Get your patient on Colchicine - Colchicine capsule (Colchicine)
Colchicine - Colchicine capsule prescribing information
1 INDICATIONS AND USAGE
Colchicine capsules are indicated for prophylaxis of gout flares in adults.
Limitations of use:
The safety and effectiveness of colchicine capsules for acute treatment of gout flares during prophylaxis has not been studied.
Colchicine capsules are not an analgesic medication and should not be used to treat pain from other causes.
2 DOSAGE AND ADMINISTRATION
Recommended Dosage for Gout Prophylaxis
For prophylaxis of gout flares, the recommended dosage of colchicine capsules is 0.6 mg once or twice daily. The maximum dose is 1.2 mg per day.
Colchicine capsules are administered orally, without regard to meals.
3 DOSAGE FORMS AND STRENGTHS
0.6 mg capsules - Hard Gelatin Capsules, blue green opaque cap printed with “GPI 0.6mg” and aqua blue opaque body printed with “001” contains white to off-white powder.
8 USE IN SPECIFIC POPULATIONS
N/A
Pregnancy
Risk Summary
Available data from published literature on colchicine use in pregnancy over several decades have not identified any drug associated risks for major birth defects, miscarriage, or other adverse maternal or fetal outcomes (see Data) . Colchicine crosses the human placenta. Although animal reproductive and developmental studies were not conducted with colchicine capsules, published animal reproduction and development studies indicate that colchicine causes embryofetal toxicity, teratogenicity, and altered postnatal development at exposures within or above the clinical therapeutic range.
The background risk of major birth defects and miscarriage for the indicated population is unknown. All pregnancies have a background risk of birth defect, loss or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Data
Human Data
Available data from published observational studies, case series, and case reports over several decades do not suggest an increased risk for major birth defects or miscarriage in pregnant women with rheumatic diseases (such as rheumatoid arthritis, Behcet’s disease, or Familial Mediterranean Fever (FMF)) treated with colchicine at therapeutic doses during pregnancy. Limitations of these data include the lack of randomization and inability to control for confounders such as underlying maternal disease and maternal use of concomitant medications.
Lactation
Risk Summary
Colchicine is present in human milk (see Data) . Adverse events in breastfed infants have not been reported in the published literature after administration of colchicine to lactating women. There are no data on the effects of colchicine on milk production. The developmental and health benefits of breastfeeding should be considered along with the mother’s clinical need for colchicine capsules and any potential adverse effects on the breastfed child from colchicine capsules or from the underlying maternal condition.
Data
Human data
Limited published data from case reports and a small lactation study demonstrate that colchicine is present in breastmilk. A systematic review of literature reported no adverse effects in 149 breastfed children. In a prospective observational cohort study, no gastrointestinal or other symptoms were reported in 38 colchicine-exposed breastfed infants.
Females and Males of Reproductive Potential
Infertility
Case reports and epidemiology studies in human male subjects on colchicine therapy indicated that infertility from colchicine is rare and may be reversible.
Pediatric Use
Gout is rare in pediatric patients; the safety and effectiveness of colchicine capsules in pediatric patients has not been evaluated in controlled studies.
Geriatric Use
Because of the increased incidence of decreased renal function in the elderly population, and the higher incidence of other co-morbid conditions in the elderly population requiring the use of other medications, reducing the dosage of colchicine when elderly patients are treated with colchicine should be carefully considered.
Renal Impairment
No dedicated pharmacokinetic study has been conducted using colchicine capsules in patients with varying degrees of renal impairment. Colchicine is known to be excreted in urine in humans and the presence of severe renal impairment has been associated with colchicine toxicity. Urinary clearance of colchicine and its metabolites may be decreased in patients with impaired renal function. Dose reduction or alternatives should be considered for the prophylaxis of gout flares in patients with severe renal impairment. Colchicine is not effectively removed by hemodialysis. Patients who are undergoing hemodialysis should be monitored carefully for colchicine toxicity.
Hepatic Impairment
No dedicated pharmacokinetic study using colchicine capsules has been conducted in patients with varying degrees of hepatic impairment. Colchicine is known to be metabolized in humans and the presence of severe hepatic impairment has been associated with colchicine toxicity. Hepatic clearance of colchicine may be significantly reduced and plasma half-life prolonged in patients with chronic hepatic impairment.
Dose reduction or alternatives should be considered for the prophylaxis of gout flares in patients with severe hepatic impairment.
4 CONTRAINDICATIONS
Patients with renal or hepatic impairment should not be given colchicine capsules with drugs that inhibit both Pglycoprotein and CYP3A4 inhibitors [see Drug Interactions (7) ] . Combining these dual inhibitors with colchicine in patients with renal or hepatic impairment has resulted in life-threatening or fatal colchicine toxicity.
Patients with both renal and hepatic impairment should not be given colchicine capsules.
5 WARNINGS AND PRECAUTIONS
Fatal Overdose
Fatal overdoses, both accidental and intentional, have been reported in adults and children who have ingested colchicine [see Overdosage (10) ] . Colchicine capsules should be kept out of the reach of children.
Blood Dyscrasias
Myelosuppression, leukopenia, granulocytopenia, thrombocytopenia, pancytopenia, and aplastic anemia have been reported with colchicine used in therapeutic doses.
Interactions with CYP3A4 and P-gp Inhibitors
Because colchicine is a substrate for both the CYP3A4 metabolizing enzyme and the P-glycoprotein efflux transporter, inhibition of either of these pathways may lead to colchicine-related toxicity. Inhibition of both CYP3A4 and P-gp by dual inhibitors such as clarithromycin has been reported to produce life-threatening or fatal colchicine toxicity due to significant increases in systemic colchicine levels. Therefore, concomitant use of colchicine capsules and inhibitors of CYP3A4 or Pglycoprotein should be avoided [see Drug Interactions (7) ] . If avoidance is not possible, reduced daily dose should be considered and the patient should be monitored closely for colchicine toxicity. Use of colchicine capsules in conjunction with drugs that inhibit both P-gp and CYP3A4 is contraindicated in patients with renal or hepatic impairment [see Contraindications (4) ] .
Neuromuscular Toxicity
Neuromuscular toxicity and rhabdomyolysis have been reported from chronic treatment with colchicine in therapeutic doses, especially in combination with other drugs known to cause this effect. Patients with impaired renal function and elderly patients (even those with normal renal and hepatic function) are at increased risk. Once colchicine treatment is ceased, the symptoms generally resolve within 1 week to several months.
6 ADVERSE REACTIONS
Gastrointestinal disorders are the most common adverse reactions with colchicine. They are often the first signs of toxicity and may indicate that the colchicine dosage needs to be reduced or therapy stopped. These include diarrhea, nausea, vomiting, and abdominal pain.
Colchicine has been reported to cause neuromuscular toxicity, which may present as muscle pain or weakness [see Warnings and Precautions (5.4) ] .
Toxic manifestations associated with colchicine include myelosuppression, disseminated intravascular coagulation, and injury to cells in the renal, hepatic, circulatory, and central nervous system. These most often occur with excessive accumulation or overdosage [see Overdosage (10) ] .
The following reactions have been reported with colchicine. These have been generally reversible by interrupting treatment or lowering the dose of colchicine:
Digestive: abdominal cramping, abdominal pain, diarrhea, lactose intolerance, nausea, vomiting
Neurological: sensory motor neuropathy
Dermatological: alopecia, maculopapular rash, purpura, rash
Hematological: leukopenia, granulocytopenia, thrombocytopenia, pancytopenia, aplastic anemia
Hepatobiliary: elevated AST, elevated ALT
Musculoskeletal: myopathy, elevated CPK, myotonia, muscle weakness, muscle pain, rhabdomyolysis
Reproductive: azoospermia, oligospermia
7 DRUG INTERACTIONS
Colchicine is a substrate of the efflux transporter P-glycoprotein (P-gp), and the CYP3A4 metabolizing enzyme. Fatal drug interactions have been reported when colchicine is administered with clarithromycin, a dual inhibitor of CYP3A4 and P-glycoprotein. Toxicities have also been reported when colchicine is administered with inhibitors of CYP3A4 that may not be potent inhibitors of P-gp (e.g., grapefruit juice, erythromycin, verapamil), or inhibitors of P-gp that may not be potent inhibitors of CYP3A4 (e.g., cyclosporine).
Patients with renal or hepatic impairment should not be given colchicine capsules with drugs that inhibit both Pglycoprotein and CYP3A4 [see Contraindications (4) ] . Combining these dual inhibitors with colchicine capsules in patients with renal and hepatic impairment has resulted in life-threatening or fatal colchicine toxicity.
Physicians should ensure that patients are suitable candidates for treatment with colchicine capsules and remain alert for signs and symptoms of toxic reactions associated with increased colchicine exposure due to drug interactions. Signs and symptoms of colchicine toxicity should be evaluated promptly and, if toxicity is suspected, colchicine capsules should be discontinued immediately.
CYP3A4
The concomitant use of colchicine capsules and CYP3A4 inhibitors (e.g., clarithromycin, ketoconazole, grapefruit juice, erythromycin, verapamil, etc.) should be avoided due to the potential for serious and life-threatening toxicity [see Warnings and Precautions (5.3) and Clinical Pharmacology (12) ] .
If co-administration of colchicine capsules and a CYP3A4 inhibitor is necessary, the dose of colchicine capsules should be adjusted by either reducing the daily dose or reducing the dose frequency, and the patient should be monitored carefully for colchicine toxicity [see Clinical Pharmacology (12) ] .
P-glycoprotein
The concomitant use of colchicine capsules and inhibitors of P-glycoprotein (e.g. clarithromycin, ketoconazole, cyclosporine, etc.) should be avoided due to the potential for serious and life-threatening toxicity [see Warnings and Precautions (5.3) and Clinical Pharmacology (12) ] .
If co-administration of colchicine capsules and a P-gp inhibitor is necessary, the dose of colchicine capsules should be adjusted by either reducing the daily dose or reducing the dose frequency, and the patient should be monitored carefully for colchicine toxicity [see Clinical Pharmacology (12) ] .
HMG-CoA Reductase Inhibitors and Fibrates
Some drugs such as HMG-CoA reductase inhibitors and fibrates may increase the risk of myopathy when combined with colchicine capsules. Complaints of muscle pain or weakness could be an indication to check serum creatinine kinase levels for signs of myopathy.
Drug-Drug Interaction Studies
Four pharmacokinetic studies evaluated the effects of co-administration of voriconazole (200 mg BID), fluconazole (200 mg QD), cimetidine (800 mg BID), and propafenone (225 mg BID) on systemic levels of colchicine. Colchicine can be administered with these drugs at the tested doses without a need for dose adjustment. However, these results should not be extrapolated to other co-administered drugs [see Drug-Drug Interactions (7.1 , 7.2 ) and Pharmacokinetics (12.3) ] .
11 DESCRIPTION
Colchicine is an alkaloid obtained from the plant colchicum autumnale .
The chemical name for colchicine is ( S)-N- (5,6,7,9-tetrahydro-1,2,3,10-tetramethoxy-9-oxobenzol[a] heptalen-7-yl) acetamide. The structural formula is represented below:
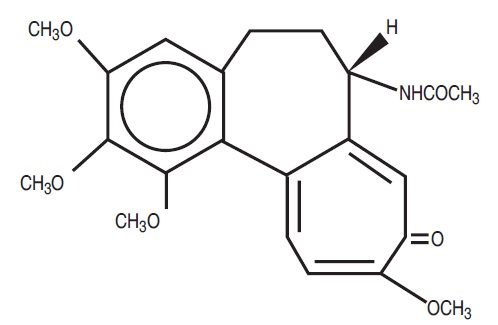
C 22 H 25 NO 6 M.W. 399.4
Colchicine consists of pale yellow scales or powder; it darkens on exposure to light. Colchicine is soluble in water, freely soluble in alcohol, and slightly soluble in ether.
Colchicine capsules are supplied for oral administration. Each capsule contains 0.6 mg Colchicine, USP and the following inactive ingredients: colloidal silicon dioxide, lactose anhydrous, magnesium stearate, microcrystalline cellulose, and sodium starch glycolate. The capsule shell contains ammonium hydroxide, FD&C Blue #1, ferrosoferric oxide, gelatin, propylene glycol, shellac, titanium dioxide and yellow iron oxide.
12 CLINICAL PHARMACOLOGY
Mechanism of Action
Colchicine’s effectiveness as a treatment for gout has been postulated to be due to its ability to block neutrophil-mediated inflammatory responses induced by monosodium urate crystals in synovial fluid. Colchicine disrupts the polymerization of β-tubulin into microtubules, thereby preventing the activation, degranulation, and migration of neutrophils to sites of inflammation. Colchicine also interferes with the inflammasome complex found in neutrophils and monocytes that mediates interleukin-1β (IL-1β) activation.
Pharmacokinetics
Absorption
In healthy adults, colchicine capsules when given orally reached a mean C max of 3 ng/mL in 1.3 h (range 0.7 to 2.5 h) after 0.6 mg single dose administration.
Absolute bioavailability is reported to be approximately 45%.
Administration with food has no effect on the rate or extent of colchicine absorption.
Colchicine is not effectively removed by hemodialysis.
Distribution
Colchicine has a mean apparent volume of distribution in healthy young volunteers of approximately 5 to 8 L/kg. Colchicine binding to serum protein is about 39%, primarily to albumin. Colchicine crosses the placenta and distributes into breast milk [see Pregnancy (8.1) and Lactation (8.2) ] .
Metabolism
A published in vitro human liver microsome study showed that about 16% of colchicine is metabolized to 2-O-demethylcolchicine and 3-O-demethylcolchicine (2- and 3-DMC, respectively) by CYP3A4. Glucuronidation is also believed to be a metabolic pathway for colchicine.
Excretion
In a published study in healthy volunteers, 40 to 65% of the total absorbed dose of colchicine (1 mg administered orally) was recovered unchanged in urine. Enterohepatic recirculation and biliary excretion are also believed to play a role in colchicine elimination. Colchicine is a substrate of P-gp and P-gp efflux is postulated to play an important role in colchicine disposition. Elimination half-life in humans was found to be 31 h (range 21.7 to 49.9 h).
Special Populations
There is no difference between men and women in the pharmacokinetic disposition of colchicine.
Pediatric Patients: Pharmacokinetics of colchicine was not evaluated in pediatric patients.
Elderly: Pharmacokinetics of colchicine have not been determined in elderly patients. A published report described the pharmacokinetics of 1 mg oral colchicine tablet in four elderly women compared to six young healthy males. The mean age of the four elderly women was 83 years (range 75 to 93), mean weight was 47 kg (38 to 61 kg) and mean creatinine clearance was 46 mL/min (range 25 to 75 mL/min). Mean peak plasma levels and AUC of colchicine were two times higher in elderly subjects compared to young healthy males. It is possible that the higher exposure in the elderly subjects was due to decreased renal function.
Renal impairment: Pharmacokinetics of colchicine in patients with mild and moderate renal impairment is not known. A published report described the disposition of colchicine (1 mg) in young adult men and women patients who had end-stage renal disease requiring dialysis compared to patients with normal renal function. Patients with end-stage renal disease had 75% lower colchicine clearance (0.17 vs. 0.73 L/hr/kg) and prolonged plasma elimination half-life (18.8 hrs vs. 4.4 hrs) as compared to subjects with normal renal function [see Renal Impairment (8.6) ] .
Hepatic impairment: Published reports on the pharmacokinetics of intravenous colchicine in patients with severe chronic liver disease, as well as those with alcoholic or primary biliary cirrhosis, and normal renal function suggest wide inter-patient variability. In some subjects with mild to moderate cirrhosis, the clearance of colchicine is significantly reduced and plasma half-life prolonged compared to healthy subjects. In subjects with primary biliary cirrhosis, no consistent trends were noted [see Hepatic Impairment (8.7) ] . No pharmacokinetic data are available for patients with severe hepatic impairment (Child-Pugh C).
Drug Interactions
Pharmacokinetic studies evaluating changes in systemic levels of colchicine when co-administered with CYP3A4 inhibitors in healthy volunteers have been conducted with colchicine capsules. While voriconazole 200 mg BID for 5 days (considered a strong CYP3A4 inhibitor) and cimetidine 800 mg BID for 5 days (considered a weak CYP3A4 inhibitor) did not cause any changes in colchicine systemic levels, fluconazole 200 mg QD for 4 days with a 400 mg loading dose (considered a moderate CYP3A4 inhibitor) increased colchicine AUC by 40%. As voriconazole, cimetidine, and fluconazole are known as CYP3A4 inhibitors that do not inhibit P-gp, these studies show that CYP3A4 inhibition by itself may not lead to clinically significant increases in colchicine systemic levels in humans, and P-gp inhibition in addition to CYP3A4 inhibition may be necessary for clinically meaningful interactions of colchicine. However, based on published case reports that indicate the presence of colchicine toxicity when colchicine is co-administered with strong to moderate CYP3A4 inhibitors such as clarithromycin, erythromycin, grapefruit juice, etc., as well as the 40% increase in systemic levels of colchicine observed with concomitantly administered fluconazole (a moderate CYP3A4 inhibitor that is not known to inhibit P-gp) in a drug-drug interaction study, the drug-drug interaction potential of colchicine with strong or moderate CYP3A4 inhibitors that do not inhibit P-gp cannot be ruled out completely.
Co-administration of colchicine capsules with propafenone (a P-gp inhibitor) at 225 mg BID for 5 days, in a pharmacokinetic study in healthy volunteers, did not cause any changes in systemic levels of colchicine. This indicates that propafenone can be administered with colchicine capsules without any dose adjustment. However, these results should not be extrapolated to other P-gp inhibitors as colchicine is known to be a substrate for P-gp and case reports of colchicine toxicity associated with the co-administration of P-gp inhibitors such as cyclosporine have been published.
13 NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Carcinogenicity studies of colchicine have not been conducted. Due to the potential for colchicine to produce aneuploid cells (cells with an unequal number of chromosomes), colchicine presents a theoretical increased risk of malignancy.
Mutagenesis
Published studies demonstrated that colchicine was negative for mutagenicity in the bacterial reverse mutation assay. However, in vitro chromosomal aberration assays demonstrated the formation of micronuclei following colchicine treatment. Because published studies demonstrated that colchicine induces aneuploidy through the process of mitotic nondisjunction without structural DNA changes, colchicine is not considered clastogenic, although micronuclei are formed.
Impairment of Fertility
There were no studies of the effects of colchicine capsules on fertility. However, published nonclinical studies have demonstrated that colchicine-induced disruption of microtubule formation affects meiosis and mitosis. Published reproductive studies with colchicine reported abnormal sperm morphology and reduced sperm counts in males, and interference with sperm penetration, second meiotic division, and normal cleavage in females.
Case reports and epidemiology studies in human male subjects on colchicine therapy indicate that infertility from colchicine is rare. A case report indicated that azoospermia was reversed when therapy was stopped. Case reports and epidemiology studies in female subjects on colchicine therapy have not established a clear relationship between colchicine use and female infertility.
14 CLINICAL STUDIES
The evidence for the efficacy of colchicine in patients with chronic gout is derived from the published literature. Two randomized clinical trials assessed the efficacy of colchicine 0.6 mg twice a day for the prophylaxis of gout flares in patients with gout initiating treatment with urate lowering therapy. In both trials, treatment with colchicine decreased the frequency of gout flares.
16 HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
Colchicine capsules, 0.6 mg are Hard Gelatin Capsules, blue green opaque cap printed with “GPI 0.6mg” and aqua blue opaque body printed with “001” contains white to off-white powder.
Bottles of 30 capsules NDC 70010-001-03
Bottles of 100 capsules NDC 70010-001-01
Bottles of 1000 capsules NDC 70010-001-10
Storage
Store at 20°C to 25°C (68°F to 77°F). [See USP Controlled Room Temperature].
Protect from light and moisture.