatric patients 8 years of age and older. Use of FERRIPROX for this indication is supported by evidence of efficacy from clinical trials in adult patients with thalassemia and evidence of safety in pediatric patients with sickle cell disease.
The safety and effectiveness of FERRIPROX for the treatment of transfusional iron overload due to sickle cell disease or other anemias have been established in 86 pediatric patients 3 to 16 years of age, among the 152 patients treated with FERRIPROX Tablets or Oral Solution in an adequate and well-controlled study [see Adverse Reactions (6.1 ) and Clinical Studies (14.2 )] . The study included 56 patients 3 to <12 years of age and 30 patients 12 to 16 years of age. Seventy-six percent of these patients had sickle cell disease. The recommended starting dose and dose-modifications are the same for children and adults [see Indications and Usage (1 ), Dosage and Administration (2.1 ), and Clinical Studies (14 ) ].
Fourteen patients with spherocytosis (including hereditary) (ages 3-15), two patients with pyruvate kinase deficiency (ages 4 and 6), two patients with dyserythropoietic anemia (ages 10-12) and two patients with hemolytic anemia (ages 8 and 10 years old) were treated with FERRIPROX in the clinical trial, LA38-0411.
A US registry established from December 2011 through December 2019, contains 125 patients from 4 to < 17 years old who have received FERRIPROX and have sickle cell disease. The adverse reactions, including agranulocytosis, seen in the 8 year period of the registry are similar to those seen in the most recent clinical studies.
Safety and effectiveness of FERRIPROX Tablets have not been established in pediatric patients with chronic iron overload due to blood transfusions who are less than 8 years of age.
8.5 Geriatric Use
Clinical studies of deferiprone did not include sufficient numbers of subjects aged 65 and over to determine whether they respond differently from younger subjects. Other reported clinical experience has not identified differences in responses between the elderly and younger patients.
4 CONTRAINDICATIONS
FERRIPROX is contraindicated in patients with known hypersensitivity to deferiprone or to any of the excipients in the formulations. The following reactions have been reported in association with the administration of deferiprone: Henoch-Schönlein purpura; urticaria; and periorbital edema with skin rash [ see Adverse Reactions (6.2 )] .
5 WARNINGS AND PRECAUTIONS
5.1 Agranulocytosis and Neutropenia
Fatal agranulocytosis can occur with FERRIPROX use. FERRIPROX can also cause neutropenia, which may foreshadow agranulocytosis. Measure the absolute neutrophil count (ANC) before starting FERRIPROX therapy and monitor it regularly while on therapy [see Dosage and Administration (2.1 )] .
Reduction in the frequency of ANC monitoring should be considered on an individual patient basis, according to the health care provider’s assessment of the patient’s understanding of the risk minimization measures required during therapy.
Interrupt FERRIPROX therapy if neutropenia develops (ANC < 1.5 x 10 9 /L).
Interrupt FERRIPROX if infection develops and monitor the ANC frequently.
Advise patients taking FERRIPROX to immediately interrupt therapy and report to their physician if they experience any symptoms indicative of infection.
The incidence of agranulocytosis was 1% of patients in pooled clinical trials of 642 patients with thalassemia syndromes and 0.5% of patients in pooled clinical trials of 196 patients with sickle cell disease or other anemias. The mechanism of FERRIPROX-associated agranulocytosis is unknown. Agranulocytosis and neutropenia usually resolve upon discontinuation of FERRIPROX, but there have been reports of agranulocytosis leading to death.
Implement a plan to monitor for and to manage agranulocytosis and neutropenia prior to initiating FERRIPROX treatment.
For agranulocytosis (ANC < 0.2 x 10 9 /L) and severe neutropenia (0.2 x 10 9 /L ≤ ANC < 0.5 x 10 9 /L):
Consider hospitalization and other management as clinically appropriate.
Do not resume FERRIPROX in patients who have developed agranulocytosis unless potential benefits outweigh potential risks. Do not rechallenge patients who have developed neutropenia with FERRIPROX unless potential benefits outweigh potential risks.
For neutropenia (ANC < 1.5 x 10 9 /L and ≥ 0.5 x 10 9 /L):
Instruct the patient to immediately discontinue FERRIPROX and all other medications with a potential to cause neutropenia.
Obtain a complete blood cell (CBC) count, including a white blood cell (WBC) count corrected for the presence of nucleated red blood cells, an absolute neutrophil count (ANC), and a platelet count daily until recovery (ANC ≥ 1.5 x 10 9 /L).
5.000000000000000e+00 2 Liver Enzyme Elevations
In pooled clinical trials, 7.5% of 642 patients with thalassemia syndromes treated with FERRIPROX developed increased ALT values. Four (0.62%) FERRIPROX-treated subjects discontinued the drug due to increased serum ALT levels and 1 (0.16%) due to an increase in both ALT and AST. In pooled clinical trials, 7.7% of 196 patients with sickle cell disease or other anemias treated with FERRIPROX developed increased ALT values.
Monitor serum ALT values monthly during therapy with FERRIPROX and consider interruption of therapy if there is a persistent increase in the serum transaminase levels [see Dosage and Administration (2.1 )] .
5.000000000000000e+00 3 Zinc Deficiency
Decreased plasma zinc concentrations have been observed on FERRIPROX therapy. Monitor plasma zinc annually, and supplement in the event of a deficiency [see Dosage and Administration (2.1 )] .
5.4 Embryo -F etal Toxicity
Based on findings from animal reproduction studies and evidence of genotoxicity, FERRIPROX can cause fetal harm when administered to a pregnant woman. The available data on the use of FERRIPROX in pregnant women are insufficient to inform risk. In animal studies, administration of deferiprone during the period of organogenesis resulted in embryo-fetal death and malformations at doses lower than equivalent human clinical doses. Advise pregnant women and females of reproductive potential of the potential risk to the fetus [see Use in Specific Populations (8.1 )] .
Advise females of reproductive potential to use an effective method of contraception during treatment with FERRIPROX and for at least six months after the last dose. Advise males with female partners of reproductive potential to use effective contraception during treatment with FERRIPROX and for at least three months after the last dose [ see Use in Specific Populations (8.1 , 8.3 ) ] .
6 ADVERSE REACTIONS
The following clinically significant adverse reactions are described below and elsewhere in the labeling:
6.1 Clinical Trial Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
FERRIPROX Tablets (twice a day) were evaluated in trials in healthy subjects. FERRIPROX Tablets (twice a day) contain deferiprone, the same active ingredient as FERRIPROX Tablets (deferiprone) (three times a day) and FERRIPROX Oral Solution (deferiprone).
The following adverse reaction information represents the pooled data collected from single arm or active-controlled clinical trials with FERRIPROX Tablets (deferiprone) (three times a day) or FERRIPROX Oral Solution (deferiprone).
Thalassemia Syndromes
The safety of FERRIPROX was evaluated in the pooled clinical trial database [see Clinical Studies (14.1 )] . Patients received FERRIPROX Tablets (three times a day) or FERRIPROX Oral Solution . FERRIPROX was administered orally three times a day (total daily dose either 50, 75, or 99 mg/kg), N=642. Among 642 patients receiving FERRIPROX, 492 (76.6%) were exposed for 6 months or longer and 365 (56.9%) were exposed for greater than one year.
The median age of patients who received FERRIPROX was 19 years (range 1, 77 years); 50.2% female; 71.2% White, 17.8% Asian, 9.2% Unknown, 1.2% Multi-racial and 0.6% Black.
The most serious adverse reaction reported in clinical trials with FERRIPROX was agranulocytosis [see Warnings and Precautions (5.1 ) ] .
The most common adverse reactions (≥6%) reported during clinical trials were nausea, vomiting, abdominal pain, arthralgia, alanine aminotransferase increased and neutropenia.
The table below lists the adverse drug reactions that occurred in at least 1% of patients treated with FERRIPROX in clinical trials in patients with thalassemia syndromes.
| Body System | (N=642) |
| Adverse Reaction | % Patients |
| BLOOD AND LYMPHATIC SYSTEM DISORDERS | |
| Neutropenia • | 7 |
| Agranulocytosis † | 1 |
| GASTROINTESTINAL DISORDERS | |
| Nausea | 13 |
| Abdominal pain/discomfort | 10 |
| Vomiting | 10 |
| Diarrhea | 3 |
| Dyspepsia | 2 |
| INVESTIGATIONS | |
| Alanine aminotransferase increased | 7 |
| Weight increased | 2 |
| Aspartate aminotransferase increased | 1 |
| METABOLISM AND NUTRITION DISORDERS | |
| Increased appetite | 4 |
| Decreased appetite | 1 |
| MUSCULOSKELETAL AND CONNECTIVE TISSUE DISORDERS | |
| Arthralgia | 10 |
| Back pain | 2 |
| Pain in extremity | 2 |
| Arthropathy | 1 |
| NERVOUS SYSTEM DISORDERS | |
| Headache | 2 |
| • Neutropenia includes events of severe neutropenia (ANC ≥0.2 x 10 9 /L and <0.5 x 10 9 /L). †Agranulocytosis (ANC< 0.2 x 10 9 /L) | |
Gastrointestinal symptoms such as nausea, vomiting, and abdominal pain were the most frequent adverse reactions reported by patients participating in clinical trials and led to the discontinuation of FERRIPROX therapy in 1.6% of patients.
Chromaturia (reddish/brown discoloration of the urine) is a result of the excretion of iron in the urine.
Sickle Cell Disease or Other Anemias
The safety of FERRIPROX compared to deferoxamine was evaluated in LA38-0411 [see Clinical Studies (14.2 )] . Patients received FERRIPROX Tablets or FERRIPROX Oral Solution orally three times a day (total daily dose 75-99 mg/kg/day) n=152) or the control arm, deferoxamine, 20-40 mg/kg/day (children) or 40-50 mg/kg/day (adults), by subcutaneous infusion for 5 – 7 days per week, n=76. Among 152 patients receiving FERRIPROX, 120 (78.9%) were exposed for 6 months or longer and 17 (11.2%) were exposed for greater than one year.
The median age of patients who received FERRIPROX was 15 years (range 3, 59 years); 54.6% male; 78.9% White, 15.1% Black and 5.9% Multi-racial.
The most common adverse reactions (≥6%) reported during clinical trials in patients with SCD or other anemias were pyrexia, abdominal pain, bone pain, headache, vomiting, pain in extremity, sickle cell anemia with crisis, back pain, alanine aminotransferase (ALT) increased, aspartate aminotransferase (AST) increased, arthralgia, oropharyngeal pain, nasopharyngitis, neutrophil count decreased, cough and nausea.
The table below lists the adverse reactions (irrespective of a causal assessment; adverse events) of interest that occurred in patients treated with FERRIPROX in clinical trials in subjects with sickle cell disease or other anemias.
| Body System Adverse Reaction | FERRIPROX (N=152) % Patients | DEFEROXAMINE (N=76) % Patients |
| BLOOD AND LYMPHATIC SYSTEM DISORDERS | ||
| Sickle cell anemia with crisis | 17 | 13 |
| GASTROINTESTINAL DISORDERS | ||
| Abdominal pain• | 26 | 13 |
| Vomiting | 19 | 11 |
| Nausea | 7 | 9 |
| Diarrhea | 5 | 8 |
| GENERAL DISORDERS AND ADMINISTRATION SITE CONDITIONS | ||
| Pyrexia | 28 | 33 |
| Pain | 5 | 4 |
| INFECTIONS AND INFESTATIONS | ||
| Nasopharyngitis | 9 | 12 |
| Upper respiratory tract infection | 5 | 3 |
| INVESTIGATIONS | ||
| Alanine aminotransferase increased | 12 | 0 |
| Aspartate aminotransferase increased | 11 | 0 |
| Neutrophil count decreased | 8 | 4 |
| MUSCULOSKELETAL AND CONNECTIVE TISSUE DISORDERS | ||
| Bone pain | 25 | 34 |
| Pain in extremity | 18 | 15 |
| Back pain | 13 | 18 |
| Arthralgia | 10 | 8 |
| NERVOUS SYSTEM DISORDERS | ||
| Headache | 20 | 13 |
| RESPIRATORY, THORACIC AND MEDIASTINAL DISORDERS | ||
| Oropharyngeal pain | 10 | 15 |
| Cough | 8 | 15 |
•Grouped term
Clinically relevant adverse reactions in <5% of patients include neutropenia and agranulocytosis.
Pediatric Patients
FERRIPROX has been studied in 86 pediatric patients with sickle cell disease or other anemias. Pediatric patients (<17 years) had an increase in the following adverse reactions as compared to adults: abdominal pain, neutrophil count decreased, bone pain and oropharyngeal pain.
6.2 Postmarketing Experience
The following additional adverse reactions have been reported in patients receiving FERRIPROX. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or to establish a causal relationship to drug exposure.
Blood and lymphatic system disorders: thrombocytosis, pancytopenia.
Cardiac disorders: atrial fibrillation, cardiac failure.
Congenital, familial and genetic disorders: hypospadias.
Eye disorders: diplopia, papilledema, retinal toxicity.
Gastrointestinal disorders: enterocolitis, rectal hemorrhage, gastric ulcer, pancreatitis, parotid gland enlargement.
General disorders and administration site conditions: chills, edema peripheral, multi-organ failure.
Hepatobiliary disorders: jaundice, hepatomegaly.
Immune system disorders: anaphylactic shock, hypersensitivity.
Infections and infestations: cryptococcal cutaneous infection, enteroviral encephalitis, pharyngitis, pneumonia, sepsis, furuncle, infectious hepatitis, rash pustular, subcutaneous abscess.
Investigations: blood bilirubin increased, blood creatinine phosphokinase increased.
Metabolism and nutrition disorders: metabolic acidosis, dehydration.
Musculoskeletal and connective tissue disorders: myositis, chondropathy, trismus.
Nervous system disorders: cerebellar syndrome, cerebral hemorrhage, convulsion, gait disturbance, intracranial pressure increased, psychomotor skills impaired, pyramidal tract syndrome, somnolence.
Psychiatric disorders: bruxism, depression, obsessive-compulsive disorder.
Renal disorders: glycosuria, hemoglobinuria.
Respiratory, thoracic and mediastinal disorders: acute respiratory distress syndrome, epistaxis, hemoptysis, pulmonary embolism.
Skin, subcutaneous tissue disorders: hyperhidrosis, periorbital edema, photosensitivity reaction, pruritis, urticaria, rash, Henoch-Schönlein purpura.
Vascular disorders: hypotension, hypertension.
7 DRUG INTERACTIONS
7.1 Drugs A ssociated with N eutropenia or A granulocytosis
Avoid co-administration of FERRIPROX with other drugs known to be associated with neutropenia or agranulocytosis. If co-administration is unavoidable, closely monitor the absolute neutrophil count [ see Warnings and Precautions (5.1 ) ] .
7.2 Effect of Other Drugs on FERRIPROX
UDP-Glucuronosyltransferases (UGT)
Avoid use of UGT1A6 inhibitors (e.g., diclofenac, probenecid, or silymarin (milk thistle)) with FERRIPROX [ see Dosage and Administration (2.2 ) , Adverse Reactions (6.1 ), Clinical Pharmacology (12.3 ) ] .
Polyvalent Cations
Deferiprone has the potential to bind polyvalent cations (e.g., iron, aluminum, and zinc); allow at least a 4-hour interval between FERRIPROX and other medications (e.g., antacids), or supplements containing these polyvalent cations [see Dosage and Administration (2.2 ) ] .
11 DESCRIPTION
FERRIPROX Tablets (deferiprone) contain 1,000 mg deferiprone (3-hydroxy-1,2-dimethylpyridin-4-one), a synthetic, orally active, iron-chelating agent. The molecular formula for deferiprone is C 7 H 9 NO 2 and its molecular weight is 139.15 g/mol. Deferiprone has the following structural formula:
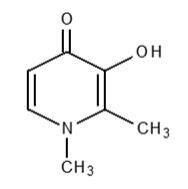
Deferiprone is a white to pinkish-white powder. It is sparingly soluble in deionized water (14.3 mg/mL) and has a melting point range of 272 °C - 278 °C.
FERRIPROX Tablets ( twice a day) , 1,000 mg
White to off-white, capsule-shaped tablets, and imprinted with “FPX” score “DR” on one side and “APO” score “1000” on the other. The tablets can be broken in half along the score line. Each tablet contains 1,000 mg deferiprone and the following inactive ingredients: Tablet core - hypromellose acetate succinate, magnesium oxide, colloidal silicon dioxide and magnesium stearate; Coating - triethyl citrate, talc, titanium dioxide, and methacrylic acid and ethyl acrylate copolymer.
FERRIPROX T ablets (three times a day) , 1,000 mg
White to off-white, capsule-shaped tablets, and imprinted with “APO” score “1000” on one side and plain on the other. The tablets can be broken in half along the score line. Each tablet contains 1,000 mg deferiprone and the following inactive ingredients: Tablet core - methylcellulose, crospovidone, and magnesium stearate; Coating - hypromellose, hydroxypropyl cellulose, macrogol, and titanium dioxide.
12 CLINICAL PHARMACOLOGY
12.1 Mechanism of Action
Deferiprone is a chelating agent with an affinity for ferric ions (iron III). Deferiprone binds with ferric ions to form neutral 3:1 (deferiprone:iron) complexes that are stable at physiological pH.
12.2 Pharmacodynamics
No clinical studies were performed to assess the relationship between the dose of deferiprone and the amount of iron eliminated from the body.
Cardiac Electrophysiology
At the maximum approved recommended dose, deferiprone does not prolong the QT interval to any clinically relevant extent.
12.3 Pharmacokinetics
FERRIPROX Tablets (twice a day), 1,000 mg
In healthy subjects, the mean ± SD C max of deferiprone in serum was 6 ± 2 mcg/mL, and the mean ± SD AUC was 28 ± 7 mcg∙h/mL following oral administration of a 1,000 mg dose of FERRIPROX Tablets (twice a day) with food.
Absorption
Peak serum concentrations of deferiprone occur approximately 2 hours after a single dose of FERRIPROX Tablets (twice a day) in fasted healthy subjects.
Effect of Food
Following the administration of FERRIPROX Tablets (twice a day) to healthy volunteers, the C max and the AUC of deferiprone remain unchanged after a high-fat meal (approximately 1,000 calories, 53% fat, 33% carbohydrates, and 14% protein) compared to fasted conditions.
Effect of Alcohol
At 40% (v/v) alcohol concentration in vitro dissolution studies, there was 88% release of deferiprone from a 1,000 mg FERRIPROX tablet (twice a day) within two hours compared to 4% release of deferiprone within 2 hours in the absence of alcohol.
Distribution
The apparent mean ± SD volume of distribution (V/F) of deferiprone was 97 ± 28 L following oral administration of a 1,000 mg dose of FERRIPROX Tablets (twice a day) with food.
Elimination
The mean ± SD elimination half-life of deferiprone is 1.8 ± 0.3 hours following the administration of FERRIPROX Tablets (twice a day).
Metabolism
Deferiprone is metabolized primarily by UGT1A6. The major metabolite of deferiprone is the 3- O -glucuronide, which lacks iron- binding capability.
Excretion
Following oral administration, 75% to 90% of the administered dose was recovered in urine (primarily as metabolite) in the first 24 hours.
FERRIPROX Tablets (three times a day) , 1,000 mg
The mean C max and AUC of deferiprone was 20 mcg/mL and 50 mcg∙h/mL, respectively, in healthy subjects. The dose proportionality of deferiprone over the approved recommended dosage range is unknown.
Absorption
Deferiprone appeared in the blood within 5 to 10 minutes after oral administration. Peak serum concentration of deferiprone was reached approximately 1 to 2 hours after a single dose.
Effect of Food
No clinically significant differences in the pharmacokinetics of deferiprone were observed following administration with food.
Elimination
The elimination half-life of deferiprone is approximately 2 hours.
Metabolism
Deferiprone is metabolized primarily by UGT1A6. The major metabolite of deferiprone is the 3- O -glucuronide, which lacks iron binding capability.
Excretion
Following oral administration, 75% to 90% of the administered dose was recovered in urine (primarily as metabolite) in the first 24 hours.
Specific P opulations
No clinically significant differences in the pharmacokinetics of deferiprone were observed based on sex, race/ethnicity, body weight, mild to severe (eGFR 15 to 89 mL/min/1.73 m 2 ) renal impairment, or mild (Child Pugh Class A) to moderate (Child Pugh Class B) hepatic impairment. The effect of age, including geriatric or pediatric populations, end stage renal disease or severe (Child Pugh Class C) hepatic impairment on the pharmacokinetics of deferiprone is unknown.
Drug Interaction Studie s
In Vitro Studies
UGTIA6 Inhibitors : Phenylbutazone (UGT1A6 inhibitor) decreased glucuronidation of deferiprone by up to 78%.
Polyvalent Cations: Deferiprone has the potential to bind polyvalent cations (e.g., iron, aluminum, and zinc).
13 NONCLINICAL TOXICOLOGY
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenicity studies have not been conducted with deferiprone. However, in view of the genotoxicity results, and the findings of mammary gland hyperplasia and mammary gland tumors in rats treated with deferiprone in the 52-week toxicology study, tumor formation in carcinogenicity studies must be regarded as likely.
Deferiprone was positive in a mouse lymphoma cell assay in vitro . Deferiprone was clastogenic in an in vitro chromosomal aberration test in mice and in a chromosomal aberration test in Chinese Hamster Ovary cells. Deferiprone given orally or intraperitoneally was clastogenic in a bone marrow micronucleus assay in non-iron-loaded mice. A micronucleus test was also positive when mice predosed with iron dextran were treated with deferiprone. Deferiprone was not mutagenic in the Ames bacterial reverse mutation test.
A fertility and early embryonic development study of deferiprone was conducted in rats. Sperm counts, motility and morphology were unaffected by treatment with deferiprone. There were no effects observed on male or female fertility or reproductive function at the highest dose which was 25% of the MRHD.
14 CLINICAL STUDIES
FERRIPROX Tablets (twice a day) were evaluated in trials in healthy subjects. FERRIPROX Tablets (twice a day) contain deferiprone, the same active ingredient as FERRIPROX Tablets and FERRIPROX Oral Solution. The following information is based on studies with FERRIPROX Tablets (deferiprone) (three times a day) and FERRIPROX Oral Solution (deferiprone).
14.1 Transfusional Iron Overload in Patients with Thalassemia Syndromes
In a prospective, planned, pooled analysis of patients with thalassemia syndromes from several studies, the efficacy of deferiprone was assessed in transfusion-dependent iron overload patients in whom previous iron chelation therapy had failed or was considered inadequate due to poor tolerance. The main criterion for chelation failure was serum ferritin > 2,500 mcg/L before treatment with deferiprone. Deferiprone therapy (35-99 mg/kg/day) was considered successful in individual patients who experienced a ≥ 20% decline in serum ferritin within one year of starting therapy.
Data from a total of 236 patients were analyzed. Of the 224 patients with thalassemia who received deferiprone monotherapy and were eligible for serum ferritin analysis, 105 (47%) were male and 119 (53%) were female. The mean age of these patients was 18.2 years (range 2 to 62; 91 patients were <17).
For the patients in the analysis, the endpoint of at least a 20% reduction in serum ferritin was met in 50% (of 236 subjects), with a 95% confidence interval of 43% to 57%.
A small number of patients with thalassemia and iron overload were assessed by measuring the change in the number of milliseconds (ms) in the cardiac MRI T2• value before and after treatment with deferiprone for one year. There was an increase in cardiac MRI T2• from a mean at baseline of 11.8 ± 4.9 ms to a mean of 15.1 ± 7.0 ms after approximately one year of treatment. The clinical significance of this observation is not known.
14.2 Transfusional Iron Overload in Patients with Sickle Cell Disease and other A nemias
Study LA38-0411, an actively-controlled non-inferiority study compared the efficacy of FERRIPROX to that of deferoxamine in patients with sickle cell disease and other transfusion-dependent anemias by evaluating liver iron concentration (LIC). The efficacy of FERRIPROX was established based upon the change in LIC from baseline after 12 months of FERRIPROX (75 or 99 mg/kg/day) compared to deferoxamine (20 or 40 mg/kg (pediatric patients); 40 or 50 mg/kg (adult patients)). Patient enrollment was stopped following an interim analysis. After adjusting for the type I (alpha) error, the non-inferiority criterion was established as the upper limit of the 96.01% confidence interval for the difference between treatments being ≤2 mg/g dry weight (dw).
Data from 185 patients (122 on FERRIPROX and 63 on deferoxamine) were available. Among the 122 FERRIPROX treated patients, the mean age was 15.9 years (range 3-46); 57.4% were male; 75.4% were White, 17.2% were Black and 7.4% were Multi-racial; 85% were diagnosed with Sickle Cell Disease and 15% with other anemias. Over 12 months, the Least Squares estimate of mean decrease from baseline in LIC was 4.13 ± 0.50 mg/g dw for FERRIPROX and 4.38 ± 0.59 mg/g dw for deferoxamine, and the non-inferiority criterion was met.
Upon completion of the first year of therapy in the non inferiority study, 89 patients from the FERRIPROX group opted to continue with treatment and 45 from the deferoxamine group opted to switch to ferriprox treatment. This group continued for up to an additional 2 years. LIC continued to decrease over time, with the mean value dropping from 14.93 mg/g dw at baseline to 12.30 mg/g dw after one year of treatment, to 11.19 mg/g dw after two years of treatment, and to 10.45 mg/g dw after three years of treatment.
16 HOW SUPPLIED/STORAGE AND HANDLING
FERRIPROX Tablets ( twice a day) , 1,000 mg
FERRIPROX ® Tablets (deferiprone) (twice a day) are white to off-white capsule-shaped, beveled edge, biconvex coated tablets, and have a functional score engraved “FPX” bisect “DR” on one side, “APO” bisect “1000” on the other. They are supplied in child-resistant blister packs or HDPE bottles.
1,000 mg tablets, carton of 5 x 10-count blister packs NDC 10122-104-01
1,000 mg tablets, bottle of 50 tablets NDC 10122-104-05
1,000 mg tablets, bottle of 500 tablets NDC 10122-104-50
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
F ERRIPROX T ablets (three times a day) , 1,000 mg
FERRIPROX ® Tablets (deferiprone) (three times a day) are white to off-white capsule-shaped tablets, film-coated, and have a functional score imprinted with “APO” score “1000” on one side and are plain on the other. They are provided in HDPE bottles.
1,000 mg film-coated tablets, 50 tablets NDC 10122-103-05
Store at 20°C to 25°C (68°F to 77°F); excursions permitted to 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature]. Keep the bottle tightly closed to protect from moisture.
12.1 Mechanism of Action
Deferiprone is a chelating agent with an affinity for ferric ions (iron III). Deferiprone binds with ferric ions to form neutral 3:1 (deferiprone:iron) complexes that are stable at physiological pH.
Ferriprox - Deferiprone tablet PubMed™ news
- Journal Article • 2026 MayApparent plateaus during iron chelation in transfusion-dependent β-thalassemia: interpretation and clinical implications.
- Journal Article • 2026 MayEffects of Sex and Fed State Differences on the Pharmacokinetics of Drugs in Humans.
- Journal Article • 2026 AprLinking Iron Metabolism, Ferroptosis, and Cancer: New Targets and Prospects for Effective Anticancer Therapeutic Interventions.
- Journal Article • 2026 AprPoly-GR promotes ferroptosis-associated vulnerability in C9orf72-ALS.
- Journal Article • 2026 AprBlue LED light induces dry eye disease via NCOA4-mediated ferritinophagy and iron-overload.