Get your patient on Dexamethasone - Dexamethasone tablet (Dexamethasone)
Dexamethasone - Dexamethasone tablet prescribing information
INDICATIONS AND USAGE
Allergic States
Control of severe or incapacitating allergic conditions intractable to adequate trials of conventional treatment in asthma, atopic dermatitis, contact dermatitis, drug hypersensitivity reactions, seasonal or perennial allergic rhinitis and serum sickness.
Dermatologic Diseases
Bullous dermatitis herpetiformis, exfoliative erythroderma, mycosis fungoides, pemphigus, and severe erythema multiforme (Stevens-Johnson syndrome).
Endocrine Disorders
Primary or secondary adrenocortical insufficiency (hydrocortisone or cortisone is the drug of choice; may be used in conjunction with synthetic mineralocorticoid analogs where applicable; in infancy mineralocorticoid supplementation is of particular importance), congenital adrenal hyperplasia, hypercalcemia associated with cancer, and nonsuppurative thyroiditis.
Gastrointestinal Diseases
To tide the patient over a critical period of the disease in regional enteritis and ulcerative colitis.
Hematologic Disorders
Acquired (autoimmune) hemolytic anemia, congenital (erythroid) hypoplastic anemia (Diamond-Blackfan anemia), idiopathic thrombocytopenic purpura in adults, pure red cell aplasia, and selected cases of secondary thrombocytopenia.
Miscellaneous
Diagnostic testing of adrenocortical hyperfunction, trichinosis with neurologic or myocardial involvement, tuberculous meningitis with subarachnoid block or impending block when used with appropriate antituberculous chemotherapy.
Neoplastic Diseases
For palliative management of leukemias and lymphomas.
Nervous System
Acute exacerbations of multiple sclerosis, cerebral edema associated with primary or metastatic brain tumor, craniotomy, or head injury.
Ophthalmic Diseases
Sympathetic ophthalmia, temporal arteritis, uveitis, and ocular inflammatory conditions unresponsive to topical corticosteroids.
Renal Diseases
To induce a diuresis or remission of proteinuria in idiopathic nephrotic syndrome or that due to lupus erythematosus.
Respiratory Diseases
Berylliosis, fulminating or disseminated pulmonary tuberculosis when used concurrently with appropriate antituberculous chemotherapy, idiopathic eosinophilic pneumonias, symptomatic sarcoidosis.
Rheumatic Disorders
As adjunctive therapy for short-term administration (to tide the patient over an acute episode or exacerbation) in acute gouty arthritis, acute rheumatic carditis, ankylosing spondylitis, psoriatic arthritis, rheumatoid arthritis, including juvenile rheumatoid arthritis (selected cases may require low-dose maintenance therapy). For the treatment of dermatomyositis, polymyositis, and systemic lupus erythematosus.
DOSAGE AND ADMINISTRATION
For Oral Administration:
The initial dose varies from 0.75 to 9 mg a day depending on the disease being treated.
IT SHOULD BE EMPHASIZED THAT DOSAGE REQUIREMENTS ARE VARIABLE AND MUST BE INDIVIDUALIZED ON THE BASIS OF THE DISEASE UNDER TREATMENT AND THE RESPONSE OF THE PATIENT.
After a favorable response is noted, the proper maintenance dosage should be determined by decreasing the initial dosage in small decrements at appropriate time intervals until the lowest dosage that maintains an adequate clinical response is reached.
Situations which may make dosage adjustments necessary are changes in clinical status secondary to remissions or exacerbations in the disease process, the patient's individual drug responsiveness, and the effect of patient exposure to stressful situations not directly related to the disease entity under treatment. In this latter situation it may be necessary to increase the dosage of the corticosteroid for a period of time consistent with the patient's condition. If after long-term therapy the drug is to be stopped, it is recommended that it be withdrawn gradually rather than abruptly.
In the treatment of acute exacerbations of multiple sclerosis, daily doses of 30 mg of dexamethasone for a week followed by 4 to 12 mg every other day for one month have been shown to be effective (see PRECAUTIONS: Neuro-Psychiatric).
In pediatric patients, the initial dose of dexamethasone may vary depending on the specific disease entity being treated. The range of initial doses is 0.02 to 0.3 mg/kg/day in three or four divided doses (0.6 to 9 mg/m 2 bsa/day).
For the purpose of comparison, the following is the equivalent milligram dosage of the various corticosteroids:
| Cortisone, 25 Hydrocortisone, 20 Prednisolone, 5 Prednisone, 5 Methylprednisolone, 4 | Triamcinolone, 4 Paramethasone, 2 Betamethasone, 0.75 Dexamethasone, 0.75 |
These dose relationships apply only to oral or intravenous administration of these compounds. When these substances or their derivatives are injected intramuscularly or into joint spaces, their relative properties may be greatly altered.
In acute, self-limited allergic disorders or acute exacerbations of chronic allergic disorders, the following dosage schedule combining parenteral and oral therapy is suggested:
Dexamethasone Sodium Phosphate injection, 4 mg per mL:
First Day
- 1 or 2 mL, intramuscularly
Dexamethasone tablets, 0.75 mg:
Second Day
- 4 tablets in two divided doses
Third Day
- 4 tablets in two divided doses
Fourth Day
- 2 tablets in two divided doses
Fifth Day
- 1 tablet
Sixth Day
- 1 tablet
Seventh Day
- No treatment
Eighth Day
- Follow-up visit
This schedule is designed to ensure adequate therapy during acute episodes, while minimizing the risk of overdosage in chronic cases.
In cerebral edema , dexamethasone sodium phosphate injection is generally administered initially in a dosage of 10 mg intravenously followed by 4 mg every six hours intramuscularly until the symptoms of cerebral edema subside. Response is usually noted within 12 to 24 hours and dosage may be reduced after two to four days and gradually discontinued over a period of five to seven days. For palliative management of patients with recurrent or inoperable brain tumors, maintenance therapy with either dexamethasone sodium phosphate injection or dexamethasone tablets in a dosage of 2 mg two or three times daily may be effective.
Dexamethasone Suppression Tests
1. Tests for Cushing’s syndrome
Give 1.0 mg of dexamethasone orally at 11:00 p.m. Blood is drawn for plasma cortisol determination at 8:00 a.m. the following morning. For greater accuracy, give 0.5 mg of dexamethasone orally every 6 hours for 48 hours. Twenty-four hour urine collections are made for determination of 17-hydroxycorticosteroid excretion.
2. Test to distinguish Cushing’s syndrome due to pituitary ACTH excess from Cushing’s syndrome due to other causes.
Give 2.0 mg of dexamethasone orally every 6 hours for 48 hours. Twenty-four hour urine collections are made for determination of 17-hydroxycorticosteroid excretion.
CONTRAINDICATIONS
Systemic fungal infections (see WARNINGS : Fungal Infections). Dexamethasone tablets are contraindicated in patients who are hypersensitive to any components of this product.
ADVERSE REACTIONS
(listed alphabetically, under each subsection)
The following adverse reactions have been reported with dexamethasone or other corticosteroids:
Allergic Reactions:
Anaphylactoid reaction, anaphylaxis, angioedema.
Cardiovascular:
Bradycardia, cardiac arrest, cardiac arrhythmias, cardiac enlargement, circulatory collapse, congestive heart failure, fat embolism, hypertension, hypertrophic cardiomyopathy in premature infants, myocardial rupture following recent myocardial infarction (see WARNINGS : Cardio-renal), edema, pulmonary edema, syncope, tachycardia, thromboembolism, thrombophlebitis, vasculitis.
Dermatologic:
Acne, allergic dermatitis, dry scaly skin, ecchymoses and petechiae, erythema, impaired wound healing, increased sweating, rash, striae, suppression of reactions to skin tests, thin fragile skin, thinning scalp hair, urticaria.
Endocrine:
Decreased carbohydrate and glucose tolerance, development of cushingoid state, hyperglycemia, glycosuria, hirsutism, hypertrichosis, increased requirements for insulin or oral hypoglycemic agents in diabetes, manifestations of latent diabetes mellitus, menstrual irregularities, secondary adrenocortical and pituitary unresponsiveness (particularly in times of stress, as in trauma, surgery, or illness), suppression of growth in pediatric patients.
Fluid and Electrolyte Disturbances:
Congestive heart failure in susceptible patients, fluid retention, hypokalemic alkalosis, potassium loss, sodium retention, tumor lysis syndrome.
Gastrointestinal:
Abdominal distention, elevation in serum liver enzyme levels (usually reversible upon discontinuation), hepatomegaly, increased appetite, nausea, pancreatitis, peptic ulcer with possible perforation and hemorrhage, perforation of the small and large intestine (particularly in patients with inflammatory bowel disease), ulcerative esophagitis.
Metabolic:
Negative nitrogen balance due to protein catabolism.
Musculoskeletal:
Aseptic necrosis of femoral and humeral heads, loss of muscle mass, muscle weakness, osteoporosis, pathologic fracture of long bones, steroid myopathy, tendon rupture, vertebral compression fractures.
Neurological/Psychiatric:
Convulsions, depression, emotional instability, euphoria, headache, increased intracranial pressure with papilledema (pseudotumor cerebri) usually following discontinuation of treatment, insomnia, mood swings, neuritis, neuropathy, paresthesia, personality changes, psychic disorders, vertigo.
Ophthalmic:
Exophthalmos, glaucoma, increased intraocular pressure, posterior subcapsular cataracts, vision blurred.
Other:
Abnormal fat deposits, decreased resistance to infection, hiccups, increased or decreased motility and number of spermatozoa, malaise, moon face, weight gain.
To report SUSPECTED ADVERSE REACTIONS, contact Alvogen, Inc. at 1-866-770-3024 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch for voluntary reporting of adverse reactions.
Drug Interactions
Aminoglutethimide:
Aminoglutethimide may diminish adrenal suppression by corticosteroids.
Amphotericin B injection and potassium-depleting agents:
When corticosteroids are administered concomitantly with potassium-depleting agents (e.g., amphotericin B, diuretics), patients should be observed closely for development of hypokalemia. In addition, there have been cases reported in which concomitant use of amphotericin B and hydrocortisone was followed by cardiac enlargement and congestive heart failure.
Antibiotics:
Macrolide antibiotics have been reported to cause a significant decrease in corticosteroid clearance (see Drug Interactions: Hepatic Enzyme Inducers, Inhibitors and Substrates).
Anticholinesterases:
Concomitant use of anticholinesterase agents and corticosteroids may produce severe weakness in patients with myasthenia gravis. If possible, anticholinesterase agents should be withdrawn at least 24 hours before initiating corticosteroid therapy.
Anticoagulants, Oral
Co-administration of corticosteroids and warfarin usually results in inhibition of response to warfarin, although there have been some conflicting reports. Therefore, coagulation indices should be monitored frequently to maintain the desired anticoagulant effect.
Antidiabetics:
Because corticosteroids may increase blood glucose concentrations, dosage adjustments of antidiabetic agents may be required.
Antitubercular Drugs:
Serum concentrations of isoniazid may be decreased.
Cholestyramine:
Cholestyramine may increase the clearance of corticosteroids.
Cyclosporine:
Increased activity of both cyclosporine and corticosteroids may occur when the two are used concurrently. Convulsions have been reported with this concurrent use.
Dexamethasone Suppression Test (DST):
False-negative results in the dexamethasone suppression test (DST) in patients being treated with indomethacin have been reported. Thus, results of the DST should be interpreted with caution in these patients.
Digitalis Glycosides:
Patients on digitalis glycosides may be at increased risk of arrhythmias due to hypokalemia.
Ephedrine:
Ephedrine may enhance the metabolic clearance of corticosteroids, resulting in decreased blood levels and lessened physiologic activity, thus requiring an increase in corticosteroid dosage.
Estrogens, including Oral Contraceptives:
Estrogens may decrease the hepatic metabolism of certain corticosteroids, thereby increasing their effect.
CYP 3A4 Inducers:
Dexamethasone is metabolized by CYP 3A4. Drugs which induce cytochrome P450 3A4 (CYP 3A4) enzyme activity (e.g., barbiturates, phenytoin, carbamazepine, rifampin) may enhance the metabolism of corticosteroids and require that the dosage of the corticosteroid be increased.
CYP 3A4 Inhibitors:
Concomitant administration of dexamethasone with erythromycin, a moderate CYP 3A4 inhibitor, has the potential to result in increased plasma concentrations of dexamethasone. Ketoconazole, a strong CYP3A4 inhibitor, has been reported to decrease the metabolism of certain corticosteroids by up to 60%, leading to increased risk of corticosteroid side effects. In addition, ketoconazole alone can inhibit adrenal corticosteroid synthesis and may cause adrenal insufficiency during corticosteroid withdrawal. Co-administration with other drugs which strongly inhibit CYP 3A4 (e.g., itraconazole, clarithromycin, ritonavir, cobicistat-containing products) may lead to increased plasma concentrations of corticosteroids and potentially increase the risk for systemic corticosteroid side effects. Consider the benefit of co-administration versus the potential risk of systemic corticosteroid effects, in which case patients should be monitored for systemic corticosteroid side effects.
CYP 3A4 Substrates:
Dexamethasone is a moderate inducer of CYP 3A4. Co-administration with other drugs that are metabolized by CYP 3A4 (e.g., indinavir, erythromycin) may increase their clearance, resulting in decreased plasma concentration.
Nonsteroidal Anti-Inflammatory Agents (NSAIDS):
Concomitant use of aspirin (or other nonsteroidal anti-inflammatory agents) and corticosteroids increases the risk of gastrointestinal side effects. Aspirin should be used cautiously in conjunction with corticosteroids in hypoprothrombinemia. The clearance of salicylates may be increased with concurrent use of corticosteroids.
Phenytoin:
In post-marketing experience, there have been reports of both increases and decreases in phenytoin levels with dexamethasone co-administration, leading to alterations in seizure control.
Skin Tests:
Corticosteroids may suppress reactions to skin tests.
Thalidomide:
Co-administration with thalidomide should be employed cautiously, as toxic epidermal necrolysis has been reported with concomitant use.
Vaccines:
Patients on corticosteroid therapy may exhibit a diminished response to toxoids and live or inactivated vaccines due to inhibition of antibody response. Corticosteroids may also potentiate the replication of some organisms contained in live attenuated vaccines. Routine administration of vaccines or toxoids should be deferred until corticosteroid therapy is discontinued if possible (see WARNINGS : Infections, Vaccination ).
DESCRIPTION
Dexamethasone Tablets 0.5 mg, 0.75 mg, 4 mg and 6 mg are for oral administration. Each tablet contains 0.5 mg, 0.75 mg, 4 mg or 6 mg of dexamethasone.
Dexamethasone, a synthetic adrenocortical steroid, is a white to practically white, odorless, crystalline powder. It is stable in air. It is practically insoluble in water. It is designated chemically as 9-fluoro-11β, 17, 21-trihydroxy-16α-methylpregna-1,4-diene-3,20-dione.
The structural formula is represented below:
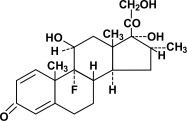 | |
| C 22 H 29 FO 5 | MW 392.47 |
Each tablet contains anhydrous lactose, croscarmellose sodium, magnesium stearate, microcrystalline cellulose and stearic acid. In addition, the 0.5 mg tablet contains D&C Yellow #10. The 0.75 mg tablet contains D&C Yellow #10 and FD&C Blue #1.
CLINICAL PHARMACOLOGY
Glucocorticoids, naturally occurring and synthetic, are adrenocortical steroids that are readily absorbed from the gastrointestinal tract. Glucocorticoids cause varied metabolic effects. In addition, they modify the body's immune responses to diverse stimuli. Naturally occurring glucocorticoids (hydrocortisone and cortisone), which also have sodium-retaining properties, are used as replacement therapy in adrenocortical deficiency states. Their synthetic analogs including dexamethasone are primarily used for their anti-inflammatory effects in disorders of many organ systems.
At equipotent anti-inflammatory doses, dexamethasone almost completely lacks the sodium-retaining property of hydrocortisone and closely related derivatives of hydrocortisone.
HOW SUPPLIED
Dexamethasone tablets are available as:
| 0.5 mg tablets scored (yellow), debossed “F 084” and supplied in: | |
| Bottles of 100, | NDC 47781-905-01 |
| 0.75 mg tablets scored (blue), debossed “F 085” and supplied in: | |
| Bottles of 100, | NDC 47781-907-01 |
| 4 mg tablets scored (white), debossed “F 087” and supplied in: | |
| Bottles of 100, | NDC 47781-914-01 |
| Bottles of 40, | NDC 47781-914-40 |
| Blister Carton of 100, | NDC 47781-914-51 |
| 6 mg tablets scored (white), debossed “F 129” and supplied in: | |
| Bottles of 100, | NDC 47781-916-01 |
Store at 20°C to 25°C (68°F to 77°F) [See USP Controlled Room Temperature]. Dispense in a tight, light resistant container as defined in the USP/NF.
Product of USA
Distributed by: Alvogen, Inc. Morristown, NJ 07960 USA
PI905-00 Revised: February 2024