Estradiol - Estradiol Gel 0.1% gel prescribing information
WARNING: ENDOMETRIAL CANCER WITH UNOPPOSED ESTROGEN IN WOMEN WITH A UTERUS
There is an increased risk of endometrial cancer in a woman with a uterus who uses unopposed estrogens. Adding a progestogen to estrogen-only therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer.
Perform adequate diagnostic measures, including directed or random endometrial sampling when indicated, to rule out malignancy in menopausal women abnormal genital bleeding of unknown etiology [see Warnings and Precautions (5.2 )].
RECENT MAJOR CHANGES SECTION
Boxed Warning, Cardiovascular Disorders, Breast Cancer, Probable Dementia removed 2/2026
Dosage and Administration, Important Use Information (2.1 ) 2/2026
Contraindications (4 ) 2/2026
Warnings and Precautions, Cardiovascular Disorders (5.1 ) 2/2026
Warnings and Precautions, Malignant Neoplasms (5.2 ) 2/2026
Warnings and Precautions, Risks Associated with Co-administration of Estrogen Plus Progestogen (5.3 ) 2/2026
Warnings and Precautions, Probable Dementia removed 2/2026
Warnings and Precautions, Addition of a Progestogen When a Woman Has Not Had a Hysterectomy removed 2/2026
INDICATIONS AND USAGE
Treatment of Moderate to Severe Vasomotor Symptoms due to Menopause
DOSAGE AND ADMINISTRATION
Important Use Information
The timing of estradiol gel 0.1% initiation can affect the overall benefit-risk profile. Consider initiating estradiol gel 0.1% in women <60 years old or <10 years since menopause onset [see Warnings and Precautions (5 ), Use in Specific Populations (8.5 ) and Clinical Studies (14 )].
When estrogen is prescribed for a menopausal woman with a uterus, the addition of a progestogen has been shown to reduce the risk of endometrial cancer. There are possible risks associated with the use of progestogens plus estrogens that differ from those of estrogen-alone regimens. See prescribing information for progestogens indicated for the prevention of endometrial hyperplasia in non-hysterectomized menopausal women receiving estrogens [see Warnings and Precautions (5.2 , 5.3 )] .
Generally, a woman without a uterus, does not need to use a progestogen with estrogen therapy. In some cases, however, hysterectomized women with a history of endometriosis may benefit from the addition of a progestogen [see Warnings and Precautions (5.13 )].
Treatment of Moderate to Severe Vasomotor Symptoms due to Menopause
Start therapy with the 0.25 grams applied once daily on the skin of either the right or left upper thigh. Adjust the dose up to a maximum of 1.25 grams, as needed.
The application surface area should be about 5 by 7 inches (approximately the size of two palm prints). The entire contents of a unit dose packet should be applied each day. To avoid potential skin irritation, apply estradiol gel 0.1% to the right or left upper thigh on alternating days. Do not apply Estradiol gel 0.1% on the face, breasts, or irritated skin or in or around the vagina. Allow gel to dry after application before dressing. Do not wash the application site within 1 hour after applying estradiol gel 0.1%. Avoid contact of the gel with eyes. Wash hands after application.
DOSAGE FORMS AND STRENGTHS
Estradiol gel 0.1% is available in five doses of 0.25, 0.5, 0.75, 1.0, and 1.25 grams for transdermal application (corresponding to 0.25, 0.5, 0.75, 1.0, and 1.25 mg estradiol, respectively). Estradiol gel 0.1% is a clear, colorless gel, which is odorless when dry.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary Estradiol gel 0.1% is not indicated for use in pregnant women. There are no data with the use of estradiol gel 0.1% in pregnant women; however, epidemiologic studies and meta-analyses have not found an increased risk of genital or nongenital birth defects (including cardiac anomalies and limb-reduction defects) following exposure to combined hormonal contraceptives (estrogen and progestins) before conception or during early pregnancy.
In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively.
Lactation
Risk Summary Estrogens are present in human milk and can reduce milk production in breast-feeding women. This reduction can occur at any time but is less likely to occur once breast-feeding is well established.
The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for estradiol gel 0.1% and any potential adverse effects on the breastfed child from estradiol gel 0.1% or from the underlying maternal condition.
Pediatric Use
Estradiol gel 0.1% is not indicated for use in pediatric patients. Clinical studies have not been conducted in the pediatric population.
Geriatric Use
There have not been sufficient numbers of geriatric women involved in clinical studies utilizing estradiol gel 0.1% to determine whether those over 65 years of age differ from younger subjects in their response to estradiol gel 0.1%.
The Women's Health Initiative Studies
In the WHI estrogen-alone trial (daily CE [0.625 mg]-alone versus placebo), there was a higher relative risk of stroke in women greater than 65 years of age [see Clinical Studies (14.2 )].
The Women's Health Initiative Memory Study
In the WHIMS ancillary studies of postmenopausal women 65 to 79 years of age, there was an increased risk of probable dementia in women receiving estrogen-alone [see Clinical Studies (14.3 )].
Since the trial was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women [see Clinical Studies (14.3 )] . The safety and efficacy of estradiol gel 0.1% for the prevention of dementia has not been established.
CONTRAINDICATIONS
Estradiol gel 0.1% is contraindicated in women with any of the following conditions:
Abnormal genital bleeding of unknown etiology [see Warning and Precautions (5.2 )]
Current or history of breast cancer [see Warning and Precautions (5.2 )]
Estrogen-dependent neoplasia [see Warning and Precautions (5.2 )]
Active DVT, PE, or history of these conditions [see Warning and Precautions (5.1 )]
Active arterial thromboembolic disease (for example, stroke or MI), or a history of these conditions [see Warning and Precautions (5.1 )]
Known anaphylactic reaction, angioedema, or hypersensitivity to estradiol gel 0.1%
Hepatic impairment or disease [see Warnings and Precautions (5.9 )]
Protein C, protein S, or antithrombin deficiency, or other known thrombophilic disorders
WARNINGS AND PRECAUTIONS
Cardiovascular Disorders: Increased risk of PE, DVT, and stroke with estrogen-alone therapy. Discontinue if an arterial or venous thrombotic or thromboembolic event occurs. (5.1 )
Estrogens increase the risk of gallbladder disease (5.4 )
Discontinue estrogen if severe hypercalcemia, loss of vision, severe hypertriglyceridemia or cholestatic jaundice occurs (5.5 , 5.6 , 5.8 , 5.9 )
Monitor thyroid function in women on thyroid replacement therapy (5.10 , 5.21 )
Cardiovascular Disorders
Estradiol gel 0.1%is contraindicated in women with active DVT, PE, stroke, or a history of these conditions [see Contraindications (4 )]. Immediately discontinue estradiol gel 0.1% if a PE, DVT, or stroke, occurs or is suspected. If feasible, discontinue estradiol gel 0.1% at least 4 to 6 weeks before surgery of the type associated with an increased risk of thromboembolism, or during periods of prolonged immobilization.
The safety and efficacy of estradiol gel 0.1% for the prevention of cardiovascular disorders has not been established.
The Women’s Health Initiate (WHI) estrogen-alone trial reported increased risks of pulmonary embolism (PE), deep vein thrombosis (DVT), and stroke, in postmenopausal women (50 to 79 years of age, average age 63.4 years) during 7.2 years of treatment with daily oral conjugated estrogen (CE) [0.625 mg] relative to placebo. Analyses were also conducted in women aged 50-59 years, a group of women more likely to present with onset of moderate to severe VMS compared to women of other age groups in the trial.
Only daily oral 0.625 mg CE was studied in the WHI estrogen-alone trial. Therefore, the relevance of the WHI findings regarding adverse cardiovascular events to lower CE doses, other routes of administration, or other estrogen products is not known. Without such data, it is not possible to definitively exclude these risks or determine the extent of these risks for other products [see Clinical Studies (14.2 )].
Venous Thromboembolism
In women aged 50-59 years, the WHI estrogen-alone trial reported a relative risk for PE of 1.53 (95% confidence interval [CI], 0.63, 3.75) for CE compared to placebo, with an absolute risk difference of 4 per 10,000 women-years (WYs; 10 versus 6). The relative risk for DVT was 1.66 (95% CI 0.75, 3.67) for CE compared to placebo, with a risk difference of 5 per 10,000 WYs (13 versus 8).
In the overall study population of women aged 50-79 years, the WHI estrogen-alone trial reported a relative risk of PE of 1.35 (95% CI 0.89, 2.05) for CE compared to placebo, with a risk difference of 4 per 10,000 WYs (14 versus 10). The relative risk for DVT was 1.48 (95% 1.06, 2.07) for CE compared to placebo, with a risk difference of 7 per 10,000 WYs (23 versus 15) [see Clinical Studies (14.2 )].
Stroke
In women aged 50-59 years, the WHI estrogen-alone trial reported a relative risk for stroke of 0.99 (95% 0.53, 1.85) for CE compared to placebo, with a risk difference of -1 per 10,000 WYs (16 versus 17).
In the overall study population of women aged 50-79 years, the WHI estrogen-alone trial reported a relative risk for stroke of 1.35 (95%, 1.07, 1.70) for CE compared to placebo, with a risk difference of 11 per 10,000 WYs (45 versus 34) [see Clinical Studies (14.2 )].
Malignant Neoplasms
Endometrial Cancer
In estradiol gel 0.1%-treated menopausal women with a uterus with persistent or recurring abnormal genital bleeding of unknown etiology, perform adequate diagnostic measures, including directed or random endometrial sampling when indicated, to assess for endometrial cancer.
An increased risk of endometrial cancer has been reported with the use of unopposed estrogen therapy in a woman with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2 to 12 times greater than in non-users and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with use of estrogens for less than 1 year. The greatest risk appears to be associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more. This risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose.
Adding a progestogen to estrogen-alone therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer. There are, however, possible risks associated with the use of progestogens plus estrogens that differ from those of estrogen-alone regimens [see Warnings and Precautions (5.3 )].
Breast Cancer
Surveillance measures for breast cancer, such as breast examinations and mammography, are recommended. The use of estrogen-alone therapy has been reported to result in an increase in abnormal mammograms requiring further evaluation.
In the WHI estrogen-alone trial, after an average follow-up of 7.1 years, daily CE-alone was not associated with an increased risk of invasive breast cancer. Among women 50-59 years old, the relative risk was 0.82 (95% CI, 0.50, 1.34) for CE compared to placebo, with a risk difference of -5 per 10,000 WYs (24 versus 29). In the overall study population of women aged 50-79 years (average age 63.4 years), the relative risk was 0.79 (95% CI, 0.61, 1.02), with a risk difference of -7 per 10,000 WYs (28 versus 35). [see Clinical Studies (14.2 )] .
However, a large meta-analysis including 24 prospective studies of postmenopausal women comparing current use of estrogen-only products with use duration of 5 to 14 years (average of 9 years) versus never use reported a relative risk for breast cancer of 1.33 (95% CI, 1.28 to 1.38). 1
Ovarian Cancer
A large meta-analysis including 17 prospective studies of postmenopausal women compared current use of estrogen-only products versus never use and reported a relative risk for ovarian cancer of 1.37 (95% CI, 1.26 to 1.50). The duration of hormone therapy use that was associated with an increased risk of ovarian cancer is unknown. 2
Risks Associated with Co-administration of Estrogen Plus Progestogen
Studies of the addition of a progestogen for 10 or more days of a cycle of estrogen administration, or daily with estrogen in a continuous regimen, have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer.
If estradiol gel 0.1% is administered with a progestogen, there are possible risks associated with the use of progestogens plus estrogens that differ from those of estrogen-alone regimens. Refer to prescribing information for progestogens indicated for the prevention of endometrial hyperplasia in non-hysterectomized women receiving estrogens.
Gallbladder Disease
A 2- to 4-fold increase in the risk of gallbladder disease requiring surgery in postmenopausal women receiving estrogens has been reported.
Hypercalcemia
Estrogen administration may lead to severe hypercalcemia in women with breast cancer and bone metastases. Discontinue estrogens, including estradiol gel 0.1%, if hypercalcemia occurs, and take appropriate measures to reduce the serum calcium level.
Visual Abnormalities
Retinal vascular thrombosis has been reported in patients receiving estrogens. Discontinue estradiol gel 0.1% pending examination if there is sudden partial or complete loss of vision, or a sudden onset of proptosis, diplopia, or migraine. Permanently discontinue estrogens, including estradiol gel 0.1%, if examination reveals papilledema or retinal vascular lesions.
Elevated Blood Pressure
In a small number of case reports, substantial increases in blood pressure have been attributed to idiosyncratic reactions to estrogens. In a large, randomized, placebo-controlled clinical trial, a generalized effect of estrogens on blood pressure was not seen.
Exacerbation of Hypertriglyceridemia
In women with pre-existing hypertriglyceridemia, estrogen therapy may be associated with elevations of plasma triglycerides leading to pancreatitis. Discontinue estradiol gel 0.1% if pancreatitis occurs.
Hepatic Impairment and/or Past History of Cholestatic Jaundice
Estrogens may be poorly metabolized in women with hepatic impairment. Exercise caution in any woman with a history of cholestatic jaundice associated with past estrogen use or with pregnancy. In the case of recurrence of cholestatic jaundice, discontinue estradiol gel 0.1%.
Exacerbation of Hypothyroidism
Estrogen administration leads to increased thyroid-binding globulin (TBG) levels. Women with normal thyroid function can compensate for the increased TBG by making more thyroid hormone, thus maintaining free T 4 and T 3 serum concentrations in the normal range. Women dependent on thyroid hormone replacement therapy who are also receiving estrogens may require increased doses of their thyroid replacement therapy. Monitor thyroid function in these women during treatment with estradiol gel 0.1% to maintain their free thyroid hormone levels in an acceptable range.
Fluid Retention
Estrogens may cause some degree of fluid retention. Monitor any woman with a condition(s) that might predispose her to fluid retention, such as a cardiac or renal impairment. Discontinue estrogen-alone therapy, including estradiol gel 0.1%, with evidence of medically concerning fluid retention.
Hypocalcemia
Estrogen-induced hypocalcemia may occur in women with hypoparathyroidism. Consider whether the benefits of estrogen therapy outweigh the risks in such women.
Exacerbation of Endometriosis
A few cases of malignant transformation of residual endometrial implants have been reported in women treated post-hysterectomy with estrogen-alone therapy. Consider the addition of a progestogen therapy for a woman known to have residual endometriosis post-hysterectomy.
Hereditary Angioedema
Exogenous estrogens may exacerbate symptoms of angioedema in women with hereditary angioedema. Consider whether the benefits of estrogen therapy, including estradiol gel 0.1%, outweigh the risks in such women.
Exacerbation of Other Conditions
Estrogen therapy, including estradiol gel 0.1%, may cause an exacerbation of asthma, diabetes mellitus, epilepsy, migraine, porphyria, systemic lupus erythematosus, and hepatic hemangiomas. Consider whether the benefits of estrogen therapy outweigh the risks in women with such conditions.
Photosensitivity
The effects of direct sun exposure to estradiol gel 0.1% application sites have not been evaluated in clinical trials.
Application of Sunscreen and Topical Solutions
Studies conducted using other approved topical estrogen gel products have shown that sunscreens have the potential for changing the systemic exposure of topically applied estrogen gels.
The effect of sunscreens and other topical lotions on the systemic exposure of estradiol gel 0.1% has not been evaluated in clinical trials.
Flammability of Alcohol-Based Gels
Alcohol based gels are flammable. Avoid fire, flame, or smoking until estradiol gel 0.1% has dried.
Occlusion of the area where the topical drug product is applied with clothing or other barriers is not recommended until estradiol gel 0.1% has completely dried.
Potential for Estradiol Transfer and Effects of Washing
There is a potential for drug transfer from one individual to the other following physical contact of estradiol gel 0.1% application sites. In a study to evaluate transferability to males from their female contacts, there was some elevation of estradiol levels over baseline in the male subjects; however, the degree of transferability in this study was inconclusive. Women are advised to avoid skin contact with other persons until the gel is completely dried. The site of application should be covered (clothed) after drying.
Washing the application site with soap and water 1 hour after application resulted in a 30 to 38 percent decrease in the mean total 24-hour exposure to estradiol. Therefore, women should refrain from washing the application site for at least one hour after application.
Laboratory Tests
Serum follicle stimulating hormone (FSH) and estradiol levels are not useful in the management of moderate to severe vasomotor symptoms.
Drug-Laboratory Test Interactions
- Accelerated prothrombin time, partial thromboplastin time, and platelet aggregation time; increased platelet count; increased factors II, VII antigen, VIII antigen, VIII coagulant activity, IX, X, XII, VII-X complex, II-VII-X complex, and beta-thromboglobulin; decreased levels of anti-factor Xa and antithrombin III, decreased antithrombin III activity; increased levels of fibrinogen and fibrinogen activity; increased plasminogen antigen and activity.
- Increased thyroid binding globulin (TBG) levels leading to increased circulating total thyroid hormone levels, as measured by protein-bound iodine (PBI), T 4 levels (by column or by radioimmunoassay) or T 3 levels by radioimmunoassay. T 3 resin uptake is decreased, reflecting the elevated TBG. Free T 4 and free T 3 concentrations are unaltered. Women on thyroid replacement therapy may require higher doses of thyroid hormone.
- Other binding proteins may be elevated in serum, for example, corticosteroid binding globulin (CBG), sex hormone-binding globulin (SHBG), leading to increased total circulating corticosteroids and sex steroids, respectively. Free hormone concentrations, such as testosterone and estradiol, may be decreased. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-l-antitrypsin, ceruloplasmin).
- Increased plasma high-density lipoprotein (HDL) and HDL 2 cholesterol subfraction concentrations, reduced low-density lipoprotein (LDL) cholesterol concentration, increased triglyceride levels.
- Impaired glucose tolerance.
ADVERSE REACTIONS
The following serious adverse reactions are discussed elsewhere in the labeling:
Cardiovascular Disorders [see Boxed Warning , Warnings and Precautions (5.1) ].
Malignant Neoplasms [see Boxed Warning , Warnings and Precautions (5.2) ].
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Estradiol gel 0.1% was studied at doses of 0.25, 0.5 and 1.0 gram per day in a 12-week, double-blind, placebo-controlled study that included a total of 495 postmenopausal women (86.5 percent Caucasian). The adverse reactions that occurred at a rate greater than 5 percent and greater than placebo in any of the treatment groups are summarized in Table 1.
| Estradiol Gel 0.1% | Placebo | |||
|---|---|---|---|---|
| SYSTEM ORGAN CLASS Preferred Term | 0.25 grams/day N=122 n (%) | 0.5 grams/day N=123 n (%) | 1.0 gram/day N=125 n (%) | N=125 n (%) |
| •Adverse reactions reported by >5 percent of patients in any treatment group. | ||||
| INFECTIONS & INFESTATIONS | ||||
| Nasopharyngitis | 7 (5.7) | 5 (4.1) | 6 (4.8) | 5 (4.0) |
| Upper Respiratory Tract Infection | 7 (5.7) | 3 (2.4) | 2 (1.6) | 2 (1.6) |
| Vaginal mycosis | 1 (0.8) | 3 (2.4) | 8 (6.4) | 4 (3.2) |
| REPRODUCTIVE SYSTEM & BREAST DISORDERS | ||||
| Breast Tenderness | 3 (2.5) | 7 (5.7) | 11 (8.8) | 2 (1.6) |
| Metrorrhagia | 5 (4.1) | 7 (5.7) | 12 (9.6) | 2 (1.6) |
In a 12-week placebo-controlled study of estradiol gel 0.1%, application site reactions were seen in <1 percent of participating women.
Postmarketing Experience
The following adverse reactions have been identified during post-approval use of estradiol gel 0.1%. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Genitourinary System Amenorrhea, dysmenorrhea, ovarian cyst, vaginal discharge
Breasts Gynecomastia
Cardiovascular Palpitations, ventricular extrasystoles
Gastrointestinal Flatulence
Skin Rash pruritic, urticaria
Eyes Retinal vein occlusion
Central Nervous System Tremor
Miscellaneous Arthralgia, application site rash, asthenia, chest discomfort, fatigue, feeling abnormal, heart rate increased, insomnia, malaise, muscle spasms, pain in extremity, weight increased
DRUG INTERACTIONS
In vitro and in vivo studies have shown that estrogens are metabolized partially by cytochrome P450 3A4 (CYP3A4). Therefore, inducers or inhibitors of CYP3A4 may affect estrogen drug metabolism. Inducers of CYP3A4, such as St. John's wort ( Hypericum perforatum ) preparations, phenobarbital, carbamazepine, and rifampin, may reduce plasma concentrations of estrogens, possibly resulting in a decrease in therapeutic effects and/or changes in the uterine bleeding profile. Inhibitors of CYP3A4, such as erythromycin, clarithromycin, ketoconazole, itraconazole, ritonavir, and grapefruit juice, may increase plasma concentrations of estrogens and result in adverse reactions.
DESCRIPTION
Estradiol gel 0.1%, is a clear, colorless gel, which is odorless when dry. It is designed to deliver sustained circulating concentrations of estradiol when applied once daily to the skin. The gel is applied to a small area (200 cm 2 ) of the thigh in a thin layer. Estradiol gel 0.1% is available in five doses of 0.25, 0.5, 0.75, 1.0, and 1.25 grams for topical application (corresponding to 0.25, 0.5, 0.75, 1.0, and 1.25 mg estradiol, respectively).
The active component of the topical gel is estradiol, an estrogen.
Estradiol is a white crystalline powder, chemically described as estra-1,3,5(10)-triene-3,17ß-diol. It has an empirical formula of C 18 H 24 O 2 and molecular weight of 272.39. The structural formula is:
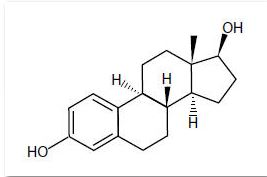
The remaining components of the gel (carbomer, ethanol, propylene glycol, purified water, and triethanolamine) are pharmacologically inactive.
Estradiol gel 0.1% contains: 58.6% alcohol.
CLINICAL PHARMACOLOGY
Mechanism of Action
Endogenous estrogens are largely responsible for the development and maintenance of the female reproductive system and secondary sexual characteristics. Although circulating estrogens exist in a dynamic equilibrium of metabolic interconversions, estradiol is the principal intracellular human estrogen and is substantially more potent than its metabolites, estrone and estriol, at the receptor level.
The primary source of estrogen in normally cycling adult women is the ovarian follicle, which secretes 70 to 500 mcg of estradiol daily, depending on the phase of the menstrual cycle. After menopause, most endogenous estrogen is produced by conversion of androstenedione, which is secreted by the adrenal cortex, to estrone in the peripheral tissues. Thus, estrone and the sulfate conjugated form, estrone sulfate, are the most abundant circulating estrogens in postmenopausal women.
Estrogens act through binding to nuclear receptors in estrogen-responsive tissues. To date, two estrogen receptors have been identified. These vary in proportion from tissue to tissue.
Circulating estrogens modulate the pituitary secretion of the gonadotropins, luteinizing hormone (LH) and FSH, through a negative feedback mechanism. Estrogens act to reduce the elevated levels of these hormones seen in postmenopausal women.
Pharmacodynamics
Generally, a serum estrogen concentration does not predict an individual woman’s therapeutic response to estradiol gel 0.1% nor her risk for adverse outcomes. Likewise, exposure comparisons across different estrogen products to infer efficacy or safety for the individual woman may not be valid.
Pharmacokinetics
Absorption
Estradiol diffuses across intact skin and into the systemic circulation by a passive absorption process, with diffusion across the stratum corneum being the rate-limiting factor.
In a 14-day, Phase 1, multiple-dose study, estradiol gel 0.1% demonstrated linear and approximately dose- proportional estradiol pharmacokinetics at steady state for both AUC 0-24 and C max following once daily dosing to the skin of either the right or left upper thigh (Table 2).
Table 2: Mean (%CV) Pharmacokinetic Parameters for Estradiol (uncorrected for baseline) on Day 14 Following Multiple Daily Doses of Estradiol Gel 0.1%
| Parameter (units) | Estradiol Gel 0.25 grams | Estradiol Gel 0.5 grams | Estradiol Gel 1.0 gram |
| AUC 0-24 (pg•h/mL) | 236 (94) | 504 (149) | 732 (81) |
| C max (pg/mL) | 14.7 (84) | 28.4 (139) | 51.5 (86) |
| C avg (pg/mL) | 9.8 (92) | 21 (148) | 30.5 (81) |
| t max • (h) | 16 (0,72) | 10 (0,72) | 8 (0,48) |
| E2:E1 ratio | 0.42 | 0.65 | 0.65 |
•Median (Min, Max).
Steady-state serum concentration of estradiol are achieved by day 12 following daily application of estradiol gel 0.1% to the skin of the upper thigh. The mean (SD) serum estradiol levels following once daily dosing at day 14 are shown in Figure 1.
Figure 1: Mean (SD) Serum Estradiol Concentrations (Values Uncorrected for Baseline) on Day 14 Following Multiple Daily Doses of Estradiol Gel 0.1%
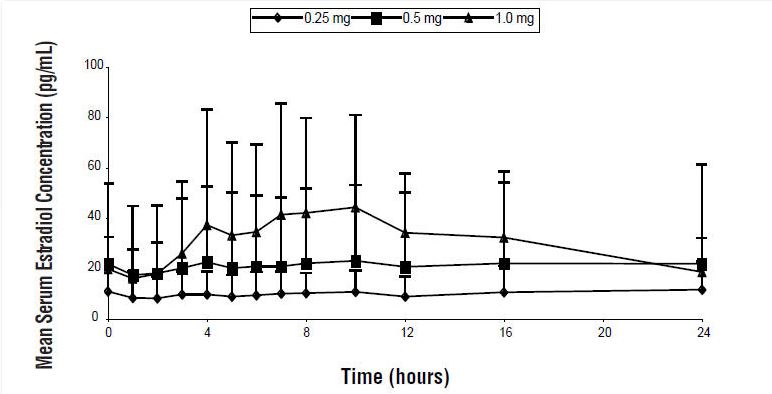
The effect of sunscreens and other topical lotions on the systemic exposure of estradiol gel 0.1% has not been evaluated. Studies conducted using topical estrogen gel approved products have shown that sunscreens have the potential for changing the systemic exposure of topically applied estrogen gels.
Distribution
The distribution of exogenous estrogens is similar to that of endogenous estrogens. Estrogens are widely distributed in the body and are generally found in higher concentrations in the sex hormone target organs. Estrogens circulate in the blood largely bound to SHBG and albumin.
Metabolism
Exogenous estrogens are metabolized in the same manner as endogenous estrogens. Circulating estrogens exist in a dynamic equilibrium of metabolic interconversions. These transformations take place mainly in the liver. Estradiol is converted reversibly to estrone, and both can be converted to estriol, which is a major urinary metabolite. Estrogens also undergo enterohepatic recirculation via sulfate and glucuronide conjugation in the liver, biliary secretion of conjugates into the intestine, and hydrolysis in the intestine followed by reabsorption. In postmenopausal women, a significant proportion of the circulating estrogens exist as sulfate conjugates, especially estrone sulfate, which serves as a circulating reservoir for the formation of more active estrogens.
Although the clinical significance has not been determined, estradiol from estradiol gel 0.1% does not undergo first pass metabolism and provides estradiol to estrone ratios at steady state in the range of 0.42 to 0.65.
Excretion
Estradiol, estrone, and estriol are excreted in the urine along with glucuronide and sulfate conjugates. The apparent terminal half-life for estradiol was about 10 hours following administration of estradiol gel 0.1%.
Potential for Estradiol Transfer
The effect of estradiol transfer was evaluated in healthy postmenopausal women who topically applied 1.0 gram of estradiol gel 0.1% (single dose) on one thigh. One and 8 hours after gel application, they engaged in direct thigh-to-arm contact with a partner for 15 minutes. While some elevation of estradiol levels over baseline was seen in the male subjects, the degree of transferability in this study was inconclusive.
Effects of Washing
The effect of application site washing on skin surface levels and serum concentrations of estradiol was determined in 16 healthy postmenopausal women after application of 1.0 gram of estradiol gel 0.1% to a 200 cm 2 area on the thigh. Washing the application site with soap and water 1 hour after application removed all detectable amounts of estradiol from the surface of the skin and resulted in a 30 to 38 percent decrease in the mean total 24-hour exposure to estradiol.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, and Impairment of Fertility
Long-term continuous administration of natural and synthetic estrogens in certain animal species increases the frequency of carcinomas of the breast, uterus, cervix, vagina, testis and liver.
CLINICAL STUDIES
Effects on Vasomotor Symptoms in Postmenopausal Women
A randomized, double-blind, placebo-controlled trial evaluated the efficacy of 12-week treatment with three different daily doses of estradiol gel 0.1% for vasomotor symptoms in 495 postmenopausal women (86.5 percent White; 10.1 percent Black) between 34 and 89 years of age (mean age 54.6) who had at least 50 moderate to severe hot flushes per week at baseline (2-week period prior to treatment). Women applied placebo, estradiol gel 0.1% 0.25 grams (0.25 mg estradiol), estradiol gel 0.1% 0.5 grams (0.5 mg estradiol) or estradiol gel 0.1% 1.0 gram (1.0 mg estradiol) once daily to the thigh. Reductions in both the median daily frequency and the median daily severity of moderate to severe hot flushes were statistically significant for the 0.5 grams per day and the 1.0 gram per day estradiol gel 0.1% doses when compared to placebo at week 4. Statistically significant reductions in both the median daily frequency and the median daily severity of moderate to severe hot flushes for the estradiol gel 0.1% 0.25 grams per day dose when compared to placebo were delayed to week 7. There were statistically significant reductions in median daily frequency and severity of hot flushes for all three estradiol gel 0.1% doses (0.25 grams per day, 0.5 grams per day and 1.0 gram per day) compared to placebo at week 12. See Table 3 for results.
Table 3: Summary of Change From Baseline in the Median Daily Frequency and Severity of Hot Flushes during Estradiol Gel 0.1% Treatment (ITT Population)
| Estradiol Gel 0.1% | Placebo | |||
| Evaluation | 0.25 grams/day N=121 | 0.5 grams/day N=119 | 1.0 gram/day N=124 | N=124 |
| Frequency of Daily Hot Flushes | ||||
| Baseline Median | 9.72 | 9.24 | 9.64 | 9.32 |
Median Change: Week 4 p-value † | -5.00 0.132 | -5.73 0.011 | -7.20 <0.001 | -3.63 |
Median Change: Week 7 p-value † | -6.62 <0.001 | -7.14 <0.001 | -7.71 <0.001 | -4.37 |
Median Change: Week 12 p-value † | -6.88 <0.001 | -7.29 <0.001 | -8.35 <0.001 | -4.48 |
| Severity of Daily Hot Flushes | ||||
| Baseline Median | 2.52 | 2.51 | 2.52 | 2.54 |
Median Change: Week 4 p-value † | -0.07 0.283 | -0.18 <0.001 | -0.47 <0.001 | -0.04 |
Median Change: Week 7 p-value † | -0.24 <0.001 | -0.46 <0.001 | -1.06 <0.001 | -0.06 |
Median Change: Week 12 p-value † | -0.33 0.021 | -0.56 0.002 | -1.69 <0.001 | -0.13 |
† p-values from the van Elteren’s test stratified by pooled center; comparison in median change was significant if p<0.05.
Women's Health Initiative Estrogen-Alone Trial
The WHI estrogen-alone trial enrolled predominantly healthy postmenopausal women in trial to assess the risks and benefits of daily oral CE (0.625 mg)-alone compared to placebo in the prevention of certain chronic diseases. The primary endpoint was the incidence of CHD (defined as nonfatal MI, silent MI and CHD death), with invasive breast cancer as the primary adverse outcome. A "global index" included the earliest occurrence of CHD, invasive breast cancer, stroke, PE, colorectal cancer, hip fracture, or death due to other cause. This trial did not evaluate the effects of CE- alone on menopausal symptoms.
The WHI estrogen-alone trial was stopped early because an increased risk of stroke was observed, and it was deemed that no further information would be obtained regarding the risks and benefits of estrogen-alone in predetermined primary endpoints. Centrally adjudicated results for stroke events, after an average follow-up of 7.1 years, reported estrogen-alone increased the risk for ischemic stroke compared to placebo, and this excess risk was present in all subgroups of women examined.
No overall difference for primary CHD events (nonfatal MI, silent MI and CHD death) and invasive breast cancer incidence in women receiving CE-alone compared to placebo was reported in final centrally adjudicated results from the estrogen-alone trial, after an average follow-up of 7.1 years. 3,4
Results of the estrogen-alone trial, which included 10,739 women (average age of 63 years, range 50 to 79; 75.3% White, 15.1% Black, 6.1% Hispanic, 3.6% Other), after an average follow-up of 7.1 years are presented in Table A.
Table A: Relative Risk and Risk Difference Observed in the WHI Estrogen-Alone Trial at an Average of 7.1 Years of Follow-up a
| Event | Relative Ratio (95% CI) c | Risk Difference (CE vs placebo/10,000 WYs) |
CHD events Non-fatal MI CHD death | 0.94 (0.78-1.14) 0.97 (0.79-1.21) 1.00 (0.77-1.31) | -3 (55 vs 58) -1 (44 vs 45) 0 (29 vs 29) |
| All Strokes | 1.35 (1.07-1.70) | 11 (45 vs 34) |
| Deep vein thrombosis d | 1.48 (1.06-2.07) | 7 (23 vs 15) |
| Pulmonary embolism | 1.35 (0.89-2.05) | 4 (14 vs 10) |
| Invasive breast cancer e | 0.79 (0.61-1.02) | -7 (28 vs 35) |
| Colorectal cancer | 1.15 (0.81-1.64) | 2 (17 vs 15) |
| Hip fracture | 0.67 (0.46-0.96) | -6 (13 vs 19) |
| Vertebral fractures d | 0.64 (0.44-0.93) | -6 (12 vs 18) |
| Total fractures d | 0.72 (0.64-0.80) | -61 (153 vs 214) |
| Overall mortality c,f | 1.03 (0.88-1.21) | 3 (80 vs 77) |
| Global Index g | 1.03 (0.93-1.13) | 4 (208 vs 204) |
a Adapted from 2013 WHI trial (CE n=5,310, placebo n=5,429). WHI publications can be viewed at www.nhlbi.nih.gov/whi.
b Results are based on centrally adjudicated data.
c In the WHI studies, hazard ratios were estimated using Cox proportional hazards models comparing treatment to placebo; however, they are described here as relative risks. Nominal confidence intervals unadjusted for multiple looks and multiple comparisons.
d Not included in “global index.”
e Includes metastatic and non-metastatic breast cancer with the exception of in situ cancer.
f All deaths, except from breast or colorectal cancer, definite or probable CHD, PE or cerebrovascular disease.
g Asubset of the events was combined in a “global index,” defined as the earliest occurrence of CHD events, invasive breast cancer, stroke, PE, colorectal cancer, hip fracture, or death due to other causes.
Timing of the initiation of estrogen-alone therapy to the start of menopause may affect the overall risk benefit profile. The study results for women 50-59 years old in the WHI estrogen-alone trial are shown in Table B.
Table B: Relative Risk and Risk Difference Observed Among Women 50-59 Years of Age in the WHI Estrogen-Alone Trial at an Average of 7.1 Years a,b
| Event | Relative Ratio (95% CI) c | Risk Difference (CE vs placebo/10,000 WYs) |
CHD events Non-fatal MI CHD death | 0.60 (0.35-1.04) 0.55 (0.31-1.00) 0.80 (0.32-2.04) | -11 (17 vs 28) -11 (14 vs 25) -1 (7 vs 8) |
| All Strokes | 0.99 (0.53-1.85) | -1 (16 vs 17) |
| Deep vein thrombosis d | 1.66 (0.75-3.67) | 5 (13 vs 8) |
| Pulmonary embolism | 1.53 (0.63-3.75) | 4 (10 vs 6) |
| Invasive breast cancer e | 0.82 (0.50-1.34) | -5 (24 vs 29) |
| Colorectal cancer | 0.71 (0.30-1.67) | -3 (7 vs 10) |
| Hip fracture | 5.01 (0.59-42.91) | 3 (1 vs 3) |
| Vertebral fractures d | 0.50 (0.17-1.47) | -4 (4 vs 8) |
| Total fractures d | 0.90 (0.72-1.11) | -16 (133 vs 149) |
| Overall mortality c,f | 0.70 (0.46-1.09) | -11 (29 vs 40) |
| Global Index g | 0.84 (0.66-1.07) | -19 (98 vs 117) |
a Adapted from 2013 WHI trial (CE n=1,639, placebo n=1,674). WHI publications can be viewed at www.nhlbi.nih.gov/whi.
b Results are based on centrally adjudicated data.
c In the WHI studies, hazard ratios were estimated using Cox proportional hazards models comparing treatment to placebo; however, they are described here as relative risks. Nominal confidence intervals unadjusted for multiple looks and multiple comparisons.
d Not included in “global index.”
e Includes metastatic and non-metastatic breast cancer with the exception of in situ cancer.
f All deaths, except from breast or colorectal cancer, definite or probable CHD, PE or cerebrovascular disease.
g A subset of the events was combined in a “global index,” defined as the earliest occurrence of CHD events, invasive breast cancer, stroke, PE, colorectal cancer, hip fracture, or death due to other causes.
Women's Health Initiative Memory Study
The WHIMS estrogen-alone ancillary study of WHI enrolled 2,947 predominantly healthy hysterectomized postmenopausal women 65 to 79 years of age (45% were 65 to 69 years of age, 36% were 70 to 74 years of age, and 19% were 75 years of age and older) to evaluate the effects of daily CE (0.625 mg)-alone on the incidence of probable dementia (primary outcome) compared to placebo. Probable dementia as defined in this study included Alzheimer’s disease (AD), vascular dementia (VaD) and mixed type (having features of both AD and VaD). The most common classification of probable dementia in the treatment group and the placebo group was AD.
After an average follow-up of 5.2 years, the relative risk of probable dementia for CE-alone versus placebo was 1.49 (95% CI, 0.83– 2.66). The absolute risk of probable dementia for CE-alone versus placebo was 37 versus 25 cases per 10,000 women-years. Since the ancillary study was conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women [see Warnings and Precautions (5.3 ), and Use in Specific Populations (8.5 )] . 5
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
Estradiol gel 0.1% is a clear, colorless, smooth, opalescent gel supplied in single-dose foil packets of 0.25, 0.5, 0.75, 1.0, and 1.25 grams, corresponding to 0.25, 0.5, 0.75, 1.0, and 1.25 mg estradiol, respectively.
NDC 70700-143-35, carton of 30 packets, 0.25 mg estradiol per single-dose foil packet
NDC 70700-144-35, carton of 30 packets, 0.5 mg estradiol per single-dose foil packet
NDC 70700-194-35, carton of 30 packets, 0.75 mg estradiol per single-dose foil packet
NDC 70700-145-35, carton of 30 packets, 1.0 mg estradiol per single-dose foil packet
NDC 70700-195-35, carton of 30 packets, 1.25 mg estradiol per single-dose foil packet
Keep out of the reach of children.
Storage and Handling
Store at 20 to 25°C (68 to 77°F). Excursions permitted to 15 to 30°C (59 to 86°F). [See USP Controlled Room Temperature.]
Mechanism of Action
Endogenous estrogens are largely responsible for the development and maintenance of the female reproductive system and secondary sexual characteristics. Although circulating estrogens exist in a dynamic equilibrium of metabolic interconversions, estradiol is the principal intracellular human estrogen and is substantially more potent than its metabolites, estrone and estriol, at the receptor level.
The primary source of estrogen in normally cycling adult women is the ovarian follicle, which secretes 70 to 500 mcg of estradiol daily, depending on the phase of the menstrual cycle. After menopause, most endogenous estrogen is produced by conversion of androstenedione, which is secreted by the adrenal cortex, to estrone in the peripheral tissues. Thus, estrone and the sulfate conjugated form, estrone sulfate, are the most abundant circulating estrogens in postmenopausal women.
Estrogens act through binding to nuclear receptors in estrogen-responsive tissues. To date, two estrogen receptors have been identified. These vary in proportion from tissue to tissue.
Circulating estrogens modulate the pituitary secretion of the gonadotropins, luteinizing hormone (LH) and FSH, through a negative feedback mechanism. Estrogens act to reduce the elevated levels of these hormones seen in postmenopausal women.