Get your patient on Droperidol - Droperidol injection, Solution (Droperidol)
Droperidol - Droperidol injection, Solution prescribing information
WARNING
Cases of QT prolongation and/or torsade de pointes have been reported in patients receiving droperidol at doses at or below recommended doses. Some cases have occurred in patients with no known risk factors for QT prolongation and some cases have been fatal.
Due to its potential for serious proarrhythmic effects and death, droperidol should be reserved for use in the treatment of patients who fail to show an acceptable response to other adequate treatments, either because of insufficient effectiveness or the inability to achieve an effective dose due to intolerable adverse effects from those drugs (see CONTRAINDICATIONS , WARNINGS , PRECAUTIONS , and ADVERSE REACTIONS ).
Cases of QT prolongation and serious arrhythmias (e.g., torsade de pointes) have been reported in patients treated with droperidol. Based on these reports, all patients should undergo a 12-lead ECG prior to administration of droperidol to determine if a prolonged QT interval (i.e., QTc greater than 440 msec for males or 450 msec for females) is present. If there is a prolonged QT interval, droperidol should NOT be administered. For patients in whom the potential benefit of droperidol treatment is felt to outweigh the risks of potentially serious arrhythmias, ECG monitoring should be performed prior to treatment and continued for 2-3 hours after completing treatment to monitor for arrhythmias.
Droperidol is contraindicated in patients with known or suspected QT prolongation, including patients with congenital long QT syndrome.
Droperidol should be administered with extreme caution to patients who may be at risk for development of prolonged QT syndrome (e.g., congestive heart failure, bradycardia, use of a diuretic, cardiac hypertrophy, hypokalemia, hypomagnesemia, or administration of other drugs known to increase the QT interval). Other risk factors may include age over 65 years, alcohol abuse, and use of agents such as benzodiazepines, volatile anesthetics, and IV opiates. Droperidol should be initiated at a low dose and adjusted upward, with caution, as needed to achieve the desired effect.
INDICATIONS AND USAGE
Droperidol Injection is indicated to reduce the incidence of nausea and vomiting associated with surgical and diagnostic procedures.
DOSAGE AND ADMINISTRATION
Dosage should be individualized . Some of the factors to be considered in determining the dose are age, body weight, physical status, underlying pathological condition, use of other drugs, type of anesthesia to be used, and the surgical procedure involved.
Vital signs and ECG should be monitored routinely.
Adult Dosage: The maximum recommended initial dose of droperidol is 2.5 mg IM or slow IV. Additional 1.25 mg doses of droperidol may be administered to achieve the desired effect. However, additional doses should be administered with caution, and only if the potential benefit outweighs the potential risk.
Children’s Dosage: For children two to 12 years of age, the maximum recommended initial dose is 0.1 mg/kg, taking into account the patient's age and other clinical factors. However, additional doses should be administered with caution, and only if the potential benefit outweighs the potential risk.
See WARNINGS and PRECAUTIONS for use of droperidol with other CNS depressants, and in patients with altered response.
Parenteral drug products should be inspected visually for particulate matter and discoloration prior to administration, whenever solution and container permit. If such abnormalities are observed, the drug should not be administered.
CONTRAINDICATIONS
Droperidol is contraindicated in patients with known or suspected QT prolongation (i.e., QTc interval greater than 440 msec for males or 450 msec for females). This would include patients with congenital long QT syndrome.
Droperidol is contraindicated in patients with known hypersensitivity to the drug.
Droperidol is not recommended for any use other than for the treatment of perioperative nausea and vomiting in patients for whom other treatments are ineffective or inappropriate (see WARNINGS ).
ADVERSE REACTIONS
QT interval prolongation, torsade de pointes, cardiac arrest, and ventricular tachycardia have been reported in patients treated with droperidol. Some of these cases were associated with death. Some cases occurred in patients with no known risk factors, and some were associated with droperidol doses at or below recommended doses.
Physicians should be alert to palpitations, syncope, or other symptoms suggestive of episodes of irregular cardiac rhythm in patients taking droperidol and promptly evaluate such cases (see WARNINGS, Effects on Cardiac Conduction ).
The most common somatic adverse reactions reported to occur with droperidol are mild to moderate hypotension and tachycardia, but these effects usually subside without treatment. If hypotension occurs and is severe or persists, the possibility of hypovolemia should be considered and managed with appropriate parenteral fluid therapy.
The most common behavioral adverse effects of droperidol include dysphoria, postoperative drowsiness, restlessness, hyperactivity and anxiety, which can either be the result of an inadequate dosage (lack of adequate treatment effect) or of an adverse drug reaction (part of the symptom complex of akathisia).
Care should be taken to search for extrapyramidal signs and symptoms (dystonia, akathisia, oculogyric crisis) to differentiate these different clinical conditions. When extrapyramidal symptoms are the cause, they can usually be controlled with anticholinergic agents.
Postoperative hallucinatory episodes (sometimes associated with transient periods of mental depression) have also been reported.
Other less common reported adverse reactions include anaphylaxis, dizziness, chills and/or shivering, laryngospasm and bronchospasm.
Elevated blood pressure, with or without pre-existing hypertension, has been reported following administration of droperidol combined with fentanyl citrate or other parenteral analgesics. This might be due to unexplained alterations in sympathetic activity following large doses; however, it is also frequently attributed to anesthetic or surgical stimulation during light anesthesia.
Drug Interactions
Potentially Arrhythmogenic Agents:
Any drug known to have the potential to prolong the QT interval should not be used together with droperidol. Possible pharmacodynamic interactions can occur between droperidol and potentially arrhythmogenic agents such as class I or III antiarrhythmics, antihistamines that prolong the QT interval, antimalarials, calcium channel blockers, neuroleptics that prolong the QT interval, and antidepressants.
Caution should be used when patients are taking concomitant drugs known to induce hypokalemia or hypomagnesemia as they may precipitate QT prolongation and interact with droperidol. These would include diuretics, laxatives and supraphysiological use of steroid hormones with mineralocorticoid potential.
CNS Depressant Drugs:
Other CNS depressant drugs (e.g. barbiturates, tranquilizers, opioids and general anesthetics) have additive or potentiating effects with droperidol. When patients have received such drugs, the dose of droperidol required will be less than usual. Following the administration of droperidol, the dose of other CNS depressant drugs should be reduced.
DESCRIPTION
Droperidol Injection, USP, is a sterile, non-pyrogenic, aqueous solution for intravenous or intramuscular use only.
Each mL contains:
Droperidol…………………………………….2.5 mg
Water for Injection………………………........q.s.
pH adjusted between 3.0 and 3.8 with lactic acid and, if necessary, with sodium hydroxide.
Droperidol is a neuroleptic (tranquilizer) agent. Chemically it is 1-(1-[3-(p-fluorobenzoyl)propyl]-1,2,3,6-tetrahydro-4-pyridyl)-2-benzimidazolinone and the structural formula is:
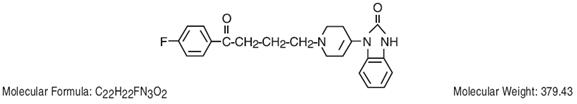
CLINICAL PHARMACOLOGY
Droperidol produces marked tranquilization and sedation. It allays apprehension and provides a state of mental detachment and indifference while maintaining a state of reflex alertness.
Droperidol produces an antiemetic effect as evidenced by the antagonism of apomorphine in dogs. It lowers the incidence of nausea and vomiting during surgical procedures and provides antiemetic protection in the postoperative period.
Droperidol potentiates other CNS depressants. It produces mild alpha-adrenergic blockade, peripheral vascular dilatation and reduction of the pressor effect of epinephrine. It can produce hypotension and decreased peripheral vascular resistance and may decrease pulmonary arterial pressure (particularly if it is abnormally high). It may reduce the incidence of epinephrine-induced arrhythmias but it does not prevent other cardiac arrhythmias.
The onset of action of single intramuscular and intravenous doses is from three to ten minutes following administration, although the peak effect may not be apparent for up to thirty minutes. The duration of the tranquilizing and sedative effects generally is two to four hours, although alteration of alertness may persist for as long as twelve hours.
HOW SUPPLIED
Droperidol Injection USP, (2.5 mg/mL) is available as:
| Product No. | Strength | Size | How Packaged |
| NDC 0517-9702-25 | 5 mg/2 mL | 2 mL Single Dose Vial | Boxes of 25 |
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) (See USP Controlled Room Temperature).
PROTECT FROM LIGHT. RETAIN IN CARTON UNTIL TIME OF USE.
Droperidol - Droperidol injection, Solution PubMed™ news
- Journal Article • 2026 MayShrinking pharmacological options in modern anaesthesia.
- Journal Article • 2026 MaySuccessful use of intravenous droperidol in hyperemesis following failure of sequential antiemetic therapy.
- Journal Article • 2026 MarNational survey of Dutch emergency physicians on pharmacological sedation practices for extreme agitation.
- Journal Article • 2026 MarPrehospital management of acute behavioural disturbance: managing severe agitation in the prehospital setting - a systematic literature review.
- Journal Article • 2026 FebFrom Limited Use to Standard Practice: Retrospective Analysis of Droperidol Administration by Emergency Medical Services (2018-2023).