Get your patient on Cevimeline Hydrochloride - Cevimeline Hydrochloride capsule (Cevimeline Hydrochloride)
Cevimeline Hydrochloride - Cevimeline Hydrochloride capsule prescribing information
INDICATIONS AND USAGE
Cevimeline is indicated for the treatment of symptoms of dry mouth in patients with SjÖgren's Syndrome.
DOSAGE AND ADMINISTRATION
The recommended dose of cevimeline hydrochloride is 30 mg taken three times a day. There is insufficient safety information to support doses greater than 30 mg tid. There is also insufficient evidence for additional efficacy of cevimeline hydrochloride at doses greater than 30 mg tid.
CONTRAINDICATIONS
Cevimeline is contraindicated in patients with uncontrolled asthma, known hypersensitivity to cevimeline, and when miosis is undesirable, e.g., in acute iritis and in narrow-angle (angle-closure) glaucoma.
ADVERSE REACTIONS
Cevimeline was administered to 1777 patients during clinical trials worldwide, including SjÖgren's patients and patients with other conditions. In placebo-controlled SjÖgren's studies in the U.S., 320 patients received cevimeline doses ranging from 15 mg tid to 60 mg tid, of whom 93% were women and 7% were men. Demographic distribution was 90% Caucasian, 5% Hispanic, 3% Black and 2% of other origin. In these studies, 14.6% of patients discontinued treatment with cevimeline due to adverse events.
The following adverse events associated with muscarinic agonism were observed in the clinical trials of cevimeline in SjÖgren's syndrome patients:
•n is the total number of patients exposed to the dose at any time during the study. | ||
| Adverse Event | Cevimeline 30 mg (tid) n •= 533 | Placebo (tid) n = 164 |
| Excessive Sweating | 18.7% | 2.4% |
| Nausea | 13.8% | 7.9% |
| Rhinitis | 11.2% | 5.4% |
| Diarrhea | 10.3% | 10.3% |
| Excessive Salivation | 2.2% | 0.6% |
| Urinary Frequency | 0.9% | 1.8% |
| Asthenia | 0.5% | 0.0% |
| Flushing | 0.3% | 0.6% |
| Polyuria | 0.1% | 0.6% |
In addition, the following adverse events (≥3% incidence) were reported in the SjÖgren's clinical trials:
•n is the total number of patients exposed to the dose at any time during the study. | ||
| Adverse Event | Cevimeline 30 mg (tid) n •= 533 | Placebo (tid) n = 164 |
| Headache | 14.4% | 20.1% |
| Sinusitis | 12.3% | 10.9% |
| Upper Respiratory | 11.4% | 9.1% |
| Tract Infection | ||
| Dyspepsia | 7.8% | 8.5% |
| Abdominal Pain | 7.6% | 6.7% |
| Urinary Tract Infection | 6.1% | 3.0% |
| Coughing | 6.1% | 3.0% |
| Pharyngitis | 5.2% | 5.4% |
| Vomiting | 4.6% | 2.4% |
| Injury | 4.5% | 2.4% |
| Back Pain | 4.5% | 4.2% |
| Rash | 4.3% | 6.0% |
| Conjunctivitis | 4.3% | 3.6% |
| Dizziness | 4.1% | 7.3% |
| Bronchitis | 4.1% | 1.2% |
| Arthralgia | 3.7% | 1.8% |
| Surgical Intervention | 3.3% | 3.0% |
| Fatigue | 3.3% | 1.2% |
| Pain | 3.3% | 3.0% |
| Skeletal Pain | 2.8% | 1.8% |
| Insomnia | 2.4% | 1.2% |
| Hot Flushes | 2.4% | 0.0% |
| Rigors | 1.3% | 1.2% |
| Anxiety | 1.3% | 1.2% |
The following events were reported in SjÖgren's patients at incidences of <3% and ≥1%: constipation, tremor, abnormal vision, hypertonia, peripheral edema, chest pain, myalgia, fever, anorexia, eye pain, earache, dry mouth, vertigo, salivary gland pain, pruritus, influenza-like symptoms, eye infection, post-operative pain, vaginitis, skin disorder, depression, hiccup, hyporeflexia, infection, fungal infection, sialoadenitis, otitis media, erythematous rash, pneumonia, edema, salivary gland enlargement, allergy, gastroesophageal reflux, eye abnormality, migraine, tooth disorder, epistaxis, flatulence, toothache, ulcerative stomatitis, anemia, hypoesthesia, cystitis, leg cramps, abscess, eructation, moniliasis, palpitation, increased amylase, xerophthalmia, allergic reaction.
The following events were reported rarely in treated SjÖgren's patients (<1%): Causal relation is unknown:
Body as a Whole Disorders: aggravated allergy, precordial chest pain, abnormal crying, hematoma, leg pain, edema, periorbital edema, activated pain trauma, pallor, changed sensation temperature, weight decrease, weight increase, choking, mouth edema, syncope, malaise, face edema, substernal chest pain
Cardiovascular Disorders: abnormal ECG, heart disorder, heart murmur, aggravated hypertension, hypotension, arrhythmia, extrasystoles, t wave inversion, tachycardia, supraventricular tachycardia, angina pectoris, myocardial infarction, pericarditis, pulmonary embolism, peripheral ischemia, superficial phlebitis, purpura, deep thrombophlebitis, vascular disorder, vasculitis, hypertension
Digestive Disorders: appendicitis, increased appetite, ulcerative colitis, diverticulitis, duodenitis, dysphagia, enterocolitis, gastric ulcer, gastritis, gastroenteritis, gastrointestinal hemorrhage, gingivitis, glossitis, rectum hemorrhage, hemorrhoids, ileus, irritable bowel syndrome, melena, mucositis, esophageal stricture, esophagitis, oral hemorrhage, peptic ulcer, periodontal destruction, rectal disorder, stomatitis, tenesmus, tongue discoloration, tongue disorder, geographic tongue, tongue ulceration, dental caries
Endocrine Disorders: increased glucocorticoids, goiter, hypothyroidism
Hematologic Disorders: thrombocytopenic purpura, thrombocythemia, thrombocytopenia, hypochromic anemia, eosinophilia, granulocytopenia, leucopenia, leukocytosis, cervical lymphadenopathy, lymphadenopathy
Liver and Biliary System Disorders: cholelithiasis, increased gamma-glutamyl transferase, increased hepatic enzymes, abnormal hepatic function, viral hepatitis, increased serum glutamate oxaloacetic transaminase (SGOT) (also called AST-aspartate aminotransferase), increased serum glutamate pyruvate transaminase (SGPT) (also called ALT-alanine aminotransferase)
Metabolic and Nutritional Disorders: dehydration, diabetes mellitus, hypercalcemia, hypercholesterolemia, hyperglycemia, hyperlipemia, hypertriglyceridemia, hyperuricemia, hypoglycemia, hypokalemia, hyponatremia, thirst
Musculoskeletal Disorders: arthritis, aggravated arthritis, arthropathy, femoral head avascular necrosis, bone disorder, bursitis, costochondritis, plantar fasciitis, muscle weakness, osteomyelitis, osteoporosis, synovitis, tendinitis, tenosynovitis
Neoplasms: basal cell carcinoma, squamous carcinoma
Nervous Disorders: carpal tunnel syndrome, coma, abnormal coordination, dysesthesia, dyskinesia, dysphonia, aggravated multiple sclerosis, involuntary muscle contractions, neuralgia, neuropathy, paresthesia, speech disorder, agitation, confusion, depersonalization, aggravated depression, abnormal dreaming, emotional lability, manic reaction, paroniria, somnolence, abnormal thinking, hyperkinesia, hallucination
Miscellaneous Disorders: fall, food poisoning, heat stroke, joint dislocation, post-operative hemorrhage
Resistance Mechanism Disorders: cellulitis, herpes simplex, herpes zoster, bacterial infection, viral infection, genital moniliasis, sepsis
Respiratory Disorders: asthma, bronchospasm, chronic obstructive airway disease, dyspnea, hemoptysis, laryngitis, nasal ulcer, pleural effusion, pleurisy, pulmonary congestion, pulmonary fibrosis, respiratory disorder
Rheumatologic Disorders: aggravated rheumatoid arthritis, lupus erythematosus rash, lupus erythematosus syndrome
Skin and Appendages Disorders: acne, alopecia, burn, dermatitis, contact dermatitis, lichenoid dermatitis, eczema, furunculosis, hyperkeratosis, lichen planus, nail discoloration, nail disorder, onychia, onychomycosis, paronychia, photosensitivity reaction, rosacea, scleroderma, seborrhea, skin discoloration, dry skin, skin exfoliation, skin hypertrophy, skin ulceration, urticaria, verruca, bullous eruption, cold clammy skin
Special Senses Disorders: deafness, decreased hearing, motion sickness, parosmia, taste perversion, blepharitis, cataract, corneal opacity, corneal ulceration, diplopia, glaucoma, anterior chamber eye hemorrhage, keratitis, keratoconjunctivitis, mydriasis, myopia, photopsia, retinal deposits, retinal disorder, scleritis, vitreous detachment, tinnitus
Urogenital Disorders: epididymitis, prostatic disorder, abnormal sexual function, amenorrhea, female breast neoplasm, malignant female breast neoplasm, female breast pain, positive cervical smear test, dysmenorrhea, endometrial disorder, intermenstrual bleeding, leukorrhea, menorrhagia, menstrual disorder, ovarian cyst, ovarian disorder, genital pruritus, uterine hemorrhage, vaginal hemorrhage, atrophic vaginitis, albuminuria, bladder discomfort, increased blood urea nitrogen, dysuria, hematuria, micturition disorder, nephrosis, nocturia, increased nonprotein nitrogen, pyelonephritis, renal calculus, abnormal renal function, renal pain, strangury, urethral disorder, abnormal urine, urinary incontinence, decreased urine flow, pyuria
In one subject with lupus erythematosus receiving concomitant multiple drug therapy, a highly elevated ALT level was noted after the fourth week of cevimeline therapy. In two other subjects receiving cevimeline in the clinical trials, very high AST levels were noted. The significance of these findings is unknown.
Additional adverse events (relationship unknown) which occurred in other clinical studies (patient population different from SjÖgren's patients) are as follows:
cholinergic syndrome, blood pressure fluctuation, cardiomegaly, postural hypotension, aphasia, convulsions, abnormal gait, hyperesthesia, paralysis, abnormal sexual function, enlarged abdomen, change in bowel habits, gum hyperplasia, intestinal obstruction, bundle branch block, increased creatine phosphokinase, electrolyte abnormality, glycosuria, gout, hyperkalemia, hyperproteinemia, increased lactic dehydrogenase (LDH), increased alkaline phosphatase, failure to thrive, abnormal platelets, aggressive reaction, amnesia, apathy, delirium, delusion, dementia, illusion, impotence, neurosis, paranoid reaction, personality disorder, hyperhemoglobinemia, apnea, atelectasis, yawning, oliguria, urinary retention, distended vein, lymphocytosis.
The following adverse reaction has been identified during post-approval use of Cevimeline Hydrochloride Capsules. Because post-marketing adverse reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
POST-MARKETING ADVERSE EVENTS
Liver and Biliary System Disorders: cholecystitis
Drug Interactions
Cevimeline should be administered with caution to patients taking beta adrenergic antagonists, because of the possibility of conduction disturbances. Drugs with parasympathomimetic effects administered concurrently with cevimeline can be expected to have additive effects. Cevimeline might interfere with desirable antimuscarinic effects of drugs used concomitantly.
Drugs which inhibit CYP2D6 and CYP3A3/4 also inhibit the metabolism of cevimeline. Cevimeline should be used with caution in individuals known or suspected to be deficient in CYP2D6 activity, based on previous experience, as they may be at a higher risk of adverse events. In an in vitro study, cytochrome P450 isozymes 1A2, 2A6, 2C9, 2C19, 2D6, 2E1, and 3A4 were not inhibited by exposure to cevimeline.
DESCRIPTION
Cevimeline is cis-2'-methylspiro {1-azabicyclo [2.2.2] octane-3, 5'-[1,3] oxathiolane} hydrochloride, hydrate (2:1). Its empirical formula is C 10 H 17 NOS.HCl.1/2 H 2 O, and its structural formula is:
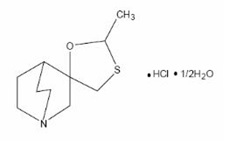
Cevimeline has a molecular weight of 244.79. It is a white to off white crystalline powder with a melting point range of 201 to 203°C. It is freely soluble in alcohol and chloroform, very soluble in water, and virtually insoluble in ether. The pH of a 1% solution ranges from 4.6 to 5.6. Inactive ingredients include lactose monohydrate, hydroxypropyl cellulose, and magnesium stearate; a hard gelatin capsule which contains D&C Yellow #10, FD&C Red #40, FD&C Yellow #6, titanium dioxide and gelatin; and an imprinting ink which contains shellac, iron oxide black, isopropyl alcohol, butyl alcohol, propylene glycol and ammonium hydroxide.
CLINICAL PHARMACOLOGY
Pharmacodynamics
Cevimeline is a cholinergic agonist which binds to muscarinic receptors. Muscarinic agonists in sufficient dosage can increase secretion of exocrine glands, such as salivary and sweat glands and increase tone of the smooth muscle in the gastrointestinal and urinary tracts.
Pharmacokinetics
Absorption: After administration of a single 30 mg capsule, cevimeline was rapidly absorbed with a mean time to peak concentration of 1.5 to 2 hours. No accumulation of active drug or its metabolites was observed following multiple dose administration. When administered with food, there is a decrease in the rate of absorption, with a fasting T MAX of 1.53 hours and a T MAX of 2.86 hours after a meal; the peak concentration is reduced by 17.3%. Single oral doses across the clinical dose range are dose proportional.
Distribution: Cevimeline has a volume of distribution of approximately 6L/kg and is <20% bound to human plasma proteins. This suggests that cevimeline is extensively bound to tissues; however, the specific binding sites are unknown.
Metabolism: Isozymes CYP2D6 and CYP3A3/4 are responsible for the metabolism of cevimeline. After 24 hours, 86.7% of the dose was recovered (16.0% unchanged, 44.5% as cis and trans-sulfoxide, 22.3% of the dose as glucuronic acid conjugate and 4% of the dose as N-oxide of cevimeline). Approximately 8% of the trans-sulfoxide metabolite is then converted into the corresponding glucuronic acid conjugate and eliminated. Cevimeline did not inhibit cytochrome P450 isozymes 1A2, 2A6, 2C9, 2C19, 2D6, 2E1, and 3A4.
Excretion: The mean half-life of cevimeline is 5+/-1 hours. After 24 hours, 84% of a 30 mg dose of cevimeline was excreted in urine. After seven days, 97% of the dose was recovered in the urine and 0.5% was recovered in the feces.
Special Populations: The effects of renal impairment, hepatic impairment, or ethnicity on the pharmacokinetics of cevimeline have not been investigated.
Clinical Studies
Cevimeline has been shown to improve the symptoms of dry mouth in patients with SjÖgren's Syndrome.
A 6-week, randomized, double blind, placebo-controlled study was conducted in 75 patients (10 men, 65 women) with a mean age of 53.6 years (range 33-75). The racial distribution was Caucasian 92%, Black 1% and other 7%. The effects of cevimeline at 30 mg tid (90 mg/day) and 60 mg tid (180 mg/day) were compared to those of placebo. Patients were evaluated by a measure called global improvement, which is defined as a response of "better" to the question, "Please rate the overall condition of your dry mouth now compared with how you felt before starting treatment in this study." Patients also had the option of selecting "worse" or "no change" as answers. Seventy-six percent of the patients in the 30 mg tid group reported a global improvement in their dry mouth symptoms compared to 35% of the patients in the placebo group. This difference was statistically significant at p=0.0043. There was no evidence that patients in the 60 mg tid group had better global evaluation scores than the patients in the 30 mg tid group.
A 12-week, randomized, double-blind, placebo-controlled study was conducted in 197 patients (10 men, 187 women) with a mean age of 54.5 years (range 23-74). The racial distribution was Caucasian 91.4%, Black 3% and other 5.6%. The effects of cevimeline at 15 mg tid (45 mg/day) and 30 mg tid (90 mg/day) were compared to those of placebo. Statistically significant global improvement in the symptoms of dry mouth (p=0.0004) was seen for the 30 mg tid group compared to placebo, but not for the 15 mg group compared to placebo. Salivary flow showed statistically significant increases at both doses of cevimeline during the study compared to placebo.
A second 12-week, randomized, double-blind, placebo-controlled study was conducted in 212 patients (11 men, 201 women) with a mean age of 55.3 years (range 24-75). The racial distribution was Caucasian 88.7%, Black 1.9% and other 9.4%. The effects of cevimeline at 15 mg tid (45 mg/day) and 30 mg tid (90 mg/day) were compared to those of placebo. No statistically significant differences were noted in the patient global evaluations. However, there was a higher placebo response rate in this study compared to the aforementioned studies. The 30 mg tid group showed a statistically significant increase in salivary flow from pre-dose to post-dose compared to placebo (p=0.0017).
Clinical Studies
Cevimeline has been shown to improve the symptoms of dry mouth in patients with SjÖgren's Syndrome.
A 6-week, randomized, double blind, placebo-controlled study was conducted in 75 patients (10 men, 65 women) with a mean age of 53.6 years (range 33-75). The racial distribution was Caucasian 92%, Black 1% and other 7%. The effects of cevimeline at 30 mg tid (90 mg/day) and 60 mg tid (180 mg/day) were compared to those of placebo. Patients were evaluated by a measure called global improvement, which is defined as a response of "better" to the question, "Please rate the overall condition of your dry mouth now compared with how you felt before starting treatment in this study." Patients also had the option of selecting "worse" or "no change" as answers. Seventy-six percent of the patients in the 30 mg tid group reported a global improvement in their dry mouth symptoms compared to 35% of the patients in the placebo group. This difference was statistically significant at p=0.0043. There was no evidence that patients in the 60 mg tid group had better global evaluation scores than the patients in the 30 mg tid group.
A 12-week, randomized, double-blind, placebo-controlled study was conducted in 197 patients (10 men, 187 women) with a mean age of 54.5 years (range 23-74). The racial distribution was Caucasian 91.4%, Black 3% and other 5.6%. The effects of cevimeline at 15 mg tid (45 mg/day) and 30 mg tid (90 mg/day) were compared to those of placebo. Statistically significant global improvement in the symptoms of dry mouth (p=0.0004) was seen for the 30 mg tid group compared to placebo, but not for the 15 mg group compared to placebo. Salivary flow showed statistically significant increases at both doses of cevimeline during the study compared to placebo.
A second 12-week, randomized, double-blind, placebo-controlled study was conducted in 212 patients (11 men, 201 women) with a mean age of 55.3 years (range 24-75). The racial distribution was Caucasian 88.7%, Black 1.9% and other 9.4%. The effects of cevimeline at 15 mg tid (45 mg/day) and 30 mg tid (90 mg/day) were compared to those of placebo. No statistically significant differences were noted in the patient global evaluations. However, there was a higher placebo response rate in this study compared to the aforementioned studies. The 30 mg tid group showed a statistically significant increase in salivary flow from pre-dose to post-dose compared to placebo (p=0.0017).
HOW SUPPLIED
Cevimeline Hydrochloride Capsules are available as hard gelatin capsule with tan opaque cap and tan opaque body imprinted with "NL 999" on the cap and "30 mg" on the body with black ink, filled with white to off white granular powder.
It is supplied in:
Child-resistant bottles of 30 Capsules (NDC 40032-999-03)
Child-resistant bottles of 100 Capsules (NDC 40032-999-01)
Bottles of 500 Capsules (NDC 40032-999-05)
Store at 20° to 25°C (68° to 77°F). [See USP Controlled Room Temperature].
Dispense in a tight, light resistant container as defined in the USP/NF.
Rx Only
Manufactured by:
Novel Laboratories, Inc.
Somerset, NJ 08873
Iss. 02/2016
PI9990000101