Get your patient on Efavirenz - Efavirenz tablet, Film Coated (Efavirenz)
Efavirenz - Efavirenz tablet, Film Coated prescribing information
INDICATIONS AND USAGE
Efavirenz tablets are a non-nucleoside reverse transcriptase inhibitor indicated in combination with other antiretroviral agents for the treatment of human immunodeficiency virus type 1 infection in adults and in pediatric patients at least 3 months old and weighing at least 3.5kg. (1 )
Efavirenz in combination with other antiretroviral agents is indicated for the treatment of human immunodeficiency virus type 1 (HIV-1) infection in adults and in pediatric patients at least 3 months old and weighing at least 3.5 kg.
DOSAGE AND ADMINISTRATION
- Efavirenz should be taken orally once daily on an empty stomach, preferably at bedtime. (2 )
- Recommended adult dose: 600 mg. (2.2 )
- With voriconazole, increase voriconazole maintenance dose to 400 mg every 12 hours and decrease efavirenz dose to 300 mg once daily using the capsule formulation. (2.2 )
- With rifampin, increase efavirenz dose to 800 mg once daily for patients weighing 50 kg or more. (2.2 )
- Pediatric dosing is based on weight. (2.3 )
Hepatic Function
Monitor hepatic function prior to and during treatment with efavirenz tablets [see Warnings and Precautions (5.9 )].
Efavirenz tablets are not recommended in patients with moderate or severe hepatic impairment (Child Pugh B or C) [see Warnings and Precautions (5.9 ) and Use in Specific Populations (8.6 )] .
Adults
The recommended dosage of efavirenz is 600 mg orally, once daily, in combination with a protease inhibitor and/or nucleoside analogue reverse transcriptase inhibitors (NRTIs). It is recommended that efavirenz be taken on an empty stomach, preferably at bedtime. The increased efavirenz concentrations observed following administration of efavirenz with food may lead to an increase in frequency of adverse reactions [see Clinical Pharmacology (12.3 ) ] . Dosing at bedtime may improve the tolerability of nervous system symptoms [see Warnings and Precautions (5.6 ) , Adverse Reactions (6.1 ) , and Patient Counseling Information (17 )]. Efavirenz tablets should be swallowed intact with liquid.
Concomitant Antiretroviral Therapy
Efavirenz must be given in combination with other antiretroviral medications [see Indications and Usage (1 ) , Warnings and Precautions (5.3 ) , Drug Interactions (7.1 ) , and Clinical Pharmacology (12.3 ) ] .
Dosage Adjustment
If efavirenz is coadministered with voriconazole, the voriconazole maintenance dose should be increased to 400 mg every 12 hours and the efavirenz dose should be decreased to 300 mg once daily using the capsule formulation. Efavirenz tablets must not be broken [see Drug Interactions (7.1 , Table 5 ) and Clinical Pharmacology (12.3 , Tables 7 and 8 )] .
If efavirenz is coadministered with rifampin to patients weighing 50 kg or more, an increase in the dose of efavirenz to 800 mg once daily is recommended [see Drug Interactions (7.1 , Table 5 ) and Clinical Pharmacology (12.3 , Table 8 )].
Pediatric Patients
It is recommended that efavirenz be taken on an empty stomach, preferably at bedtime. Table 1 describes the recommended dose of efavirenz for pediatric patients weighing at least 40 kg [see Clinical Pharmacology (12.3 ) ] . The recommended dosage of efavirenz for pediatric patients weighing 40 kg or greater is 600 mg once daily.
b Tablets must not be crushed. | ||
| Patient Body Weight | Efavirenz Daily Dose | Number of Tablets b and Strength to Administer |
| at least 40 kg | 600 mg | one 600 mg tablet |
DOSAGE FORMS AND STRENGTHS
- Tablets: 600 mg (3)
- Tablets
600-mg tablets are yellow coloured, capsule-shaped, biconvex, film coated tablets debossed with '301' on one side and 'CL' on other side.
USE IN SPECIFIC POPULATIONS
- Lactation: Breastfeeding not recommended. (8.2 )
- Females and Males of Reproductive Potential: Pregnancy testing and contraception are recommended. (8.3 )
- Hepatic impairment: Efavirenz is not recommended for patients with moderate or severe hepatic impairment. Use caution in patients with mild hepatic impairment. (8.6 )
- Pediatric patients : The incidence of rash was higher than in adults. (5.8 , 6.2 , 8.4 )
Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to efavirenz during pregnancy. Physicians are encouraged to register patients by calling the Antiretroviral Pregnancy Registry at 1-800-258-4263.
Risk Summary
There are retrospective case reports of neural tube defects in infants whose mothers were exposed to efavirenz-containing regimens in the first trimester of pregnancy. Prospective pregnancy data from the Antiretroviral Pregnancy Registry are not sufficient to adequately assess this risk. Available data from the Antiretroviral Pregnancy Registry show no difference in the risk of overall major birth defects compared to the background rate for major birth defects of 2.7% in the U.S. reference population of the Metropolitan Atlanta Congenital Defects Program (MACDP). Although a causal relationship has not been established between exposure to efavirenz in the first trimester and neural tube defects, similar malformations have been observed in studies conducted in monkeys at doses similar to the human dose. In addition, fetal and embryonic toxicities occurred in rats, at a dose ten times less than the human exposure at recommended clinical dose. Because of the potential risk of neural tube defects, efavirenz should not be used in the first trimester of pregnancy. Advise pregnant women of the potential risk to a fetus.
Data
Human Data
There are retrospective postmarketing reports of findings consistent with neural tube defects, including meningomyelocele, all in infants of mothers exposed to efavirenz-containing regimens in the first trimester.
Based on prospective reports from the Antiretroviral Pregnancy Registry (APR) of approximately 1000 live births following exposure to efavirenz-containing regimens (including over 800 live births exposed in the first trimester), there was no difference between efavirenz and overall birth defects compared with the background birth defect rate of 2.7% in the U.S. reference population of the Metropolitan Atlanta Congenital Defects Program. As of the interim APR report issued December 2014, the prevalence of birth defects following first-trimester exposure was 2.3% (95% CI: 1.4%-3.6%). One of these prospectively reported defects with first-trimester exposure was a neural tube defect. A single case of anophthalmia with first-trimester exposure to efavirenz has also been prospectively reported. This case also included severe oblique facial clefts and amniotic banding, which have a known association with anophthalmia.
Animal Data
Effects of efavirenz on embryo-fetal development have been studied in three nonclinical species (cynomolgus monkeys, rats, and rabbits). In monkeys, efavirenz 60 mg/kg/day was administered to pregnant females throughout pregnancy (gestation days 20 through 150). The maternal systemic drug exposures (AUC) were 1.3 times the exposure in humans at the recommended clinical dose (600 mg/day), with fetal umbilical venous drug concentrations approximately 0.7 times the maternal values. Three of 20 fetuses/infants had one or more malformations; there were no malformed fetuses or infants from placebo-treated mothers. The malformations that occurred in these three monkey fetuses included anencephaly and unilateral anophthalmia in one fetus, microphthalmia in a second, and cleft palate in the third. There was no NOAEL (no observable adverse effect level) established for this study because only one dosage was evaluated. In rats, efavirenz was administered either during organogenesis (gestation days 7 to 18) or from gestation day 7 through lactation day 21 at 50, 100, or 200 mg/kg/day. Administration of 200 mg/kg/day in rats was associated with increase in the incidence of early resorptions; and doses 100 mg/kg/day and greater were associated with early neonatal mortality. The AUC at the NOAEL (50 mg/kg/day) in this rat study was 0.1 times that in humans at the recommended clinical dose. Drug concentrations in the milk on lactation day 10 were approximately 8 times higher than those in maternal plasma. In pregnant rabbits, efavirenz was neither embryo lethal nor teratogenic when administered at doses of 25, 50, and 75 mg/kg/day over the period of organogenesis (gestation days 6 through 18). The AUC at the NOAEL (75 mg/kg/day) in rabbits was 0.4 times that in humans at the recommended clinical dose.
Lactation
Risk Summary
The Centers for Disease Control and Prevention recommend that HIV-infected mothers not breastfeed their infants to avoid risking postnatal transmission of HIV. Because of the potential for HIV transmission in breastfed infants, advise women not to breastfeed.
Females and Males of Reproductive Potential
Because of potential teratogenic effects, pregnancy should be avoided in women receiving efavirenz [see Use in Specific Populations (8.1 )] .
Pregnancy Testing
Females of reproductive potential should undergo pregnancy testing before initiation of efavirenz.
Contraception
Females of reproductive potential should use effective contraception during treatment with efavirenz and for 12 weeks after discontinuing efavirenz due to the long half-life of efavirenz. Barrier contraception should always be used in combination with other methods of contraception. Hormonal methods that contain progesterone may have decreased effectiveness [see Drug Interactions (7.1 )] .
Pediatric Use
The safety, pharmacokinetic profile, and virologic and immunologic responses of efavirenz were evaluated in antiretroviral-naive and -experienced HIV-1 infected pediatric patients 3 months to 21 years of age in three open-label clinical trials [see Adverse Reactions (6.2 ), Clinical Pharmacology (12.3 ), and Clinical Studies (14.2 ) ] . The type and frequency of adverse reactions in these trials were generally similar to those of adult patients with the exception of a higher frequency of rash, including a higher frequency of Grade 3 or 4 rash, in pediatric patients compared to adults [see Warnings and Precautions (5.8 ) and Adverse Reactions 6.2 ) ] .
Use of efavirenz in patients younger than 3 months of age OR less than 3.5 kg body weight is not recommended because the safety, pharmacokinetics, and antiviral activity of efavirenz have not been evaluated in this age group and there is a risk of developing HIV resistance if efavirenz is underdosed. See Dosage and Administration (2.2 ) for dosing recommendations for pediatric patients.
Geriatric Use
Clinical studies of efavirenz did not include sufficient numbers of subjects aged 65 years and over to determine whether they respond differently from younger subjects. In general, dose selection for an elderly patient should be cautious, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other therapy.
Hepatic Impairment
Efavirenz is not recommended for patients with moderate or severe hepatic impairment because there are insufficient data to determine whether dose adjustment is necessary. Patients with mild hepatic impairment may be treated with efavirenz without any adjustment in dose. Because of the extensive cytochrome P450-mediated metabolism of efavirenz and limited clinical experience in patients with hepatic impairment, caution should be exercised in administering efavirenz to these patients [see Warnings and Precautions (5.9 ) and Clinical Pharmacology (12.3 ) ] .
CONTRAINDICATIONS
- Efavirenz is contraindicated in patients with previously demonstrated clinically significant hypersensitivity (e.g., Stevens-Johnson syndrome, erythema multiforme, or toxic skin eruptions) to any of the components of this product.
- Coadministration of efavirenz with elbasvir and grazoprevir is contraindicated [see Warnings and Precautions (5.1 ) and Drug Interactions (7.1 )].
WARNINGS AND PRECAUTIONS
- QTc prolongation: Consider alternatives to efavirenz in patients taking other medications with a known risk of Torsade de Pointes or in patients at higher risk of Torsade de Pointes. (5.2 )
- Do not use as a single agent or add on as a sole agent to a failing regimen. Consider potential for cross-resistance when choosing other agents. (5.3 )
- Not recommended with ATRIPLA, which contains efavirenz, emtricitabine, and tenofovir disoproxil fumarate, unless needed for dose adjustment when coadministered with rifampin. (5.4 )
- Serious psychiatric symptoms: Immediate medical evaluation is recommended for serious psychiatric symptoms such as severe depression or suicidal ideation. (5.5 , 17 )
- Nervous system symptoms (NSS): NSS are frequent and usually begin 1-2 days after initiating therapy and resolve in 2-4 weeks. Dosing at bedtime may improve tolerability. NSS are not predictive of onset of psychiatric symptoms. (5.6 , 6.1 , 17 )
- Embryo-Fetal Toxicity: Avoid administration in the first trimester of pregnancy as fetal harm may occur. (5.7 , 8.1 )
- Hepatotoxicity: Monitor liver function tests before and during treatment in patients with underlying hepatic disease, including hepatitis B or C coinfection, marked transaminase elevations, or who are taking medications associated with liver toxicity. Among reported cases of hepatic failure, a few occurred in patients with no pre-existing hepatic disease. (5.9 , 6.1 , 8.6 )
- Rash: Rash usually begins within 1-2 weeks after initiating therapy and resolves within 4 weeks. Discontinue if severe rash develops. (5.8 , 6.1 , 17 )
- Convulsions: Use caution in patients with a history of seizures. (5.10 )
- Lipids: Total cholesterol and triglyceride elevations. Monitor before therapy and periodically thereafter. (5.11 )
- Immune reconstitution syndrome: May necessitate further evaluation and treatment. (5.12 )
- Redistribution/accumulation of body fat: Observed in patients receiving antiretroviral therapy. (5.13 , 17 )
Drug Interactions
Efavirenz plasma concentrations may be altered by substrates, inhibitors, or inducers of CYP3A. Likewise, efavirenz may alter plasma concentrations of drugs metabolized by CYP3A or CYP2B6. The most prominent effect of efavirenz at steady state is induction of CYP3A and CYP2B6 [see Dosage and Administration (2.2 ) and Drug Interactions (7.1 )].
QTc Prolongation
QTc prolongation has been observed with the use of efavirenz [see Drug Interactions (7.3 , 7.4 ) and Clinical Pharmacology (12.2 )]. Consider alternatives to efavirenz when coadministered with a drug with a known risk of Torsade de Pointes or when administered to patients at higher risk of Torsade de Pointes.
Resistance
Efavirenz must not be used as a single agent to treat HIV-1 infection or added on as a sole agent to a failing regimen. Resistant virus emerges rapidly when efavirenz is administered as monotherapy. The choice of new antiretroviral agents to be used in combination with efavirenz should take into consideration the potential for viral cross-resistance.
Coadministration with Related Products
Coadministration of efavirenz with ATRIPLA (efavirenz 600 mg/emtricitabine 200 mg/tenofovir disoproxil fumarate 300 mg) is not recommended unless needed for dose adjustment (e.g., with rifampin), since efavirenz is one of its active ingredients.
Psychiatric Symptoms
Serious psychiatric adverse experiences have been reported in patients treated with efavirenz. In controlled trials of 1008 patients treated with regimens containing efavirenz for a mean of 2.1 years and 635 patients treated with control regimens for a mean of 1.5 years, the frequency (regardless of causality) of specific serious psychiatric events among patients who received efavirenz or control regimens, respectively, were severe depression (2.4%, 0.9%), suicidal ideation (0.7%, 0.3%), nonfatal suicide attempts (0.5%, 0), aggressive behavior (0.4%, 0.5%), paranoid reactions (0.4%, 0.3%), and manic reactions (0.2%, 0.3%). When psychiatric symptoms similar to those noted above were combined and evaluated as a group in a multifactorial analysis of data from Study 006, treatment with efavirenz was associated with an increase in the occurrence of these selected psychiatric symptoms. Other factors associated with an increase in the occurrence of these psychiatric symptoms were history of injection drug use, psychiatric history, and receipt of psychiatric medication at study entry; similar associations were observed in both the efavirenz and control treatment groups. In Study 006, onset of new serious psychiatric symptoms occurred throughout the study for both efavirenz-treated and control-treated patients. One percent of efavirenz-treated patients discontinued or interrupted treatment because of one or more of these selected psychiatric symptoms. There have also been occasional postmarketing reports of death by suicide, delusions, and psychosis-like behavior although a causal relationship to the use of efavirenz cannot be determined from these reports. Postmarketing cases of catatonia have also been reported and may be associated with increased efavirenz exposure. Patients with serious psychiatric adverse experiences should seek immediate medical evaluation to assess the possibility that the symptoms may be related to the use of efavirenz, and if so, to determine whether the risks of continued therapy outweigh the benefits [see Adverse Reactions (6.1 ) ] .
Nervous System Symptoms
Fifty-three percent (531/1008) of patients receiving efavirenz in controlled trials reported central nervous system symptoms (any grade, regardless of causality) compared to 25% (156/635) of patients receiving control regimens [see Adverse Reactions (6.1 , Table 3 ) ] . These symptoms included, but were not limited to, dizziness (28.1% of the 1008 patients), insomnia (16.3%), impaired concentration (8.3%), somnolence (7.0%), abnormal dreams (6.2%), and hallucinations (1.2%). These symptoms were severe in 2.0% of patients; and 2.1% of patients discontinued therapy as a result. These symptoms usually begin during the first or second day of therapy and generally resolve after the first 2-4 weeks of therapy. After 4 weeks of therapy, the prevalence of nervous system symptoms of at least moderate severity ranged from 5% to 9% in patients treated with regimens containing efavirenz and from 3% to 5% in patients treated with a control regimen. Patients should be informed that these common symptoms were likely to improve with continued therapy and were not predictive of subsequent onset of the less frequent psychiatric symptoms [see Warnings and Precautions (5.5 ) ]. Dosing at bedtime may improve the tolerability of these nervous system symptoms [see Dosage and Administration (2 ) ] .
Analysis of long-term data from Study 006 (median follow-up 180 weeks, 102 weeks, and 76 weeks for patients treated with efavirenz + zidovudine + lamivudine, efavirenz + indinavir, and indinavir + zidovudine + lamivudine, respectively) showed that, beyond 24 weeks of therapy, the incidences of new-onset nervous system symptoms among efavirenz-treated patients were generally similar to those in the indinavir-containing control arm.
Late-onset neurotoxicity, including ataxia and encephalopathy (impaired consciousness, confusion, psychomotor slowing, psychosis, delirium), may occur months to years after beginning efavirenz therapy. Some events of late-onset neurotoxicity have occurred in patients with CYP2B6 genetic polymorphisms which are associated with increased efavirenz levels despite standard dosing of efavirenz. Patients presenting with signs and symptoms of serious neurologic adverse experiences should be evaluated promptly to assess the possibility that these events may be related to efavirenz use, and whether discontinuation of efavirenz is warranted.
Patients receiving efavirenz should be alerted to the potential for additive central nervous system effects when efavirenz is used concomitantly with alcohol or psychoactive drugs.
Patients who experience central nervous system symptoms such as dizziness, impaired concentration, and/or drowsiness should avoid potentially hazardous tasks such as driving or operating machinery.
Embryo-Fetal Toxicity
Rash
In controlled clinical trials, 26% (266/1008) of adult patients treated with 600 mg efavirenz experienced new-onset skin rash compared with 17% (111/635) of those treated in control groups [see Adverse Reactions (6.1 )]. Rash associated with blistering, moist desquamation, or ulceration occurred in 0.9% (9/1008) of patients treated with efavirenz. The incidence of Grade 4 rash (e.g., erythema multiforme, Stevens-Johnson syndrome) in adult patients treated with efavirenz in all studies and expanded access was 0.1%. Rashes are usually mild-to-moderate maculopapular skin eruptions that occur within the first 2 weeks of initiating therapy with efavirenz (median time to onset of rash in adults was 11 days) and, in most patients continuing therapy with efavirenz, rash resolves within 1 month (median duration, 16 days). The discontinuation rate for rash in adult clinical trials was 1.7% (17/1008).
Rash was reported in 59 of 182 pediatric patients (32%) treated with efavirenz [see Adverse Reactions (6.2 )] . Two pediatric patients experienced Grade 3 rash (confluent rash with fever, generalized rash), and four patients had Grade 4 rash (erythema multiforme). The median time to onset of rash in pediatric patients was 28 days (range 3-1642 days). Prophylaxis with appropriate antihistamines before initiating therapy with efavirenz in pediatric patients should be considered.
Efavirenz can generally be reinitiated in patients interrupting therapy because of rash. Efavirenz should be discontinued in patients developing severe rash associated with blistering, desquamation, mucosal involvement, or fever. Appropriate antihistamines and/or corticosteroids may improve the tolerability and hasten the resolution of rash. For patients who have had a life-threatening cutaneous reaction (e.g., Stevens-Johnson syndrome), alternative therapy should be considered [see Contraindications (4 ) ] .
Hepatotoxicity
Postmarketing cases of hepatitis, including fulminant hepatitis progressing to liver failure requiring transplantation or resulting in death, have been reported in patients treated with efavirenz. Reports have included patients with underlying hepatic disease, including coinfection with hepatitis B or C, and patients without pre-existing hepatic disease or other identifiable risk factors.
Efavirenz is not recommended for patients with moderate or severe hepatic impairment. Careful monitoring is recommended for patients with mild hepatic impairment receiving efavirenz. [see Adverse Reactions (6.1 ) and Use in Specific Populations (8.6 )].
Monitoring of liver enzymes before and during treatment is recommended for all patients [see Dosage and Administration (2.1 )] . Consider discontinuing efavirenz in patients with persistent elevations of serum transaminases to greater than five times the upper limit of the normal range.
Discontinue efavirenz if elevation of serum transaminases is accompanied by clinical signs or symptoms of hepatitis or hepatic decompensation.
Convulsions
Convulsions have been observed in adult and pediatric patients receiving efavirenz, generally in the presence of known medical history of seizures [see Nonclinical Toxicology (13.2 ) ] . Caution should be taken in any patient with a history of seizures. Patients who are receiving concomitant anticonvulsant medications primarily metabolized by the liver, such as phenytoin and phenobarbital, may require periodic monitoring of plasma levels [see Drug Interactions (7.1 ) ] .
Lipid Elevations
Treatment with efavirenz has resulted in increases in the concentration of total cholesterol and triglycerides [see Adverse Reactions (6.1 ) ] . Cholesterol and triglyceride testing should be performed before initiating efavirenz therapy and at periodic intervals during therapy.
Immune Reconstitution Syndrome
Immune reconstitution syndrome has been reported in patients treated with combination antiretroviral therapy, including efavirenz. During the initial phase of combination antiretroviral treatment, patients whose immune system responds may develop an inflammatory response to indolent or residual opportunistic infections (such as Mycobacterium avium infection, cytomegalovirus, Pneumocystis jirovecii pneumonia [PCP], or tuberculosis), which may necessitate further evaluation and treatment.
Autoimmune disorders (such as Graves' disease, polymyositis, Guillain-Barre syndrome, and autoimmune hepatitis) have also been reported to occur in the setting of immune reconstitution; however, the time to onset is more variable, and can occur many months after initiation of treatment.
Fat Redistribution
Redistribution/accumulation of body fat including central obesity, dorsocervical fat enlargement (buffalo hump), peripheral wasting, facial wasting, breast enlargement, and "cushingoid appearance" have been observed in patients receiving antiretroviral therapy. The mechanism and long-term consequences of these events are currently unknown. A causal relationship has not been established.
ADVERSE REACTIONS
The most significant adverse reactions observed in patients treated with efavirenz are:
Clinical Trials Experience
Because clinical studies are conducted under widely varying conditions, the adverse reaction rates reported cannot be directly compared to rates in other clinical studies and may not reflect the rates observed in clinical practice.
Adverse Reactions in Adults
The most common (>5% in either efavirenz treatment group) adverse reactions of at least moderate severity among patients in Study 006 treated with efavirenz in combination with zidovudine/lamivudine or indinavir were rash, dizziness, nausea, headache, fatigue, insomnia, and vomiting.
Selected clinical adverse reactions of moderate or severe intensity observed in ≥2% of efavirenz-treated patients in two controlled clinical trials are presented in Table 2 .
a Includes adverse events at least possibly related to study drug or of unknown relationship for Study 006. Includes all adverse events regardless of relationship to study drug for Study ACTG 364. | ||||||
b Efavirenz provided as 600 mg once daily. | ||||||
c Median duration of treatment. | ||||||
d Includes erythema multiforme, rash, rash erythematous, rash follicular, rash maculopapular, rash petechial, rash pustular, and urticaria for Study 006 and macules, papules, rash, erythema, redness, inflammation, allergic rash, urticaria, welts, hives, itchy, and pruritus for ACTG 364. | ||||||
– = Not Specified. | ||||||
ZDV = zidovudine, LAM = lamivudine. | ||||||
| Adverse Reactions | Study 006 | LAM-, NNRTI-, and | Protease Inhibitor- Naive Patients | Study ACTG 364 NNRTI- ,and Protease | NRTI-experienced, Inhibitor-Naive | Patients |
| Efavirenz b +ZDV/LAM (n=412) 180 weeks c | Efavirenz b +Indinavir (n=415) 102 weeks c | Indinavir +ZDV/LAM (n=401) 76 weeks c | Efavirenz b +Nelfinavir + NRTIs (n=64) 71.1 weeks c | Efavirenz b +NRTIs (n=65) 70.9 weeks c | Nelfinavir +NRTIs (n=66) 62.7 weeks c | |
| Body as a Whole | ||||||
| Fatigue | 8% | 5% | 9% | 0 | 2% | 3% |
| Pain | 1% | 2% | 8% | 13% | 6% | 17% |
| Central and Peripheral Nervous System | ||||||
| Dizziness | 9% | 9% | 2% | 2% | 6% | 6% |
| Headache | 8% | 5% | 3% | 5% | 2% | 3% |
| Insomnia | 7% | 7% | 2% | 0 | 0 | 2% |
| Concentration impaired | 5% | 3% | <1% | 0 | 0 | 0 |
| Abnormal dreams | 3% | 1% | 0 | – | – | – |
| Somnolence | 2% | 2% | <1% | 0 | 0 | 0 |
| Anorexia | 1% | <1% | <1% | 0 | 2% | 2% |
| Gastrointestinal | ||||||
| Nausea | 10% | 6% | 24% | 3% | 2% | 2% |
| Vomiting | 6% | 3% | 14% | – | – | – |
| Diarrhea | 3% | 5% | 6% | 14% | 3% | 9% |
| Dyspepsia | 4% | 4% | 6% | 0 | 0 | 2% |
| Abdominal pain | 2% | 2% | 5% | 3% | 3% | 3% |
| Psychiatric | ||||||
| Anxiety | 2% | 4% | <1% | – | – | – |
| Depression | 5% | 4% | <1% | 3% | 0 | 5% |
| Nervousness | 2% | 2% | 0 | 2% | 0 | 2% |
| Skin and Appendages | ||||||
| Rash d | 11% | 16% | 5% | 9% | 5% | 9% |
| Pruritus | <1% | 1% | 1% | 9% | 5% | 9% |
Pancreatitis has been reported, although a causal relationship with efavirenz has not been established. Asymptomatic increases in serum amylase levels were observed in a significantly higher number of patients treated with efavirenz 600 mg than in control patients (see Laboratory Abnormalities ).
Nervous System Symptoms
For 1008 patients treated with regimens containing efavirenz and 635 patients treated with a control regimen in controlled trials, Table 3 lists the frequency of symptoms of different degrees of severity and gives the discontinuation rates for one or more of the following nervous system symptoms: dizziness, insomnia, impaired concentration, somnolence, abnormal dreaming, euphoria, confusion, agitation, amnesia, hallucinations, stupor, abnormal thinking, and depersonalization [see Warnings and Precautions (5.6 )]. The frequencies of specific central and peripheral nervous system symptoms are provided in Table 2 .
a Includes events reported regardless of causality. | ||
b Data from Study 006 and three Phase 2/3 studies. | ||
c "Mild" = Symptoms which do not interfere with patient's daily activities. | ||
d "Moderate" = Symptoms which may interfere with daily activities. | ||
e "Severe" = Events which interrupt patient's usual daily activities. | ||
| Percent of Patients with: | Efavirenz 600 mg Once Daily (n=1008) % | Control Groups (n=635) % |
| Symptoms of any severity | 52.7 | 24.6 |
| Mild symptoms c | 33.3 | 15.6 |
| Moderate symptoms d | 17.4 | 7.7 |
| Severe symptoms e | 2.0 | 1.3 |
| Treatment discontinuation as a result of symptoms | 2.1 | 1.1 |
Psychiatric Symptoms
Serious psychiatric adverse experiences have been reported in patients treated with efavirenz. In controlled trials, psychiatric symptoms observed at a frequency greater than 2% among patients treated with efavirenz or control regimens, respectively, were depression (19%, 16%), anxiety (13%, 9%), and nervousness (7%, 2%).
Rash
In controlled clinical trials, the frequency of rash (all grades, regardless of causality) was 26% for 1008 adults treated with regimens containing efavirenz and 17% for 635 adults treated with a control regimen. Most reports of rash were mild or moderate in severity. The frequency of Grade 3 rash was 0.8% for efavirenz-treated patients and 0.3% for control groups, and the frequency of Grade 4 rash was 0.1% for efavirenz and 0 for control groups. The discontinuation rates as a result of rash were 1.7% for efavirenz-treated patients and 0.3% for control groups [see Warnings and Precautions (5.8 ) ] .
Experience with efavirenz in patients who discontinued other antiretroviral agents of the NNRTI class is limited. Nineteen patients who discontinued nevirapine because of rash have been treated with efavirenz. Nine of these patients developed mild-to-moderate rash while receiving therapy with efavirenz, and two of these patients discontinued because of rash.
Laboratory Abnormalities
Selected Grade 3-4 laboratory abnormalities reported in ≥2% of efavirenz-treated patients in two clinical trials are presented in Table 4 .
a Efavirenz provided as 600 mg once daily. | |||||||
b Median duration of treatment. | |||||||
c Isolated elevations of GGT in patients receiving efavirenz may reflect enzyme induction not associated with liver toxicity. | |||||||
d Nonfasting. | |||||||
ZDV = zidovudine, LAM = lamivudine, ULN = upper limit of normal, ALT = alanine aminotransferase, AST = aspartate aminotransferase, GGT = gamma-glutamyltransferase. | |||||||
| Variable | Limit | Study 006 LAM-, | NNRTI -, Naive Patients | and Protease Inhibitor- | Study ACTG 364, | NRTI-experienced, Protease Inhibitor | NNRTI- and - Naive Patients |
| Efavirenz a +ZDV/LAM (n=412) 180 weeks b | Efavirenz a + Indinavir (n=415) 102 weeks b | Indinavir + ZDV/ LAM (n=401) 76 weeks b | Efavirenz a + Nelfinavir + NRTIs (n=64) 71.1 weeks b | Efavirenz a + NRTIs (n=65) 70.9 weeks b | Nelfinavir + NRTIs (n=66) 62.7 weeks b | ||
| Chemistry | |||||||
| ALT | >5 × ULN | 5% | 8% | 5% | 2% | 6% | 3% |
| AST | >5 × ULN | 5% | 6% | 5% | 6% | 8% | 8% |
| GGT c | >5 × ULN | 8% | 7% | 3% | 5% | 0 | 5% |
| Amylase | >2 × ULN | 4% | 4% | 1% | 0 | 6% | 2% |
| Glucose | >250 mg/dL | 3% | 3% | 3% | 5% | 2% | 3% |
| Triglycerides d | ≥751 mg/dL | 9% | 6% | 6% | 11% | 8% | 17% |
| Hematology | |||||||
| Neutrophils | <750/ mm 3 | 10% | 3% | 5% | 2% | 3% | 2% |
Patients Coinfected with Hepatitis B or C
Liver function tests should be monitored in patients with a history of hepatitis B and/or C. In the long-term data set from Study 006, 137 patients treated with efavirenz-containing regimens (median duration of therapy, 68 weeks) and 84 treated with a control regimen (median duration, 56 weeks) were seropositive at screening for hepatitis B (surface antigen positive) and/or C (hepatitis C antibody positive). Among these coinfected patients, elevations in AST to greater than five times ULN developed in 13% of patients in the efavirenz arms and 7% of those in the control arm, and elevations in ALT to greater than five times ULN developed in 20% of patients in the efavirenz arms and 7% of patients in the control arm. Among coinfected patients, 3% of those treated with efavirenz-containing regimens and 2% in the control arm discontinued from the study because of liver or biliary system disorders [see Warnings and Precautions (5.9 )].
Lipids
Increases from baseline in total cholesterol of 10-20% have been observed in some uninfected volunteers receiving efavirenz. In patients treated with efavirenz + zidovudine + lamivudine, increases from baseline in nonfasting total cholesterol and HDL of approximately 20% and 25%, respectively, were observed. In patients treated with efavirenz + indinavir, increases from baseline in nonfasting cholesterol and HDL of approximately 40% and 35%, respectively, were observed. Nonfasting total cholesterol levels ≥240 mg/dL and ≥300 mg/dL were reported in 34% and 9%, respectively, of patients treated with efavirenz + zidovudine + lamivudine; 54% and 20%, respectively, of patients treated with efavirenz + indinavir; and 28% and 4%, respectively, of patients treated with indinavir + zidovudine + lamivudine. The effects of efavirenz on triglycerides and LDL in this study were not well characterized since samples were taken from nonfasting patients. The clinical significance of these findings is unknown [see Warnings and Precautions (5.11 )].
Adverse Reactions in Pediatric Patients
Because clinical studies are conducted under widely varying conditions, the adverse reaction rates reported cannot be directly compared to rates in other clinical studies and may not reflect the rates observed in clinical practice.
Assessment of adverse reactions is based on three clinical trials in 182 HIV-1 infected pediatric patients (3 months to 21 years of age) who received efavirenz in combination with other antiretroviral agents for a median of 123 weeks. The adverse reactions observed in the three trials were similar to those observed in clinical trials in adults except that rash was more common in pediatric patients (32% for all grades regardless of causality) and more often of higher grade (ie, more severe). Two (1.1%) pediatric patients experienced Grade 3 rash (confluent rash with fever, generalized rash), and four (2.2%) pediatric patients had Grade 4 rash (all erythema multiforme). Five pediatric patients (2.7%) discontinued from the study because of rash [see Warnings and Precautions (5.8 ) ] .
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of efavirenz. Because these reactions are reported voluntarily from a population of unknown size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Body as a Whole: allergic reactions, asthenia, redistribution/accumulation of body fat [see Warnings and Precautions (5.13 ) ] .
Central and Peripheral Nervous System: abnormal coordination, ataxia, encephalopathy, cerebellar coordination and balance disturbances, convulsions, hypoesthesia, paresthesia, neuropathy, tremor, vertigo
Endocrine: gynecomastia
Gastrointestinal: constipation, malabsorption
Cardiovascular: flushing, palpitations
Liver and Biliary System: hepatic enzyme increase, hepatic failure, hepatitis.
Metabolic and Nutritional: hypercholesterolemia, hypertriglyceridemia
Musculoskeletal: arthralgia, myalgia, myopathy
Psychiatric: aggressive reactions, agitation, delusions, emotional lability, mania, neurosis, paranoia, psychosis, suicide, catatonia
Respiratory: dyspnea
Skin and Appendages: erythema multiforme, photoallergic dermatitis, Stevens-Johnson syndrome
Special Senses: abnormal vision, tinnitus
Drug Interactions
Efavirenz plasma concentrations may be altered by substrates, inhibitors, or inducers of CYP3A. Likewise, efavirenz may alter plasma concentrations of drugs metabolized by CYP3A or CYP2B6. The most prominent effect of efavirenz at steady state is induction of CYP3A and CYP2B6 [see Dosage and Administration (2.2 ) and Drug Interactions (7.1 )].
DESCRIPTION
Efavirenz is an HIV-1 specific, non-nucleoside, reverse transcriptase inhibitor (NNRTI). Efavirenz is chemically described as (S)-6-chloro-4-(cyclopropylethynyl)-1,4-dihydro-4-(trifluoromethyl)-2H-3,1-benzoxazin-2-one. Its empirical formula is C 14 H 9 ClF 3 NO 2 and its structural formula is:
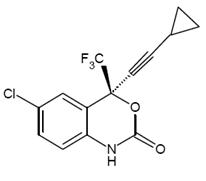
Efavirenz is a white to slightly pink crystalline powder with a molecular mass of 315.68. It is practically insoluble in water (<10 microgram/mL).
Tablets: Efavirenz tablets, USP is available as film-coated tablets for oral administration containing 600 mg of efavirenz and the following inactive ingredients: Lactose monohydrate, croscarmellose sodium, povidone, anhydrous dibasic calcium phosphate, magnesium stearate. The film coating contains opadry yellow (consist of hypromellose, titanium dioxide, macrogol, iron oxide yellow).
CLINICAL PHARMACOLOGY
Mechanism of Action
Efavirenz is an antiviral drug [see Microbiology (12.4 ) ] .
Pharmacodynamics
Cardiac Electrophysiology
The effect of efavirenz on the QTc interval was evaluated in an open-label, positive and placebo controlled, fixed single sequence 3-period, 3-treatment crossover QT study in 58 healthy subjects enriched for CYP2B6 polymorphisms. The mean C max of efavirenz in subjects with CYP2B6 •6/•6 genotype following the administration of 600 mg daily dose for 14 days was 2.25-fold the mean C max observed in subjects with CYP2B6 •1/•1 genotype. A positive relationship between efavirenz concentration and QTc prolongation was observed. Based on the concentration-QTc relationship, the mean QTc prolongation and its upper bound 90% confidence interval are 8.7 ms and 11.3 ms in subjects with CYP2B6•6/•6 genotype following the administration of 600 mg daily dose for 14 days [see Warnings and Precautions (5.2 )].
Pharmacokinetics
Absorption
Peak efavirenz plasma concentrations of 1.6-9.1 μM were attained by 5 hours following single oral doses of 100 mg to 1600 mg administered to uninfected volunteers. Dose-related increases in C max and AUC were seen for doses up to 1600 mg; the increases were less than proportional suggesting diminished absorption at higher doses.
In HIV-1-infected patients at steady state, mean C max , mean C min , and mean AUC were dose proportional following 200 mg, 400 mg, and 600 mg daily doses. Time-to-peak plasma concentrations were approximately 3-5 hours and steady-state plasma concentrations were reached in 6-10 days. In 35 patients receiving efavirenz 600 mg once daily, steady-state C max was 12.9 ± 3.7 μM (mean ± SD), steady-state C min was 5.6 ± 3.2 μM, and AUC was 184 ± 73 μM•h.
Effect of Food on Oral Absorption:
Tablets: Administration of a single 600 mg efavirenz tablet with a high-fat/high-caloric meal (approximately 1000 kcal, 500-600 kcal from fat) was associated with a 28% increase in mean AUC ∞ of efavirenz and a 79% increase in mean C max of efavirenz relative to the exposures achieved under fasted conditions [See Dosage and Administration (2 ) and Patient Counseling Information (17 )] .
Distribution
Efavirenz is highly bound (approximately 99.5-99.75%) to human plasma proteins, predominantly albumin. In HIV-1 infected patients (n=9) who received efavirenz 200 to 600 mg once daily for at least one month, cerebrospinal fluid concentrations ranged from 0.26 to 1.19% (mean 0.69%) of the corresponding plasma concentration. This proportion is approximately 3-fold higher than the non-protein-bound (free) fraction of efavirenz in plasma.
Metabolism
Studies in humans and in vitro studies using human liver microsomes have demonstrated that efavirenz is principally metabolized by the cytochrome P450 system to hydroxylated metabolites with subsequent glucuronidation of these hydroxylated metabolites. These metabolites are essentially inactive against HIV-1. The in vitro studies suggest that CYP3A and CYP2B6 are the major isozymes responsible for efavirenz metabolism.
Efavirenz has been shown to induce CYP enzymes, resulting in the induction of its own metabolism. Multiple doses of 200-400 mg per day for 10 days resulted in a lower than predicted extent of accumulation (22-42% lower) and a shorter terminal half-life of 40-55 hours (single dose half-life 52-76 hours).
Elimination
Efavirenz has a terminal half-life of 52-76 hours after single doses and 40-55 hours after multiple doses. A one-month mass balance/excretion study was conducted using 400 mg per day with a 14 C-labeled dose administered on Day 8. Approximately 14-34% of the radiolabel was recovered in the urine and 16-61% was recovered in the feces. Nearly all of the urinary excretion of the radiolabeled drug was in the form of metabolites. Efavirenz accounted for the majority of the total radioactivity measured in feces.
Special Populations
Pediatric: The pharmacokinetic parameters for efavirenz at steady state in pediatric patients were predicted by a population pharmacokinetic model and are summarized in Table 6 by weight ranges that correspond to the recommended doses.
| Body Weight | Dose | Mean AUC (0-24) µM•h | Mean C max µg/mL | Mean C min µg/mL |
| 3.5-5 kg | 100 mg | 220.52 | 5.81 | 2.43 |
| 5-7.5 kg | 150 mg | 262.62 | 7.07 | 2.71 |
| 7.5-10 kg | 200 mg | 284.28 | 7.75 | 2.87 |
| 10-15 kg | 200 mg | 238.14 | 6.54 | 2.32 |
| 15-20 kg | 250 mg | 233.98 | 6.47 | 2.3 |
| 20-25 kg | 300 mg | 257.56 | 7.04 | 2.55 |
| 25-32.5 kg | 350 mg | 262.37 | 7.12 | 2.68 |
| 32.5-40 kg | 400 mg | 259.79 | 6.96 | 2.69 |
| >40 kg | 600 mg | 254.78 | 6.57 | 2.82 |
Gender and race: The pharmacokinetics of efavirenz in patients appear to be similar between men and women and among the racial groups studied.
Renal impairment: The pharmacokinetics of efavirenz have not been studied in patients with renal insufficiency; however, less than 1% of efavirenz is excreted unchanged in the urine, so the impact of renal impairment on efavirenz elimination should be minimal.
Hepatic impairment: A multiple-dose study showed no significant effect on efavirenz pharmacokinetics in patients with mild hepatic impairment (Child-Pugh Class A) compared with controls. There were insufficient data to determine whether moderate or severe hepatic impairment (Child-Pugh Class B or C) affects efavirenz pharmacokinetics.
Drug Interaction Studies
Efavirenz has been shown in vivo to cause hepatic enzyme induction, thus increasing the biotransformation of some drugs metabolized by CYP3A and CYP2B6. In vitro studies have shown that efavirenz inhibited CYP isozymes 2C9 and 2C19 with Ki values (8.5-17 μM) in the range of observed efavirenz plasma concentrations. In in vitro studies, efavirenz did not inhibit CYP2E1 and inhibited CYP2D6 and CYP1A2 (Ki values 82-160 μM) only at concentrations well above those achieved clinically. Coadministration of efavirenz with drugs primarily metabolized by CYP2C9, CYP2C19, CYP3A, or CYP2B6 isozymes may result in altered plasma concentrations of the coadministered drug. Drugs which induce CYP3A and CYP2B6 activity would be expected to increase the clearance of efavirenz resulting in lowered plasma concentrations.
Drug interaction studies were performed with efavirenz and other drugs likely to be coadministered or drugs commonly used as probes for pharmacokinetic interaction. The effects of coadministration of efavirenz on the Cmax, AUC, and Cmin are summarized in Table 7 (effect of efavirenz on other drugs) and Table 8 (effect of other drugs on efavirenz). For information regarding clinical recommendations [see Drug Interactions (7.1 )].
| Coadministered Drug | Dose | EfavirenzDose | Number of Subjects | Coadministered Drug (mean %change) | ||
| C max (90% CI) | AUC (90% CI) | C min (90% CI) | ||||
| Atazanavir | 400 mg qd with a light meal d 1 - 20 | 600 mg qd with a light meal d 7 - 20 | 27 | ↓59% (49 - 67%) | ↓74% (68 - 78%) | ↓93% (90 - 95%) |
| 400 mg qd d 1- 6, then 300 mg qd d 7 - 20 with ritonavir 100 mg qd and a light meal | 600 mg qd 2h after atazanavir and ritonavir d 7 - 20 | 13 | ↑14% a (↓17-↑58%) | ↑39% a (2 - 88%) | ↑48% a (24 - 76%) | |
| 300 mg qd/ritonavir 100 mg qd d 1 - 10 (pm), then 400 mg qd/ritonavir 100 mg qd d 11 - 24 (pm) (simultaneous with efavirenz) | 600 mg qd with a light snack d 11 – 24 (pm) | 14 | ↑17% (8 - 27%) | ↔ | ↓42% (31 - 51%) | |
| Indinavir | 1000 mg q8h x 10 days | 600 mg qd x 10 days | 20 | |||
| After morning dose | ↔ b | ↓33% b (26 - 39%) | ↓39% b (24 - 51%) | |||
| After afternoon dose | ↔ b | ↓37% b (26 - 46%) | ↓52% b (47 - 57%) | |||
| After evening dose | ↓29% b (11 - 43%) | ↓ 46% b (37 - 54%) | ↓57% b (50 - 63%) | |||
| Lopinavir/ ritonavir | 400/100 mg capsule q12h x 9 days | 600 mg qd x 9 days | 11, 7 c | ↔ d | ↓19% d (↓ 36 -↑ 3%) | ↓ 39% d (3 - 62%) |
| 600/150 mg tablet q12h x 10 days with efavirenz compared to 400/100 mg q12h alone | 600 mg qd x9 days | 23 | ↑ 36% d (28 - 44%) | ↑ 36% d (28 - 44%) | ↑ 32% d (21 - 44%) | |
| Nelfinavir Metabolite AG-1402 | 750 mg q8h x 7 days | 600 mg qd x 7 days | 10 | ↑21% (10-33%) ↓40% (30-48%) | ↑20% (8 - 34%) ↓37% (25- 48%) | ↔ ↓ 43% (21 - 59%) |
| Ritonavir | 500 mg q12h x 8 days | 600 mg qd x 10 days | 11 | |||
| After AM dose | ↑24% (12 - 38%) | ↑18% (6 - 33%) | ↑42% (9 - 86%) e | |||
| After PM dose | ↔ | ↔ | ↑24% (3 - 50%) e | |||
| Saquinavir SGC f | 1200 mg q8h x 10 days | 600 mg qd x 10 days | 12 | ↓ 50% (28-66%) | ↓ 62% (45 - 74%) | ↓ 56% (16 - 77%) e |
| Lamivudine | 150 mg q12h x 14 days | 600 mg qd x 14 days | 9 | ↔ | ↔ | ↑265% (37 - 873%) |
| Tenofovir g | 300 mg qd | 600 mg qd x 14 days | 29 | ↔ | ↔ | ↔ |
| Zidovudine | 300 mg q12h x 14 days | 600 mg qd x 14 days | 9 | ↔ | ↔ | ↑225% (43 - 640%) |
| Maraviroc | 100 mg bid | 600 mg qd | 12 | ↓51% (37 - 62%) | ↓45% (38 - 51%) | ↓45% (28 - 57%) |
| Raltegravir | 400 mg single dose | 600 mg qd | 9 | ↓36% (2 - 59%) | ↓36% (20 - 48%) | ↓21% (↓51 -↑28%) |
| Boceprevir | 800 mg tid x 6 days | 600 mg qd x 6 days | NA | ↓ 8% (↓ 22 -↑ 8%) | ↓ 19% (11 - 25%) | ↓ 44% (26 - 58%) |
| Simeprevir | 150 mg qd x 14 days | 600 mg qd x 14 days | 23 | ↓51% (↓46-↓56%) | ↓71% (↓67- ↓74%) | ↓91% (↓88- ↓92%) |
| Azithromycin | 600 mg s ingle dose | 400 mg qd x 7 days | 14 | ↑22% (4 - 42%) | ↔ | NA |
| Clarithromycin 14-OH metabolite | 500 mg q12h x 7 days | 400 mg qd x 7 days | 11 | ↓26% (15-35%) ↑49% (32 - 69%) | ↓ 39% (30- 46%) ↑34% (18 - 53%) | ↓53% (42 - 63%) ↑26% (9 - 45%) |
| Fluconazole | 200 mg x 7 days | 400 mg qd x 7 days | 10 | ↔ | ↔ | ↔ |
| Itraconazole Hydroxy- itraconazole | 200 mg q 12 h x 28 days | 600 mg qd x 14 days | 18 | ↓37% (20 – 51%) ↓35 (12 - 52%) | ↓ 39% (21 – 53%) ↓ 37 (14 - 55%) | ↓ 44% (27 – 58%) ↓43 (18 - 60%) |
| Posaconazole | 400 mg (oral suspension) bid × 10 and 20 days | 400 mg qd × 10 and 20 Days | 11 | ↓45% (34 - 53%) | ↓50% (40 - 57%) | NA |
| Rifabutin | 300 mg,qd x 14 days | 600 mg qd x 14 days | 9 | ↓ 32% (15 - 46%) | ↓38% (28 - 47%) | ↓45% (31 - 56%) |
| Voriconazole | 400 mg po q12h x 1 day then 200 mg po q12h x 8 days | 400 mg qd x 9 days | NA | ↓ 61% h | ↓77% h | NA |
| 300 mg po q 12 h days 2 - 7 | 300 mg qd x 7 days | NA | ↓36% i (21 - 49%) | ↓ 55% i (45 - 62%) | NA | |
| 400 mg po q12h days 2 - 7 | 300 mg qd x 7 days | NA | ↑23% i (↓ 1 -↑53%) | ↓ 7% i (↓ 23 - ↑13%) | NA | |
| Artemether/ lumefantrine | Artemether 20 mg/ lumefantrine 120 mg tablets (6 4-tablet doses over 3 days) | 600 mg qd × 26 days | 12 | |||
| Artemether | 21% | 51% | ||||
| Dihydroartemisinin | 38% | 46% | NA | |||
| lumefantrine | 21% | NA | ||||
| Atorvastatin Total active (including metabolites) | 10 mg qd x 4 days | 600 mg qd x 15 days | 14 | ↓ 14% (1 - 26%) ↓15% (2 - 26%) | ↓ 43% (34 - 50%) ↓32% (21-41%) | ↓ 69% (49 - 81%) ↓ 48% (23 - 64%) |
| Pravastatin | 40 mg qd x 4 days | 600 mg qd x 15 days | 13 | ↓ 32% (↓59-↑12%) | ↓ 44% (26- 57%) | ↓ 19% (0 - 35%) |
| Simvastatin Total active (including metabolites) | 40 mg qd x 4 days | 600 mg qd x 15 days | 14 | ↓ 72% (63 - 79%) ↓ 68% (55 - 78%) | ↓68% (62 - 73%) ↓ 60% (52 - 68%) | ↓45% (20 - 62%) NA j |
| Carbamazepine Epoxide metabolite | 200 mg qd x 3 days, 200 mg bid x 3 days, then 400 mg qd x 29 days | 600 mg qd x 14 days | 12 | ↓20% (15 - 24%) ↔ | ↓ 27% (20 - 33%) ↔ | ↓ 35% (24 - 44%) ↓ 13% (↓ 30 - ↑7%) |
| Cetirizine | 10 mg single dose | 600 mg qd x 10 days | 11 | ↓24% (18 - 30%) | ↔ | NA |
| Diltiazem Desacetyl diltiazem N-monodesmethyl diltiazem | 240 mg x 21 days | 600 mg qd x 14 days | 13 | ↓ 60% (50 - 68%) ↓ 64% (57 - 69%) ↓ 28% (7 - 44%) | ↓69% (55 - 79%) ↓ 75% (59 - 84%) ↓ 37% (17 - 52%) | ↓ 63% (44 - 75%) ↓ 62% (44 - 75%) ↓ 37% (17 - 52%) |
| Ethinyl estradiol/Norgestimate | 0.035 mg/0.25 mg x 14 days | 600 mg qd x 14 days | ||||
| Ethinyl estradiol | 21 | ↔ | ↔ | ↔ | ||
| Norelgestromin | 21 | ↓ 46% (39 - 52%) | ↓64% (62 - 67%) | ↓82% (79 - 85%) | ||
| Levonorgestrel | 6 | ↓80% (77 - 83%) | ↓83% (79 - 87%) | ↓86% (80 - 90%) | ||
| Lorazepam | 2 mg single dose | 600 mg qd x 10 days | 12 | ↑16% (2 - 32%) | ↔ | NA |
| Methadone | Stable maintenance 35 - 100 mg daily | 600 mg qd x 14 - 21 days | 11 | ↓45% (25 - 59%) | ↓52% (33 - 66%) | NA |
| Bupropion Hydroxy- bupropion | 150 mg single dose (sustained-release) | 600 mg qd x 14 days | 13 | ↓ 34% (21 - 47%) ↑50% (20 - 80%) | ↓ 55% (48 - 62%) ↔ | NA NA |
| Paroxetine | 20 mg qd x 14 days | 600 mg qd x 14 days | 16 | ↔ | ↔ | ↔ |
| Sertraline | 50 mg qd x 14 days | 600 mg qd x 14 days | 13 | ↓ 29% (15 - 40%) | ↓39% (27 - 50%) | ↓46% (31 - 58%) |
| ↑ Indicates increase ↓ Indicates decrease " Indicates no change or a mean increase or decrease of < 10%. a Compared with atazanavir 400 mg qd alone. b Comparator dose of indinavir was 800 mg q8h × 10 days. c Parallel-group design; n for efavirenz + lopinavir/ritonavir, n for lopinavir/ritonavir alone. d Values are for lopinavir; the pharmacokinetics of ritonavir in this study were unaffected by concurrent efavirenz. e 95% CI. f Soft Gelatin Capsule. g Tenofovir disoproxil fumarate. h 90% CI not available. i Relative to steady-state administration of voriconazole (400 mg for 1 day, then 200 mg po q12h for 2 days). j Not available because of insufficient data. NA = not available. | ||||||
| Coadministered Drug | Dose | Efavirenz Dose | Number of Subjects | Efavirenz (mean % change) | ||
| C max (90% CI) | AUC (90% CI) | C min (90% CI) | ||||
| Indinavir | 800 mg q8h x 14 days | 200 mg qd x 14 days | 11 | ↔ | ↔ | ↔ |
| Lopinavir/ritonavir | 400/100 mg q12h x 9 days | 600 mg qd x 9 days | 11, 12 a | ↔ | ↓16% (↓38-↑15%) | ↓16% (↓ 42-↑20%) |
| Nelfinavir | 750 mg q8hx 7 days | 600 mg qd x 7 days | 10 | ↓12% (↓32-↑13%) b | ↓12% (↓35-↑18%) b | ↓21% (↓53 -↑33%) |
| Ritonavir | 500 mg q 12h x 8 days | 600 mg qd x 10 days | 9 | ↑ 14% (4 - 26%) | ↑ 21% (10 - 34%) | ↑25% (7 - 46%) b |
| Saquinavir SGC c | 1200 mg q8hx 10 days | 600 mg qd x 10 days | 13 | ↓13% (5 - 20%) | ↓12% (4 - 19%) | ↓14% (2 - 24%) b |
| Tenofovir d | 300 mg qd | 600 mg qd x 14 days | 30 | ↔ | ↔ | ↔ |
| Boceprevir | 800 mg tid x 6 days | 600 mg qd x 16 days | NA | ↑11% (2 - 20%) | ↑20% (15 - 26%) | NA |
| Simeprevir | 150 mg qd × 14 days | 600 mg qd × 14 days | 23 | ↔ | ↓ 10% (5-15%) | ↓ 13% (7-19%) |
| Azithromycin | 600 mg single dose | 400 mg qd x 7 days | 14 | ↔ | ↔ | ↔ |
| Clarithromycin | 500 mg q12h x 7 days | 400 mg qd x 7 days | 12 | ↑11% (3-19%) | ↔ | ↔ |
| Fluconazole | 200 mg x 7 days | 400 mg qd x 7 days | 10 | ↔ | ↑16% (6-26%) | ↑22% (5-41%) |
| Itraconazole | 200 mg q12h x 14 days | 600 mg qd x 28 days | 16 | ↔ | ↔ | ↔ |
| Rifabutin | 300 mg qd x 14 days | 600 mg qd x 14 days | 11 | ↔ | ↔ | ↓ 12% (↓24 - ↑1%) |
| Rifampin | 600 mg x 7 days | 600 mg qd x 7 days | 12 | ↓20% (11 - 28%) | ↓26% (15 - 36%) | ↓32% (15 - 46%) |
| Voriconazole | 400 mg po q12h x 1 day then 200 mg po q12h x 8 days | 400 mg qd x 9 days | NA | ↑38% e | ↑44% e | NA |
| 300 mg Po q12h days 2 - 7 | 300 mg qd x 7 days | NA | ↓14% f (7 - 21%) | ↔ f | NA | |
| 400 mg Po q12h days 2-7 | 300 mg qd x7 days | NA | ↔ f | ↑17% f (6 - 29%) | NA | |
| Artemether/Lumefantrine | Artemether 20 mg/ lumefantrine 120 mg tablets (6 4-tablet doses over 3 days) | 600 mg qd × 26 days | 12 | ↔ | ↓ 17% | NA |
| Atorvastatin | 10 mg qd x 4 days | 600 mg qd x 15 days | 14 | ↔ | ↔ | ↔ |
| Pravastatin | 40 mg qd x 4 days | 600 mg qd x 15 days | 11 | ↔ | ↔ | ↔ |
| Simvastatin | 40 mg qd x 4 days | 600 mg qd x 15 days | 14 | ↓12% (↓28 -↑8%) | ↔ | ↓12% (↓ 25-↑3%) |
| Aluminum hydroxide 400 mg, Magnesium hydroxide 400 mg, plus simethicone 40 mg | 30 mL single dose | 400 mg single dose | 17 | ↔ | ↔ | NA |
| Carbamazepine | 200 mg qd x 3 days, 200 mg bid x 3 days, then 400 mg qd x 15 days | 600 mg qd x 35 days | 14 | ↓21% (15 - 26%) | ↓36% (32 - 40%) | ↓47% (41 - 53%) |
| Cetirizine | 10 mg single dose | 600 mg qd x 10 days | 11 | ↔ | ↔ | ↔ |
| Diltiazem | 240 mg x 14 days | 600 mg qd x 28 days | 12 | ↑16% (6 - 26%) | ↑11% (5 - 18%) | ↑13% (1 - 26%) |
| Famotidine | 40 mg single dose | 400 mg single dose | 17 | ↔ | ↔ | NA |
| Paroxetine | 20 mg qd x 14 days | 600 mg qd x 14 days | 12 | ↔ | ↔ | ↔ |
| Sertraline | 50 mg qd x 14 days | 600 mg qd x 14 days | 13 | ↑11% (6 - 16%) | ↔ | ↔ |
| ↑Indicates increase ↓Indicates decrease ↔Indicates no change or a mean increase or decrease of <10%. a Parallel-group design; n for efavirenz + lopinavir/ritonavir, n for efavirenz alone. b 95% CI. c Soft Gelatin Capsule. d Tenofovir disoproxil fumarate. e 90% CI not available. f Relative to steady-state administration of efavirenz (600 mg once daily for 9 days). NA = not available. | ||||||
Microbiology
Mechanism of Action
Efavirenz is an NNRTI of HIV-1. Efavirenz activity is mediated predominantly by noncompetitive inhibition of HIV-1 reverse transcriptase. HIV-2 reverse transcriptase and human cellular DNA polymerases α, β, γ, and δ are not inhibited by efavirenz
Antiviral Activity in Cell Culture
The concentration of efavirenz inhibiting replication of wild-type laboratory adapted strains and clinical isolates in cell culture by 90-95% (EC 90-95 ) ranged from 1.7 to 25 nM in lymphoblastoid cell lines, peripheral blood mononuclear cells (PBMCs), and macrophage/monocyte cultures. Efavirenz demonstrated antiviral activity against clade B and most non-clade B isolates (subtypes A, AE, AG, C, D, F, G, J, N), but had reduced antiviral activity against group O viruses. Efavirenz demonstrated additive antiviral activity without cytotoxicity against HIV-1 in cell culture when combined with the NNRTIs delavirdine and nevirapine, NRTIs (abacavir, didanosine, emtricitabine, lamivudine, stavudine, tenofovir, zalcitabine, zidovudine), PIs (amprenavir, indinavir, lopinavir, nelfinavir, ritonavir, saquinavir), and the fusion inhibitor enfuvirtide. Efavirenz demonstrated additive to antagonistic antiviral activity in cell culture with atazanavir. Efavirenz was not antagonistic with adefovir, used for the treatment of hepatitis B virus infection, or ribavirin, used in combination with interferon for the treatment of hepatitis C virus infection.
Resistance
In cell culture
In cell culture, HIV-1 isolates with reduced susceptibility to efavirenz (>380-fold increase in EC 90 value) emerged rapidly in the presence of drug. Genotypic characterization of these viruses identified single amino acid substitutions L100I or V179D, double substitutions L100I/V108I, and triple substitutions L100I/V179D/Y181C in reverse transcriptase.
Clinical studies
Clinical isolates with reduced susceptibility in cell culture to efavirenz have been obtained. One or more substitutions at amino acid positions 98, 100, 101, 103, 106, 108, 188, 190, 225, and 227 in reverse transcriptase were observed in patients failing treatment with efavirenz in combination with indinavir, or with zidovudine plus lamivudine. The K103N substitution was the most frequently observed. Long-term resistance surveillance (average 52 weeks, range 4-106 weeks) analyzed 28 matching baseline and virologic failure isolates. Sixty-one percent (17/28) of these failure isolates had decreased efavirenz susceptibility in cell culture with a median 88-fold change in efavirenz susceptibility (EC 50 value) from reference. The most frequent NNRTI substitution to develop in these patient isolates was K103N (54%). Other NNRTI substitutions that developed included L100I (7%), K101E/Q/R (14%), V108I (11%), G190S/T/A (7%), P225H (18%), and M230I/L (11%).
Cross-Resistance
Cross-resistance among NNRTIs has been observed. Clinical isolates previously characterized as efavirenz-resistant were also phenotypically resistant in cell culture to delavirdine and nevirapine compared to baseline. Delavirdine- and/or nevirapine-resistant clinical viral isolates with NNRTI resistance-associated substitutions (A98G, L100I, K101E/P, K103N/S, V106A, Y181X, Y188X, G190X, P225H, F227L, or M230L) showed reduced susceptibility to efavirenz in cell culture. Greater than 90% of NRTI-resistant clinical isolates tested in cell culture retained susceptibility to efavirenz.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Long-term carcinogenicity studies in mice and rats were carried out with efavirenz. Mice were dosed with 0, 25, 75, 150, or 300 mg/kg/day for 2 years. Incidences of hepatocellular adenomas and carcinomas and pulmonary alveolar/bronchiolar adenomas were increased above background in females. No increases in tumor incidence above background were seen in males. There was no NOAEL in females established for this study because tumor findings occurred at all doses. AUC at the NOAEL (150 mg/kg) in the males was approximately 0.9 times that in humans at the recommended clinical dose. In the rat study, no increases in tumor incidence were observed at doses up to 100 mg/kg/day, for which AUCs were 0.1 (males) or 0.2 (females) times those in humans at the recommended clinical dose.
Mutagenesis
Efavirenz tested negative in a battery of in vitro and in vivo genotoxicity assays. These included bacterial mutation assays in S. typhimurium and E. coli , mammalian mutation assays in Chinese hamster ovary cells, chromosome aberration assays in human peripheral blood lymphocytes or Chinese hamster ovary cells, and an in vivo mouse bone marrow micronucleus assay.
Impairment of Fertility
Efavirenz did not impair mating or fertility of male or female rats, and did not affect sperm of treated male rats. The reproductive performance of offspring born to female rats given efavirenz was not affected. The AUCs at the NOAEL values in male (200 mg/kg) and female (100 mg/kg) rats were approximately ≤0.15 times that in humans at the recommended clinical dose.
Animal Toxicology
Nonsustained convulsions were observed in 6 of 20 monkeys receiving efavirenz at doses yielding plasma AUC values 4- to 13-fold greater than those in humans given the recommended dose [see Warnings and Precautions (5.10 )].
CLINICAL STUDIES
Adults
Study 006 , a randomized, open-label trial, compared efavirenz (600 mg once daily) + zidovudine (ZDV, 300 mg q12h) + lamivudine (LAM, 150 mg q12h) or efavirenz (600 mg once daily) + indinavir (IDV, 1000 mg q8h) with indinavir (800 mg q8h) + zidovudine (300 mg q12h) + lamivudine (150 mg q12h). Twelve hundred sixty-six patients (mean age 36.5 years [range 18-81], 60% Caucasian, 83% male) were enrolled. All patients were efavirenz-, lamivudine-, NNRTI-, and PI-naive at study entry. The median baseline CD4+ cell count was 320 cells/mm 3 and the median baseline HIV-1 RNA level was 4.8 log 10 copies/mL. Treatment outcomes with standard assay (assay limit 400 copies/mL) through 48 and 168 weeks are shown in Table 9 . Plasma HIV RNA levels were quantified with standard (assay limit 400 copies/mL) and ultrasensitive (assay limit 50 copies/mL) versions of the AMPLICOR HIV-1 MONITOR assay. During the study, version 1.5 of the assay was introduced in Europe to enhance detection of non-clade B virus.
a Patients achieved and maintained confirmed HIV-1 RNA <400 copies/mL through Week 48 or Week 168. | ||||||
b Includes patients who rebounded, patients who were on study at Week 48 and failed to achieve confirmed HIV-1 RNA <400 copies/mL at time of discontinuation, and patients who discontinued due to lack of efficacy. | ||||||
c Includes consent withdrawn, lost to follow-up, noncompliance, never treated, missing data, protocol violation, death, and other reasons. Patients with HIV-1 RNA levels <400 copies/mL who chose not to continue in the voluntary extension phases of the study were censored at date of last dose of study medication. | ||||||
| Efavirenz + ZDV + LAM (n=422) | Efavirenz + IDV (n=429) | IDV + ZDV + LAM (n=415) | ||||
| Outcome | Week 48 | Week 168 | Week 48 | Week 168 | Week 48 | Week 168 |
| Responder a | 69% | 48% | 57% | 40% | 50% | 29% |
| Virologic failure b | 6% | 12% | 15% | 20% | 13% | 19% |
| Discontinued for adverse events | 7% | 8% | 6% | 8% | 16% | 20% |
| Discontinued for other reasons c | 17% | 31% | 22% | 32% | 21% | 32% |
| CD4+ cell count (cells/mm 3 ) | ||||||
| Observed subjects (n) | (279) | (205) | (256) | (158) | (228) | (129) |
| Mean change from baseline | 190 | 329 | 191 | 319 | 180 | 329 |
For patients treated with efavirenz + zidovudine + lamivudine, efavirenz + indinavir, or indinavir + zidovudine + lamivudine, the percentage of responders with HIV-1 RNA <50 copies/mL was 65%, 50%, and 45%, respectively, through 48 weeks, and 43%, 31%, and 23%, respectively, through 168 weeks. A Kaplan-Meier analysis of time to loss of virologic response (HIV RNA <400 copies/mL) suggests that both the trends of virologic response and differences in response continue through 4 years.
ACTG 364 is a randomized, double-blind, placebo-controlled, 48-week study in NRTI-experienced patients who had completed two prior ACTG studies. One-hundred ninety-six patients (mean age 41 years [range 18-76], 74% Caucasian, 88% male) received NRTIs in combination with efavirenz (600 mg once daily), or nelfinavir (NFV, 750 mg three times daily), or efavirenz (600 mg once daily) + nelfinavir in a randomized, double-blinded manner. The mean baseline CD4+ cell count was 389 cells/mm 3 and mean baseline HIV-1 RNA level was 8130 copies/mL. Upon entry into the study, all patients were assigned a new open-label NRTI regimen, which was dependent on their previous NRTI treatment experience. There was no significant difference in the mean CD4+ cell count among treatment groups; the overall mean increase was approximately 100 cells at 48 weeks among patients who continued on study regimens. Treatment outcomes are shown in Table 10 Plasma HIV RNA levels were quantified with the AMPLICOR HIV-1 MONITOR assay using a lower limit of quantification of 500 copies/mL.
• For some patients, Week 56 data were used to confirm the status at Week 48. | |||
a Subjects achieved virologic response (two consecutive viral loads <500 copies/mL) and maintained it through Week 48. | |||
b Includes viral rebound and failure to achieve confirmed <500 copies/mL by Week 48. | |||
c See Adverse Reactions (6.1 ) for a safety profile of these regimens. | |||
d Includes loss to follow-up, consent withdrawn, noncompliance. | |||
| Outcome | EFAVIRENZ + NFV + NRTIs (n=65) | EFAVIRENZ + NRTIs (n=65) | NFV + NRTIs (n=66) |
| HIV-1 RNA <500 copies/mL a | 71% | 63% | 41% |
| HIV-1 RNA ≥500 copies/mL b | 17% | 34% | 54% |
| CDC Category C Event | 2% | 0% | 0% |
| Discontinuations for adverse events c | 3% | 3% | 5% |
| Discontinuations for other reasons d | 8% | 0% | 0% |
A Kaplan-Meier analysis of time to treatment failure through 72 weeks demonstrates a longer duration of virologic suppression (HIV RNA <500 copies/mL) in the efavirenz-containing treatment arms.
Pediatric Patients
Study AI266922 is an open-label study to evaluate the pharmacokinetics, safety, tolerability, and antiviral activity of efavirenz in combination with didanosine and emtricitabine in antiretroviral- naive and -experienced pediatric patients. Thirty-seven patients 3 months to 6 years of age (median 0.7 years) were treated with efavirenz. At baseline, median plasma HIV-1 RNA was 5.88 log 10 copies/mL, median CD4+ cell count was 1144 cells/mm 3 , and median CD4+ percentage was 25%. The median time on study therapy was 60 weeks; 27% of patients discontinued before Week 48. Using an ITT analysis, the overall proportions of patients with HIV RNA <400 copies/mL and <50 copies/mL at Week 48 were 57% (21/37) and 46% (17/37), respectively. The median increase from baseline in CD4+ count at 48 weeks was 196 cells/mm 3 and the median increase in CD4+ percentage was 6%.
Study PACTG 1021 was an open-label study to evaluate the pharmacokinetics, safety, tolerability, and antiviral activity of efavirenz in combination with didanosine and emtricitabine in pediatric patients who were antiretroviral therapy naive. Forty-three patients 3 months to 21 years of age (median 9.6 years) were dosed with efavirenz. At baseline, median plasma HIV-1 RNA was 4.8 log 10 copies/mL, median CD4+ cell count was 367 cells/mm 3 , and median CD4+ percentage was 18%. The median time on study therapy was 181 weeks; 16% of patients discontinued before Week 48. Using an ITT analysis, the overall proportions of patients with HIV RNA <400 copies/mL and <50 copies/mL at Week 48 were 77% (33/43) and 70% (30/43), respectively. The median increase from baseline in CD4+ count at 48 weeks of therapy was 238 cells/mm 3 and the median increase in CD4+ percentage was 13%.
Study PACTG 382 was an open-label study to evaluate the pharmacokinetics, safety, tolerability, and antiviral activity of efavirenz in combination with nelfinavir and an NRTI in antiretroviral- naive and NRTI-experienced pediatric patients. One hundred two patients 3 months to 16 years of age (median 5.7 years) were treated with efavirenz. Eighty-seven percent of patients had received prior antiretroviral therapy. At baseline, median plasma HIV-1 RNA was 4.57 log 10 copies/mL, median CD4+ cell count was 755 cells/mm 3 , and median CD4+ percentage was 30%. The median time on study therapy was 118 weeks; 25% of patients discontinued before Week 48. Using an ITT analysis, the overall proportion of patients with HIV RNA <400 copies/mL and <50 copies/mL at Week 48 were 57% (58/102) and 43% (44/102), respectively. The median increase from baseline in CD4+ count at 48 weeks of therapy was 128 cells/mm3 and the median increase in CD4+ percentage was 5%.
HOW SUPPLIED/STORAGE AND HANDLING
Tablets
Efavirenz tablets, USP are available as follows:
600-mg tablets are yellow coloured, capsule-shaped, biconvex, film coated tablets debossed with '301' on one side and 'CL' on other side.
Bottle of 30 tablets NDC 69097-301-02
Storage
Efavirenz tablets, USP should be stored at 25°C (77°F); excursions permitted between 15°C to 30°C (59°F to 86°F) [see USP Controlled Room Temperature].
Mechanism of Action
Efavirenz is an antiviral drug [see Microbiology (12.4 ) ] .