Get your patient on Atzumi - Dihydroergotamine Mesylate powder (Dihydroergotamine Mesylate)
Atzumi - Dihydroergotamine Mesylate powder prescribing information
WARNING: PERIPHERAL ISCHEMIA FOLLOWING COADMINISTRATION WITH STRONG CYP3A4 INHIBITORS
INDICATIONS AND USAGE
ATZUMI is indicated for the acute treatment of migraine with or without aura in adults.
Limitations of Use
ATZUMI is not indicated for the preventive treatment of migraine.
ATZUMI is not indicated for the management of hemiplegic migraine or migraine with brainstem aura.
DOSAGE AND ADMINISTRATION
- ATZUMI is for nasal administration only. (2.1 )
- The recommended dose of ATZUMI is 5.2 mg, the contents of one nasal device, administered into one nostril. (2.1 )
- To administer a dose, the white air pump of the ATZUMI device must be squeezed three separate times into one nostril. (2.1 )
- The dose may be repeated, if needed, a minimum of 1 hour after the first dose. The maximum dose in a 24-hour period is 10.4 mg (two doses of ATZUMI 5.2 mg). (2.1 )
- The safety of taking more than 4 doses within a 7-day period or 12 doses within a 30-day period has not been established. (2.1 )
- Prior to initiation, a cardiovascular evaluation is recommended. (2.2 )
Dosing Information
ATZUMI is for nasal administration only.
The recommended dose of ATZUMI is 5.2 mg (the contents of one nasal device) and is administered as a powdered medicine into one nostril [see Dosage and Administration (2.3) ].
The dose may be repeated, if needed, a minimum of 1 hour after the first dose. The maximum dose in a 24-hour period is 10.4 mg (two doses of ATZUMI 5.2 mg). The safety of taking more than 4 doses in a 7-day period or 12 doses within a 30-day period has not been established.
Assessment Prior to First Dose
Prior to initiation of ATZUMI, a cardiovascular evaluation is recommended [see Warnings and Precautions (5.2) ] . For patients with risk factors predictive of coronary artery disease who are determined to have a satisfactory cardiovascular evaluation, it is strongly recommended that administration of the first dose of ATZUMI take place in the setting of an equipped healthcare facility.
Administration Instructions
- Priming is not required.
- To administer a dose of ATZUMI, remove the round blue tab from the blue nozzle, and insert the blue nozzle into one nostril. Squeeze the white air pump 3 separate times into 1 nostril while inhaling. Allow the white air pump to expand back to its original shape between squeezes [see Instructions for Use ].
- Fast, complete, pulse-like squeezes are needed to deliver the complete dose. Do not squeeze slowly, partially or with any hesitation.
DOSAGE FORMS AND STRENGTHS
Nasal Powder: 5.2 mg dihydroergotamine as a white powder in a single-dose nasal device.
USE IN SPECIFIC POPULATIONS
Pregnancy
Risk Summary
Available data from published literature indicate an increased risk of preterm delivery with dihydroergotamine, the active moiety in ATZUMI, use during pregnancy. Avoid use of ATZUMI during pregnancy [see Warnings and Precautions (5.7) ] . Data collected over decades have shown no increased risk of major birth defects or miscarriage with the use of dihydroergotamine during pregnancy.
In animal reproduction studies, adverse effects on development were observed following intranasal administration of dihydroergotamine mesylate during pregnancy (decreased fetal body weight and/or skeletal ossification) in rats and rabbits or during pregnancy and lactation in rats (decreased body weight and impaired reproductive function in the offspring) at doses that were not associated with maternal toxicity (see Data ) .
All pregnancies have a background risk of birth defect, loss, or other adverse outcomes. In the U.S. general population, the estimated background risk of major birth defects and miscarriages in clinically recognized pregnancies is 2% to 4% and 15% to 20%, respectively. The estimated rate of major birth defects (2.2% to 2.9%) and miscarriage (17%) among deliveries to women with migraine are similar to rates reported in women without migraine.
Clinical Considerations
Disease-Associated Maternal and/or Embryo/Fetal Risk
Published data have suggested that women with migraine may be at increased risk of preeclampsia and gestational hypertension during pregnancy.
Data
Animal Data
Intranasal administration of dihydroergotamine mesylate to pregnant rats throughout the period of organogenesis resulted in decreased fetal body weight and/or skeletal ossification at doses of 0.16 mg/day and greater. A no-effect level for adverse effects on embryofetal development was not identified in rats.
Intranasal administration of dihydroergotamine mesylate to pregnant rabbits throughout organogenesis resulted in decreased skeletal ossification at 3.6 mg/day. The no-effect dose for adverse effects on embryofetal development in rabbits was 1.2 mg/day.
Intranasal administration of dihydroergotamine mesylate to female rats throughout pregnancy and lactation resulted in decreased body weight and impaired reproductive function (decreased mating indices) in the offspring at doses of 0.16 mg/day or greater. A no-effect dose for adverse effects on pre- and postnatal development in rats was not established. Effects on offspring development occurred at doses below those that produced evidence of significant maternal toxicity in these studies.
Dihydroergotamine-induced intrauterine growth retardation has been attributed to reduced uteroplacental blood flow resulting from prolonged vasoconstriction of the uterine vessels and/or increased myometrial tone.
Lactation
Risk Summary
There are no data on the presence of dihydroergotamine in human milk; however, ergotamine, a related drug, is present in human milk. There are reports of diarrhea, vomiting, weak pulse, and unstable blood pressure in breastfed infants exposed to ergotamine. ATZUMI may reduce milk supply because it may decrease prolactin levels. Because of the potential for reduced milk supply and serious adverse events in the breastfed infant, including diarrhea, vomiting, weak pulse, and unstable blood pressure, advise patients not to breastfeed during treatment with ATZUMI and for 3 days after the last dose. Breast milk supply during this time should be pumped and discarded.
Pediatric Use
The safety and effectiveness of ATZUMI have not been established in pediatric patients.
Geriatric Use
Clinical studies of ATZUMI and other dihydroergotamine products did not include sufficient numbers of subjects aged 65 and older to determine whether they respond differently from younger subjects. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function and of concomitant disease or other drug therapy.
CONTRAINDICATIONS
ATZUMI is contraindicated in patients:
- with concomitant use of strong CYP3A4 inhibitors [see Warnings and Precautions (5.1) and Drug Interactions (7.1) ]
- with ischemic heart disease (e.g., angina pectoris, history of myocardial infarction, or documented silent ischemia) or patients who have clinical symptoms or findings consistent with coronary artery vasospasm, including Prinzmetal's variant angina [see Warnings and Precautions (5.4) ]
- with uncontrolled hypertension [see Warnings and Precautions (5.5) ]
- with peripheral arterial disease
- with sepsis
- following vascular surgery
- with severe hepatic impairment
- with severe renal impairment
- with known hypersensitivity to ergot alkaloids
- with recent use (i.e., within 24 hours) of other 5-HT 1 agonists or ergotamine-containing or ergot-type medications [see Drug Interactions (7.2) ]
- with concomitant use of peripheral and central vasoconstrictors because the combination may result in additive or synergistic elevation of blood pressure [see Warnings and Precautions (5.5) ]
WARNINGS AND PRECAUTIONS
- Myocardial Ischemia and/or Infarction, Other Cardiac Adverse Reactions, and Fatalities: In patients with risk factors predictive of coronary artery disease, consider first dose administration under medical supervision with electrocardiogram. (5.2 )
- Cerebrovascular Adverse Reactions and Fatalities: Cerebral hemorrhage, subarachnoid hemorrhage, and stroke have been reported; discontinue ATZUMI if suspected. (5.3 )
- Other Vasospasm Related Adverse Reactions: ATZUMI may cause vasospasm or elevation in blood pressure. Discontinue if signs or symptoms of vasoconstriction develop. (5.4 , 5.5 )
- Medication Overuse Headache: Detoxification may be necessary. (5.6 )
- Preterm Labor: Advise pregnant women of the risk. (5.7 , 8.1 )
- Fibrotic Complications: Pleural and retroperitoneal fibrosis have been reported following prolonged daily use of dihydroergotamine. Administration of ATZUMI should not exceed the dosing guidelines or be used for chronic daily administration. (5.8 )
- Local Irritation: If severe local irritation occurs for no other attributable reason, suspend ATZUMI until resolution. (5.9 )
Peripheral Ischemia Following Coadministration with Strong CYP3A4 Inhibitors
Serious and/or life-threatening peripheral ischemia has been associated with the coadministration of dihydroergotamine with strong CYP3A4 inhibitors, including protease inhibitors, macrolide antibiotics, and antifungals. Because CYP3A4 inhibition elevates the serum levels of dihydroergotamine, the risk for vasospasm leading to cerebral ischemia and/or ischemia of the extremities is increased. Hence, concomitant use of ATZUMI with strong CYP3A4 inhibitors is contraindicated [see Contraindications (4) and Drug Interactions (7.1) ] .
Myocardial Ischemia and/or Infarction, Other Cardiac Adverse Reactions, and Fatalities
The potential for cardiac adverse reactions exists with ATZUMI treatment. Serious adverse cardiac events, including some that have been fatal, have occurred following use of dihydroergotamine. These events have included acute myocardial infarction, life-threatening disturbances of cardiac rhythm (e.g., ventricular tachycardia and ventricular fibrillation), coronary artery vasospasm, and transient myocardial ischemia.
Prior to initiation of ATZUMI, a cardiovascular evaluation is recommended to determine if the patient is free of coronary artery and ischemic myocardial disease or other significant underlying cardiovascular disease. If, during the cardiovascular evaluation, the patient's medical history (including risk factors), or electrocardiographic investigation, findings are consistent with coronary artery vasospasm or myocardial ischemia, ATZUMI should not be administered [see Contraindications (4) ] .
For patients with risk factors predictive of coronary artery disease (e.g., hypertension, hypercholesterolemia, smoker, obesity, diabetes, strong family history of coronary artery disease, females who are surgically or physiologically postmenopausal, or males who are over 40 years of age) who are determined to have a satisfactory cardiovascular evaluation, it is strongly recommended that administration of the first dose of ATZUMI take place in the setting of an equipped healthcare facility, unless the patient has previously received dihydroergotamine. During the interval immediately following the first use of ATZUMI, an electrocardiogram is recommended in those patients with risk factors because ischemia can occur in the absence of clinical symptoms.
Cerebrovascular Adverse Reactions and Fatalities
The potential for adverse cerebrovascular adverse reactions exists with ATZUMI treatment. Cerebral hemorrhage, subarachnoid hemorrhage, stroke, and other cerebrovascular events have been reported in patients treated with dihydroergotamine; and some have resulted in fatalities. In a number of cases, it appears possible that the cerebrovascular events were primary, the dihydroergotamine having been administered in the incorrect belief that the symptoms experienced were a consequence of migraine, when they were not. It should be noted that patients with migraine may be at increased risk of certain cerebrovascular events (e.g., stroke, hemorrhage, transient ischemic attack).
Discontinue ATZUMI if a cerebrovascular event is suspected.
Other Vasospasm Related Adverse Reactions
ATZUMI, like other ergot alkaloids, may cause vasospastic reactions other than coronary artery vasospasm. Myocardial, peripheral vascular, and colonic ischemia have been reported with dihydroergotamine.
Dihydroergotamine associated vasospastic phenomena may also cause muscle pains, numbness, coldness, pallor, and cyanosis of the digits. In patients with compromised circulation, persistent vasospasm may result in gangrene or death. ATZUMI should be discontinued immediately if signs or symptoms of vasoconstriction develop.
Patients who experience other symptoms or signs suggestive of decreased arterial flow, such as ischemic bowel syndrome or Raynaud's syndrome, following the use of any 5-HT 1 agonist, including ATZUMI, should be evaluated by a healthcare provider.
Increase in Blood Pressure
Significant elevation in blood pressure has been reported on rare occasions in patients with and without a history of hypertension treated with dihydroergotamine. ATZUMI is contraindicated in patients with uncontrolled hypertension [see Contraindications (4) ].
An 18% increase in mean pulmonary artery pressure was seen following dosing with another 5-HT 1 agonist in a study evaluating subjects undergoing cardiac catheterization.
Medication Overuse Headache
Overuse of acute migraine drugs (e.g., ergotamines, triptans, opioids, or a combination of these drugs for 10 or more days per month) may lead to exacerbation of headache (i.e., medication overuse headache). Medication overuse headache may present as migraine-like daily headaches or as a marked increase in frequency of migraine attacks. Detoxification of patients including withdrawal of the overused drugs and treatment of withdrawal symptoms (which often includes a transient worsening of headache) may be necessary.
Preterm Labor
Based on the mechanism of action of dihydroergotamine and findings from the published literature, ATZUMI may cause preterm labor. Avoid use of ATZUMI during pregnancy [see Use in Specific Populations (8.1) and Clinical Pharmacology (12.2) ] .
Fibrotic Complications
The potential for fibrotic complications exists with ATZUMI treatment. There have been reports of pleural and retroperitoneal fibrosis in patients following prolonged daily use of dihydroergotamine . Rarely, prolonged daily use of other ergot alkaloid drugs has been associated with cardiac valvular fibrosis. Rare cases have also been reported in association with the use of dihydroergotamine; however, in those cases, patients also received drugs known to be associated with cardiac valvular fibrosis.
Administration of ATZUMI should not exceed the dosing guidelines and should not be used for chronic daily administration [see Dosage and Administration (2.1) ] .
Local Irritation
Local irritative symptoms were reported in 29% of patients treated with at least one dose of ATZUMI in an open-labeled trial, which allowed repeated use of ATZUMI up to 12 months. The common local irritative symptoms (at least 1% of patients) were nasal discomfort (11%), altered taste (8%), nasal congestion (5%), nasopharyngitis (5%), rhinorrhea (4%), cough (3%), nasal pain (3%), epistaxis (2%), sneezing (2%), nasal pruritus (1%), and increased lacrimation (1%). If a severe local irritation event occurs for no other attributable reasons, avoid further use of ATZUMI until the event resolves. Monitor patients for severe recurrent local irritation.
Nasal tissue in animals treated with dihydroergotamine mesylate daily showed mild mucosal irritation characterized by mucous cell and transitional cell hyperplasia and squamous cell metaplasia. Changes in rat nasal mucosa at 64 weeks were less severe than at 13 weeks. Local effects on respiratory tissue after chronic intranasal dosing in animals have not been evaluated.
ADVERSE REACTIONS
The following clinically significant adverse reactions are described elsewhere in the labeling:
- Peripheral Ischemia Following Coadministration with Strong CYP3A4 Inhibitors [see Boxed Warning and Warnings and Precautions (5.1) ]
- Myocardial Ischemia and/or Infarction, Other Adverse Cardiac Events, and Fatalities [see Warnings and Precautions (5.2) ]
- Cerebrovascular Adverse Reactions and Fatalities [see Warnings and Precautions (5.3) ]
- Other Vasospasm Related Adverse Reactions [see Warnings and Precautions (5.4) ]
- Increase in Blood Pressure [see Warnings and Precautions (5.5) ]
- Medication Overuse Headache [see Warnings and Precautions (5.6) ]
- Preterm Labor [see Warnings and Precautions (5.7) ]
- Fibrotic Complications [see Warnings and Precautions (5.8) ]
- Local Irritation [see Warnings and Precautions (5.9) ]
Clinical Trials Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
The studies described below were conducted with dihydroergotamine mesylate nasal spray; adverse reactions with ATZUMI nasal powder are expected to be similar to adverse reactions with dihydroergotamine mesylate nasal spray.
Adverse Reactions in Placebo-Controlled Trials with Dihydroergotamine Mesylate Nasal Spray [see Clinical Studies (14) ]
Of the 1,796 patients and subjects treated with dihydroergotamine mesylate nasal spray doses 2 mg or less in U.S. and foreign clinical studies, 26 (1.4%) discontinued because of adverse events. The adverse events associated with discontinuation were, in decreasing order of frequency: rhinitis (13), dizziness (2), facial edema (2), and one patient each due to cold sweats, accidental trauma, depression, elective surgery, somnolence, allergy, vomiting, hypotension, and paraesthesia.
Table 1 summarizes the incidence rates of adverse reactions reported by at least 1% of patients who received dihydroergotamine mesylate nasal spray for the treatment of migraine during placebo-controlled, double-blind clinical studies and were more frequent than in those patients receiving placebo. The most commonly reported adverse reactions (greater than 1% of patients who received dihydroergotamine mesylate nasal spray) were rhinitis, nausea, altered sense of taste, application site reactions, dizziness, vomiting, somnolence, pharyngitis, and diarrhea. In most instances these events were transient and self-limited and did not result in patient discontinuation from a study.
| Dihydroergotamine Mesylate Nasal Spray N=597 % | Placebo N=631 % | |
|---|---|---|
| Respiratory System | ||
| Rhinitis | 26 | 7 |
| Pharyngitis | 3 | 1 |
| Gastrointestinal System | ||
| Nausea | 10 | 4 |
| Vomiting | 4 | 1 |
| Diarrhea | 2 | <1 |
| Special Senses, Other | ||
| Altered Sense of Taste | 8 | 1 |
| Application Site | ||
| Application Site Reaction | 6 | 2 |
| Central and Peripheral Nervous System | ||
| Dizziness | 4 | 2 |
| Somnolence | 3 | 2 |
| Body as a Whole, General | ||
| Hot Flashes | 1 | <1 |
| Asthenia | 1 | 0 |
| Musculoskeletal System | ||
| Stiffness | 1 | <1 |
Adverse Reactions in Studies with ATZUMI
An open-label study in adults was conducted to evaluate the safety and tolerability of ATZUMI, with repeated use of ATZUMI over the course of 6 to 12 months. A total of 344 patients with migraine received at least one dose of ATZUMI. One hundred and eighty-eight patients treated on average at least two migraines per month for at least 6 months, and 86 patients treated at least two migraines per month for at least one year. Of the patients who received at least one dose of ATZUMI, 99 (29%) experienced local irritative symptoms. Of these, the most common local irritative symptoms (at least 5% of patients) were nasal discomfort, altered taste, nasal congestion, and nasopharyngitis [see Warnings and Precautions (5.9) ] . The most common adverse reaction resulting in discontinuation in the long-term safety study was nasal discomfort (1.5%).
Postmarketing Experience
The following adverse reactions have been identified during postapproval use of dihydroergotamine. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure:
- Vasospasm, paresthesia, hypertension, dizziness, anxiety, dyspnea, headache, flushing, diarrhea, rash, increased sweating, and pleural and retroperitoneal fibrosis after long-term use of dihydroergotamine. Cases of myocardial infarction and stroke have been reported following the use of dihydroergotamine [see Warnings and Precautions (5.2) ] .
DRUG INTERACTIONS
CYP3A4 Inhibitors
There have been rare reports of serious adverse events in connection with the coadministration of intravenous administration of dihydroergotamine and strong CYP3A4 inhibitors, resulting in vasospasm that led to cerebral ischemia and/or ischemia of the extremities [see Warnings and Precautions (5.1) ]. The use of strong CYP3A4 inhibitors with ATZUMI is contraindicated [see Contraindications (4) ]. Administer moderate CYP3A4 inhibitors with caution.
Triptans
Triptans (serotonin [5-HT] 1B/1D receptor agonists) have been reported to cause coronary artery vasospasm, and its effects could be additive with ATZUMI. Therefore, triptans and ATZUMI should not be taken within 24 hours of each other [see Contraindications (4) ] .
Beta Blockers
There have been reports that propranolol may potentiate the vasoconstrictive action of ergotamine by blocking the vasodilating property of epinephrine.
Vasoconstrictors
ATZUMI is contraindicated for use with peripheral and central vasoconstrictors because the combination may cause synergistic elevation of blood pressure [see Warnings and Precautions (5.5) ] .
Nicotine
Nicotine may provoke vasoconstriction in some patients, predisposing to a greater ischemic response to ergot therapy [see Warnings and Precautions (5.2 , 5.4) ] .
Selective Serotonin Reuptake Inhibitors
Weakness, hyperreflexia, and incoordination have been reported rarely when 5-HT 1 agonists have been co-administered with selective serotonin reuptake inhibitors (e.g., fluoxetine, fluvoxamine, paroxetine, sertraline).
DESCRIPTION
ATZUMI contains dihydroergotamine, an ergotamine derivative, as the mesylate salt. Dihydroergotamine mesylate is a white or almost white crystalline powder. It is slightly soluble in water and chloroform and sparingly soluble in methanol. The chemical designation for dihydroergotamine mesylate is (6aR,9R,10aR)-N-[(2R,5S,10aS,10bS)-5-benzyl-10b-hydroxy-2-methyl-3,6-dioxo-octahydro-8H-oxazolo[3,2-α]pyrrolo[2,1-c]pyrazin-2-yl]-7-methyl- 4,6,6a,7,8,9,10,10a-octahydroindolo[4,3-fg]quinoline-9-carboxamide methanesulphonate. The empirical formula is C 33 H 37 N 5 O 5 ∙ CH 4 O 3 S. The molecular weight is 679.80, and it has the following structure:
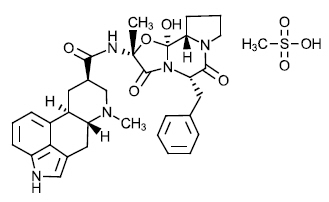
ATZUMI contains dihydroergotamine 5.2 mg (equivalent to 6.0 mg dihydroergotamine mesylate).
ATZUMI nasal powder is a drug-device combination product consisting of a powder prefilled in a single-dose delivery device for nasal administration into one nostril. ATZUMI does not need to be assembled or primed before use. Inactive ingredients are hypromellose, mannitol, and microcrystalline cellulose.
CLINICAL PHARMACOLOGY
Mechanism of Action
Dihydroergotamine binds with high affinity to 5-HT 1Dα and 5-HT 1Dβ receptors.
The therapeutic activity of dihydroergotamine in migraine is generally attributed to the agonist effects at 5-HT 1D receptors.
Pharmacodynamics
Significant elevation in blood pressure has been reported in patients treated with dihydroergotamine with and without a history of hypertension [see Warnings and Precautions (5.5) ] .
Dihydroergotamine possesses oxytocic properties [see Warnings and Precautions (5.7) ] .
Pharmacokinetics
Absorption
Following ATZUMI administration, the mean maximum plasma concentration was 2.1 ng/mL, and the median time from dosing to maximum plasma concentration was approximately 0.5 hours.
Distribution
Dihydroergotamine is 93% plasma protein bound. The apparent steady-state volume of distribution is approximately 800 liters.
Elimination
The mean apparent half-life of dihydroergotamine following nasal administration of ATZUMI in healthy subjects is approximately 13 hours.
Metabolism
Four dihydroergotamine mesylate metabolites have been identified in human plasma following oral administration. The major metabolite, 8'-β-hydroxydihydroergotamine, exhibits affinity equivalent to its parent for adrenergic and 5-HT 1 receptors and demonstrates equivalent potency in several venoconstrictor activity models, in vivo and in vitro. The other metabolites, (i.e., dihydrolysergic acid, dihydrolysergic amide) and a metabolite formed by oxidative opening of the proline ring are of minor importance.
Following nasal administration of ATZUMI, the 8'-β-hydroxydihydroergotamine metabolite plasma AUC was approximately 16% of the plasma AUC of dihydroergotamine, and the mean C max (5.7% of parent) was below the minimal concentrations required for receptor binding for adrenergic and 5-HT 1 receptors.
Excretion
The major excretory route of dihydroergotamine is via the bile in the feces. The total body clearance following ATZUMI administration is 1.5 L/min which reflects mainly hepatic clearance. The renal clearance (0.1 L/min) is unaffected by the route of dihydroergotamine administration based on other dihydroergotamine products.
Specific Populations
No studies have been conducted on the effect of renal or hepatic impairment, gender, race, ethnicity, or pregnancy on dihydroergotamine pharmacokinetics [see Contraindications (4) , Use in Specific Populations (8.1) ] .
Drug Interaction Studies
CYP3A4 Inhibitors
In a drug interaction study, administration of ATZUMI with itraconazole increased dihydroergotamine plasma exposure by 14% for C max and 19% for AUC while the plasma exposures (C max and AUC 0-inf ) of 8'-β-hydroxy dihydroergotamine (8'-OH-DHE, active metabolite) were increased by approximately 4-fold and 3-fold, respectively [see Contraindications (4) , Warnings and Precautions (5.1) , Drug Interactions (7.1) ] .
Other Drugs
The pharmacokinetics of dihydroergotamine did not appear to be significantly affected by the concomitant use of a local vasoconstrictor.
Multiple oral doses of the β-adrenoceptor antagonist propranolol, used for preventive treatment of migraine, had no significant influence on the C max , T max or AUC of dihydroergotamine doses up to 4 mg [see Drug Interactions (7.3) ].
The effect of oral contraceptives on the pharmacokinetics of dihydroergotamine has not been studied.
NONCLINICAL TOXICOLOGY
Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
In a 2-year mouse carcinogenicity study, subcutaneous administration of dihydroergotamine mesylate (0, 0.5, 1.5, or 5 mg/kg/day) resulted in an increased incidence of fibrosarcoma at the injection sites in males and females at the high dose.
In a 2-year rat carcinogenicity study, intranasal administration of dihydroergotamine mesylate (0, 0.4, 0.8, or 1.6 mg/day for 13 weeks, followed by 0, 0.08, 0.24, or 0.8 mg/day for the remainder of the study) did not result in an increase in tumors.
Mutagenesis
Dihydroergotamine mesylate was negative in an in vitro mutagenicity (Ames) assay and positive in in vitro chromosomal aberration (V79 Chinese hamster cell assay with metabolic activation, and human peripheral blood lymphocyte) assays. Dihydroergotamine was negative in in vivo micronucleus assays in mouse and hamster.
Impairment of Fertility
Intranasal administration of dihydroergotamine to rats at doses up to 1.6 mg/day was not associated with adverse effects on fertility.
CLINICAL STUDIES
The efficacy of ATZUMI for the acute treatment of migraine with or without aura in adults was based on the relative bioavailability of ATZUMI nasal powder compared to dihydroergotamine mesylate nasal spray .
The clinical trials described below were conducted using dihydroergotamine mesylate nasal spray.
The efficacy of dihydroergotamine mesylate nasal spray for the acute treatment of migraine headaches was evaluated in four randomized, double-blind, placebo controlled studies in the U.S. The patient population for the trials was predominantly female (87%) and Caucasian (95%) with a mean age of 39 years (range 18 to 65 years). Patients treated a single moderate to severe migraine headache with a single dose of study medication and assessed pain severity over the 24 hours following treatment. Headache response was determined 0.5, 1, 2, 3 and 4 hours after dosing and was defined as a reduction in headache severity to mild or no pain. In studies 1 and 2, a four-point pain intensity scale was utilized; in studies 3 and 4, a five-point scale was used to record pain response. Although rescue medication was allowed in all four studies, patients were instructed not to use them during the four hour observation period. In studies 3 and 4, a total dose of 2 mg was compared to placebo. In studies 1 and 2, doses of 2 and 3 mg were evaluated, and showed no advantage of the higher dose for a single treatment. In all studies, patients received a regimen consisting of 0.5 mg in each nostril, repeated in 15 minutes (and again in another 15 minutes for the 3 mg dose in studies 1 and 2).
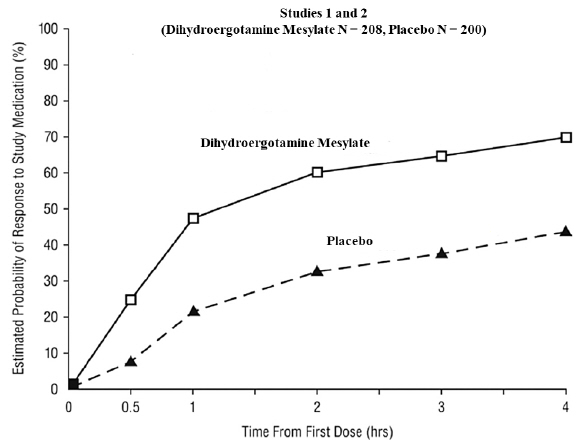
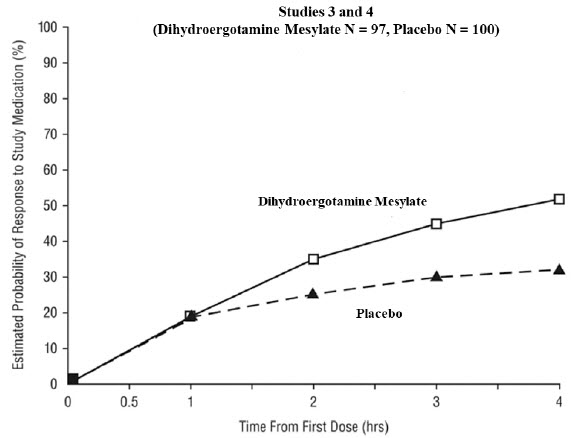
The percentage of patients achieving headache response 4 hours after treatment was significantly greater in patients receiving 2 mg doses of dihydroergotamine mesylate nasal spray compared to those receiving placebo in 3 of the 4 studies (see Table 2 and Table 3 and Figure 1 and Figure 2 ).
| N | 2 hours | 4 hours | ||
|---|---|---|---|---|
| Study 1 | Dihydroergotamine mesylate nasal spray | 105 | 61% p value < 0.001 | 70% |
| Placebo | 98 | 23% | 28% | |
| Difference from Placebo | 37% | 42% | ||
| Study 2 | Dihydroergotamine mesylate nasal spray | 103 | 47% | 56% p value < 0.01 |
| Placebo | 102 | 33% | 35% | |
| Difference from Placebo | 14% | 21% |
| N | 2 hours | 4 hours | ||
|---|---|---|---|---|
| Study 3 | Dihydroergotamine mesylate nasal spray | 50 | 32% | 48% p value < 0.01 |
| Placebo | 50 | 20% | 22% | |
| Difference from Placebo | 12% | 26% | ||
| Study 4 | Dihydroergotamine mesylate nasal spray | 47 | 30% | 47% |
| Placebo | 50 | 20% | 30% | |
| Difference from Placebo | 10% | 17% |
The Kaplan-Meier plots below (Figure 1 and Figure 2) provides an estimate of the probability that a patient will have responded to a single 2 mg dose of dihydroergotamine mesylate nasal spray as a function of the time elapsed since initiation of treatment.
 |
 |
For patients with migraine-associated nausea, photophobia, and phonophobia at baseline, there was a lower incidence of these symptoms at 2 and 4 hours following administration of dihydroergotamine mesylate nasal spray compared to placebo.
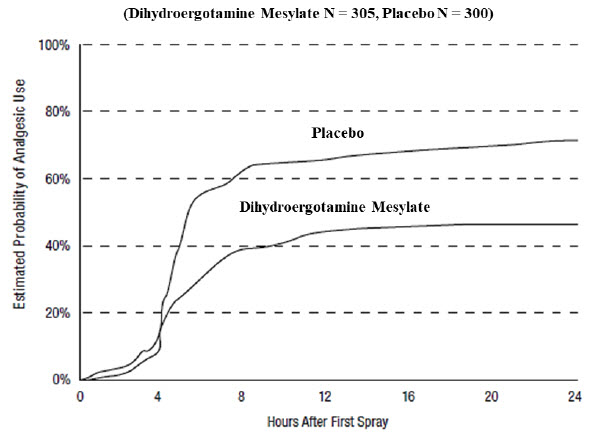
Patients were not allowed to use additional treatments for 8 hours prior to study medication dosing and during the 4-hour observation period following study treatment. Following the 4-hour observation period, patients were allowed to use additional treatments. For all studies, the estimated probability of patients using additional treatments for their migraines over the 24 hours following the single 2 mg dose of study treatment is summarized in Figure 3 below.
 |
Neither age nor sex appear to affect the patient's response to dihydroergotamine mesylate nasal spray. The racial distribution of patients was insufficient to determine the effect of race on the efficacy of dihydroergotamine mesylate nasal spray.
HOW SUPPLIED/STORAGE AND HANDLING
How Supplied
ATZUMI (dihydroergotamine) nasal powder is supplied in a single-dose nasal device with white powder containing 5.2 mg of dihydroergotamine. ATZUMI is available in a carton of 8 nasal devices each individually packaged in a protective foil pouch (NDC 76978-101-08).
Storage and Handling
Store ATZUMI at controlled room temperature, 20°C to 25°C (68°F to 77°F), with excursions allowed between 15°C to 30°C (59°F to 86°F).
Store ATZUMI in its protective foil pouch until ready to use.
INSTRUCTIONS FOR USE
This Instructions for Use contains information on how to use ATZUMI.
Read this Instructions for Use before using ATZUMI.
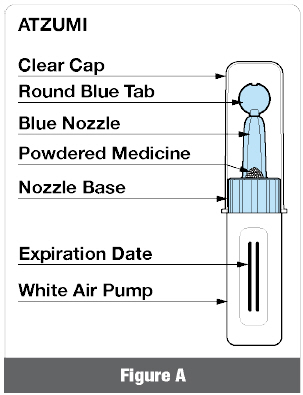
Important Information You Need to Know Before Using ATZUMI
- ATZUMI contains 1 complete dose of medicine and should be thrown away after each use.
- ATZUMI is for nasal (nose) use only.
- Deliver all the powdered medicine into only 1 nostril.
- Do not use ATZUMI if it is damaged or expired.
- Do not squeeze ATZUMI before inserting it into the nostril. Priming is not required.
- Powdered medicine is inside the blue nozzle. When you squeeze the white air pump, air is pushed into the blue nozzle and pushes the powdered medicine into your nose.
- Do not squeeze slowly, partially or with any hesitation. When dosing, you must fully squeeze the white air pump as fast as you can. A fast, pulse-like squeezing action is needed.
How often can you use ATZUMI?
- If needed, you may take a second dose 1 hour after your first dose. Wait at least 1 hour before taking the second dose.
- Do not take more than 2 doses within a 24-hour period.
- It is not known if it is safe to take more than 4 doses of ATZUMI in a 7-day period or 12 doses in a 30-day period.
Storing ATZUMI
- Store ATZUMI at room temperature between 68°F to 77°F (20°C to 25°C).
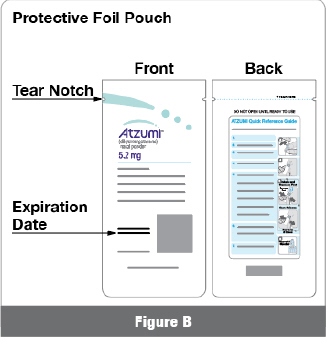
- Store ATZUMI in its protective foil pouch until ready to use (Figure C).
- Keep ATZUMI and all medicines out of the reach of children.

- 1.1 Blow Your Nose
 Blow your nose to clear your nostrils (Figure D).
Blow your nose to clear your nostrils (Figure D). - 1.2 Take Out ATZUMI
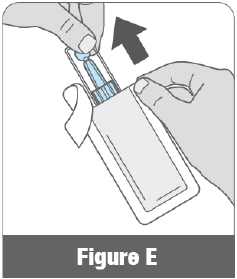 Open the protective foil pouch by tearing at the notch. Remove ATZUMI from the protective foil pouch (Figure E).
Open the protective foil pouch by tearing at the notch. Remove ATZUMI from the protective foil pouch (Figure E). - 1.3 Check ATZUMI
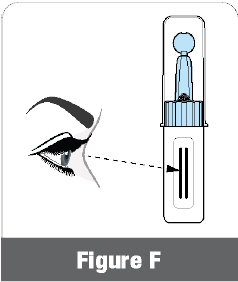 Check the Expiration Date to make sure ATZUMI is not expired (Figure F). Check ATZUMI for damage . If ATZUMI is expired or damaged, throw it away in your household trash and get a new ATZUMI.
Check the Expiration Date to make sure ATZUMI is not expired (Figure F). Check ATZUMI for damage . If ATZUMI is expired or damaged, throw it away in your household trash and get a new ATZUMI. - 1.4 Remove Clear Cap
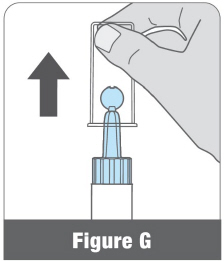 Pull the clear cap straight off (Figure G).
Pull the clear cap straight off (Figure G).
- 2.1 Remove Round Blue Tab
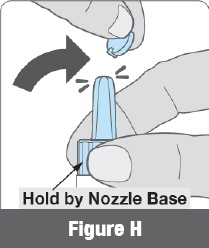 Hold the nozzle base in 1 hand. Remove the round blue tab by bending it back and forth or twisting it to break it off (Figure H). This creates an opening for the powdered medicine to pass through. Important: Do not squeeze the white air pump yet. Wait until Step 2.3.
Hold the nozzle base in 1 hand. Remove the round blue tab by bending it back and forth or twisting it to break it off (Figure H). This creates an opening for the powdered medicine to pass through. Important: Do not squeeze the white air pump yet. Wait until Step 2.3. - 2.2 Insert Into Nostril
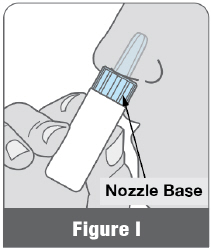 Hold the white air pump as shown in Figure I and insert the blue nozzle into 1 nostril as far as it will comfortably go. The nozzle base should touch your nose (Figure I).
Hold the white air pump as shown in Figure I and insert the blue nozzle into 1 nostril as far as it will comfortably go. The nozzle base should touch your nose (Figure I). - 2.3 Deliver All of the Powdered Medicine into Only 1 Nostril
- • Squeeze the white air pump 3 separate times into 1 nostril. Inhale through your nose each time you squeeze (Figure J).
- • Fast, complete, pulse-like squeezes are needed to push the powdered medicine and deliver the complete dose.
- • Do not squeeze slowly, partially or with any hesitation.
- • Allow the white air pump to expand back to its original shape between squeezes (Figure J).
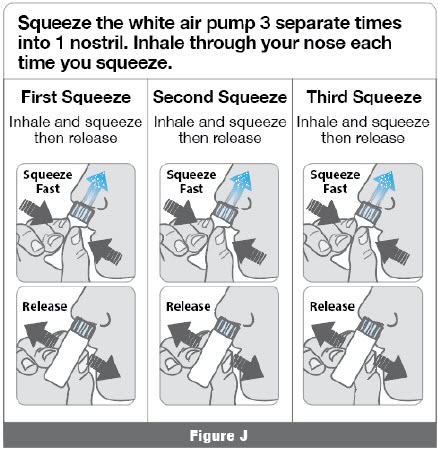 Important: Deliver all the powdered medicine into only 1 nostril.
Important: Deliver all the powdered medicine into only 1 nostril. 
- 3.1 Check for Remaining Powdered Medicine
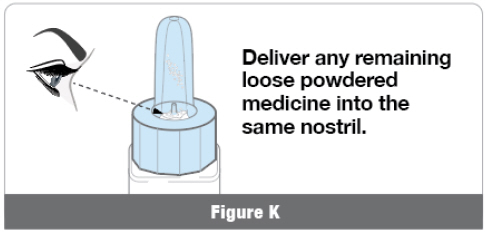
- • Keep ATZUMI upright and look inside the blue nozzle to see if any loose powdered medicine remains at the bottom (Figure K).
- • If loose powdered medicine remains, repeat Step 2.3 to dose into the same nostril, but squeeze the white air pump faster . Repeat Step 2.3 until no loose powdered medicine remains. Note:
- • It is normal to see a light coating of powdered medicine in the blue nozzle after delivering the complete dose.
- • If you are not sure whether you have delivered all of the loose powdered medicine, then repeat Step 2.3 with the same ATZUMI device in the same nostril.
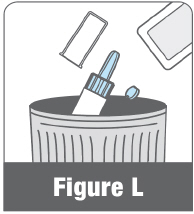 After use, throw away the protective foil pouch, the ATZUMI device, the round blue tab, and the clear cap in your household trash (Figure L). Do not save ATZUMI after use. ATZUMI contains a one-time (single) dose.
After use, throw away the protective foil pouch, the ATZUMI device, the round blue tab, and the clear cap in your household trash (Figure L). Do not save ATZUMI after use. ATZUMI contains a one-time (single) dose.
This Instructions for Use has been approved by the U.S. Food and Drug Administration. Approved: 4/2025
Quick Reference GuideThis is a Quick Reference Guide. Read the full Instructions for Use before using ATZUMI. Deliver ATZUMI into only 1 nostril.
- Blow your nose to clear your nostrils.
- Pull the clear cap straight off.
- Twist or bend the round blue tab to break it off.
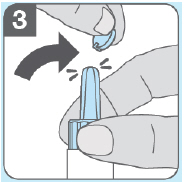
- Insert the blue nozzle all the way into your nostril.
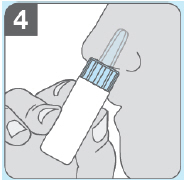
- Squeeze the white air pump 3 separate times into 1 nostril. Inhale through your nose each time you squeeze . Fast, complete, pulse-like squeezes are needed. Do not squeeze slowly, partially or with hesitation. Allow the white air pump to expand back to its original shape between squeezes. Deliver all of the powdered medicine into only 1 nostril.
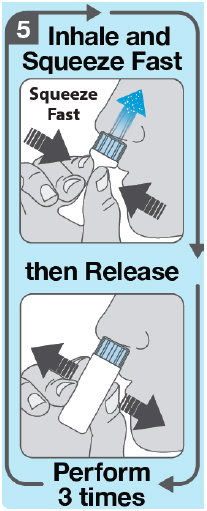
- Check inside the blue nozzle. If loose powdered medicine remains, repeat Step 5 with the same ATZUMI device in the same nostril, but with a faster squeeze .
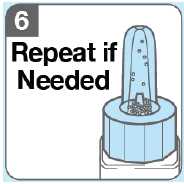
- Throw away ATZUMI in your household trash. ATZUMI is for one-time (single) use only.
This Quick Reference Guide has been approved by the U.S. Food and Drug Administration. Approved: 04/2025
Mechanism of Action
Dihydroergotamine binds with high affinity to 5-HT 1Dα and 5-HT 1Dβ receptors.
The therapeutic activity of dihydroergotamine in migraine is generally attributed to the agonist effects at 5-HT 1D receptors.